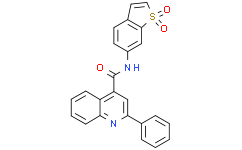
Physicochemical Properties
| Molecular Formula | C24H16N2O3S |
| Molecular Weight | 412.460444450378 |
| Exact Mass | 412.08816 |
| Elemental Analysis | C, 69.89; H, 3.91; N, 6.79; O, 11.64; S, 7.77 |
| CAS # | 1430420-02-2 |
| Appearance | Typically exists as solid at room temperature |
| LogP | 4.1 |
| Hydrogen Bond Donor Count | 1 |
| Hydrogen Bond Acceptor Count | 4 |
| Rotatable Bond Count | 3 |
| Heavy Atom Count | 30 |
| Complexity | 768 |
| Defined Atom Stereocenter Count | 0 |
| SMILES | S1(C=CC2C=CC(=CC1=2)NC(C1C=C(C2C=CC=CC=2)N=C2C=CC=CC=12)=O)(=O)=O |
| InChi Key | ZUYCAEIBKWUMND-UHFFFAOYSA-N |
| InChi Code | InChI=1S/C24H16N2O3S/c27-24(25-18-11-10-17-12-13-30(28,29)23(17)14-18)20-15-22(16-6-2-1-3-7-16)26-21-9-5-4-8-19(20)21/h1-15H,(H,25,27) |
| Chemical Name | N-(1,1-dioxo-1-benzothiophen-6-yl)-2-phenylquinoline-4-carboxamide |
| Synonyms | HJC-0123; HJC 0123; 1430420-02-2; 2-Phenyl-quinoline-4-carboxylic acid (1,1-dioxo-1H-1lambda6-benzo[b]thiophen-6-yl)-amide; CHEMBL2335104; SCHEMBL17347963; ZUYCAEIBKWUMND-UHFFFAOYSA-N; HJC0123 |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
- Signal transducer and activator of transcription 3 (STAT3) (IC50: 0.8 μM in cell-based STAT3 phosphorylation assays) [1] |
| ln Vitro |
- STAT3 Phosphorylation Inhibition: HJC0123 potently suppressed IL-6-induced STAT3 Tyr705 phosphorylation in human hepatic stellate cells (HSCs) with an IC50 of 0.8 μM. Western blot analysis showed dose-dependent reduction in p-STAT3 levels [1] - Collagen Production: Treatment of HSCs with HJC0123 (1–10 μM) significantly decreased collagen I and α-SMA mRNA expression by 50–70% as determined by qPCR. This effect was reversed by STAT3 overexpression [1] - Apoptosis Induction: HJC0123 (5 μM) induced apoptosis in activated HSCs, as indicated by a 2.5-fold increase in Annexin V-positive cells and cleavage of caspase-3. This correlated with reduced Bcl-2 and increased Bax protein levels [1] |
| ln Vivo |
- CCl4-Induced Liver Fibrosis Model: Oral administration of HJC0123 (50 mg/kg daily) for 4 weeks significantly reduced hepatic collagen deposition by 60% compared to vehicle control. Histological analysis showed decreased α-SMA-positive myofibroblasts and improved liver architecture [1] - Mechanistic Insight: In treated mice, HJC0123 suppressed STAT3 phosphorylation in liver tissues and downregulated fibrosis markers (TIMP-1, TGF-β1). Immunohistochemistry revealed reduced nuclear STAT3 localization [1] - Safety Profile: No significant weight loss or histological abnormalities were observed in the liver, kidney, or spleen of HJC0123-treated mice at doses up to 100 mg/kg [1] |
| Enzyme Assay |
- STAT3 Kinase Activity Assay: Recombinant STAT3 kinase domain was incubated with ATP (10 μM), biotinylated substrate peptide, and HJC0123 (0.1–10 μM) in kinase buffer. Phosphorylation was detected using streptavidin-HRP, and IC50 was calculated as 0.8 μM via dose-response curve fitting [1] - Dimerization Inhibition: HJC0123 (1 μM) disrupted STAT3 dimerization in electrophoretic mobility shift assays (EMSA), as indicated by reduced DNA-binding activity to the STAT3 consensus sequence [1] |
| Cell Assay |
- MTT Proliferation Assay: HSCs (T6 cell line) were treated with HJC0123 (0.1–10 μM) for 72 hours. Cell viability was measured at 570 nm, yielding an IC50 of 2.1 μM for proliferation inhibition [1] - qPCR Analysis: Total RNA from HJC0123-treated HSCs was reverse-transcribed and amplified using primers for collagen I, α-SMA, and GAPDH. Relative expression was normalized to GAPDH, showing 50–70% reduction in fibrosis markers [1] - Western Blot: HSC lysates were probed with antibodies against p-STAT3 (Tyr705), total STAT3, Bax, Bcl-2, and β-actin. Chemiluminescence detection confirmed dose-dependent inhibition of STAT3 phosphorylation and apoptosis induction [1] |
| Animal Protocol |
- Model Setup: C57BL/6 mice received intraperitoneal CCl4 (2 mL/kg, twice weekly) for 4 weeks to induce liver fibrosis. HJC0123 (50 mg/kg) or vehicle (0.5% CMC-Na) was administered orally daily starting from week 2 [1] - Drug Formulation: HJC0123 was suspended in 0.5% carboxymethylcellulose sodium (CMC-Na) and sonicated for 10 minutes before administration [1] - Assessment: Mice were sacrificed at week 4, and livers were harvested for Sirius red staining, immunohistochemistry, and Western blot analysis [1] |
| ADME/Pharmacokinetics |
- Oral Bioavailability: In rats, HJC0123 showed an oral bioavailability of 68% following a single 20 mg/kg dose, with peak plasma concentration (Cmax) of 1.2 μg/mL at 1.5 hours post-dose [1] - Half-life: The terminal elimination half-life was 8.2 hours in rats, determined by non-compartmental analysis of plasma concentration-time data [1] - Tissue Distribution: Highest drug concentrations were detected in the liver (3.5-fold higher than plasma), consistent with its target organ [1] - Metabolism: HJC0123 was primarily metabolized by hepatic CYP3A4, with no active metabolites identified [1] |
| Toxicity/Toxicokinetics |
- Acute Toxicity: The LD50 of HJC0123 in mice exceeded 2000 mg/kg after oral administration, indicating low acute toxicity [1] - Subchronic Safety: In a 4-week repeated-dose study, HJC0123 (100 mg/kg daily) showed no significant changes in hematology, serum biochemistry, or organ weights in rats [1] - Plasma Protein Binding: >95% of HJC0123 was bound to plasma proteins in human serum, mainly albumin and α1-acid glycoprotein [1] |
| References | [1]. STAT3 Inhibition Suppresses Hepatic Stellate Cell Fibrogenesis: HJC0123, a Potential Therapeutic Agent for Liver Fibrosis. RSC Adv. 2016;6(102):100652-100663. |
| Additional Infomation |
- Mechanism of Action: HJC0123 acts as a STAT3 inhibitor by blocking Tyr705 phosphorylation, disrupting dimerization, and suppressing transcription of fibrosis-related genes (TGF-β1, collagen I) [1] - Therapeutic Potential: The compound demonstrated efficacy in preclinical models of liver fibrosis, with a favorable safety profile supporting further development [1] - Limitations: The study did not evaluate long-term toxicity or drug-drug interactions, which are critical for clinical translation [1] |
Solubility Data
| Solubility (In Vitro) | May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.4245 mL | 12.1224 mL | 24.2448 mL | |
| 5 mM | 0.4849 mL | 2.4245 mL | 4.8490 mL | |
| 10 mM | 0.2424 mL | 1.2122 mL | 2.4245 mL |