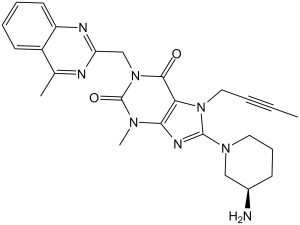
Linagliptin (formerly known as BI-1356; trade names Tradjenta and Trajenta) is a xanthine-based, highly potent, selective, and competitive DPP-4 inhibitor based on xanthine that may have anti-diabetic effects. At an IC50 of 1 nM, it inhibits DPP-4. The breakdown of incretins like GLP-1, which is crucial to the process of glucose metabolism, is largely mediated by DPP-4. DPP-4, which is found on the capillary endothelium close to the L-cells where GLP-1 is secreted in the ileum, quickly truncates GLP-1 under physiological conditions. The FDA approved linagliptin on May 2, 2011, for the treatment of type II diabetes. Lilly and Boehringer Ingelheim are the companies marketing it.
Physicochemical Properties
| Molecular Formula | C25H28N8O2 |
| Molecular Weight | 472.54 |
| Exact Mass | 472.233 |
| Elemental Analysis | C, 63.54; H, 5.97; N, 23.71; O, 6.77 |
| CAS # | 668270-12-0 |
| Related CAS # | Linagliptin-d4;2140263-92-7;Linagliptin-13C,d3;1398044-43-3 |
| PubChem CID | 10096344 |
| Appearance | White to yellow solid; also reported as a crystalline solid |
| Density | 1.4±0.1 g/cm3 |
| Boiling Point | 661.2±65.0 °C at 760 mmHg |
| Melting Point | 202ºC |
| Flash Point | 353.7±34.3 °C |
| Vapour Pressure | 0.0±2.0 mmHg at 25°C |
| Index of Refraction | 1.717 |
| LogP | 1.99 |
| Hydrogen Bond Donor Count | 1 |
| Hydrogen Bond Acceptor Count | 7 |
| Rotatable Bond Count | 4 |
| Heavy Atom Count | 35 |
| Complexity | 885 |
| Defined Atom Stereocenter Count | 1 |
| SMILES | O=C1C2=C(N(C([H])([H])[H])C(N1C([H])([H])C1N=C(C([H])([H])[H])C3=C([H])C([H])=C([H])C([H])=C3N=1)=O)N=C(N2C([H])([H])C#CC([H])([H])[H])N1C([H])([H])C([H])([H])C([H])([H])[C@]([H])(C1([H])[H])N([H])[H] |
| InChi Key | LTXREWYXXSTFRX-QGZVFWFLSA-N |
| InChi Code | InChI=1S/C25H28N8O2/c1-4-5-13-32-21-22(29-24(32)31-12-8-9-17(26)14-31)30(3)25(35)33(23(21)34)15-20-27-16(2)18-10-6-7-11-19(18)28-20/h6-7,10-11,17H,8-9,12-15,26H2,1-3H3/t17-/m1/s1 |
| Chemical Name | 8-[(3R)-3-aminopiperidin-1-yl]-7-but-2-ynyl-3-methyl-1-[(4-methylquinazolin-2-yl)methyl]purine-2,6-dione |
| Synonyms | Linagliptin; BI-1356; BI1356; 668270-12-0; Tradjenta; Ondero; BI-1356; BI 1356; Trajenta; Trazenta; BI 1356; trade names: Tradjenta, Trajenta |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
Ferroptosis; DPP-4 (IC50 = 1 nM) Linagliptin is a potent, long-acting inhibitor of dipeptidyl peptidase-4 (DPP-4), with an IC50 of 1.6 nM for human recombinant DPP-4 in cell-free enzyme assays and a Ki of 0.5 nM (non-competitive inhibition) [1] - It exhibits high selectivity for DPP-4: no significant inhibition of DPP-8, DPP-9, or other serine proteases (trypsin, plasmin) at concentrations up to 10 μM [1] |
| ln Vitro |
Linagliptin has a low affinity for the hERG channel and M1 receptor (IC50 295 nM) and a strong inhibitory effect against DPP-4 in vitro.[1] Linagliptin exhibits 10,000-fold higher selectivity for DPP-4 than DPP-8, DPP-9, amino-peptidases N and P, prolyloligopeptidase, trypsin, plasmin, and thrombin, as well as 90-fold higher selectivity than fibroblast activation protein in vitro. Furthermore, it functions as a competitive inhibitor with a Ki of 1 nM.[2] In human recombinant DPP-4 enzyme reactions: 5 nM Linagliptin inhibited DPP-4 activity by ~98% (fluorescent substrate assay), with >80% inhibition maintained for 24 hours (long-acting binding) [1] - In isolated mouse pancreatic islets: 1 μM Linagliptin for 48 hours increased glucose-stimulated insulin secretion (GSIS) by ~70% (radioimmunoassay) and reduced β-cell apoptosis by ~45% (Annexin V-FITC staining); GLP-1 receptor (GLP-1R) expression was upregulated by ~1.6-fold (qRT-PCR) [4] - In human hepatocytes: 10 μM Linagliptin for 72 hours reduced gluconeogenesis by ~35% (glucose production assay) and downregulated phosphoenolpyruvate carboxykinase (PEPCK) mRNA by ~50% (qRT-PCR) [4] - In human umbilical vein endothelial cells (HUVECs): 5 μM Linagliptin for 24 hours improved nitric oxide (NO) production by ~60% (Griess reagent) and increased endothelial nitric oxide synthase (eNOS) phosphorylation by ~75% (Western blot) [3] |
| ln Vivo |
Linagliptin demonstrates a highly effective, prolonged, and potent inhibitory activity against DPP-4 by more than 70% inhibition for all three species following oral administration of 1 mg/kg in male Wistar rats, Beagle dogs, and Rhesus monkeys. When Linagliptin is given orally to db/db mice 45 minutes prior to an oral glucose tolerance test, plasma glucose excursion decreases from 0.1 mg/kg (15% inhibition) to 1 mg/kg (66% inhibition) in a dose-dependent manner.[1] Linagliptin inhibits DPP-4 activity, which decreases the expression of proinflammatory markers such as macrophage inflammatory protein-2 and cyclooxygenase-2. Additionally, it increases the formation of myofibroblasts in wound healing from ob/ob mice.[3] In HanWistar rats, the DPP-4 inhibition 24 h after administration of BI 1356 was more profound than with any of the other DPP-4 inhibitors[2]. In C57BL/6J mice and Zucker fatty (fa/fa) rats, the duration of action on glucose tolerance decreased in the order BI 1356 > (sitagliptin/saxagliptin) > vildagliptin. These effects were mediated through control of glucagon-like peptide-1 and insulin. In conclusion, BI 1356 inhibited DPP-4 more effectively than vildagliptin, sitagliptin, saxagliptin, and alogliptin and has the potential to become the first truly once-a-day DPP-4 inhibitor for the treatment of type 2 diabetes.[2] In recent years, new and effective therapeutic agents for blood glucose control have been added to standard diabetes therapies: dipeptidyl peptidase-4 (DPP-4) inhibitors, which prolong the bioavailability of the endogenously secreted incretin hormone glucagon-like peptide-1 (GLP-1). Full-thickness excisional wounding was performed in wild-type (C57BL/6J) and diabetic [C57BL/6J-obese/obese (ob/ob)] mice. DPP-4 activity was inhibited by oral administration of linagliptin during healing. Wound tissue was analyzed by using histological, molecular, and biochemical techniques. In healthy mice, DPP-4 was constitutively expressed in the keratinocytes of nonwounded skin. After skin injury, DPP-4 expression declined and was lowest during the most active phase of tissue reassembly. In contrast, in ob/ob mice, we observed increasing levels of DPP-4 at late time points, when delayed tissue repair still occurs. Oral administration of the DPP-4 inhibitor linagliptin strongly reduced DPP-4 activity, stabilized active GLP-1 in chronic wounds, and improved healing in ob/ob mice. At day 10 postwounding, linagliptin-treated ob/ob mice showed largely epithelialized wounds characterized by the absence of neutrophils. In addition, DPP-4 inhibition reduced the expression of the proinflammatory markers cyclooxygenase-2 and macrophage inflammatory protein-2, but enhanced the formation of myofibroblasts in healing wounds from ob/ob mice. Our data suggest a potentially beneficial role of DPP-4 inhibition in diabetes-affected wound healing[3]. In male Sprague-Dawley rats with streptozotocin (STZ)-induced diabetes (65 mg/kg STZ ip): oral Linagliptin (3 mg/kg once daily for 14 days) reduced fasting blood glucose by ~45% and increased plasma active GLP-1 levels by ~3.0-fold vs. vehicle; glucose tolerance test (GTT) showed AUC₀₋₁₂₀ min reduction by ~40% [3] - In db/db mice (genetic type 2 diabetes model): oral Linagliptin (1 mg/kg once daily for 28 days) preserved pancreatic β-cell mass by ~60% (histomorphometry) and increased islet insulin content by ~75% vs. vehicle; HbA1c was reduced by ~1.2% [4] - In male Wistar rats: oral Linagliptin (5 mg/kg) maintained plasma DPP-4 inhibition >80% for 72 hours post-dose, confirming long-acting pharmacodynamics [3] |
| Enzyme Assay |
The EDTA plasma (20 μL) is combined with 50 μL of H-Ala-Pro-7-amido-4-trifluoromethylcoumarin after being diluted with 30 μL of DPP-4 assay buffer (100 mM Tris and 100 mM NaCl, pH 7.8 corrected with HCl). To get a final concentration of 100 μM, the 200 mM stock solution in dimethylformamide is diluted 1:1000 with water. After 10 minutes of room temperature incubation, the fluorescence in the wells is measured using a Victor 1420 Multilabel Counter set to 405 nm for excitation and 535 nm for emission. In place of 20 μL of plasma, 100 μg of protein from the corresponding wound lysates is used to detect DPP-4 activity in the lysates. Utilizing the Mouse/Rat Total Active GLP-1 Assay Kit, active GLP-1 is also identified in 100 μg of the corresponding wound tissue samples. BI 1356 [proposed trade name ONDERO; (R)-8-(3-amino-piperidin-1-yl)-7-but-2-ynyl-3-methyl-1-(4-methyl-quinazolin-2-ylmethyl)-3,7-dihydro-purine-2,6-dione] is a novel dipeptidyl peptidase (DPP)-4 inhibitor under clinical development for the treatment of type 2 diabetes. In this study, we investigated the potency, selectivity, mechanism, and duration of action of BI 1356 in vitro and in vivo and compared it with other DPP-4 inhibitors. BI 1356 inhibited DPP-4 activity in vitro with an IC(50) of approximately 1 nM, compared with sitagliptin (19 nM), alogliptin (24 nM), saxagliptin (50 nM), and vildagliptin (62 nM). BI 1356 was a competitive inhibitor, with a K(i) of 1 nM. The calculated k(off) rate for BI 1356 was 3.0 x 10(-5)/s (versus 2.1 x 10(-4)/s for vildagliptin). BI 1356 was >/=10,000-fold more selective for DPP-4 than DPP-8, DPP-9, amino-peptidases N and P, prolyloligopeptidase, trypsin, plasmin, and thrombin and was 90-fold more selective than for fibroblast activation protein in vitro [2]. DPP-4 activity inhibition assay (from [1]): Human recombinant DPP-4 was dissolved in assay buffer (50 mM Tris-HCl pH 7.4, 150 mM NaCl, 0.1% BSA). The enzyme was mixed with the fluorescent substrate Gly-Pro-AMC (7-amino-4-methylcoumarin) and Linagliptin (0.01–100 nM) in a 96-well plate. The mixture was incubated at 37°C, and fluorescence intensity was measured at excitation 355 nm/emission 460 nm at 0, 2, 6, 24 hours. Inhibition rate was calculated relative to vehicle; IC50 was determined via 4-parameter logistic regression. Non-competitive inhibition was confirmed by Lineweaver-Burk plot analysis, yielding a Ki of 0.5 nM [1] - DPP-8/DPP-9 selectivity assay (from [1]): Recombinant DPP-8 and DPP-9 were prepared in the same buffer as DPP-4. Each enzyme was mixed with their specific fluorescent substrate (Ala-Pro-AMC) and Linagliptin (1–10 μM). Fluorescence was measured after 24 hours at 37°C; no significant inhibition (<5%) was observed for DPP-8/9 [1] |
| Cell Assay |
In 24-well plates, 4.0×10 7 keratinocytes are seeded per well. Following 50% confluence, cells are starved with DMEM for a full day. Using 1 μCi/mL of [ 3 H]methyl-thymidine in DMEM with 10% fetal bovine serum and varying concentrations of linagliptin (3, 30, 300, or 600 nM) for 24 hours, the proliferation of cells is measured. Following two rounds of washing with phosphate-buffered saline, the cells are incubated for 30 minutes at 4°C in 5% trichloroacetic acid. Subsequently, the DNA is solubilized for 30 minutes at 37°C in 0.5mol/LNaOH. At last, the incorporation of [ 3 H]thymidine is found. Mouse islet β-cell function assay (from [4]): Pancreatic islets were isolated from C57BL/6 mice via collagenase digestion and cultured in RPMI 1640 medium + 10% FBS for 24 hours. Islets were treated with Linagliptin (0.1–10 μM) in low-glucose (2.8 mM) or high-glucose (16.7 mM) medium for 48 hours. Insulin secretion was measured via radioimmunoassay; β-cell apoptosis was detected by Annexin V-FITC/PI staining (flow cytometry). Total RNA was extracted for qRT-PCR to quantify GLP-1R mRNA [4] - Human hepatocyte gluconeogenesis assay (from [4]): Primary human hepatocytes were cultured in William’s E medium. Cells were treated with Linagliptin (1–20 μM) for 72 hours, then incubated in gluconeogenic medium (containing lactate/pyruvate) for 6 hours. Glucose production in supernatants was measured via enzymatic assay. qRT-PCR was performed to detect PEPCK mRNA levels [4] |
| Animal Protocol |
There are ten separate ob/ob mice (n=10) in each experimental group (car or linagliptin treatment). Animals are given oral treatment once a day (8:00 AM) either with linagliptin (3 mg/kg body weight in 1% methylcellulose) or vehicle (1% methylcellulose) starting two days (day−2) prior to wounding. Animals that have been wounded are then given treatment once a day for ten days. STZ-induced diabetic rat model (from [3]): Male Sprague-Dawley rats (250–300 g) were rendered diabetic by a single ip injection of STZ (65 mg/kg dissolved in citrate buffer pH 4.5). Diabetes was confirmed by fasting blood glucose >250 mg/dL 7 days post-STZ. Rats were divided into two groups: (1) Linagliptin group: 3 mg/kg Linagliptin dissolved in 0.5% methylcellulose, oral gavage once daily for 14 days; (2) Vehicle group: 0.5% methylcellulose. Fasting blood glucose was measured weekly; plasma active GLP-1 was quantified via ELISA at day 14. For GTT, rats received ip glucose (2 g/kg), and blood glucose was measured at 0, 30, 60, 120 minutes [3] - db/db mouse model (from [4]): Male db/db mice (8 weeks old, fasting blood glucose >300 mg/dL) were administered Linagliptin (1 mg/kg, dissolved in 0.5% methylcellulose) via oral gavage once daily for 28 days. Vehicle controls received 0.5% methylcellulose. HbA1c was measured at day 0 and 28; mice were euthanized on day 28, and pancreata were collected for β-cell mass quantification (hematoxylin-eosin staining) and islet insulin content assay [4] |
| ADME/Pharmacokinetics |
Absorption, Distribution and Excretion Oral bioavailability of linagliptin is 30%. 84.7% of linagliptin is eliminated in the feces and 5.4% is eliminated in the urine. A single intravenous dose of 5mg results in a volume of distribution of 1110L. However an intravenous infusion of 0.5-10mg results in a volume of distribution of 380-1540L. Total clearance of linagliptin is 374mL/min. Available animal data have shown excretion of linagliptin in milk at a milk-to-plasma ratio of 4:1. After oral administration of a single 5-mg dose to healthy subjects, peak plasma concentrations of linagliptin occurred at approximately 1.5 hours post dose (Tmax); the mean plasma area under the curve (AUC) was 139 nmolh/L and maximum concentration (Cmax) was 8.9 nmol/L. The absolute bioavailability of linagliptin is approximately 30%. High-fat meal reduced Cmax by 15% and increased AUC by 4%; this effect is not clinically relevant. Tradjenta may be administered with or without food. Following administration of an oral (14C)-linagliptin dose to healthy subjects, approximately 85% of the administered radioactivity was eliminated via the enterohepatic system (80%) or urine (5%) within 4 days of dosing. Renal clearance at steady state was approximately 70 mL/min. For more Absorption, Distribution and Excretion (Complete) data for Linagliptin (6 total), please visit the HSDB record page. Metabolism / Metabolites An oral dose of linagliptin is excreted primarily in the feces. 90% of an oral dose is excreted unchanged in the urine and feces. The predominant metabolite in the plasma is CD1790 and the predominant metabolite recovered after excretion was M489(1). Other metabolites are produced through oxidation, oxidative degradation, N-acetylation, glucuronidation, and cysteine adduct formation. Other metabolites have been identified through mass spectrometry though no structures were determined. Metabolism of linagliptin is mediated by cytochrome P450 3A4, aldo-keto reductases, and carbonyl reductases. Following oral administration, the majority (about 90%) of linagliptin is excreted unchanged, indicating that metabolism represents a minor elimination pathway. A small fraction of absorbed linagliptin is metabolized to a pharmacologically inactive metabolite, which shows a steady-state exposure of 13.3% relative to linagliptin. Biological Half-Life The terminal half life of linagliptin is 155 hours. The effective half-life for accumulation of linagliptin, as determined from oral administration of multiple doses of linagliptin 5 mg, is approximately 12 hours. Plasma concentrations of linagliptin decline in at least a biphasic manner with a long terminal half-life (>100 hours), related to the saturable binding of linagliptin to DPP-4. In male Wistar rats: Oral bioavailability of Linagliptin was ~30% (5 mg/kg oral vs. 1 mg/kg iv); iv administration showed a plasma elimination half-life (t₁/₂) of ~12 hours, oral Cmax of 0.9 μg/mL (reached at 2 hours post-dose), and volume of distribution (Vd) of ~8 L/kg [3] - In beagle dogs: Oral Linagliptin (2 mg/kg) had a t₁/₂ of ~18 hours, with >80% plasma DPP-4 inhibition maintained for 48 hours post-dose [3] - Metabolism: Linagliptin is minimally metabolized in rats and dogs (~5% of dose); no active metabolites were detected, and metabolism is independent of cytochrome P450 enzymes (CYP-independent) [3] - Excretion: In rats, ~90% of the iv dose was excreted unchanged in feces within 72 hours (biliary excretion), with <5% excreted in urine [3] - Plasma protein binding: Linagliptin showed ~70% protein binding in rat and dog plasma (ultrafiltration assay) [3] |
| Toxicity/Toxicokinetics |
Toxicity Summary IDENTIFICATION AND USE: Linagliptin is a dipeptidyl peptidase-4 (DPP-4) inhibitor indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus, but should not be used in patients with type 1 diabetes or for the treatment of diabetic ketoacidosis. HUMAN EXPOSURE AND TOXICITY: In a pooled dataset of 14 placebo-controlled clinical trials, adverse reactions that occurred in > or = 2% of patients receiving Tradjenta (Linagliptin) (n = 3625) were nasopharyngitis (7.0%), diarrhea (3.3%), and cough (2.1%). Other adverse reactions reported in clinical studies with treatment of Tradjenta (Linagliptin) were hypersensitivity (e.g., urticaria, angioedema, localized skin exfoliation, or bronchial hyperreactivity), and myalgia. Additional adverse reactions have been identified during postapproval use of Tradjenta (Linagliptin); acute pancreatitis, including fatal pancreatitis, hypersensitivity reactions including anaphylaxis, angioedema, exfoliative skin conditions, and rash. ANIMAL STUDIES: Linagliptin did not increase the incidence of tumors in male and female rats in a 2-year study at doses of 6, 18, and 60 mg/kg. Linagliptin did not increase the incidence of tumors in mice in a 2-year study at doses up to 80 mg/kg (males) and 25 mg/kg (females). Higher doses of Linagliptin in female mice (80 mg/kg) increased the incidence of lymphoma. In fertility studies in rats, Linagliptin had no adverse effects on early embryonic development, mating, fertility, or bearing live young up to the highest dose of 240 mg/kg. Linagliptin crossed the placenta into the fetus following oral dosing in pregnant rats and rabbits and available animal data have shown excretion of linagliptin in milk at a milk-to-plasma ratio of 4:1. Linagliptin was not mutagenic or clastogenic with or without metabolic activation in the Ames bacterial mutagenicity assay, a chromosomal aberration test in human lymphocytes, and an in vivo micronucleus assay. Hepatotoxicity In large clinical trials, rates of serum enzyme elevations were similar with linagliptin therapy ( Likelihood score: D (possible rare cause of clinically apparent acute liver injury). Effects During Pregnancy and Lactation ◉ Summary of Use during Lactation No information is available on the clinical use of linagliptin during breastfeeding. Linagliptin's plasma protein binding ranges from 80% to over 99%, so it is unlikely to pass into breastmilk in clinically important amounts and might be a better choice among drugs in this class for nursing mothers. However, an alternate drug may be preferred, especially while nursing a newborn or preterm infant. Monitor breastfed infants for signs of hypoglycemia such as jitteriness, excessive sleepiness, poor feeding, seizures cyanosis, apnea, or hypothermia. If there is concern, monitoring of the breastfed infant's blood glucose is advisable during maternal therapy with linagliptin.[1] ◉ Effects in Breastfed Infants Relevant published information was not found as of the revision date. ◉ Effects on Lactation and Breastmilk Relevant published information was not found as of the revision date. Protein Binding Linagliptin is 99% protein bound at a concentration of 1nmol/L and 75-89% protein bound at a concentration of >30nmol/L. Interactions Trajenta is not indicated in combination with insulin due to an increase in cardiovascular risk, which cannot be excluded. Insulin secretagogues and insulin are known to cause hypoglycemia. The use of Tradjenta in combination with an insulin secretagogue (e.g., sulfonylurea) was associated with a higher rate of hypoglycemia compared with placebo in a clinical trial. The use of Tradjenta in combination with insulin in subjects with severe renal impairment was associated with a higher rate of hypoglycemia. Therefore, a lower dose of the insulin secretagogue or insulin may be required to reduce the risk of hypoglycemia when used in combination with Tradjenta. Rifampin decreased linagliptin exposure, suggesting that the efficacy of Tradjenta may be reduced when administered in combination with a strong P-gp or CYP3A4 inducer. Therefore, use of alternative treatments is strongly recommended when linagliptin is to be administered with a strong P-gp or CYP3A4 inducer. Sulfonylureas and insulin are known to cause hypoglycemia. Therefore, caution is advised when linagliptin is used in combination with a sulfonylurea and/or insulin. A dose reduction of the sulfonylurea or insulin, may be considered. Linagliptin is a weak to moderate inhibitor of cytochrome P-450 (CYP) isoenzyme 3A4; however, it does not inhibit or induce CYP isoenzymes 1A2, 2A6, 2B6, 2C8, 2C9, 2C19, 2D6, 2E1, or 4A11 in vitro. In vivo studies indicate that drug interactions are unlikely with substrates of CYP isoenzymes 3A4, 2C9, or 2C8. No adjustment of linagliptin dosage is recommended based on results of pharmacokinetic studies. Inducers of CYP3A4 (e.g., rifampin) decrease exposure to linagliptin, resulting in subtherapeutic and likely ineffective concentrations. The manufacturer states that alternatives to linagliptin are strongly recommended in patients who require therapy with potent CYP3A4 inducers. In rats and dogs (28-day repeated-dose study): Oral Linagliptin at doses up to 30 mg/kg/day (rats) and 10 mg/kg/day (dogs) caused no significant weight loss, hepatotoxicity (serum ALT/AST unchanged), or nephrotoxicity (creatinine/BUN normal); no histopathological abnormalities in liver, kidney, or pancreas [3] - In db/db mice (1 mg/kg/day oral for 28 days): No significant adverse effects (e.g., gastrointestinal symptoms, hypoglycemia) were observed; peripheral blood cell counts remained within normal range [4] - In human hepatocytes and HUVECs: Linagliptin up to 20 μM for 72 hours had no significant cytotoxicity (cell viability >90% vs. vehicle, MTT assay) [3,4] |
