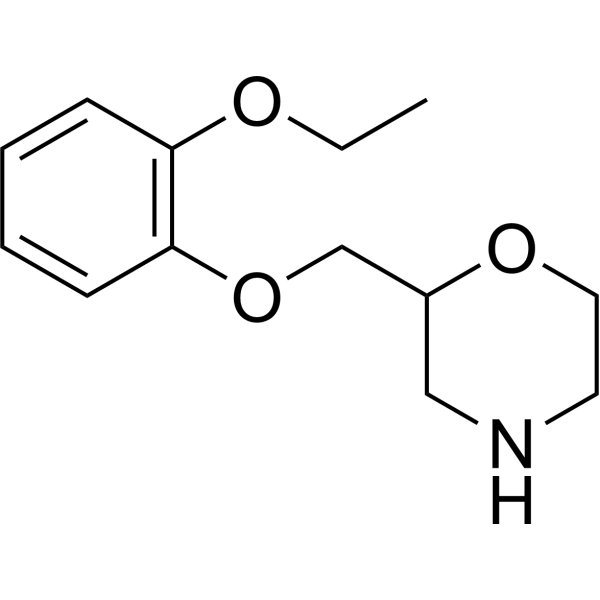
Physicochemical Properties
| Molecular Formula | C13H19NO3 |
| Exact Mass | 237.136 |
| CAS # | 46817-91-8 |
| Related CAS # | Viloxazine hydrochloride;35604-67-2 |
| PubChem CID | 5666 |
| Appearance | Colorless to light yellow oil |
| Density | 1.061 g/cm3 |
| Boiling Point | 350.5ºC at 760 mmHg |
| Melting Point | 185-186ºC |
| Flash Point | 144.3ºC |
| Index of Refraction | 1.499 |
| LogP | 1.781 |
| Hydrogen Bond Donor Count | 1 |
| Hydrogen Bond Acceptor Count | 4 |
| Rotatable Bond Count | 5 |
| Heavy Atom Count | 17 |
| Complexity | 213 |
| Defined Atom Stereocenter Count | 0 |
| SMILES | C(OC1C=CC=CC=1OCC1CNCCO1)C |
| InChi Key | YWPHCCPCQOJSGZ-UHFFFAOYSA-N |
| InChi Code | InChI=1S/C13H19NO3/c1-2-15-12-5-3-4-6-13(12)17-10-11-9-14-7-8-16-11/h3-6,11,14H,2,7-10H2,1H3 |
| Chemical Name | 2-[(2-ethoxyphenoxy)methyl]morpholine |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| ADME/Pharmacokinetics |
Absorption, Distribution and Excretion Viloxazine is rapidly absorbed following oral administration. The relative bioavailability of viloxazine extended-release relative to an immediate-release formulation was about 88%. Viloxazine Cmax and AUC increase proportionally over a dosage range from 100 mg to 600 mg once daily. The Cmax ranges between 540 and 1600 ng/mL. Following administration of a single 200 mg dose, the median Tmax was approximately five hours, with a range of three to nine hours. Steady-state was reached after two days of once-daily administration, and no accumulation was observed. A high-fat meal decreases Cmax and AUC by about 9% and 8%, respectively, and delays Tmax by two hours. Viloxazine is primarily excreted via renal elimination. After administration of radiolabeled viloxazine, 90% of the dose was recovered in urine within the first 24 hours post-dose. Less than 1% of the dose is excreted in the feces. About 12-15% of the total drug is eliminated as unchanged parent drug. The volume of distribution was 0.73 ± 0.28 L/kg following intravenous administration. The clearance rate was 124 ± 11 mL/hour/kg following intravenous administration. Metabolism / Metabolites Viloxazine undergoes CYP2D6-mediated 5-hydroxylation to form 5-hydroxyviloxazine. This metabolite can be glucuronidated by UGT1A9 and UGT2B15 to form 5-hydroxyviloxazine glucuronide, which is the major metabolite detected in plasma. Viloxazine can also be glucuronidated to form Viloxazine N-carbamoyl glucuronide. Biological Half-Life The mean (± SD) half-life of viloxazine was 7.02 (± 4.74) hours. |
| Toxicity/Toxicokinetics |
Hepatotoxicity In four placebo-controlled trials of viloxazine in children with ADHD, minor serum aminotransferase elevations occurred in 5% to 10% of recipients but were more than 2 times the upper limit of normal in less than 1%. In the preregistration trials, there were no instances of clinically apparent liver injury or serum aminotransferase elevations with jaundice attributable to viloxazine. Since its approval as therapy for depression in Europe more than 30 years ago and as therapy of ADHD in the United States in 2021, there have been no publications describing clinically apparent liver injury due to viloxazine. Furthermore, summaries of the efficacy and safety of viloxazine do not mention hepatic adverse events. Nevertheless, long term clinical experience with viloxazine in children is limited, and other SNRIs (such as atomoxetine) have been linked to rare instances of clinically apparent liver injury. Likelihood score: E (unlikely cause of acute liver injury with jaundice). Effects During Pregnancy and Lactation ◉ Summary of Use during Lactation There is no published experience with viloxazine during breastfeeding. If viloxazine is required by the mother of an older infant, it is not a reason to discontinue breastfeeding, but until more data become available, an alternate drug may be preferred, especially while nursing a newborn or preterm infant. ◉ Effects in Breastfed Infants Relevant published information was not found as of the revision date. ◉ Effects on Lactation and Breastmilk Relevant published information was not found as of the revision date. Protein Binding Viloxazine is 76-82% bound to human plasma proteins over the blood concentration range of 0.5 mcg/mL to 10 mcg/mL. |
| Additional Infomation |
2-[(2-ethoxyphenoxy)methyl]morpholine is an aromatic ether. Viloxazine is a selective norepinephrine reuptake inhibitor. For decades, an immediate-release formulation of viloxazine has been used in Europe as an antidepressant. It was first approved in the UK in 1974; however, the immediate-release formulation was discontinued due to business reasons unrelated to drug safety and efficacy. In the US, viloxazine was assigned an orphan drug designation in 1984 under the brand name CATATROL: while this product was intended to treat cataplexy and narcolepsy, the drug was never approved for these therapeutic indications. In April 2021, an extended-release formulation of viloxazine under the brand name QELBREE was approved by the FDA for the treatment of attention deficit hyperactivity disorder (ADHD). Viloxazine is a Norepinephrine Reuptake Inhibitor. The mechanism of action of viloxazine is as a Norepinephrine Uptake Inhibitor, and Cytochrome P450 1A2 Inhibitor, and Cytochrome P450 2D6 Inhibitor, and Cytochrome P450 3A4 Inhibitor, and Cytochrome P450 2B6 Inhibitor. Viloxazine is a selective norepinephrine reuptake inhibitor that is used in the therapy of attention deficit/hyperactivity disorder in children. Viloxazine has been associated with uncommon and mild serum enzyme elevations during therapy but not with occurrence of clinically apparent liver injury. A morpholine derivative used as an antidepressant. It is similar in action to IMIPRAMINE. See also: Viloxazine Hydrochloride (active moiety of). Drug Indication Viloxazine is a selective norepinephrine reuptake inhibitor indicated for the treatment of Attention Deficit Hyperactivity Disorder (ADHD) in adults and pediatric patients 6 years and older. Mechanism of Action Attention Deficit Hyperactivity Disorder (ADHD) is a common neurodevelopmental disorder in children characterized by inattention and hyperactivity. In current literature, the pathophysiology of ADHD is understood to involve the imbalance of neurotransmitters, especially dopamine (DA) and norepinephrine (NE). The mechanism of action of viloxazine has not been fully elucidated; however, viloxazine is believed to work by modulating the monoaminergic neurotransmitter systems. Viloxazine is a selective and moderate norepinephrine reuptake inhibitor that binds to the norepinephrine transporter and inhibits the reuptake of norepinephrine. It thereby increases extracellular norepinephrine levels across several brain regions. Viloxazine potentiates serotonergic effects: it was shown to enhance neuronal sensitivity to serotonin and increase serotonin levels in the brain. _In vitro_, viloxazine is an antagonist at 5-HT2B receptors and an agonist 5-HT2C receptors. 5-HT2B receptors expressed on GABAergic interneurons are involved in tonic inhibitory control of serotonin neurons that innervate the medial prefrontal context; thus, antagonism of 5-HT2B receptors may result in disinhibition and enhanced serotonin release in the brain region. There is conflicting evidence in the literature that viloxazine increases dopamine levels in the brain via direct or indirect effects. For example, the norepinephrine transporter is also involved in the reuptake of dopamine in the prefrontal cortex and stimulation of 5-HT2C receptors facilitates DA release and enhances dopaminergic transmission in the brain. As dopamine dysregulation in the prefrontal cortex and amygdala is implicated in ADHD pathophysiology, the impact of viloxazine on dopamine levels may contribute to its mechanism of action. However, there is insufficient evidence to conclude this. Viloxazine has a negligible impact on dopamine in the nucleus accumbens and is not associated with an abuse risk. |
Solubility Data
| Solubility (In Vitro) | May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |