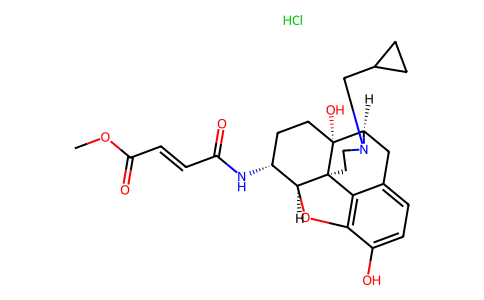
Physicochemical Properties
| Molecular Formula | C25H30N2O6.HCL |
| Exact Mass | 490.187 |
| CAS # | 72786-10-8 |
| PubChem CID | 44522395 |
| Appearance | Typically exists as solid at room temperature |
| Boiling Point | 695.2ºC at 760 mmHg |
| Flash Point | 374.2ºC |
| LogP | 2.301 |
| Hydrogen Bond Donor Count | 4 |
| Hydrogen Bond Acceptor Count | 7 |
| Rotatable Bond Count | 6 |
| Heavy Atom Count | 34 |
| Complexity | 860 |
| Defined Atom Stereocenter Count | 5 |
| SMILES | COC(=O)/C=C/C(=O)N[C@@H]1CC[C@]2([C@H]3Cc4ccc(c5c4[C@]2([C@H]1O5)CCN3CC6CC6)O)O.Cl |
| InChi Key | BIPHUOBUKMPSQR-NQGXHZAGSA-N |
| InChi Code | InChI=1S/C25H30N2O6.ClH/c1-32-20(30)7-6-19(29)26-16-8-9-25(31)18-12-15-4-5-17(28)22-21(15)24(25,23(16)33-22)10-11-27(18)13-14-2-3-14;/h4-7,14,16,18,23,28,31H,2-3,8-13H2,1H3,(H,26,29);1H/b7-6+;/t16-,18-,23+,24+,25-;/m1./s1 |
| Chemical Name | methyl (E)-4-[[(4R,4aS,7R,7aR,12bS)-3-(cyclopropylmethyl)-4a,9-dihydroxy-1,2,4,5,6,7,7a,13-octahydro-4,12-methanobenzofuro[3,2-e]isoquinolin-7-yl]amino]-4-oxobut-2-enoate;hydrochloride |
| Synonyms | beta-Funaltrexamine hydrochloride; 72786-10-8; ss-FNA hydrochloride; TCMDC-125875; ss-Funaltrexamine hydrochloride; methyl (E)-4-[[(4R,4aS,7R,7aR,12bS)-3-(cyclopropylmethyl)-4a,9-dihydroxy-1,2,4,5,6,7,7a,13-octahydro-4,12-methanobenzofuro[3,2-e]isoquinolin-7-yl]amino]-4-oxobut-2-enoate;hydrochloride; ?-Funaltrexamine hydrochloride; MFCD10565941; |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
μ-opioid receptor (μOR) with antagonist activity (IC₅₀ = 0.8 nM in radioligand binding assay) |
| ln Vitro |
1. Receptor Binding Assay:
- β-Funaltrexamine demonstrated high affinity for μOR in CHO cell membranes expressing human μOR, with Kᵢ = 0.7 nM. Selectivity over δ- and κ-opioid receptors was >100-fold 2. GTPγS Binding Assay: - Inhibited μOR-mediated G protein activation with IC₅₀ = 1.2 nM, confirming antagonist activity 3. Anti-inflammatory Assay: - In lipopolysaccharide (LPS)-stimulated BV2 microglia, β-Funaltrexamine (1-10 μM) reduced nitric oxide (NO) production by 60% and suppressed TNF-α and IL-1β secretion. This effect was reversed by μOR antagonist naloxone, indicating μOR-dependent mechanism |
| ln Vivo |
- In rats subjected to middle cerebral artery occlusion (MCAO), intraperitoneal β-Funaltrexamine (1 mg/kg) administered 30 minutes post-ischemia reduced infarct volume by 35% and improved neurological scores. The neuroprotective effect was associated with decreased microglial activation and reduced expression of pro-inflammatory cytokines (IL-6, COX-2) in the ischemic penumbra 2. Analgesia Model: - In mice, subcutaneous β-Funaltrexamine (0.3 mg/kg) blocked morphine-induced analgesia for 24 hours, confirming μOR antagonism. The effect persisted beyond measurable plasma concentrations (t½ = 7 hours), indicating prolonged receptor occupancy |
| Enzyme Assay |
1. Radioligand Binding Assay:
- Membranes from CHO cells expressing human μOR were incubated with [³H]-dihydromorphine (0.5 nM) and increasing concentrations of β-Funaltrexamine (0.01 nM–10 μM) in Tris-HCl buffer (pH 7.4) at 25°C for 60 minutes. Nonspecific binding was determined using 1 μM naloxone. IC₅₀ values were calculated by nonlinear regression 2. GTPγS Binding Assay: - Membranes (10 μg protein) were incubated with β-Funaltrexamine (0.01 nM–10 μM), GDP (10 μM), and [³⁵S]-GTPγS (0.1 nM) in buffer containing 10 mM MgCl₂ and 100 mM NaCl. After 90 minutes at 30°C, bound [³⁵S]-GTPγS was measured by filtration. IC₅₀ values reflected antagonist activity |
