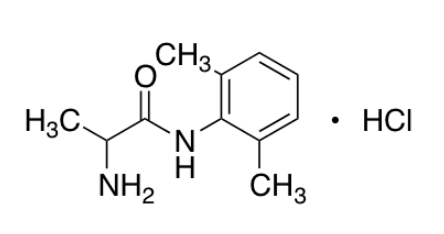
Tocainide HCl is a bioactive molecule.
Physicochemical Properties
| Molecular Formula | C11H16N2O.HCL |
| Molecular Weight | 228.71848 |
| Exact Mass | 228.103 |
| CAS # | 35891-93-1 |
| PubChem CID | 108173 |
| Appearance | Off-white to gray solid powder |
| Boiling Point | 330.1ºC at 760 mmHg |
| Melting Point | 244-245 °C |
| Flash Point | 153.5ºC |
| LogP | 3.164 |
| Hydrogen Bond Donor Count | 3 |
| Hydrogen Bond Acceptor Count | 2 |
| Rotatable Bond Count | 2 |
| Heavy Atom Count | 15 |
| Complexity | 196 |
| Defined Atom Stereocenter Count | 0 |
| InChi Key | AMZACPWEJDQXGW-UHFFFAOYSA-N |
| InChi Code | InChI=1S/C11H16N2O.ClH/c1-7-5-4-6-8(2)10(7)13-11(14)9(3)12;/h4-6,9H,12H2,1-3H3,(H,13,14);1H |
| Chemical Name | 2-amino-N-(2,6-dimethylphenyl)propanamide;hydrochloride |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month Note: Please store this product in a sealed and protected environment (e.g. under nitrogen), avoid exposure to moisture. |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
Voltage-Gated Sodium Channels (VGSCs) (skeletal muscle NaV1.4: half-maximal inhibitory concentration [IC50] = 12.3 μM; binding constant [Kd] = 8.7 μM) [2] |
| ln Vitro |
Sodium channel blocking activity: Tocainide HCl exhibited use-dependent block of skeletal muscle voltage-gated sodium channels (NaV1.4) expressed in Xenopus oocytes: at 10 μM, it reduced peak sodium current by ~35% at low stimulation frequency (0.1 Hz) and by ~68% at high frequency (10 Hz) (patch-clamp recording) [2] - Antiarrhythmic activity in isolated cardiac tissues: Tocainide HCl (5-20 μM) prolonged the effective refractory period (ERP) of isolated guinea pig papillary muscles by ~28% (20 μM) and reduced the maximum rate of rise of the action potential (Vmax) by ~32% (20 μM), suppressing ectopic electrical activity [1] - Selectivity for sodium channels: Tocainide HCl (up to 30 μM) showed no significant effect on cardiac potassium channels or calcium channels, confirming specificity for sodium channels [1] - Structure-activity relationship: The N-benzyl moiety of Tocainide HCl was critical for high affinity to NaV1.4; modification of this moiety reduced binding affinity by 3-5 fold [2] |
| ln Vivo |
Antiarrhythmic efficacy in canine ventricular arrhythmia model: Intravenous Tocainide HCl (5 mg/kg) converted electrically induced ventricular tachycardia (VT) to sinus rhythm in 8/10 dogs; oral administration (20 mg/kg) prevented VT induction in 7/10 dogs for up to 6 hours [1] - Efficacy in rat digitalis-induced arrhythmia model: Oral Tocainide HCl (30 mg/kg) reduced the incidence of ventricular premature beats (VPBs) by ~75% and prevented ventricular fibrillation (VF) in 60% of rats compared to vehicle control [1] - Hemodynamic effects: Tocainide HCl (10 mg/kg, i.v.) had no significant effect on mean arterial pressure (MAP) or heart rate (HR) in anesthetized dogs, with MAP changing by <5% and HR by <3% [1] |
| Enzyme Assay |
Sodium channel binding assay: Xenopus oocytes were injected with cRNA encoding human NaV1.4 sodium channels and cultured for 2-3 days to allow channel expression. Oocytes were voltage-clamped using two-electrode voltage clamp technique, and sodium currents were recorded in the presence of serial dilutions of Tocainide HCl (1-30 μM). Current-voltage relationships and use-dependent block were analyzed to calculate IC50 and Kd values [2] |
| Cell Assay |
Cardiac myocyte action potential assay: Isolated guinea pig papillary muscles were mounted in tissue baths with oxygenated Tyrode’s solution. Tocainide HCl (5-20 μM) was added, and action potentials were recorded using intracellular microelectrodes. Parameters including ERP, Vmax, and action potential duration (APD90) were measured and analyzed [1] - Sodium current recording in oocytes: NaV1.4-expressing Xenopus oocytes were placed in recording buffer, and voltage steps from -120 mV to +40 mV were applied to evoke sodium currents. Tocainide HCl was perfused into the bath, and currents were recorded at different stimulation frequencies (0.1-10 Hz) to assess use-dependent block [2] |
| Animal Protocol |
