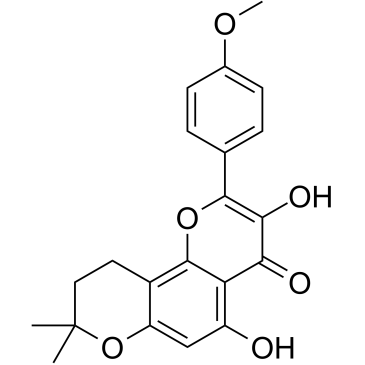
β-Anhydroicaritin is a naturally occurring bioactive compound isolated from Boswellia carterii Birdware with various biological activity such as antiosteoporosis, estrogen regulation and antitumor effects. It can decrease the production of NO, IL-10, TNF-α, MCP-1 and IL-6 in inperitonitis mice.
Physicochemical Properties
| Molecular Formula | C21H20O6 |
| Molecular Weight | 368.3799 |
| Exact Mass | 368.125 |
| CAS # | 38226-86-7 |
| PubChem CID | 14583584 |
| Appearance | Light yellow to yellow solid |
| Density | 1.4±0.1 g/cm3 |
| Boiling Point | 575.3±50.0 °C at 760 mmHg |
| Melting Point | 222-223 °C |
| Flash Point | 205.5±23.6 °C |
| Vapour Pressure | 0.0±1.7 mmHg at 25°C |
| Index of Refraction | 1.633 |
| Source | Flavonoids/Flavonols from Boswellia carterii Birdware |
| LogP | 4.2 |
| Hydrogen Bond Donor Count | 2 |
| Hydrogen Bond Acceptor Count | 6 |
| Rotatable Bond Count | 2 |
| Heavy Atom Count | 27 |
| Complexity | 618 |
| Defined Atom Stereocenter Count | 0 |
| InChi Key | PPCHTBBOSVKORE-UHFFFAOYSA-N |
| InChi Code | InChI=1S/C21H20O6/c1-21(2)9-8-13-15(27-21)10-14(22)16-17(23)18(24)19(26-20(13)16)11-4-6-12(25-3)7-5-11/h4-7,10,22,24H,8-9H2,1-3H3 |
| Chemical Name | 3,5-dihydroxy-2-(4-methoxyphenyl)-8,8-dimethyl-9,10-dihydropyrano[2,3-h]chromen-4-one |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month Note: This product requires protection from light (avoid light exposure) during transportation and storage. |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets | IL-10; MMP-3; IL-6 |
| ln Vitro |
β-anhydroicaritin Mannich base derivatives possessing moderate to potent cytotoxicity against these three cancer cells (Hela, HCC1954 and SK-OV-3). Compound 15 and 19 showed selective cytotoxicity against HCC1954 cells and Hela cells respectively, they are potential and selective anticancer agent and worthy of further development.[1] In vitro cytotoxic activity on human cancer cell lines: β-Anhydroicaritin was tested for cytotoxicity against three human cancer cell lines (A549: lung adenocarcinoma, HepG2: hepatocellular carcinoma, MCF-7: breast cancer) using MTT assay. Cells were treated with β-Anhydroicaritin at concentrations of 0.1 μM, 1 μM, 10 μM, 50 μM, and 100 μM for 48 hours. - It showed concentration-dependent cytotoxicity on all three cell lines [1] - The IC50 values were 12.3 ± 1.2 μM (A549), 8.5 ± 0.9 μM (HepG2), and 15.6 ± 1.5 μM (MCF-7); HepG2 cells were the most sensitive to β-Anhydroicaritin [1] |
| ln Vivo |
β-anhydroicaritin ameliorated the degradation of periodontal tissue and inhibited the synthesis and secretion of TNF-α and MMP-3 in diabetic rats. In conclusion, the results of the present study suggest that β-anhydroicaritin may be used in the treatment of periodontitis in patients with diabetes. However, the mechanisms by which β-anhydroicaritin ameliorates periodontal degradation, i.e. whether it directly inhibits or regulates the body’s metabolic function through the elimination of ONOO− and further inhibits TNF-α and MMP-3 expression indirectly, remains to be elucidated. Further investigations are required to shed light upon these questions.