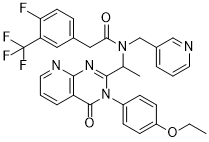
rac-NBI-74330 is a novel and potent CXCR3 antagonist
Physicochemical Properties
| Molecular Formula | C32H27F4N5O3 |
| Molecular Weight | 605.59; |
| Exact Mass | 605.205 |
| CAS # | 473722-68-8 |
| Related CAS # | 473722-68-8 (racemate);855527-92-3 (R-isomer); |
| PubChem CID | 10167713 |
| Appearance | Typically exists as solid at room temperature |
| Density | 1.3±0.1 g/cm3 |
| Boiling Point | 752.5±70.0 °C at 760 mmHg |
| Flash Point | 408.9±35.7 °C |
| Vapour Pressure | 0.0±2.5 mmHg at 25°C |
| Index of Refraction | 1.605 |
| LogP | 3.46 |
| Hydrogen Bond Donor Count | 0 |
| Hydrogen Bond Acceptor Count | 10 |
| Rotatable Bond Count | 9 |
| Heavy Atom Count | 44 |
| Complexity | 1020 |
| Defined Atom Stereocenter Count | 0 |
| SMILES | FC1C=CC(=CC=1C(F)(F)F)CC(N(CC1C=NC=CC=1)C(C)C1=NC2C(=CC=CN=2)C(N1C1C=CC(=CC=1)OCC)=O)=O |
| InChi Key | XMRGQUDUVGRCBS-UHFFFAOYSA-N |
| InChi Code | InChI=1S/C32H27F4N5O3/c1-3-44-24-11-9-23(10-12-24)41-30(39-29-25(31(41)43)7-5-15-38-29)20(2)40(19-22-6-4-14-37-18-22)28(42)17-21-8-13-27(33)26(16-21)32(34,35)36/h4-16,18,20H,3,17,19H2,1-2H3 |
| Chemical Name | N-[1-[3-(4-ethoxyphenyl)-4-oxopyrido[2,3-d]pyrimidin-2-yl]ethyl]-2-[4-fluoro-3-(trifluoromethyl)phenyl]-N-(pyridin-3-ylmethyl)acetamide |
| Synonyms | rac-NBI-74330 racNBI74330 rac NBI 74330 |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
CXCR3 chemokine receptor antagonist [1] |
| ln Vitro |
In primary microglial and astroglial cell cultures prepared from neonatal rats, pretreatment with rac-NBI-74330 (100 nM) for 30 minutes prior to LPS (100 ng/ml) stimulation for 24 hours significantly diminished the LPS-induced upregulation of CXCL10 and CXCL11 protein levels in both cell types, as determined by Western blot analysis. [1] Western blot analysis of primary glial cultures showed that rac-NBI-74330 treatment reduced the level of CXCL10 in LPS-activated microglia. [1] |
| ln Vivo |
In a rat model of neuropathic pain induced by chronic constriction injury (CCI) of the sciatic nerve, repeated intrathecal (i.t.) administration of rac-NBI-74330 (10 µg/5 µl; administered 16h and 1h before CCI, then once daily for 7 days) significantly attenuated the development of tactile and thermal hypersensitivity on day 7 post-CCI, as measured by the von Frey and cold plate tests, respectively. [1] Repeated intrathecal administration of rac-NBI-74330 (same regimen) in CCI rats significantly diminished microglial cell activation (reduced spinal IBA1 protein level) and increased astroglial cell activation (increased spinal GFAP protein level) on day 7 post-CCI. [1] Repeated intrathecal administration of rac-NBI-74330 (same regimen) in CCI rats downregulated the protein levels of its endogenous ligands CXCL4, CXCL9, and CXCL10 in the spinal cord, and decreased CXCL9 protein level in the dorsal root ganglia (DRG) on day 7 post-CCI. Concurrently, it increased the protein levels of CXCR3 and CXCL11 in the spinal cord, and CXCR3 and CXCL4 in the DRG. [1] Both single and repeated intrathecal administration of rac-NBI-74330 (10 µg/5 µl) enhanced the analgesic effectiveness of a single intrathecal dose of morphine (2.5 µg/5 µl) in CCI rats on day 7 post-CCI, but did not enhance the effectiveness of buprenorphine. [1] Repeated intrathecal administration of rac-NBI-74330 (same regimen) in CCI rats significantly increased the protein level of the mu-opioid receptor (MOR) in the spinal cord compared to naive rats on day 7 post-CCI. [1] Single intrathecal administration of rac-NBI-74330 (10 µg/5 µl) to naive mice did not influence baseline nociceptive transmission. [1] |
| Cell Assay |
Primary microglial and astroglial cell cultures were prepared from the cerebral cortex of 1-day-old Wistar rats. Cells were seeded in culture medium in 6-well plates at a density of 1.2x10^6 cells per well for protein analysis. Primary cultures were treated with rac-NBI-74330 at a concentration of 100 nM, 30 minutes before stimulation with LPS (lipopolysaccharide) at 100 ng/ml. The cells were then incubated with LPS for 24 hours. After treatment, cell lysates were collected for Western blot analysis to measure protein levels of chemokines such as CXCL10 and CXCL11. [1] Immunostaining for IBA1 (microglial marker) and GFAP (astrocyte marker) was used to identify and ensure the purity of the microglial and astroglial populations in the cultures. [1] |
| Animal Protocol |
For neuropathic pain studies in rats, rac-NBI-74330 was dissolved in 100% DMSO. It was administered intrathecally (i.t.) in a volume of 5 µl at a dose of 10 µg/5 µl. The dosing regimen involved a preemptive injection 16 hours and 1 hour before performing the chronic constriction injury (CCI) of the sciatic nerve. Following CCI, rac-NBI-74330 was administered once daily via the intrathecal catheter for 7 consecutive days. Control animals received the vehicle (100% DMSO) according to the same schedule. Behavioural tests (von Frey and cold plate) were performed 120-125 minutes after the last drug administration on day 7 post-CCI. [1] To assess the effect on opioid effectiveness, on the 7th day post-CCI, rats chronically treated with vehicle or rac-NBI-74330 received a single intrathecal dose of morphine or buprenorphine (2.5 µg/5 µl) 60 minutes after the last rac-NBI-74330 or vehicle injection. Behavioural tests were then repeated. [1] For studies in naive mice, a single intrathecal injection of rac-NBI-74330 (10 µg/5 µl, dissolved in 100% DMSO) was administered, and behavioural tests were conducted afterwards. [1] |
| References |
[1]. Pharmacological blockade of CXCR3 by (±)-NBI-74330 reduces neuropathic pain and enhances opioid effectiveness - Evidence from in vivo and in vitro studies. Biochim Biophys Acta Mol Basis Dis. 2018 Oct;1864(10):3418-3437. |
| Additional Infomation |
rac-NBI-74330 is a potent and selective CXCR3 antagonist. The study provides the first evidence that pharmacological blockade of CXCR3 with rac-NBI-74330 attenuates neuropathic pain and enhances morphine analgesia in a rat model. [1] The proposed mechanism involves rac-NBI-74330 diminishing microglial activation and the subsequent release of pronociceptive chemokines (CXCL4, CXCL9, CXCL10) in the spinal cord, while concurrently increasing astroglial activation. The enhancement of morphine's effect is also associated with an upregulation of spinal mu-opioid receptor (MOR) levels. [1] The study hypothesizes that CXCR3 signaling is important in neuropathic pain, and its blockade represents a promising target for managing neuropathic pain and improving opioid therapy. [1] |
Solubility Data
| Solubility (In Vitro) | May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |