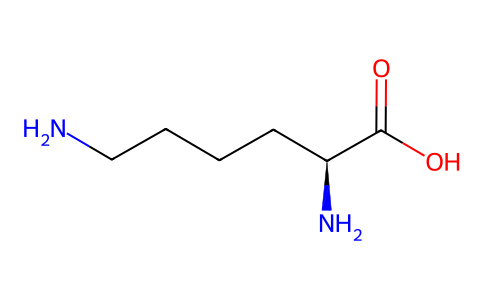
Physicochemical Properties
| Molecular Formula | C6H14N2O2 |
| Molecular Weight | 146.19 |
| Exact Mass | 146.105 |
| Elemental Analysis | C, 49.30; H, 9.65; N, 19.16; O, 21.89 |
| CAS # | 12798-06-0 |
| Related CAS # | 25104-18-1;57282-49-2 (acetate);657-27-2 (hydrochloride) |
| PubChem CID | 5962 |
| Appearance |
Needles from water, hexagonal plates from dilute alcohol Colorless crystals |
| Density | 1.1±0.1 g/cm3 |
| Boiling Point | 311.5±32.0 °C at 760 mmHg |
| Flash Point | 142.2±25.1 °C |
| Vapour Pressure | 0.0±1.4 mmHg at 25°C |
| Index of Refraction | 1.503 |
| LogP | -1.04 |
| Hydrogen Bond Donor Count | 3 |
| Hydrogen Bond Acceptor Count | 4 |
| Rotatable Bond Count | 5 |
| Heavy Atom Count | 10 |
| Complexity | 106 |
| Defined Atom Stereocenter Count | 1 |
| SMILES | NCCCC[C@@H](C(=O)O)N |
| InChi Key | KDXKERNSBIXSRK-YFKPBYRVSA-N |
| InChi Code | InChI=1S/C6H14N2O2/c7-4-2-1-3-5(8)6(9)10/h5H,1-4,7-8H2,(H,9,10)/t5-/m0/s1 |
| Chemical Name | (2S)-2,6-diaminohexanoic acid |
| Synonyms | Hydrolysine; Gidrolizin; Hydrolysin |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| ADME/Pharmacokinetics |
Absorption, Distribution and Excretion Absorbed from the lumen of the small intestine into the enterocytes by an active transport process Although the free amino acids dissolved in the body fluids are only a very small proportion of the body's total mass of amino acids, they are very important for the nutritional and metabolic control of the body's proteins. ... Although the plasma compartment is most easily sampled, the concentration of most amino acids is higher in tissue intracellular pools. Typically, large neutral amino acids, such as leucine and phenylalanine, are essentially in equilibrium with the plasma. Others, notably glutamine, glutamic acid, and glycine, are 10- to 50-fold more concentrated in the intracellular pool. Dietary variations or pathological conditions can result in substantial changes in the concentrations of the individual free amino acids in both the plasma and tissue pools. /Amino acids/ After ingestion, proteins are denatured by the acid in the stomach, where they are also cleaved into smaller peptides by the enzyme pepsin, which is activated by the increase in stomach acidity that occurs on feeding. The proteins and peptides then pass into the small intestine, where the peptide bonds are hydrolyzed by a variety of enzymes. These bond-specific enzymes originate in the pancreas and include trypsin, chymotrypsins, elastase, and carboxypeptidases. The resultant mixture of free amino acids and small peptides is then transported into the mucosal cells by a number of carrier systems for specific amino acids and for di- and tri-peptides, each specific for a limited range of peptide substrates. After intracellular hydrolysis of the absorbed peptides, the free amino acids are then secreted into the portal blood by other specific carrier systems in the mucosal cell or are further metabolized within the cell itself. Absorbed amino acids pass into the liver, where a portion of the amino acids are taken up and used; the remainder pass through into the systemic circulation and are utilized by the peripheral tissues. /Amino acids/ Protein secretion into the intestine continues even under conditions of protein-free feeding, and fecal nitrogen losses (ie, nitrogen lost as bacteria in the feces) may account for 25% of the obligatory loss of nitrogen. Under this dietary circumstance, the amino acids secreted into the intestine as components of proteolytic enzymes and from sloughed mucosal cells are the only sources of amino acids for the maintenance of the intestinal bacterial biomass. ... Other routes of loss of intact amino acids are via the urine and through skin and hair loss. These losses are small by comparison with those described above, but nonetheless may have a significant impact on estimates of requirements, especially in disease states. /Amino acids/ About 11 to 15 g of nitrogen are excreted each day in the urine of a healthy adult consuming 70 to 100 g of protein, mostly in the form of urea, with smaller contributions from ammonia, uric acid, creatinine, and some free amino acids. These are the end products of protein metabolism, with urea and ammonia arising from the partial oxidation of amino acids. Uric acid and creatinine are indirectly derived from amino acids as well. The removal of nitrogen from the individual amino acids and its conversion to a form that can be excreted by the kidney can be considered as a two-part process. The first step usually takes place by one of two types of enzymatic reactions: transamination or deamination. Transamination is a reversible reaction that uses ketoacid intermediates of glucose metabolism (e.g., pyruvate, oxaloacetate, and alpha-ketoglutarate) as recipients of the amino nitrogen. Most amino acids can take part in these reactions, with the result that their amino nitrogen is transferred to just three amino acids: alanine from pyruvate, aspartate from oxaloacetate, and glutamate from alpha-ketoglutarate. Unlike many amino acids, branched-chain amino acid transamination occurs throughout the body, particularly in skeletal muscle. Here the main recipients of amino nitrogen are alanine and glutamine (from pyruvate and glutamate, respectively), which then pass into the circulation. These serve as important carriers of nitrogen from the periphery (skeletal muscle) to the intestine and liver. In the small intestine, glutamine is extracted and metabolized to ammonia, alanine, and citrulline, which are then conveyed to the liver via the portal circulation. Nitrogen is also removed from amino acids by deamination reactions, which result in the formation of ammonia. A number of amino acids can be deaminated, either directly (histidine), by dehydration (serine, threonine), by way of the purine nucleotide cycle (aspartate), or by oxidative deamination (glutamate). ... Glutamate is also formed in the specific degradation pathways of arginine and lysine. Thus, nitrogen from any amino acid can be funneled into the two precursors of urea synthesis, ammonia and aspartate. /Amino acids/ For more Absorption, Distribution and Excretion (Complete) data for L-Lysine (7 total), please visit the HSDB record page. Metabolism / Metabolites Hepatic Like other amino acids, the metabolism of free lysine follows two principal paths: protein synthesis and oxidative catabolism. It is required for biosynthesis of such substances as carnitine, collage, and elastin. Oxidative deamination or transamination of l-lysine /yields/ alpha-keto-epsilon-aminocaproic acid; decarboxylation of l-lysine /yields/ cadaverine. /From table/ Once the amino acid deamination products enter the tricarboxylic acid (TCA) cycle (also known as the citric acid cycle or Krebs cycle) or the glycolytic pathway, their carbon skeletons are also available for use in biosynthetic pathways, particularly for glucose and fat. Whether glucose or fat is formed from the carbon skeleton of an amino acid depends on its point of entry into these two pathways. If they enter as acetyl-CoA, then only fat or ketone bodies can be formed. The carbon skeletons of other amino acids can, however, enter the pathways in such a way that their carbons can be used for gluconeogenesis. This is the basis for the classical nutritional description of amino acids as either ketogenic or glucogenic (ie, able to give rise to either ketones [or fat] or glucose). Some amino acids produce both products upon degradation and so are considered both ketogenic and glucogenic. /Amino acids/ ... Rates of lysine metabolism in fetal sheep during chronic hypoglycemia and following euglycemic recovery /were compared with/ results with normal, age-matched euglycemic control fetuses to explain the adaptive response of protein metabolism to low glucose concentrations. Restriction of the maternal glucose supply to the fetus lowered the net rates of fetal (umbilical) glucose (42%) and lactate (36%) uptake, causing compensatory alterations in fetal lysine metabolism. The plasma lysine concentration was 1.9-fold greater in hypoglycemic compared with control fetuses, but the rate of fetal (umbilical) lysine uptake was not different. In the hypoglycemic fetuses, the lysine disposal rate also was higher than in control fetuses due to greater rates of lysine flux back into the placenta and into fetal tissue. The rate of CO2 excretion from lysine decarboxylation was 2.4-fold higher in hypoglycemic than control fetuses, indicating greater rates of lysine oxidative metabolism during chronic hypoglycemia. No differences were detected for rates of fetal protein accretion or synthesis between hypoglycemic and control groups, although there was a significant increase in the rate of protein breakdown (p < 0.05) in the hypoglycemic fetuses, indicating small changes in each rate. This was supported by elevated muscle specific ubiquitin ligases and greater concentrations of 4E-BP1. Euglycemic recovery after chronic hypoglycemia normalized all fluxes and actually lowered the rate of lysine decarboxylation compared with control fetuses (p < 0.05). These results indicate that chronic hypoglycemia increases net protein breakdown and lysine oxidative metabolism, both of which contribute to slower rates of fetal growth over time. Furthermore, euglycemic correction for 5 days returns lysine fluxes to normal and causes an overcorrection of lysine oxidation. Hepatic |
| Toxicity/Toxicokinetics |
Toxicity Summary Proteins of the herpes simplex virus are rich in L-arginine, and tissue culture studies indicate an enhancing effect on viral replication when the amino acid ratio of L-arginine to L-lysine is high in the tissue culture media. When the ratio of L-lysine to L-arginine is high, viral replication and the cytopathogenicity of herpes simplex virus have been found to be inhibited. L-lysine may facilitate the absorption of calcium from the small intestine. Interactions Lysine 10 mmol/kq given to mice for 1 to 10 days significantly increased clonic and tonic seizure latencies caused by 60 mg/kg pentylenetetrazol (PTZ). On day 1 the clonic and tonic seizure latencies were increased from 160.4 +/- 26.3 and 828.6 +/- 230.8 s to 286.1 +/- 103.3 and 982.3 +/- 98.6 respectively. Both clonic and tonic seizure latencies increased steadily with additional L-lysine treatment without significant change in survival rate. On day 10, the anticonvulsant effect reached its highest level with a block of tonic seizures and survival rate of 100% without tolerance developing. Acute L-lysine significantly increased the mean clonic latency from 85.8 +/- 5.24 to 128.2 +/- 9.0 s and the mean tonic seizure from 287.2 +/- 58.7 to 313.5 +/- 42.2 s with 80 mg/kg of PTZ. On day 10 of treatment, the anticonvulsant effect of L-lysine was highest, with a significant incr of 155 and 184% in clonic and tonic latencies over control, respectively. After 15 and 20 day treatment, clonic and tonic seizure latencies and survival rate decreased, suggesting development of tolerance ... Acute intake of high levels of lysine interferes with dietary protein metabolism and competes with the transport of arginine, suggesting that adverse effects from high levels of lysine are more likely to occur if protein intake or dietary arginine intake is low. Intravenous L-lysine (16.5 to 41.3 g/day in young men) has been shown to inhibit renal tubular protein reabsorption. L-Lysine shares an intestinal transport system with L-arginine, and competes with L-arginine for reabsorption from renal tubules. Increased liver total lipids, triacylglycerol, and cholesterol concentrations were seen in rats fed 5% L-lysine and 15% casein for 2 weeks, an effect that can be reversed by feeding arginine. ... The aim of the present study was to study the effects of L-arginine transport inhibition, using acute and repeated L-lysine treatment, on phencyclidine (PCP)-induced disruption of PPI in mice. RESULTS: Subchronic, and to some extent acute, pretreatment with L-lysine blocked a PCP-induced deficit in PPI without affecting basal PPI. CONCLUSIONS: L-lysine has been shown to block L-arginine transport in vitro, most likely via a competitive blockade and down regulation of cationic amino acid transporters. However, the importance of L-arginine transport as a regulatory mechanism in NO production in vivo is still not clear. The present results lend further support to the notion that some of the effects of PCP in the central nervous system are mediated via NO and that L-arginine transport may play a role in the regulation of NO production in the brain. |
| Additional Infomation |
Therapeutic Uses Lysine appears to have antiviral, anti-osteoporotic, cardiovascular, and lipid-lowering effects, although more controlled human studies are needed. Unproven uses: The most common use of supplemental lysine is for preventing and treating episodes of herpes simplex virus. Lysine has been used in conjunction with calcium to prevent and treat osteoporosis. It has also been used for treating pain, aphthous ulcers, migraine attacks, rheumatoid arthritis, and opiate withdrawal. Many "body-building" formulations contain lysine to aid in muscle repair. /Experimental Therapy/ A major contributing factor to the loss of mobility in elderly people is the gradual and continuous loss of lean body mass ... Elderly (76 +/-1.6 years) women (n = 39) and men (n = 38) were recruited for a double-blinded controlled study. Study participants were randomly assigned to either an isonitrogenous control-supplement (n = 37) or a treatment-supplement (HMB/Arg/Lys) consisting of beta-hydroxy-beta-methylbutyrate, L-arginine, and L-lysine (n = 40) for the 1-year study ... In subjects taking the HMB/Arg/Lys supplement, lean tissue increased over the year of study while in the control group, lean tissue did not change ... Consumption of a simple amino acid-related cocktail increased protein turnover and lean tissue in elderly individuals in a year-long study. Supplementation of meals with low doses of oral lysine improved fasting plasma lysine concentrations in 27 Finnish patients with lysinuric protein intolerance (LPI) without causing hyperammonemia or other recognizable side effects during 12 months of follow-up. In conclusion, low-dose oral lysine supplementation is potentially beneficial to patients with LPI and can be started safely at an early age. Drug Warnings Patients with hypercholesterolemia should be aware that supplemental lysine has been linked to increased cholesterol levels in animal studies. However, other studies have shown lysine can also decrease cholesterol levels. Adverse reactions: renal dysfunction, including Fanconi's syndrome and renal failure, has been reported. L-lysine ibuprofen /was given/ to a preterm infant with respiratory distress to induce closure of a patent ductus arteriosus, and the infant experienced pulmonary hypertension. Only 3 cases of pulmonary hypertension following early administration of an ibuprofen solution buffered with tromethamine have previously been reported. However, this severe side effect has never been observed in multicentre, randomized, double-blind controlled trials, nor in recent reviews or meta-analyses of L-lysine ibuprofen use. Pharmacodynamics Insures the adequate absorption of calcium; helps form collagen ( which makes up bone cartilage & connective tissues); aids in the production of antibodies, hormones & enzymes. Recent studies have shown that Lysine may be effective against herpes by improving the balance of nutrients that reduce viral growth. A deficiency may result in tiredness, inability to concentrate, irritability, bloodshot eyes, retarded growth, hair loss, anemia & reproductive problems. |
Solubility Data
| Solubility (In Vitro) | May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 6.8404 mL | 34.2021 mL | 68.4041 mL | |
| 5 mM | 1.3681 mL | 6.8404 mL | 13.6808 mL | |
| 10 mM | 0.6840 mL | 3.4202 mL | 6.8404 mL |