Canine ventricular arrhythmia model: Adult mongrel dogs (15-20 kg) were anesthetized, and electrodes were implanted to electrically induce VT (burst pacing at 200 bpm for 10 seconds). Tocainide HCl was administered intravenously (5 mg/kg) or orally (20 mg/kg, 1 hour before induction), and ECG was monitored for 6 hours to assess arrhythmia conversion and prevention [1] - Rat digitalis-induced arrhythmia model: Male Sprague-Dawley rats (250-300 g) were subcutaneously injected with digoxin (0.8 mg/kg) to induce arrhythmias. Tocainide HCl (30 mg/kg) was administered orally 30 minutes after digoxin injection, and ECG was recorded for 4 hours to count VPBs and assess VF incidence [1] - Hemodynamic monitoring model: Anesthetized dogs were instrumented with arterial catheters to measure MAP and HR. Tocainide HCl (10 mg/kg) was administered intravenously, and hemodynamic parameters were recorded at 15, 30, 60, and 120 minutes post-administration [1] |
| ADME/Pharmacokinetics |
Oral absorption: Tocainide HCl was rapidly and completely absorbed after oral administration in humans, with peak plasma concentration (Cmax) of 3.2 ± 0.5 μg/mL achieved at 1-2 hours post-dose (200 mg oral dose) [1] - Bioavailability: Oral bioavailability in humans was ~90%, with minimal first-pass metabolism [1] - Distribution: Volume of distribution (Vd) was 1.2 ± 0.2 L/kg in humans; it distributed widely into tissues, including cardiac muscle and central nervous system [1] - Elimination: Plasma half-life (t1/2) was 12 ± 2 hours in humans; ~70% of the dose was excreted unchanged in urine, and ~20% was metabolized in the liver to inactive metabolites [1] |
| Toxicity/Toxicokinetics |
Acute toxicity: Intravenous LD50 of Tocainide HCl was 85 mg/kg in mice and 60 mg/kg in rats; oral LD50 was > 500 mg/kg in both species [1] - Human adverse effects: The most common adverse reactions were central nervous system (CNS) symptoms (dizziness, tremor, paresthesia) reported in 25-30% of patients, and gastrointestinal symptoms (nausea, vomiting) in 10-15% of patients; symptoms were dose-related and reversible [1] - Plasma protein binding: Tocainide HCl had a plasma protein binding rate of ~10% in humans (ultrafiltration method) [1] - No significant hepatotoxicity or nephrotoxicity was observed in clinical trials, with serum ALT, AST, BUN, and Cr levels remaining within normal ranges [1] |
| References |
[1]. Chemistry, pharmacology, antiarrhythmic efficacy and adverse effects of tocainide hydrochloride, an orally active structural analog of lidocaine. Pharmacotherapy. 1983 Nov-Dec;3(6):316-23. [2]. Optimal requirements for high affinity and use-dependent block of skeletal muscle sodium channel by N-benzyl analogs of tocainide-like compounds.Mol Pharmacol. 2003 Oct;64(4):932-45. |
| Additional Infomation |
Tocainide Hydrochloride is the hydrochloride salt form of tocainide, a primary amine analog of lidocaine exhibiting class 1b antiarrhythmic property. Tocainide hydrochloride stabilizes the neuronal membrane by reversibly binding to and blocking open and inactivated voltage-gated sodium channels. This inhibits the inward sodium current required for the initiation and conduction of impulses and reduces the excitability of myocardial cells. This agent reduces the rate of rise and amplitude, and shortens the action-potential duration (APD) in both the Purkinje and muscle fibers. Tocainide also shortens the effective refractory period (ERP) of Purkinje fibers resulting in an increased the ERP/APD ratio. Overall these effects lead to the slowing of nerve impulses and stabilization of the heartbeat. An antiarrhythmic agent which exerts a potential- and frequency-dependent block of SODIUM CHANNELS. Tocainide HCl is an orally active class IB antiarrhythmic drug and a structural analog of lidocaine [1] - Its antiarrhythmic mechanism involves blocking voltage-gated sodium channels, preferentially inhibiting inactivated channels (use-dependent block), which prolongs ERP and suppresses abnormal ventricular electrical activity [1][2] - It is indicated for the treatment of symptomatic ventricular arrhythmias (e.g., ventricular tachycardia, ventricular premature beats) in patients unresponsive to other antiarrhythmic agents [1] - Unlike lidocaine, Tocainide HCl has good oral bioavailability and a long half-life, allowing for twice-daily dosing [1] |
Solubility Data
| Solubility (In Vitro) | May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 4.3722 mL | 21.8608 mL | 43.7216 mL | |
| 5 mM | 0.8744 mL | 4.3722 mL | 8.7443 mL | |
| 10 mM | 0.4372 mL | 2.1861 mL | 4.3722 mL |