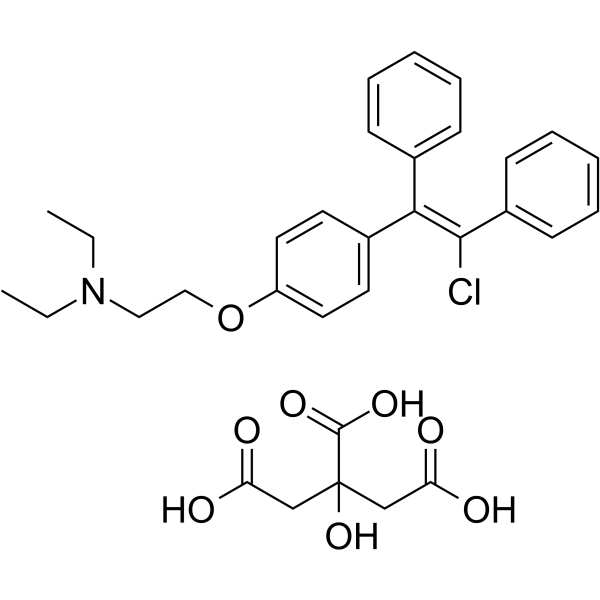
Physicochemical Properties
| Molecular Formula | C₃₂H₃₆CLNO₈ |
| Molecular Weight | 598.08 |
| Exact Mass | 597.213 |
| CAS # | 7619-53-6 |
| Related CAS # | Zuclomiphene-d4 citrate;2714316-71-7;Zuclomiphene-d5 citrate;1795132-80-7 |
| PubChem CID | 3033832 |
| Appearance | White to off-white solid powder |
| LogP | 5.314 |
| Hydrogen Bond Donor Count | 4 |
| Hydrogen Bond Acceptor Count | 9 |
| Rotatable Bond Count | 14 |
| Heavy Atom Count | 42 |
| Complexity | 708 |
| Defined Atom Stereocenter Count | 0 |
| SMILES | CCN(CC)CCOC1=CC=C(C=C1)/C(=C(/C2=CC=CC=C2)\Cl)/C3=CC=CC=C3.C(C(=O)O)C(CC(=O)O)(C(=O)O)O |
| InChi Key | PYTMYKVIJXPNBD-OQKDUQJOSA-N |
| InChi Code | InChI=1S/C26H28ClNO.C6H8O7/c1-3-28(4-2)19-20-29-24-17-15-22(16-18-24)25(21-11-7-5-8-12-21)26(27)23-13-9-6-10-14-23;7-3(8)1-6(13,5(11)12)2-4(9)10/h5-18H,3-4,19-20H2,1-2H3;13H,1-2H2,(H,7,8)(H,9,10)(H,11,12)/b26-25-; |
| Chemical Name | 2-[4-[(Z)-2-chloro-1,2-diphenylethenyl]phenoxy]-N,N-diethylethanamine;2-hydroxypropane-1,2,3-tricarboxylic acid |
| Synonyms | Zuclomiphene citrate; Zuclomiphene citrate |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month Note: Please store this product in a sealed and protected environment, avoid exposure to moisture. |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
Zuclomiphene acts as an estrogen receptor antagonist, binding to cytoplasmic and nuclear estrogen receptors [3] |
| ln Vitro |
In chick oviduct preparations, Zuclomiphene exhibits anti-estrogenic activity by competing with estrogen for binding to cytoplasmic and nuclear estrogen receptors. It inhibits estrogen-induced responses in the oviduct, as demonstrated by reduced estrogen-dependent biological activity [3] |
| ln Vivo |
In male mice, administration of Zuclomiphene (100 μg/day, subcutaneous injection) for 28 days results in a significant increase in testis weight compared to controls. It also leads to an increase in epididymal weight and affects sperm parameters, with changes in sperm count and motility. Additionally, it modulates reproductive tissue morphology, including alterations in seminiferous tubule structure [1] |
| Enzyme Assay |
In experiments with chick oviduct cytoplasmic and nuclear fractions, Zuclomiphene is incubated with these fractions in the presence of radiolabeled estrogen. The binding of Zuclomiphene to estrogen receptors is assessed by measuring the displacement of radiolabeled estrogen, allowing quantification of its affinity for the receptors [3] |
| Animal Protocol |
For male mice studies, adult male mice are subcutaneously injected with Zuclomiphene at a dose of 100 μg/day for 28 days. Control groups receive vehicle injections. At the end of the treatment period, mice are euthanized, and reproductive tissues (testes, epididymides) are harvested for weight measurement, histological analysis, and sperm parameter evaluation [1] |
| ADME/Pharmacokinetics |
Absorption, Distribution and Excretion Based on early studies with 14 C-labeled clomifene, the drug was shown to be readily absorbed orally in humans. Based on early studies with 14C-labeled clomiphene citrate, the drug was shown to be readily absorbed orally in humans and excreted principally in the feces. Mean urinary excretion was approximately 8% with fecal excretion of about 42%. SC DOSE OF (14)C CLOMIPHENE CITRATE...WAS DISTRIBUTED IN TISSUES OF FEMALE GUINEA PIG NEONATES... ESTROGENIC-RESPONSIVE TISSUES SHOWED HIGH AFFINITY FOR (14)C. LEVELS OF (14)C...CONSTANT IN UTERUS...THOSE IN OVARIES & PLASMA DECLINED...IN ADRENALS INCR. /CLOMIPHENE CITRATE/ ABOUT ONE-HALF OF THE INGESTED DOSE IS EXCRETED IN FIVE DAYS; TRACES APPEAR IN THE FECES UP TO SIX WEEKS AFTER ADMIN. /CLOMIPHENE CITRATE/ Clomiphene is well absorbed following oral administration. The drug and its metabolites are eliminated primarily in the feces and to a lesser extent in the urine. The rather long plasma half-life (approximately 5 to 7 days) is due largely to plasma protein binding, enterophepatic circulation, and accumulation in fatty tissues. Active metabolites with long half-lives also may be produced. Metabolism / Metabolites Hepatic INCUBATION OF THE NONSTEROIDAL ANTIESTROGEN CLOMIPHENE WITH RAT LIVER MICROSOMES RESULTED IN THE FORMATION OF THE 4-HYDROXY-, N-DESETHYL-, & N-OXIDE METABOLITES, IN QUALITATIVE CONTRAST TO RESULTS PREVIOUSLY OBTAINED ANALOGOUSLY WITH RABBIT MICROSOMES IN WHICH ONLY THE FIRST 2 METABOLITES WERE DETECTED. ORAL ADMIN OF CLOMIPHENE RESULTED IN NO DETECTABLE URINARY ELIMINATION OF THE DRUG OR ITS METABOLITES. 4-HYDROXYCLOMIPHENE WAS THE SOLE DETECTABLE ELIMINATION PRODUCT IN FECAL EXTRACTIONS. Biological Half-Life 5-7 days After a single oral dose of clomiphene citrate (which contains Zuclomiphene as an isomer) in normal volunteers, Zuclomiphene shows a longer elimination half-life compared to the other isomer (enclomiphene). It persists in plasma for an extended period, with detectable levels up to several weeks post-administration [2] |
| Toxicity/Toxicokinetics |
Hepatotoxicity There is little information on serum aminotransferase levels during clomiphene therapy which is typically given in low doses for a short time only. There have been a few reports of mild serum enzyme elevations in patients taking clomiphene, but no convincing instances of idiosyncratic, clinically apparent liver injury with its use. Drugs used to treat infertility in women typically act by stimulation of the ovarian follicles which can lead to the ovarian hyperstimulation syndrome (OHSS), which can occasionally be accompanied by serum enzyme elevations and even jaundice. This syndrome typically arises within 4 to 14 days of ovarian stimulation with gonadotropins or clomiphene and is characterized by the onset of abdominal pain and distension with ascites and enlarged ovaries and ovarian cysts. There can be marked fluid shifts with hemoconcentration and rapid onset of severe ascites and pleural effusions. Liver tests are elevated in 25% to 40% of patients with OHSS, typically with mild-to-moderate increases in ALT and AST values, but minimal or no elevations in serum bilirubin and alkaline phosphatase levels. The liver test abnormalities resolve with resolution of the OHSS, usually within 2 to 3 weeks of onset. In severe instances, OHSS can be fatal, but death is usually due to dehydration, shock and septicemia rather than hepatic failure. In typical cases with abnormal liver enzymes, liver histology reveals nonspecific changes of sinusoidal dilatation, mild fat accumulation and focal inflammatory infiltrates with macrophages and lymphocytes. OHSS is less common with clomiphene than with human chorionic gonadotropin (hCG) induction of ovulation. Likelihood score: C (probable cause of clinically apparent liver injury as a part of the ovarian hyperstimulation syndrome). Effects During Pregnancy and Lactation ◉ Summary of Use during Lactation Clomiphene appeared in low amounts in milk in one woman. Several studies found that clomiphene suppresses lactation in women who did not want to breastfeed. It appears to act by lowering serum prolactin, especially the post-stimulation surge in serum prolactin. It is likely that clomiphene would interfere with lactation in a nursing mother. ◉ Effects in Breastfed Infants A woman who was taking clomiphene in a dose of 2.04 mg/kg daily partially breastfed her infant. She did not observe any adverse effects in her infant. ◉ Effects on Lactation and Breastmilk A double-blind study compared clomiphene in dosages of 50 mg daily for 10 days (n = 110), 100 mg daily for 5 days (n = 26) and placebo (n = 41) in their ability to suppress lactation and relieve pain and engorgement in nonnursing postpartum mothers. Both dosages of clomiphene were superior to placebo as reported by the women, but the 100 mg daily dosage was somewhat superior to the 50 mg daily dosage. A study compared clomiphene 100 mg daily for 5 days (n = 60) to placebo (n = 30) in suppressing lactation and symptoms of engorgement. Starting clomiphene within 12 hours of delivery was more effective in all measures than starting it 12 hours or more after delivery as judged by a physician observer; both treatments were more effective than mechanical measures alone such as breast binding. A randomized trial compared clomiphene 50 mg twice daily for 14 days (n = 15) to bromocriptine 2.5 mg twice daily for 14 days (n = 15), diethylstilbestrol 5 mg 3 times daily for 14 days (n = 15), testosterone propionate 75 mg intramuscularly once (n = 15), and placebo 3 times daily by mouth (n = 15) in their ability to reduce serum prolactin and lactation postpartum. After three days of treatment, serum prolactin was reduced to 65% of baseline by clomiphene compared to a drop to 35% in patients who received bromocriptine. Clomiphene was also less effective than bromocriptine in suppressing lactation and symptoms of engorgement. A study compared clomiphene 100 mg daily for 7 days (n = 10) to placebo (n = 12) started on the first day postpartum. Clomiphene was no more effective than placebo in suppressing lactation or reducing serum prolactin concentrations. Women in the first week postpartum who did not wish to breastfeed received either clomiphene 50 mg twice daily (n = 10) or placebo (n = 10). Women who received clomiphene did not experience a rise in serum prolactin from baseline values during use of a breast pump; those given placebo had the normal post-stimulation rise in serum prolactin. Eighty postpartum women were studied. Forty received clomiphene 50 mg twice daily for 5 days beginning the first day postpartum; 20 received clomiphene 50 mg twice daily for 5 days beginning the fourth day postpartum; and, 20 received placebo. All women receiving clomiphene experienced inhibition of lactation, and reductions in breast engorgement, discomfort and serum prolactin. Prolactin serum concentrations became statistically lower than baseline on day 3 for the women who were 1 day postpartum and on day 5 for those who were 4 days postpartum at the outset. Placebo did not suppress lactation nor suppress serum prolactin. |
| References |
[1]. Differential effects of isomers of clomiphene citrate on reproductive tissues in male mice. BJU Int. 2016 Feb;117(2):344-50. [2]. Single-dose pharmacokinetics of clomiphene citrate in normal volunteers. Fertil Steril. 1986 Sep;46(3):392-6. [3]. Sutherland RL. Estrogen antagonists in chick oviduct: antagonist activity of eight synthetic triphenylethylene derivatives and their interactions with cytoplasmic and nuclear estrogen receptors. Endocrinology. 1981 Dec;109(6):2061-8. [4]. The biochemical and morphological response of hydrolytic enzymes in the developing brain to hypocholesterolemic agents. Acta Neuropathol. 1980;49(2):89-94. [5]. Discovery of High-Affinity Ligands of σ1 Receptor, ERG2, and Emopamil Binding Protein by Pharmacophore Modeling and Virtual Screening. J Med Chem. 2005 Jul 28;48(15):4754-64. |
| Additional Infomation |
Zuclomiphene is one of the geometric isomers of clomiphene citrate, a triphenylethylene derivative. Its anti-estrogenic activity in reproductive tissues contributes to its effects on male reproductive parameters, including testis weight and sperm characteristics [1] [3] Clomiphene Citrate can cause cancer and developmental toxicity according to state or federal government labeling requirements. Zuclomiphene Citrate is the cis isomer of clomiphene which exhibits weak estrogen agonist activity evaluated for antineoplastic activity against breast cancer. (NCI04) Clomiphene Citrate is the citrate salt form of clomiphene, a triphenylethylene nonsteroidal ovulatory stimulant evaluated for antineoplastic activity against breast cancer. Clomiphene has both estrogenic and anti-estrogenic activities that compete with estrogen for binding at estrogen receptor sites in target tissues. This agent causes the release of the pituitary gonadotropins follicle stimulating hormone (FSH) and luteinizing hormone (LH), leading to ovulation. (NCI04) A triphenyl ethylene stilbene derivative which is an estrogen agonist or antagonist depending on the target tissue. Note that ENCLOMIPHENE and ZUCLOMIPHENE are the (E) and (Z) isomers of Clomiphene respectively. See also: Clomiphene Citrate (annotation moved to). |
Solubility Data
| Solubility (In Vitro) | DMSO : ~100 mg/mL (~167.20 mM) |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 1.6720 mL | 8.3601 mL | 16.7202 mL | |
| 5 mM | 0.3344 mL | 1.6720 mL | 3.3440 mL | |
| 10 mM | 0.1672 mL | 0.8360 mL | 1.6720 mL |