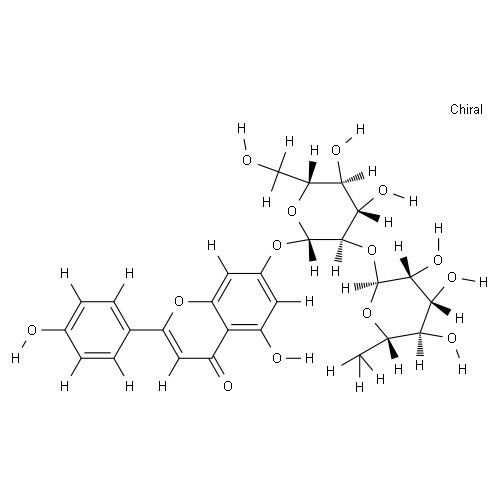
Physicochemical Properties
| Molecular Formula | C₂₇H₃₀O₁₄ |
| Molecular Weight | 578.52 |
| Exact Mass | 578.163 |
| CAS # | 17306-46-6 |
| Related CAS # | 17306-46-6 |
| PubChem CID | 5282150 |
| Appearance | Light yellow to yellow solid |
| Density | 1.7±0.1 g/cm3 |
| Boiling Point | 916.5±65.0 °C at 760 mmHg |
| Flash Point | 305.4±27.8 °C |
| Vapour Pressure | 0.0±0.3 mmHg at 25°C |
| Index of Refraction | 1.726 |
| LogP | 1.72 |
| Hydrogen Bond Donor Count | 8 |
| Hydrogen Bond Acceptor Count | 14 |
| Rotatable Bond Count | 6 |
| Heavy Atom Count | 41 |
| Complexity | 939 |
| Defined Atom Stereocenter Count | 10 |
| SMILES | O([C@@]1([H])[C@@]([H])([C@@]([H])([C@]([H])([C@]([H])(C([H])([H])[H])O1)O[H])O[H])O[H])[C@@]1([H])[C@]([H])(OC2=C([H])C(=C3C(C([H])=C(C4C([H])=C([H])C(=C([H])C=4[H])O[H])OC3=C2[H])=O)O[H])O[C@]([H])(C([H])([H])O[H])[C@]([H])([C@]1([H])O[H])O[H] |
| InChi Key | RPMNUQRUHXIGHK-PYXJVEIZSA-N |
| InChi Code | InChI=1S/C27H30O14/c1-10-20(32)22(34)24(36)26(37-10)41-25-23(35)21(33)18(9-28)40-27(25)38-13-6-14(30)19-15(31)8-16(39-17(19)7-13)11-2-4-12(29)5-3-11/h2-8,10,18,20-30,32-36H,9H2,1H3/t10-,18+,20-,21+,22+,23-,24+,25+,26-,27+/m0/s1 |
| Chemical Name | 7-[(2S,3R,4S,5S,6R)-4,5-dihydroxy-6-(hydroxymethyl)-3-[(2S,3R,4R,5R,6S)-3,4,5-trihydroxy-6-methyloxan-2-yl]oxyoxan-2-yl]oxy-5-hydroxy-2-(4-hydroxyphenyl)chromen-4-one |
| Synonyms | NSC-649413; NSC 649413; NSC649413; Rhoifolin |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month Note: (1). This product requires protection from light (avoid light exposure) during transportation and storage.(2). Please store this product in a sealed and protected environment (e.g. under nitrogen), avoid exposure to moisture. |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
insulin receptor-β; GLUT4; NF-κB; MAPK Rhoifolin exhibits toxic activity against various E. coli cell lines, which in MRC-5, HCT, HepG2, HeLa, and Hep2 are 77.0 nM, 60.1 nM, 39.0 nM, 10.7 nM, and 10.1 nM, respectively [3]. |
| ln Vitro |
Rhoifolin exhibits toxic activity against various E. coli cell lines, which in MRC-5, HCT, HepG2, HeLa, and Hep2 are 77.0 nM, 60.1 nM, 39.0 nM, 10.7 nM, and 10.1 nM, respectively [3]. In differentiated 3T3-L1 adipocytes, rhoifolin exhibited insulin-mimetic activities. It dose-dependently (0.001–5 µM) enhanced adiponectin secretion. The maximal stimulatory response was observed at 0.5 µM, increasing adiponectin level by 1.7-fold compared to control, a response similar to that of 10 nM insulin. Concentrations of 1 µM and 5 µM showed similar efficacy to 0.5 µM. Rhoifolin also enhanced tyrosine phosphorylation of the insulin receptor-β subunit (pIR-β) in a dose-dependent manner (0.5–5 µM). At 0.5 µM, 1 µM, and 5 µM, it enhanced pIR-β levels by 1.1-, 1.6-, and 3.9-fold, respectively. The response at 5 µM was similar to that of 10 nM insulin. Furthermore, rhoifolin (at 0.5 µM, 1 µM, and 5 µM) facilitated the translocation of the glucose transporter GLUT4 from intracellular compartments to the plasma membrane in 3T3-L1 adipocytes, similar to the effect of insulin. Concentrations of 0.01 µM and 0.1 µM did not induce significant GLUT4 translocation. [1] Rhoifolin strongly suppressed RANKL-stimulated osteoclast differentiation from bone marrow macrophages (BMMs) in a dose-dependent manner (2.5, 5, 10, 20 µM). It significantly reduced the number and size of tartrate-resistant acid phosphatase (TRAcP)-positive multinucleated osteoclasts, with the most prominent effect at 20 µM. Rhoifolin (5 µM) most effectively inhibited osteoclast formation when present during the early stage (days 1-3) of differentiation. It also reduced osteoclast fusion, decreasing both the number of osteoclasts and the average number of nuclei per osteoclast. In functional assays, rhoifolin attenuated osteoclastic bone resorption on hydroxyapatite-coated plates in a dose-dependent manner (2.5, 5, 10 µM), reducing the resorption area to 27% and 3.8% at 2.5 µM and 5 µM, respectively, compared to the control. Rhoifolin downregulated the mRNA expression of osteoclast-specific genes including Acp5 (encoding TRAcP), Calcr (calcitonin receptor), Ctsk (cathepsin K), and Atp6v0d2 (V-ATPase subunit) in RANKL-stimulated BMMs. Mechanistically, rhoifolin attenuated RANKL-induced activation of the NF-κB pathway. It inhibited IκBα degradation and phosphorylation of NF-κB p65, and hindered p65 nuclear translocation as shown by immunofluorescence. Rhoifolin (5 µM) also inhibited the phosphorylation of ERK and JNK in the MAPK pathway at early time points (15, 30 min) after RANKL stimulation, but had little effect on p38 phosphorylation. Furthermore, rhoifolin suppressed the transcriptional activity of NFATc1 and downregulated the protein expression of key osteoclastogenic transcription factors NFATc1 and c-Fos on days 3 and 5 of RANKL stimulation. [2] |
| ln Vivo |
Radiation from loudspeakers can induce systemic harm and biochemical damage to the heart. Rhoifolin (12, 24, 30, 36, and 40 mg/kg; PO, for 7 d) has a radioprotective effect on these effects [4]. In a mouse calvarial model of titanium particle-stimulated osteolysis, daily intraperitoneal injection of rhoifolin at doses of 2.5 mg/kg (low-dose) and 5 mg/kg (high-dose) for 14 days significantly attenuated titanium particle-induced bone erosion. Micro-CT analysis showed that rhoifolin treatment increased bone mineral density (BMD) and bone volume/total tissue volume (BV/TV), while decreasing the percentage of porosity and the number of pores compared to the vehicle control group (titanium particles only). The high-dose group showed more significant effects. Histological analysis (H&E staining) confirmed that rhoifolin treatment reduced bone destruction. TRAcP staining of calvarial sections revealed a significant decrease in the number of TRAcP-positive osteoclasts in the rhoifolin-treated groups compared to the vehicle group. [2] |
| Cell Assay |
Cell Viability (MTT Assay): Differentiated 3T3-L1 cells were seeded in 24-well plates. Upon reaching 90% confluence, cells were treated with various concentrations of rhoifolin for 24 hours. Cell viability was then determined by adding MTT reagent (0.5 mg/mL final concentration) and measuring the resulting formazan product. The assay showed no significant change in cell viability after rhoifolin treatment compared to untreated controls. [1] Lactate Dehydrogenase (LDH) Release Assay: Differentiated 3T3-L1 cells were treated with rhoifolin for 24 hours. The culture supernatant was then collected, and LDH activity was measured using a commercial cytotoxicity detection kit according to the manufacturer's instructions. Cytotoxicity was calculated as a percentage relative to controls (maximum LDH release from lysed cells). No increase in LDH release was observed after rhoifolin treatment. [1] Western Blot Analysis for Adiponectin Secretion and pIR-β: Differentiated 3T3-L1 adipocytes were serum-starved for 3 hours and then incubated with rhoifolin (0–5 µM) for 24 hours (for adiponectin) or 20 minutes (for pIR-β). Cells were lysed in ice-cold buffer containing protease inhibitors. For secreted adiponectin, the culture medium was concentrated by freeze-drying. Protein samples were separated by SDS-PAGE, transferred to a PVDF membrane, blocked with skimmed milk, and incubated overnight with primary antibodies against adiponectin or phospho-insulin receptor-β. After washing, membranes were incubated with HRP-conjugated secondary antibodies, and signals were detected using an enhanced chemiluminescence system. Band intensities were quantified using image analysis software. [1] GLUT4 Translocation Assay (Immunofluorescence): 3T3-L1 adipocytes were grown on poly-L-lysine coated cover glasses. After serum starvation, cells were treated with rhoifolin or insulin for 20 minutes. Cells were then fixed with paraformaldehyde, blocked with horse serum, and incubated overnight at 4°C with primary antibodies against GLUT4 and a plasma membrane marker (Na⁺-K⁺ ATPase). After washing, cells were incubated with fluorescent dye-conjugated secondary antibodies (e.g., Alexa Fluor 488 for GLUT4, Cy3 for Na⁺-K⁺ ATPase). Nuclei were stained with DAPI. Cellular localization of GLUT4 was visualized and photographed using a fluorescence microscope. Translocation was indicated by the movement of GLUT4 signal from perinuclear regions to the cell periphery/plasma membrane. [1] Cell Viability (MTS) Assay: Bone marrow macrophages (BMMs) were seeded in 96-well plates and treated with a wide range of rhoifolin concentrations (0 to 640 µM) for 2 days. Cell viability was assessed by adding MTS solution and measuring the absorbance at 490 nm. No cytotoxicity was observed at concentrations up to 320 µM. [2] Osteoclast Differentiation and TRAcP Staining: BMMs were seeded and stimulated with M-CSF (50 ng/ml) and RANKL (100 ng/ml) to induce osteoclast differentiation. Rhoifolin at various concentrations (0, 2.5, 5, 10, 20 µM) was added from day 2. After 5-7 days, cells were fixed and stained for tartrate-resistant acid phosphatase (TRAcP) activity. TRAcP-positive cells with three or more nuclei were counted as osteoclasts. [2] Stage-Specific Treatment Assay: To determine the effective stage, BMMs were treated with rhoifolin (5 µM) during different windows: early stage (days 1-3), mid stage (days 3-5), late stage (days 5-7), or the entire period (days 1-7). TRAcP staining was performed at the end of the culture period. [2] Bone Resorption Pit Assay: Mature osteoclasts were generated from BMMs using M-CSF and RANKL, then detached and reseeded at equal numbers onto hydroxyapatite-coated 96-well plates. The reseeded osteoclasts were cultured with or without rhoifolin (0, 2.5, 5, 10 µM) for 2 days. The cells were then removed, and the resorbed areas on the hydroxyapatite surface were visualized and quantified using image analysis software. [2] F-actin Ring Staining: BMMs were cultured on coverslips and stimulated with RANKL (100 ng/ml) in the presence or absence of rhoifolin (0, 2.5, 5, 10 µM). After osteoclast formation, cells were fixed, permeabilized, and stained with rhodamine-conjugated phalloidin to visualize F-actin rings and with DAPI to stain nuclei. Fluorescence microscopy was used to image the cells and analyze osteoclast number and nuclear count. [2] Quantitative Real-Time PCR (qRT-PCR): BMMs