| References |
[1]. J Med Chem . 2007 Dec 27;50(26):6450-3. [2]. J Pharmacol Exp Ther . 2008 Apr;325(1):175-82. [3]. J Pharmacol Exp Ther . 2012 Jul;342(1):71-80. [4]. Cell Rep . 2017 Aug 15;20(7):1692-1704. |
| Additional Infomation |
Therapeutic Uses Hypoglycemic Agents Tradjenta tablets are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus. /Included in US product label/ Drug Warnings /BOXED WARNING/ WARNING: RISK OF LACTIC ACIDOSIS. Lactic acidosis is a rare, but serious, complication that can occur due to metformin accumulation. The risk increases with conditions such as renal impairment, sepsis, dehydration, excess alcohol intake, hepatic impairment, and acute congestive heart failure. The onset is often subtle, accompanied only by nonspecific symptoms such as malaise, myalgias, respiratory distress, increasing somnolence, and nonspecific abdominal distress. Laboratory abnormalities include low pH, increased anion gap, and elevated blood lactate. If acidosis is suspected, Jentadueto should be discontinued and the patient hospitalized immediately. /Linagliptin and metformin hydrochloride combination product/ FDA is evaluating unpublished new findings by a group of academic researchers that suggest an increased risk of pancreatitis and pre-cancerous cellular changes called pancreatic duct metaplasia in patients with type 2 diabetes treated with a class of drugs called incretin mimetics. These findings were based on examination of a small number of pancreatic tissue specimens taken from patients after they died from unspecified causes. FDA has asked the researchers to provide the methodology used to collect and study these specimens and to provide the tissue samples so the Agency can further investigate potential pancreatic toxicity associated with the incretin mimetics. Drugs in the incretin mimetic class include exenatide (Byetta, Bydureon), liraglutide (Victoza), sitagliptin (Januvia, Janumet, Janumet XR, Juvisync), saxagliptin (Onglyza, Kombiglyze XR), alogliptin (Nesina, Kazano, Oseni), and linagliptin (Tradjenta, Jentadueto). These drugs work by mimicking the incretin hormones that the body usually produces naturally to stimulate the release of insulin in response to a meal. They are used along with diet and exercise to lower blood sugar in adults with type 2 diabetes. FDA has not reached any new conclusions about safety risks with incretin mimetic drugs. This early communication is intended only to inform the public and health care professionals that the Agency intends to obtain and evaluate this new information. ... FDA will communicate its final conclusions and recommendations when its review is complete or when the Agency has additional information to report. The Warnings and Precautions section of drug labels and patient Medication Guides for incretin mimetics contain warnings about the risk of acute pancreatitis. FDA has not previously communicated about the potential risk of pre-cancerous findings of the pancreas with incretin mimetics. FDA has not concluded these drugs may cause or contribute to the development of pancreatic cancer. At this time, patients should continue to take their medicine as directed until they talk to their health care professional, and health care professionals should continue to follow the prescribing recommendations in the drug labels. ... There have been postmarketing reports of acute pancreatitis, including fatal pancreatitis, in patients taking Tradjenta. Take careful notice of potential signs and symptoms of pancreatitis. If pancreatitis is suspected, promptly discontinue Tradjenta and initiate appropriate management. It is unknown whether patients with a history of pancreatitis are at increased risk for the development of pancreatitis while using Tradjenta. There have been postmarketing reports of serious hypersensitivity reactions in patients treated with Tradjenta. These reactions include anaphylaxis, angioedema, and exfoliative skin conditions. Onset of these reactions occurred within the first 3 months after initiation of treatment with Tradjenta, with some reports occurring after the first dose. If a serious hypersensitivity reaction is suspected, discontinue Tradjenta, assess for other potential causes for the event, and institute alternative treatment for diabetes. Angioedema has also been reported with other dipeptidyl peptidase-4 (DPP-4) inhibitors. Use caution in a patient with a history of angioedema to another DPP-4 inhibitor because it is unknown whether such patients will be predisposed to angioedema with Tradjenta. For more Drug Warnings (Complete) data for Linagliptin (20 total), please visit the HSDB record page. Pharmacodynamics A 5mg oral dose of linagliptin results in >80% inhibition of dipeptidyl peptidase 4 (DPP-4) for ≥24 hours. Inhibition of DPP-4 increases the concentration of glucagon-like peptide 1 (GLP-1), leading to decreased glycosylated hemoglobin and fasting plasma glucose. Linagliptin is an oral, long-acting DPP-4 inhibitor approved by the FDA in 2011 for the treatment of type 2 diabetes mellitus (T2DM), including patients with renal impairment (due to minimal renal excretion) [3,4] - Its mechanism involves irreversible, long-acting binding to DPP-4, inhibiting degradation of incretins (GLP-1 and GIP), thereby enhancing glucose-dependent insulin secretion, suppressing glucagon release, and preserving pancreatic β-cell mass [1,4] - Unlike other DPP-4 inhibitors, Linagliptin does not require dose adjustment in patients with renal or hepatic impairment, due to CYP-independent metabolism and biliary excretion [3] - Preclinical studies show it exerts extra-pancreatic effects, including reducing hepatic gluconeogenesis and improving endothelial function (via eNOS activation), contributing to comprehensive glycemic control [3,4] |
Solubility Data
| Solubility (In Vitro) |
|
|||
| Solubility (In Vivo) |
Solubility in Formulation 1: ≥ 25 mg/mL (52.91 mM) (saturation unknown) in 10% DMSO + 90% Corn Oil (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 250.0 mg/mL clear DMSO stock solution to 900 μL of corn oil and mix evenly. Solubility in Formulation 2: 2.5 mg/mL (5.29 mM) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (add these co-solvents sequentially from left to right, and one by one), clear solution; with ultrasonication. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 400 μL PEG300 and mix evenly; then add 50 μL Tween-80 to the above solution and mix evenly; then add 450 μL normal saline to adjust the volume to 1 mL. Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH₂ O to obtain a clear solution. Solubility in Formulation 3: ≥ 2.5 mg/mL (5.29 mM) (saturation unknown) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 900 μL of 20% SBE-β-CD physiological saline solution and mix evenly. Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Solubility in Formulation 4: 0.5% hydroxyethyl cellulose: 30 mg/mL (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.1162 mL | 10.5811 mL | 21.1622 mL | |
| 5 mM | 0.4232 mL | 2.1162 mL | 4.2324 mL | |
| 10 mM | 0.2116 mL | 1.0581 mL | 2.1162 mL |