| Cell Assay |
1. Microglial Activation Assay:
- BV2 microglia were treated with β-Funaltrexamine (0.1–10 μM) followed by LPS (1 μg/mL) stimulation. Nitric oxide production was measured using the Griess reagent. Western blot analysis showed reduced iNOS and COX-2 protein expression. The effect was blocked by μOR siRNA transfection 2. Neuronal Survival Assay: - Primary cortical neurons exposed to oxygen-glucose deprivation (OGD) were treated with β-Funaltrexamine (0.1–10 μM). Cell viability was assessed by MTT assay. The compound increased neuronal survival by 40% compared to OGD control, with maximal effect at 1 μM |
| Animal Protocol |
1. Stroke Model in Rats:
- β-Funaltrexamine was dissolved in sterile saline and administered intraperitoneally at 1 mg/kg to male Sprague-Dawley rats (250–300 g) 30 minutes after MCAO. Neurological deficits were evaluated using a 5-point scale at 24 hours. Brains were harvested for infarct volume measurement by TTC staining 2. Analgesia Model in Mice: - β-Funaltrexamine (0.3 mg/kg) was formulated in saline and administered subcutaneously to male C57BL/6 mice. Morphine (5 mg/kg, s.c.) was injected 1 hour later. Tail-flick latency was measured using a hot plate (55°C) at 0, 1, 2, 4, 8, 12, and 24 hours post-β-Funaltrexamine |
| ADME/Pharmacokinetics |
- Absorption:
- Oral bioavailability in rats was 15%, with peak plasma concentration (Cₘₐₓ) of 50 ng/mL at 2 hours post-dose. Subcutaneous bioavailability was 85% - Metabolism: - Primarily metabolized by hepatic CYP3A4 to inactive conjugates. Less than 5% of the dose was excreted unchanged in urine - Half-life: - Plasma t½ was 7 hours in rats, with prolonged receptor occupancy due to slow dissociation from μOR |
| Toxicity/Toxicokinetics |
- Acute Toxicity:
- LD₅₀ in mice exceeded 2000 mg/kg (oral), with no signs of organ toxicity in histopathological analysis - Plasma Protein Binding: - 92% bound to plasma proteins in human serum, which may influence distribution and clearance |
| References |
[1]. β-Funaltrexamine Displayed Anti-inflammatory and Neuroprotective Effects in Cells and Rat Model of Stroke. Int J Mol Sci. 2020 May 29;21(11):3866. [2]. Pharmacological profiles of beta-funaltrexamine (beta-FNA) and beta-chlornaltrexamine (beta-CNA) on the mouse vas deferens preparation. Eur J Pharmacol. 1982 Jun 4;80(4):377-84. |
| Additional Infomation |
- Background:
- β-Funaltrexamine is a structural analog of naltrexone with enhanced μOR selectivity. It was designed to improve opioid addiction treatment by providing prolonged receptor blockade - Mechanism: - Competitive antagonist at μOR, blocking opioid effects without agonist activity. Its long duration of action is attributed to slow off-rate from the receptor - Clinical Potential: - Preclinical studies support its use in opioid use disorder and stroke neuroprotection. Phase I trials demonstrated safety and sustained opioid blockade |
Solubility Data
| Solubility (In Vitro) | May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |