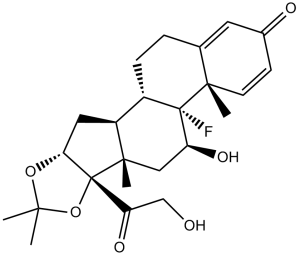
Triamcinolone acetonide (Acetospan; Adcortyl A; AllerNaze; Kenalone; Nasacort; Aristocort; Aristoderm. Aristogel) is a potent and synthetic glucocorticoid with improved anti-inflammatory activities.
Physicochemical Properties
| Molecular Formula | C24H31FO6 | |
| Molecular Weight | 434.5 | |
| Exact Mass | 434.21 | |
| CAS # | 76-25-5 | |
| Related CAS # | Triamcinolone acetonide (Standard);76-25-5;Triamcinolone acetonide-d7;Triamcinolone acetonide-d7-1;Triamcinolone acetonide-d6;352431-33-5 | |
| PubChem CID | 6436 | |
| Appearance | White to off-white solid powder | |
| Density | 1.3±0.1 g/cm3 | |
| Boiling Point | 576.9±50.0 °C at 760 mmHg | |
| Melting Point | 274-278ºC (dec.) | |
| Flash Point | 302.7±30.1 °C | |
| Vapour Pressure | 0.0±3.6 mmHg at 25°C | |
| Index of Refraction | 1.589 | |
| LogP | 2.5 | |
| Hydrogen Bond Donor Count | 2 | |
| Hydrogen Bond Acceptor Count | 7 | |
| Rotatable Bond Count | 2 | |
| Heavy Atom Count | 31 | |
| Complexity | 925 | |
| Defined Atom Stereocenter Count | 8 | |
| SMILES | C[C@]12C[C@@H]([C@]3([C@H]([C@@H]1C[C@@H]4[C@]2(OC(O4)(C)C)C(=O)CO)CCC5=CC(=O)C=C[C@@]53C)F)O |
|
| InChi Key | YNDXUCZADRHECN-JNQJZLCISA-N | |
| InChi Code | InChI=1S/C24H31FO6/c1-20(2)30-19-10-16-15-6-5-13-9-14(27)7-8-21(13,3)23(15,25)17(28)11-22(16,4)24(19,31-20)18(29)12-26/h7-9,15-17,19,26,28H,5-6,10-12H2,1-4H3/t15-,16-,17-,19+,21-,22-,23-,24+/m0/s1 | |
| Chemical Name | (6aS,6bR,7S,8aS,8bS,11aR,12aS,12bS)-6b-fluoro-7-hydroxy-8b-(2-hydroxyacetyl)-6a,8a,10,10-tetramethyl-1,2,6a,6b,7,8,8a,8b,11a,12,12a,12b-dodecahydro-4H-naphtho[2,1:4,5]indeno[1,2-d][1,3]dioxol-4-one | |
| Synonyms |
|
|
| HS Tariff Code | 2934.99.9001 | |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
|
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
Glucocorticoid Receptor (GR) [1][2][3][4][5] |
| ln Vitro |
As the concentration rises, triamcinolone acetonide (0.05-3 mg/mL, 48-60 h) decreases BRECs' capacity to proliferate [1]. In a concentration-dependent manner, triamcinolone acetonide (0.04-5 mg/mL, 24 h) decreases the viability of both normal and osteoarthritic (OA) chondrocytes [2]. The degree of cartilage structural degradation, chondrocyte loss and colony formation, and proteoglycan loss in OA cartilage are all made worse by triamcinolone acetonide (0.04-5 mg/mL, 24 h) [2]. Strongly inducing monocyte differentiation toward M2 and anti-inflammatory macrophage phenotypes is triamcinolone acetonide (100 nM, 7 days) [3]. In human retinal endothelial cells, Triamcinolone Acetonide (1 μM, 10 μM) dose-dependently inhibited cell proliferation. At 10 μM, it reduced BrdU incorporation by 65% and cell viability by 40% (MTT assay), without inducing significant apoptosis (Annexin V/PI staining)[1] - In canine normal and osteoarthritis (OA) articular chondrocytes, Triamcinolone Acetonide (10 nM, 100 nM, 1 μM) alone or combined with hyaluronan (HA) modulated matrix metabolism. At 100 nM, it increased type II collagen mRNA expression by 30% and aggrecan by 25% in OA chondrocytes; combined with HA, the effect was enhanced (type II collagen upregulated by 45%). It also reduced MMP-13 expression by 40% at 1 μM[2] - In murine bone marrow-derived macrophages, Triamcinolone Acetonide (100 nM) activated anti-inflammatory macrophages (M2 phenotype) by upregulating folate receptor β (FRβ) expression by 2.3-fold (flow cytometry). It increased IL-10 secretion by 60% and decreased TNFα by 55% (ELISA), suppressing pro-inflammatory responses[3] - In keratinocytes from atopic dermatitis patients, Triamcinolone Acetonide (0.1 μM, 1 μM) improved skin barrier function by upregulating filaggrin mRNA expression by 1.8-fold (RT-PCR) and increasing ceramide synthesis by 35% at 1 μM (lipid analysis)[4] |
| ln Vivo |
In rats with osteoarthritis, intraperitoneal injection of 1.43 mg/mL triamcinolone acetonide once a week for 6–12 weeks totally stops the development of osteophytes and improves FRβ-related macrophage activation [3]. In a rat model of retinal neovascularization, intravitreal injection of Triamcinolone Acetonide (4 mg/eye, single dose) reduced retinal endothelial cell proliferation by 70% (immunohistochemical staining for Ki-67) and attenuated neovascular tuft formation[1] - In DBA/1 mice with collagen-induced arthritis (CIA), intraperitoneal injection of Triamcinolone Acetonide (1 mg/kg weekly for 6 weeks) prevented osteophytosis by 65% (micro-CT analysis). It activated FRβ+ anti-inflammatory macrophages in joint tissues, reducing inflammatory cell infiltration and TNFα levels by 50% (ELISA)[3] - In patients with atopic dermatitis, topical application of Triamcinolone Acetonide cream (0.1%) twice daily for 4 weeks improved skin barrier structure: transepidermal water loss (TEWL) decreased by 45%, and skin hydration increased by 38% (corneometer measurement). It also reduced erythema and pruritus scores by 60%[4] |
| Cell Assay |
Cell Viability Assay[2] Cell Types: Chondrocyte Tested Concentrations: 0.04, 0.08, 0.16, 0.31, 0.63, 1.25, 2.5, and 5 mg/ml Incubation Duration: 24 h Experimental Results: decreased cell viability with the value of IC50 was 2.23 mg/ mL in normal chondrocytes and 1.14 mg/mL in OA chondrocytes. Retinal endothelial cell proliferation assay: Human retinal endothelial cells were seeded in 96-well plates and treated with Triamcinolone Acetonide (0.1 μM, 1 μM, 10 μM) for 72 hours. BrdU was added for the last 24 hours to assess proliferation; MTT assay was used to measure cell viability. Annexin V/PI staining was performed to detect apoptosis[1] - Canine chondrocyte matrix metabolism assay: Normal and OA canine articular chondrocytes were isolated and cultured in 6-well plates. Triamcinolone Acetonide (10 nM, 100 nM, 1 μM) was added alone or with HA for 7 days. RT-PCR detected type II collagen, aggrecan, and MMP-13 mRNA expression; Western blot confirmed corresponding protein levels[2] - Macrophage polarization assay: Murine bone marrow-derived macrophages were cultured in 6-well plates and treated with Triamcinolone Acetonide (10 nM, 100 nM, 1 μM) for 48 hours. Flow cytometry analyzed FRβ expression; ELISA quantified IL-10 and TNFα secretion[3] - Keratinocyte barrier function assay: Keratinocytes from atopic dermatitis patients were seeded in 24-well plates and treated with Triamcinolone Acetonide (0.01 μM, 0.1 μM, 1 μM) for 72 hours. RT-PCR measured filaggrin mRNA; lipid extraction and analysis quantified ceramide levels[4] |
| Animal Protocol |
Animal/Disease Models: Severe OA rat model [3] Doses: 1.43 mg/mL Route of Administration: intraperitoneal (ip)injection Experimental Results: diminished body weight during OA induction. demonstrated more macrophage activation and minimal or no osteophyte formation when injected knee joints. Retinal neovascularization rat model: Neonatal rats were exposed to hyperoxia to induce retinal neovascularization. On postnatal day 14, Triamcinolone Acetonide (4 mg/eye) was administered via intravitreal injection. Rats were euthanized on postnatal day 21; retinal flat mounts were prepared for immunohistochemical staining of Ki-67 to assess endothelial cell proliferation[1] - Collagen-induced arthritis (CIA) mouse model: DBA/1 mice were immunized with type II collagen to induce CIA. Starting from day 21 post-immunization, Triamcinolone Acetonide (1 mg/kg) was injected intraperitoneally once weekly for 6 weeks. Joint tissues were collected for micro-CT analysis of osteophytosis and immunohistochemical detection of FRβ+ macrophages[3] |
| ADME/Pharmacokinetics |
Absorption: Topical application results in minimal systemic absorption (<1% of dose); intravitreal administration shows local retention in ocular tissues for up to 4 weeks[1][5] - Distribution: After local administration, it primarily distributes in target tissues (skin, joints, eyes) with limited systemic spread[5] - Metabolism: Metabolized in the liver via hydroxylation and reduction to inactive metabolites[5] - Excretion: Metabolites are excreted in urine (~60%) and feces (~30%); parent drug excretion is <5%[5] - Half-life: Elimination half-life is ~3-5 hours in plasma; local tissue half-life is longer (e.g., ~2 weeks in ocular tissues)[5] |
| Toxicity/Toxicokinetics |
Local toxicity: Topical use may cause mild skin atrophy (incidence ~10%) or irritation (erythema, pruritus, ~8%); intravitreal injection may induce transient intraocular pressure elevation (incidence ~15%)[4][5] - Systemic toxicity: At therapeutic doses, no significant肝肾毒性; high doses may cause glucose intolerance (mean blood glucose increase <15%) and mild sodium retention[5] - Plasma protein binding rate: ~98% bound to human plasma proteins[5] - Drug-drug interactions: No significant interactions with common topical or systemic drugs; does not inhibit cytochrome P450 enzymes[5] |
| References |
[1]. Effect of triamcinolone acetonide on proliferation of retinal endothelial cells in vitro and in vivo . British journal of ophthalmology, 2005, 89(6): 745-747. [2]. In vitro effects of triamcinolone acetonide and in combination with hyaluronan on canine normal and spontaneous osteoarthritis articular cartilage . In Vitro Cellular & Developmental Biology-Animal, 2016, 52: 723-735. [3]. Triamcinolone acetonide activates an anti-inflammatory and folate receptor–positive macrophage that prevents osteophytosis in vivo . Arthritis research & therapy, 2015, 17(1): 1-13. [4]. Effects of pimecrolimus compared with triamcinolone acetonide cream on skin barrier structure in atopic dermatitis: a randomized, double-blind, right–left arm trial . Acta Dermato-Venereologica, 2013, 93(5): 515-519. [5]. http://en.wikipedia.org/wiki/Triamcinolone_acetonide. [6]. Glucocorticoids improve severe or critical COVID-19 by activating ACE2 and reducing IL-6 levels. Int J Biol Sci 2020; 16(13):2382-2391. |
| Additional Infomation |
Triamcinolone acetonide is a synthetic glucocorticoid that is the 16,17-acetonide of triamcinolone. Used to treat various skin infections. It has a role as an anti-inflammatory drug and an anti-allergic agent. It is an 11beta-hydroxy steroid, a 20-oxo steroid, a 21-hydroxy steroid, a 3-oxo-Delta(4) steroid, a glucocorticoid, a cyclic ketal, a fluorinated steroid and a primary alpha-hydroxy ketone. It is functionally related to a triamcinolone. It derives from a hydride of a pregnane. Triamcinolone acetonide is a Corticosteroid. The mechanism of action of triamcinolone acetonide is as a Corticosteroid Hormone Receptor Agonist. Triamcinolone Acetonide is the acetonide salt form of triamcinolone, a synthetic glucocorticosteroid with immunosuppressive and anti-inflammatory activity. Triamcinolone acetonide binds to specific cytosolic glucocorticoid receptors and subsequently interacts with glucocorticoid receptor response element on DNA and alters gene expression. This results in an induction of the synthesis of certain anti-inflammatory proteins while inhibiting the synthesis of certain inflammatory mediators. Consequently, an overall reduction in chronic inflammation and autoimmune reactions are accomplished. An esterified form of TRIAMCINOLONE. It is an anti-inflammatory glucocorticoid used topically in the treatment of various skin disorders. Intralesional, intramuscular, and intra-articular injections are also administered under certain conditions. See also: Triamcinolone (has active moiety); Triamcinolone Hexacetonide (active moiety of); Triamcinolone Benetonide (is active moiety of) ... View More ... Drug Indication Visualisation during vitrectomy Triamcinolone Acetonide is a synthetic glucocorticoid with potent anti-inflammatory, immunosuppressive, and anti-proliferative properties[1][2][3][4][5] - Its core mechanism involves binding to GR, regulating transcription of anti-inflammatory (IL-10) and pro-inflammatory (TNFα, MMP-13) genes, activating M2 macrophages, and enhancing tissue matrix synthesis[2][3] - Clinical indications include ocular inflammation (retinal neovascularization), osteoarthritis, atopic dermatitis, and other inflammatory conditions, administered via topical, intravitreal, or intra-articular routes[1][2][3][4][5] - It is FDA-approved for multiple indications and exhibits tissue-specific efficacy, such as preserving articular cartilage matrix in OA and improving skin barrier function in atopic dermatitis[2][4][5] - Combined with hyaluronan, it shows synergistic effects on chondrocyte matrix metabolism, enhancing therapeutic efficacy in OA[2] |
Solubility Data
| Solubility (In Vitro) |
|
|||
| Solubility (In Vivo) |
Solubility in Formulation 1: ≥ 2.08 mg/mL (4.79 mM) (saturation unknown) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 20.8 mg/mL clear DMSO stock solution to 400 μL PEG300 and mix evenly; then add 50 μL Tween-80 to the above solution and mix evenly; then add 450 μL normal saline to adjust the volume to 1 mL. Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH₂ O to obtain a clear solution. Solubility in Formulation 2: ≥ 2.08 mg/mL (4.79 mM) (saturation unknown) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 20.8 mg/mL clear DMSO stock solution to 900 μL of 20% SBE-β-CD physiological saline solution and mix evenly. Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Solubility in Formulation 3: ≥ 2.08 mg/mL (4.79 mM) (saturation unknown) in 10% DMSO + 90% Corn Oil (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 20.8 mg/mL clear DMSO stock solution to 900 μL of corn oil and mix evenly. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.3015 mL | 11.5075 mL | 23.0150 mL | |
| 5 mM | 0.4603 mL | 2.3015 mL | 4.6030 mL | |
| 10 mM | 0.2301 mL | 1.1507 mL | 2.3015 mL |