[2] 1. Effect on periodontal tissue of diabetic rats: Streptozotocin (STZ)-induced diabetic rats (blood glucose > 16.7 mmol/L) were divided into control group, diabetic model group, and β-Anhydroicaritin treatment groups (5 mg/kg, 10 mg/kg, oral gavage, once daily for 4 weeks). - β-Anhydroicaritin dose-dependently reduced the mRNA and protein levels of tumor necrosis factor-α (TNF-α) and matrix metalloproteinase-3 (MMP-3) in periodontal tissue [2] - The 10 mg/kg group had a more significant effect: TNF-α protein level was reduced by 42.5 ± 3.8% and MMP-3 protein level by 38.2 ± 3.5% compared to the diabetic model group [2] 2. Protective effect against mouse peritonitis: Lipopolysaccharide (LPS)-induced peritonitis mice were divided into control group, LPS model group, and β-Anhydroicaritin treatment groups (20 mg/kg, 40 mg/kg, intraperitoneal injection, 1 hour before LPS administration). - β-Anhydroicaritin dose-dependently reduced serum levels of pro-inflammatory cytokines: IL-6 was reduced by 58.3 ± 4.2% and TNF-α by 52.1 ± 3.9% in the 40 mg/kg group [3] - The 40 mg/kg group had a 70% survival rate at 72 hours, which was higher than the 30% survival rate of the LPS model group [3] - The number of inflammatory cells in peritoneal exudate was reduced by 45.6 ± 3.7% in the 40 mg/kg group compared to the model group [3] |
| Cell Assay |
MTT-based cytotoxicity assay: 1. Cell culture: A549, HepG2, and MCF-7 cells were cultured in Dulbecco's Modified Eagle Medium (DMEM) supplemented with 10% fetal bovine serum and 1% penicillin-streptomycin, and maintained at 37°C in a 5% CO₂ humidified incubator [1] 2. Cell seeding and treatment: Cells were seeded into 96-well plates at a density of 5×10³ cells per well and incubated overnight to allow attachment. The medium was then replaced with fresh medium containing β-Anhydroicaritin (final concentrations: 0.1 μM, 1 μM, 10 μM, 50 μM, 100 μM); the control group received medium without the compound [1] 3. Detection: After 48 hours of incubation, 20 μL of MTT solution (5 mg/mL) was added to each well and incubated for another 4 hours at 37°C. The supernatant was removed, 150 μL of dimethyl sulfoxide (DMSO) was added to dissolve formazan crystals, and absorbance was measured at 570 nm using a microplate reader. IC50 was determined by nonlinear regression analysis of the concentration-viability curve [1] |
| Animal Protocol |
Male Wistar rats (n=40; three months old) were randomly divided into four groups: Normal control group, diabetes group, diabetes + β-anhydroicaritin group and diabetes + urate group, (n=10 in each group). Following an overnight fast, diabetes was induced by intraperitoneal injection of streptozocin. The rats were maintained for 12 weeks and the blood sugar, urine sugar and body weight were assessed in week 12. Histological changes of the periodontal tissues were observed by hematoxylin and eosin staining, and the expression levels of TNF-α and MMP-3 were observed by immunohistochemistry. Following 12 weeks, the TNF-α grey value in the diabetes group was significantly lower compared with that in the control group (P<0.05), while no significant difference was observed between TNF-α levels in the diabetes + β-anhydroicaritin group, diabetes + urate group and the control group (P>0.05). However, TNF-α levels in the diabetes + β-anhdroicaritin group and diabetes + urate group were significantly higher compared with those in the diabetes group (P<0.05), and those in the diabetes + β-anhydroicaritin group were lower compared with those in the diabetes + urate group (P<0.05). The MMP-3 grey value in the diabetes group was significantly lower compared with that in the control group (P<0.05), while no significant difference was observed between MMP-3 levels in the diabetes + β-anhydroicaritin group, diabetes + urate group and the control group (P>0.05). However, MMP-3 levels the diabetes + β-anhydroicaritin group and diabetes + urate group were significantly higher compared with those in the diabetes group (P<0.05), and those in the diabetes + β-anhydroicaritin group were lower compared with those in the diabetes + urate group (P<0.01). β-anhydroicaritin normalized the expression levels of TNF-α and MMP-3 in the periodontal tissue of diabetic rats and led to the recovery of the changes in the morphological structure of the periodontal tissue.[2] 1. Diabetic rat periodontal experiment: - Animal model establishment: Male Sprague-Dawley rats (200-220 g) were intraperitoneally injected with STZ (60 mg/kg) to induce type 1 diabetes; rats with blood glucose > 16.7 mmol/L were considered successful models [2] - Drug preparation and administration: β-Anhydroicaritin was dissolved in 0.5% carboxymethyl cellulose sodium (CMC-Na) to prepare 0.5 mg/mL and 1 mg/mL solutions. Rats in the treatment groups received oral gavage of 5 mg/kg or 10 mg/kg β-Anhydroicaritin once daily for 4 weeks; the control group and model group received equal volumes of 0.5% CMC-Na [2] - Sample collection and detection: After 4 weeks, rats were sacrificed, and periodontal tissues (maxillary molars) were excised. Total RNA and protein were extracted from the tissues to detect TNF-α and MMP-3 expression via RT-PCR and western blot, respectively [2] 2. Mouse peritonitis experiment: - Animal preparation: Male ICR mice (20-22 g) were housed in a 12-hour light/dark cycle with free access to food and water [3] - Drug preparation and administration: β-Anhydroicaritin was dissolved in normal saline containing 5% Tween 80 to prepare 2 mg/mL and 4 mg/mL solutions. Mice in the treatment groups were intraperitoneally injected with 20 mg/kg or 40 mg/kg β-Anhydroicaritin 1 hour before intraperitoneal injection of LPS (10 mg/kg); the control group received normal saline, and the model group received LPS + vehicle [3] - Sample collection and detection: At 6 hours after LPS injection, serum was collected to detect IL-6 and TNF-α levels via ELISA, and peritoneal exudate was collected to count inflammatory cells. Survival rate was recorded every 12 hours for 72 hours [3] |
| References |
[1]. Synthesis of Icaritin and β-anhydroicaritin Mannich Base Derivatives and Their Cytotoxic Activities on Three Human Cancer Cell Lines. Anticancer Agents Med Chem. 2017;17(1):137-142. [2]. Effect of β-anhydroicaritin on the expression levels of tumor necrosis factor-α and matrix metalloproteinase-3 in periodontal tissue of diabetic rats. Mol Med Rep. 2015 Aug;12(2):1829-37. [3]. Protective effect of anhydroicaritin against peritonitis in mice. Xi Bao Yu Fen Zi Mian Yi Xue Za Zhi. 2013 Oct;29(10):1036-9. |
| Additional Infomation |
beta-Anhydroicaritin has been reported in Epimedium brevicornu with data available. 1. Background of β-Anhydroicaritin: β-Anhydroicaritin is a naturally derived flavonoid compound, structurally related to icariin [1][2][3] 2. Mechanism of action: - In diabetic rats, it protects periodontal tissue by downregulating the expression of pro-inflammatory cytokine TNF-α and matrix-degrading enzyme MMP-3 [2] - In mouse peritonitis, it alleviates inflammatory responses by inhibiting the production of pro-inflammatory cytokines (IL-6, TNF-α) and reducing inflammatory cell infiltration [3] 3. Research significance: The studies confirm β-Anhydroicaritin has potential as a candidate for cancer therapy (based on in vitro cytotoxicity) and anti-inflammatory therapy (for periodontal disease and peritonitis) [1][2][3] |
Solubility Data
| Solubility (In Vitro) | DMSO : ~8.33 mg/mL (~22.61 mM) |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.7146 mL | 13.5729 mL | 27.1459 mL | |
| 5 mM | 0.5429 mL | 2.7146 mL | 5.4292 mL | |
| 10 mM | 0.2715 mL | 1.3573 mL | 2.7146 mL |