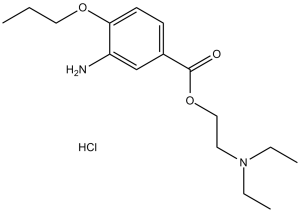
Proparacaine HCl (Proxymetacaine; Proxymetacaine), the hydrochloride salt of proparacaine, is a voltage-gated sodium channels antagonist approved as an ophthalmic solution for topical anesthetic use in ophthalmic practice. It inhibits voltage-gated sodium channels with ED50 of 3.4 mM. Proparacaine is more potent and less toxic than cocaine. Proparacaine significantly increases in FHV-1, C. felis, and 28S rDNA Ct values when fusidic acid is used. Proparacaine inhibits corneal epithelial migration and adhesion through alteration of the actin cytoskeleton. Proparacaine acts like bupivacaine or lidocaine and produces dose-related spinal blockades of motor function, proprioception and nociception.
Physicochemical Properties
| Molecular Formula | C16H26N2O3.HCL | |
| Molecular Weight | 330.85 | |
| Exact Mass | 330.171 | |
| CAS # | 5875-06-9 | |
| Related CAS # |
|
|
| PubChem CID | 517321 | |
| Appearance | Typically exists as solid at room temperature | |
| Boiling Point | 434.4ºC at 760mmHg | |
| Flash Point | 216.5ºC | |
| LogP | 3.939 | |
| Hydrogen Bond Donor Count | 2 | |
| Hydrogen Bond Acceptor Count | 5 | |
| Rotatable Bond Count | 10 | |
| Heavy Atom Count | 22 | |
| Complexity | 295 | |
| Defined Atom Stereocenter Count | 0 | |
| SMILES | O=C(OCCN(CC)CC)C1=CC=C(OCCC)C(N)=C1.[H]Cl |
|
| InChi Key | BFUUJUGQJUTPAF-UHFFFAOYSA-N | |
| InChi Code | InChI=1S/C16H26N2O3.ClH/c1-4-10-20-15-8-7-13(12-14(15)17)16(19)21-11-9-18(5-2)6-3;/h7-8,12H,4-6,9-11,17H2,1-3H3;1H | |
| Chemical Name | 2-(diethylamino)ethyl 3-amino-4-propoxybenzoate;hydrochloride | |
| Synonyms | proparacaine; Proxymetacaine; 499-67-2; 2-(Diethylamino)ethyl 3-amino-4-propoxybenzoate; Proximetacainum; Proximetacaina; Prossimetacaina; Proxymetacaine; Proxymetacaine | |
| HS Tariff Code | 2934.99.9001 | |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month Note: Please store this product in a sealed and protected environment, avoid exposure to moisture. |
|
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets | Voltage-gated sodium channels |
| ln Vitro |
Proparacaine Hydrochloride (>588.93 μM; 4-28 hours) has a dose- and time-dependent cytotoxicity to HCS cells at concentrations in vitro[1]. Proparacaine Hydrochloride (294.47-18.85 mM; 4-12 hours) can induce apoptosis of HCS Proparacaine Hydrochloride (4.71 mM; 4-12 hours) induces G1 phase arrest, plasma membrane permeability elevation, phosphatidylserine externalization, DNA fragmentation, chromatin condensation, and apoptotic body formation of HCS cells [1]. Proparacaine hydrochloride causes disruption of the mitochondrial transmembrane potential as well as activation of caspase -2, -3, and -9[1]. Proparacaine Hydrochloride (4.71 mM; 4-12 hours) downregulates and upregulates the expression of Bcl-xL and Bax, respectively, and remarkably upregulates cytoplasmic cytochrome C and apoptosis inducing factor[1]. Treatment of corneal stromal cells with Proparacaine HCl resulted in concentration-dependent cytotoxicity, as indicated by decreased cell viability. The drug induced mitochondria-dependent apoptosis, characterized by reduced mitochondrial membrane potential, increased release of cytochrome c from mitochondria to cytoplasm, upregulated expression of Bax and cleaved caspase-3/-9, and downregulated expression of Bcl-2. Additionally, Proparacaine HCl promoted reactive oxygen species (ROS) generation in corneal stromal cells[1] - In nasal mucosal epithelial cells and mast cells isolated from allergic rhinitis models, Proparacaine HCl treatment inhibited the production of Th2 cytokines (IL-4, IL-5, IL-13) and histamine. It also suppressed the activation of NF-κB signaling pathway, as evidenced by reduced phosphorylation of IκBα and p65[2] |
| ln Vivo |
When administered intranasally for seven days, proparacaine hydrochloride (75 μg/30 μL) dramatically reduces the amount of mast cells, goblet cells, and eosinophils in the nasal mucosa's lamina propria[2]. In a mouse model of corneal injury, topical application of Proparacaine HCl (0.5%, 4 times daily for 7 days) exacerbated corneal stromal cell apoptosis and delayed corneal wound healing. Histopathological examination showed increased inflammatory cell infiltration and disorganized collagen fibers in the corneal stroma. Immunohistochemical staining confirmed upregulated expression of cleaved caspase-3 and Bax, and downregulated Bcl-2 in corneal tissues[1] - In an ovalbumin (OVA)-induced mouse model of allergic rhinitis, intranasal administration of Proparacaine HCl (0.5% or 1%, 50 μL per nostril, once daily for 14 days) significantly reduced allergic rhinitis symptoms, including the number of sneezes and nasal rubbings. The drug decreased inflammatory cell infiltration (eosinophils, mast cells) in the nasal mucosa, lowered serum levels of OVA-specific IgE, and reduced the expression of IL-4, IL-5, and IL-13 in nasal mucosal tissues. It also increased the expression of IFN-γ, shifting the immune response towards Th1 polarization[2] |
| Enzyme Assay |
Caspase activity assay: After treating corneal stromal cells with Proparacaine HCl for 24 hours, cells were lysed and incubated with caspase-3/-9 specific substrates. The fluorescence intensity of the cleaved substrates was measured using a microplate reader to determine the activity of caspases[1] - NF-κB activity assay: Nuclear extracts from Proparacaine HCl-treated nasal mucosal cells were prepared. The binding activity of NF-κB to its specific DNA probe was detected by electrophoretic mobility shift assay (EMSA), and the intensity of the shifted bands was quantified[2] |
| Cell Assay |
Cell Viability Assay[1] Cell Types: HCS cells Tested Concentrations: 294.47 μM, 588.93 μM, 1.18 mM, 2.35 mM, 4.71 mM, 9.42 mM, 18.85 mM Incubation Duration: 4 hrs (hours), 8 hrs (hours), and 12 hrs (hours), 16 hrs (hours), 20 hrs (hours), 24 hrs (hours), 28 hrs (hours) Experimental Results: diminished the viability of HCS cells with concentration and time at concentrations above 588.93 μM. Apoptosis Analysis[1] Cell Types: HCS cells Tested Concentrations: 294.47 μM, 588.93 μM, 1.18 mM, 2.35 mM, 4.71 mM, 9.42 mM, 18.85 mM Incubation Duration: 4 hrs (hours), 8 hrs (hours), and 12 hrs (hours) Experimental Results: Induced apoptosis of HCS cells. Cell Cycle Analysis[1] Cell Types: HCS cells Tested Concentrations: 4.71 mM Incubation Duration: 4 hrs (hours), 8 hrs (hours), and 12 hrs (hours) Experimental Results: Arrested HCS cells at the G1 phase of the cell cycle. Western Blot Analysis[1] Cell Types: HCS cells Tested Concentrations: 4.71 mM Incubation Duration: 4 hrs (hours), 8 hrs (hours), and 12 hrs (hours) Experimental Results: Down-regulated the expression level of anti-apoptotic protein Bcl-xL and up-regulated the pro-apoptotic protein Bax, whereas Dramatically up-regulated the cytopl Corneal stromal cell viability assay: Primary corneal stromal cells were seeded in 96-well plates and treated with Proparacaine HCl at concentrations of 0.125%, 0.25%, 0.5%, 1%, and 2% for 24, 48, and 72 hours. Cell viability was assessed using the MTT assay, and absorbance was measured at 570 nm[1] - Apoptosis detection assay: Corneal stromal cells treated with Proparacaine HCl were stained with Annexin V-FITC and propidium iodide (PI), then analyzed by flow cytometry to quantify apoptotic cells. Hoechst 33258 staining was also performed to observe nuclear condensation and fragmentation of apoptotic cells[1] - Cytokine detection assay: Nasal mucosal epithelial cells were treated with Proparacaine HCl for 24 hours. The concentrations of IL-4, IL-5, IL-13, and IFN-γ in the cell culture supernatant were measured by enzyme-linked immunosorbent assay (ELISA). Total RNA was extracted from cells, and the mRNA expression levels of these cytokines were detected by quantitative real-time PCR (qPCR)[2] |
| Animal Protocol |