were treated with RANKL and different concentrations of rhoifolin. Total RNA was extracted using TRIzol reagent, and cDNA was synthesized. qRT-PCR was performed using specific primers for osteoclast marker genes (Acp5, Calcr, Ctsk, Atp6v0d2) and β-actin as an internal control, using a SYBR Green-based detection system. [2] Luciferase Reporter Assay: RAW264.7 cells stably transfected with either an NF-κB-responsive or an NFATc1-responsive luciferase construct were seeded in 48-well plates. Cells were pretreated with rhoifolin for 1 hour, then stimulated with RANKL (100 ng/ml) for 6 hours (NF-κB assay) or 24 hours (NFATc1 assay). Luciferase activity was measured using a commercial luciferase assay system. [2] Western Blot Analysis: BMMs were pretreated with or without rhoifolin (5 µM) for 1 hour, then stimulated with RANKL (100 ng/ml) for various time points (0, 15, 30, 60 min for signaling proteins; 0, 1, 3, 5 days for transcription factors). Cells were lysed, proteins were separated by SDS-PAGE, transferred to PVDF membranes, and probed with specific primary antibodies against signaling molecules (p-IκBα, IκBα, p-p65, p65, p-ERK, ERK, p-JNK, JNK, p-p38, p38) or transcription factors (NFATc1, c-Fos). After incubation with HRP-conjugated secondary antibodies, proteins were detected by enhanced chemiluminescence. [2] p65 Immunofluorescence Staining: BMMs were seeded on coverslips, serum-starved, pretreated with or without rhoifolin for 1 hour, and then stimulated with or without RANKL for 30 minutes. Cells were fixed, permeabilized, blocked, and incubated with an anti-p65 antibody overnight, followed by a fluorescent secondary antibody. Nuclei were counterstained with DAPI. The subcellular localization of p65 was visualized using a fluorescence microscope. [2] |
| Animal Protocol |
Animal/Disease Models: Swiss albino mouse (10 Gy of radiation induces certain hematological and cardiac biochemical abnormalities) [4] Doses: 12, 24, 30, 36 and 40 mg/kg Route of Administration: Orally for 7 days Experimental Results: Passed Reducing levels of lipid peroxides measured as malondialdehyde, reducing toxic effects of radiation, improving changes in plasma and tissue nitric oxide, lactate dehydrogenase, creatine kinase, and plasma lipid profiles. A titanium particle-stimulated osteolysis model was established in 8-10-week-old male C57/BL6 mice. Mice were anesthetized, and a 1 cm incision was made at the center of the calvaria. A suspension of 30 mg titanium particles in 100 µl PBS was implanted onto the calvarial surface, except for the sham group which received PBS alone. The next day, treatment began. Mice were divided into four groups: Sham (PBS), Vehicle (titanium particles + PBS), Low-dose rhoifolin (titanium particles + 2.5 mg/kg rhoifolin), and High-dose rhoifolin (titanium particles + 5 mg/kg rhoifolin). Rhoifolin or PBS was administered daily via intraperitoneal injection for 14 consecutive days. On day 14, mice were euthanized, and their calvaria were harvested, fixed in 4% paraformaldehyde, and subjected to micro-CT scanning and subsequent histological processing (decalcification, paraffin embedding, sectioning for H&E and TRAcP staining). [2] |
| Toxicity/Toxicokinetics |
In differentiated 3T3-L1 adipocytes, treatment with rhoifolin at concentrations up to 5 µM for 24 hours did not show any significant cytotoxicity as assessed by both MTT cell viability assay and LDH release assay. [1] Pathological examination of liver and kidney tissues from mice treated with rhoifolin (2.5 and 5 mg/kg) for 14 days in the calvarial osteolysis model showed no signs of toxicity or histological abnormalities compared to sham and vehicle control groups, as assessed by H&E staining. [2] |
| References |
[1]. Insulin-Mimetic Action of Rhoifolin and Cosmosiin Isolated from Citrus grandis (L.) Osbeck Leaves: Enhanced Adiponectin Secretion and Insulin Receptor Phosphorylation in 3T3-L1 Cells. Evid Based Complement Alternat Med. 2011;2011:624375. [2]. Rhoifolin ameliorates titanium particle-stimulated osteolysis and attenuates osteoclastogenesis via RANKL-induced NF-κB and MAPK pathways. J Cell Physiol. 2019 Aug;234(10):17600-17611. [3]. Rhoifolin; A Potent Antiproliferative Effect on Cancer Cell Lines. Journal of Pharmaceutical Research International, 2012, 3(1), pp. 46-53. [4]. Protective Effect of Rhoifolin on Gamma Irradiation Induced Cardiac Dysfunctions in Albino Mice. Feb 15, 2014. |
| Additional Infomation |
Apigenin 7-O-neohesperidoside is an apigenin derivative having an alpha-(1->2)-L-rhamnopyranosyl)-beta-D-glucopyranosyl moiety attached to the 7-hydroxy group. It has a role as a metabolite. It is a neohesperidoside, a dihydroxyflavone and a glycosyloxyflavone. It is functionally related to an apigenin. Rhoifolin has been reported in Gonocaryum calleryanum, Euchresta japonica, and other organisms with data available. Rhoifolin (apigenin-7-O-β-neohesperidoside) is a flavone glycoside isolated for the first time from the leaves of Citrus grandis (red wendun). The leaves are a rich source of rhoifolin (1.1% w/w). The compound exhibits insulin-mimetic activity by enhancing adiponectin secretion, promoting tyrosine phosphorylation of the insulin receptor-β subunit, and facilitating GLUT4 translocation in adipocytes. These effects suggest a potential mechanism for its anti-diabetic properties, possibly involving the potentiation of insulin signaling pathways. [1] Rhoifolin is a flavonoid compound. This study demonstrates its potential therapeutic application in preventing periprosthetic osteolysis and aseptic prosthesis loosening, common complications following total joint arthroplasty, by targeting excessive osteoclast activity. [2] |
Solubility Data
| Solubility (In Vitro) | DMSO: 62.5~100 mg/mL (108.0~172.9 mM) |
| Solubility (In Vivo) |
Solubility in Formulation 1: ≥ 2.08 mg/mL (3.60 mM) (saturation unknown) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 20.8 mg/mL clear DMSO stock solution to 400 μL PEG300 and mix evenly; then add 50 μL Tween-80 to the above solution and mix evenly; then add 450 μL normal saline to adjust the volume to 1 mL. Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH₂ O to obtain a clear solution. Solubility in Formulation 2: ≥ 2.08 mg/mL (3.60 mM) (saturation unknown) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 20.8 mg/mL clear DMSO stock solution to 900 μL of 20% SBE-β-CD physiological saline solution and mix evenly. Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Solubility in Formulation 3: ≥ 2.08 mg/mL (3.60 mM) (saturation unknown) in 10% DMSO + 90% Corn Oil (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 20.8 mg/mL clear DMSO stock solution to 900 μL of corn oil and mix evenly. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 1.7285 mL | 8.6427 mL | 17.2855 mL | |
| 5 mM | 0.3457 mL | 1.7285 mL | 3.4571 mL | |
| 10 mM | 0.1729 mL | 0.8643 mL | 1.7285 mL |