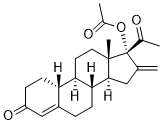
Segesterone acetate (formerly known as ST1435; ST-1435 or nestorone; trade name: Annovera) is a progesterone receptor agonist that is prescribed as a female contraceptive. In August 2018, the FDA approved a novel vaginal ring system that uses estradiol and semen to prevent pregnancy for a full year. Segesterone inhibits proinflammatory mediators and neuropathology in the wobbler mouse model of motoneuron degeneration as a female-contraceptive drug. Segesterone may have benefits for multiple sclerosis (MS) as it prevented hippocampal abnormalities and enhanced the functional outcomes of EAE mice.
Physicochemical Properties
| Molecular Formula | C23H30O4 | |
| Molecular Weight | 370.49 | |
| Exact Mass | 370.214 | |
| Elemental Analysis | C, 74.56; H, 8.16; O, 17.27 | |
| CAS # | 7759-35-5 | |
| Related CAS # | 7690-08-6;7759-35-5 (acetate); | |
| PubChem CID | 108059 | |
| Appearance | White to off-white solid powder | |
| Density | 1.15g/cm3 | |
| Boiling Point | 499.3ºC at 760mmHg | |
| Melting Point | 173-177 | |
| Flash Point | 216.2ºC | |
| Index of Refraction | 1.549 | |
| LogP | 4.185 | |
| Hydrogen Bond Donor Count | 0 | |
| Hydrogen Bond Acceptor Count | 4 | |
| Rotatable Bond Count | 3 | |
| Heavy Atom Count | 27 | |
| Complexity | 762 | |
| Defined Atom Stereocenter Count | 6 | |
| SMILES | CC([C@]1(OC(C)=O)[C@@]2([C@]([H])([C@@]3(CCC4=CC(CC[C@@]4([C@]3(CC2)[H])[H])=O)[H])CC1=C)C)=O |
|
| InChi Key | CKFBRGLGTWAVLG-GOMYTPFNSA-N | |
| InChi Code | InChI=1S/C23H30O4/c1-13-11-21-20-7-5-16-12-17(26)6-8-18(16)19(20)9-10-22(21,4)23(13,14(2)24)27-15(3)25/h12,18-21H,1,5-11H2,2-4H3/t18-,19+,20+,21-,22-,23-/m0/s1 | |
| Chemical Name | [(8R,9S,10R,13S,14S,17R)-17-acetyl-13-methyl-16-methylidene-3-oxo-2,6,7,8,9,10,11,12,14,15-decahydro-1H-cyclopenta[a]phenanthren-17-yl] acetate | |
| Synonyms |
|
|
| HS Tariff Code | 2934.99.9001 | |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
|
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
progesterone receptor (EC50 = 50.3 nM) |
| ln Vitro |
Segesterone acetate (Nestorone) (20 µM) promotes remyelination of axons by oligodendrocytes after lysolecithin-induced demyelination in organotypic cultures of cerebellar slices from postnatal rats or mice, as shown by increased myelin basic protein (MBP) immunostaining and Western blot analysis. Segesterone acetate (Nestorone) increases the number of oligodendroglial lineage cells (PLP-EGFP⁺ cells) in demyelinated cerebellar slices. Segesterone acetate (Nestorone) enhances the recruitment of NG2⁺ and Olig2⁺ oligodendrocyte progenitor cells (OPCs) and stimulates their differentiation into mature oligodendrocytes. Segesterone acetate (Nestorone) stimulates the migration of OPCs from brain stem slices into demyelinated cerebellar slices in a coculture system, increasing both the number of migrating EGFP⁺ cells and their migration distance. The proremyelinating effects of Segesterone acetate (Nestorone) are not observed in cerebellar slices from progesterone receptor knockout (PRKO) mice, indicating that its actions are mediated through PR.[2] |
| ln Vivo |
Following Segesterone acetate (400 μCi 3H Nestoron/kg BW; subcutaneous injection; female Sprague-Dawley rats) treatment, the Cmax in plasma and blood is 95.5 and 58.1 ng equiv. 3H Nestoron/g, respectively, with a t1/2 of 15.6 hours. Feces and urine excrete about 81.4% and 7.62% of the dose that was administered, respectively[1]. The study describes the distribution, metabolism, and excretion of Segesterone acetate (Nestorone) following subcutaneous administration in adult female rats. The results are primarily pharmacokinetic and metabolic in nature, not focused on in vivo efficacy or mechanism of action for a therapeutic indication (e.g., contraceptive efficacy).[1] |
| Cell Assay |
Organotypic cerebellar slice cultures were prepared from postnatal day 10 (P10) rats or mice. Slices (350 µm thick) were cultured on microporous membranes in a medium composed of basal medium, Hanks' balanced salt solution, horse serum, L-glutamine, and glucose. After 7 days in vitro (DIV), demyelination was induced by treating slices with lysolecithin (0.5 mg/ml) for approximately 17 hours. The lysolecithin-containing medium was then removed, and slices were incubated for an additional 4 days in medium containing 20 µM Segesterone acetate (Nestorone), progesterone, medroxyprogesterone acetate (MPA), or vehicle control (0.01% ethanol). The medium was replaced once after 2 days. For coculture experiments, lysolecithin-treated P10 cerebellar slices were transected and apposed to brain stem slices from P0 transgenic mice expressing enhanced green fluorescent protein (EGFP) under the proteolipid gene promoter (PLP-EGFP mice). Cocultures were treated with 20 µM Segesterone acetate (Nestorone) or vehicle for 4 days (medium replaced after 2 days) and analyzed after 10 days for OPC migration. Immunohistochemistry was performed using antibodies against myelin basic protein (MBP), NG2 proteoglycan, Olig2 transcription factor, and Calbindin (Purkinje cell marker). Stained slices were analyzed by confocal microscopy and fluorescence microscopy. MBP staining intensity, number of PLP-EGFP⁺ cells, NG2⁺ cell density, and OPC migration distance were quantified using image analysis software. Western blot analysis was performed on cerebellar slice extracts after lysolecithin treatment and 3-hour incubation with or without 20 µM Segesterone acetate (Nestorone), probing for MBP expression.[2] |
| ADME/Pharmacokinetics |
Absorption, Distribution and Excretion Contraceptive vaginal rings provided sustained release of contraceptive levels of segesterone acetate over 90 days in a pharmacokinetic study of healthy women. Following vaginal administration for up to 13 cycles, segesterone acetate was absorbed into systemic administration and reached the peak plasma concentration in 2 hours in Cycle 1, Cycle 3, and Cycle 13. Concentrations declined after time to reach plasma concentration (Tmax) and became more constant after 96 hours post-dose.Over subsequent cycles of use, the peak serum concentrations of segesterone acetate decreased. In Cycle 1, 3 and 13, the peak plasma concentrations were 1147, 363, and 294 pg/mL. In a pharmacokinetic study, approximately 81.4% and 7.62% of the subcutaneously-administered dose in rats was excreted via feces and urine, respectively. The volume of distribution of segesterone acetate is 19.6 L/kg. No pharmacokinetic data available. Metabolism / Metabolites Segesterone acetate undergoes rapid metabolism and inactivation in the liver. Based on the findings _in vitro_, the major oxidative metabolites in the serum include 5α-dihydro- and 17α-hydroxy-5α-dihydro metabolites constitute about 50% of exposure relative to segesterone acetate. The metabolites are not pharmacologically active with EC50 to progesterone receptor 10-fold higher than that of the parent compound. It was shown that 3α, 5α-tetrahydrosegesterone acetate acts as an activator at the GABA-A receptors in the brain. Biological Half-Life The mean (SD) half life of segesterone acetate is 4.5 (3.4) hours. Segesterone acetate (Nestorone) is noted to easily cross the blood-brain barrier and rapidly diffuse throughout nervous tissues. It is mentioned that Segesterone acetate (Nestorone) may be rapidly metabolized in the liver, which could explain its lack of glucocorticoid-like effects despite binding to GR with low affinity.[2] |
| Toxicity/Toxicokinetics |
Effects During Pregnancy and Lactation ◉ Summary of Use during Lactation Based on the available evidence, expert opinion in the United States holds that postpartum women who are breastfeeding should not use combined hormonal contraceptives during the first 3 weeks after delivery because of concerns about increased risk for venous thromboembolism and generally should not use combined hormonal contraceptives during the fourth week postpartum because of concerns about potential effects on breastfeeding performance. Postpartum breastfeeding women with other risk factors for venous thromboembolism generally should not use combined hormonal contraceptives until 6 weeks after delivery. World Health Organization guidelines are more restrictive, stating that combined oral contraceptives should not be used in nursing mothers before 42 days postpartum and the disadvantages of using the method generally outweigh the advantages between 6 weeks and 6 months postpartum. A decrease in milk supply can happen over the first few days of estrogen exposure. ◉ Effects in Breastfed Infants Relevant published information on segesterone acetate and ethinyl estradiol vaginal insert was not found as of the revision date. Studies on the use of segesterone acetate implants have found no adverse effects on growth and development. ◉ Effects on Lactation and Breastmilk Relevant published information was not found as of the revision date. Protein Binding Serum protein binding of segesterone acetate is approximately 95% and it displays negligible binding affinity for sex hormone-binding globulin (SHBG). Segesterone acetate (Nestorone) is described as lacking significant androgenic, estrogenic, glucocorticoid-like, or mineralocorticoid-like activities, suggesting a favorable side effect profile in the contexts studied. |
| References |
[1]. Single-dose pharmacokinetics of Nestorone, a potential female-contraceptive.Steroids. 2010 Mar;75(3):252-64. Epub 2010 Jan 11. [2]. Progesterone and Nestorone facilitate axon remyelination: a role for progesterone receptors. Endocrinology. 2011 Oct;152(10):3820-31. |
| Additional Infomation |
Pharmacodynamics Segesterone acetate suppresses ovulation. In a Phase I randomized, placebo-controlled, randomized crossover study involving healthy adult female subjects, there was no clinically significant QTc interval prolongation following a single intravenous bolus dose of segesterone acetate. Segesterone acetate shows no androgenic, anabolic, or estrogenic activity. It also did not show uterotropic activity in ovariectomized rats. In the endometrial transformation test to assess the progestational activity, dose-dependent increases in both uterine weight was observed following subcutaneous administration of segesterone acetate. Segesterone acetate (Nestorone) is a synthetic 19-norprogesterone derivative, also classified as a fourth-generation progestin. It is designed for high selectivity towards the progesterone receptor (PR). In this study, Segesterone acetate (Nestorone) demonstrated potent proremyelinating activity by stimulating OPC recruitment, migration, and differentiation, key steps in myelin repair. This effect was PR-dependent, as it was absent in PR knockout mice. In contrast, another synthetic progestin, medroxyprogesterone acetate (MPA), did not promote remyelination or oligodendrocyte replenishment in the same model. Segesterone acetate (Nestorone) is highlighted as a promising candidate for promoting endogenous myelin repair in demyelinating diseases like multiple sclerosis due to its PR selectivity, neuroprotective potential, and ability to modulate key remyelination processes. The authors note that Segesterone acetate (Nestorone) is undergoing testing as a contraceptive and may have therapeutic applications in both female and male patients. The study was supported by a research grant, and several authors are listed as inventors on a related patent.[2] |
Solubility Data
| Solubility (In Vitro) |
|
|||
| Solubility (In Vivo) |
Solubility in Formulation 1: ≥ 2.5 mg/mL (6.75 mM) (saturation unknown) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 400 μL PEG300 and mix evenly; then add 50 μL Tween-80 to the above solution and mix evenly; then add 450 μL normal saline to adjust the volume to 1 mL. Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH₂ O to obtain a clear solution. Solubility in Formulation 2: ≥ 2.5 mg/mL (6.75 mM) (saturation unknown) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 900 μL of 20% SBE-β-CD physiological saline solution and mix evenly. Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Solubility in Formulation 3: ≥ 2.5 mg/mL (6.75 mM) (saturation unknown) in 10% DMSO + 90% Corn Oil (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 900 μL of corn oil and mix evenly. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.6991 mL | 13.4956 mL | 26.9913 mL | |
| 5 mM | 0.5398 mL | 2.6991 mL | 5.3983 mL | |
| 10 mM | 0.2699 mL | 1.3496 mL | 2.6991 mL |