Animal/Disease Models: 7-week- old female balb/c (Bagg ALBino) mouse, allergic rhinitis model[2] Doses: 75 μg/30 μL Route of Administration: Intranasal administration, for 7 days Experimental Results: Dramatically decreased nasal rubbing and sneezing. Corneal injury mouse model: C57BL/6 mice (6-8 weeks old) were used to establish corneal epithelial defect models by mechanical scraping. Proparacaine HCl was formulated as a 0.5% ophthalmic solution. Mice were topically administered 5 μL of the solution to the injured eye 4 times daily for 7 days. Control mice received normal saline. At the end of the experiment, mice were euthanized, and corneal tissues were collected for histopathological, immunohistochemical, and Western blot analyses[1] - Allergic rhinitis mouse model: BALB/c mice (6-8 weeks old) were sensitized by intraperitoneal injection of OVA emulsified with aluminum hydroxide on days 0 and 7. From day 14 to day 27, mice were intranasally challenged with OVA solution daily to induce allergic rhinitis. Proparacaine HCl was prepared as 0.5% and 1% solutions. Treatment groups received 50 μL of the solution per nostril once daily from day 14 to day 27. Control groups received normal saline. Nasal symptoms were recorded 30 minutes after each challenge. Mice were sacrificed on day 28, and nasal mucosal tissues and blood samples were collected for further analysis[2] |
| Toxicity/Toxicokinetics |
In vitro toxicity: Proparacaine HCl exhibited cytotoxicity to corneal stromal cells with an IC50 value of approximately 0.5% after 24 hours of treatment[1] - In vivo toxicity: Topical application of Proparacaine HCl (0.5%) to injured corneas in mice caused excessive apoptosis of corneal stromal cells, delayed wound healing, and increased corneal inflammation[1] - No obvious systemic toxicity (such as liver or kidney damage) was observed in mice after intranasal administration of Proparacaine HCl at doses up to 1% for 14 days[2] |
| References |
[1]. Wen Yi Fan, et al. Proparacaine induces cytotoxicity and mitochondria-dependent apoptosis in corneal stromal cells both in vitro and in vivo. Toxicol Res (Camb). 2016 Sep 1; 5(5): 1434-1444. [2]. Hwan Soo Kim, et al. Effect of Proparacaine in a Mouse Model of Allergic Rhinitis. Clin Exp Otorhinolaryngol. 2017 Dec; 10(4): 325–331. |
| Additional Infomation |
Proparacaine Hydrochloride is the hydrochloride salt form of proparacaine, a benzoic acid derivative with local anesthetic property. Proparacaine hydrochloride stabilizes the neuronal membrane by binding to and inhibiting voltage-gated sodium channels, thereby inhibiting sodium ion influx required for the initiation and conduction of impulses within the neuronal cell, and resulting in a loss of sensation. See also: Proparacaine (has active moiety); Fluorescein sodium; proparacaine hydrochloride (component of). Proparacaine HCl is a commonly used topical anesthetic in ophthalmology. This study suggests that its long-term or high-concentration use may cause corneal stromal cell damage through mitochondria-dependent apoptosis, which should be noted in clinical application[1] - This study is the first to report the anti-allergic effect of Proparacaine HCl in a mouse model of allergic rhinitis, providing a potential new application for the drug beyond topical anesthesia[2] |
Solubility Data
| Solubility (In Vitro) |
|
|||
| Solubility (In Vivo) |
Solubility in Formulation 1: ≥ 2.5 mg/mL (7.56 mM) (saturation unknown) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 400 μL PEG300 and mix evenly; then add 50 μL Tween-80 to the above solution and mix evenly; then add 450 μL normal saline to adjust the volume to 1 mL. Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH₂ O to obtain a clear solution. Solubility in Formulation 2: ≥ 2.5 mg/mL (7.56 mM) (saturation unknown) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 900 μL of 20% SBE-β-CD physiological saline solution and mix evenly. Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Solubility in Formulation 3: ≥ 2.5 mg/mL (7.56 mM) (saturation unknown) in 10% DMSO + 90% Corn Oil (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 900 μL of corn oil and mix evenly. Solubility in Formulation 4: Saline: 30 mg/mL Solubility in Formulation 5: 60 mg/mL (181.35 mM) in PBS (add these co-solvents sequentially from left to right, and one by one), clear solution; with ultrasonication. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 3.0225 mL | 15.1126 mL | 30.2252 mL | |
| 5 mM | 0.6045 mL | 3.0225 mL | 6.0450 mL | |
| 10 mM | 0.3023 mL | 1.5113 mL | 3.0225 mL |