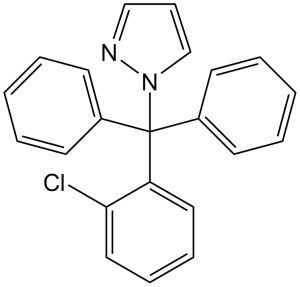
TRAM-34 (TRAM34; TRAM 34 Triarylmethane-34) is an inhibitor of Ca2+-activated K+ channel (IKCa1, KCa3.1) with important biological activity. It inhibits Ca2+-activated K+ channel with a Kd of 20 nM, and exhibits 200- to 1500-fold higher selectivity over cloasely related ion channels..
Physicochemical Properties
| Molecular Formula | C22H17CLN2 | |
| Molecular Weight | 344.84 | |
| Exact Mass | 344.108 | |
| Elemental Analysis | C, 76.63; H, 4.97; Cl, 10.28; N, 8.12 | |
| CAS # | 289905-88-0 | |
| Related CAS # |
|
|
| PubChem CID | 656734 | |
| Appearance | White to off-white solid powder | |
| Density | 1.1±0.1 g/cm3 | |
| Boiling Point | 510.2±50.0 °C at 760 mmHg | |
| Melting Point | 145-147ºC | |
| Flash Point | 262.4±30.1 °C | |
| Vapour Pressure | 0.0±1.3 mmHg at 25°C | |
| Index of Refraction | 1.617 | |
| LogP | 5.65 | |
| Hydrogen Bond Donor Count | 0 | |
| Hydrogen Bond Acceptor Count | 1 | |
| Rotatable Bond Count | 4 | |
| Heavy Atom Count | 25 | |
| Complexity | 396 | |
| Defined Atom Stereocenter Count | 0 | |
| InChi Key | KBFUQFVFYYBHBT-UHFFFAOYSA-N | |
| InChi Code | InChI=1S/C22H17ClN2/c23-21-15-8-7-14-20(21)22(25-17-9-16-24-25,18-10-3-1-4-11-18)19-12-5-2-6-13-19/h1-17H | |
| Chemical Name | 1-[(2-chlorophenyl)-diphenylmethyl]pyrazole | |
| Synonyms |
|
|
| HS Tariff Code | 2934.99.9001 | |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
|
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
Calcium-activated K+ channel (IKCa1) (Kd=20 nM) Intermediate-conductance Ca²⁺-activated K⁺ channel (IKCa1/KCa3.1) (IC50: ~20 nM)[1] |
| ln Vitro |
TRAM-34 selectively blocks IKCa1 currents (Kd=25 nM), and TRAM-34 also blocks IKCa1 currents in human T84 colon epithelial cells with same efficacy (Kd= 22 nM). TRAM-34 blocks cloned and native IKCa1 channels in human T cells with a Kd of 20-25 nM and is 200 to 1500 times more selective than other ion channels. The dosage response curve demonstrates that 1 μM calcium in the pipette has a Kd of 20±3 nM and a Hill coefficient of 1.2 [1]. TRAM-34 is a selective inhibitor of KCa 3.1 channels that boosts or lowers cell proliferation depending on concentration. At intermediate concentrations (3-10 μM) TRAM-34 enhances cell proliferation, but at higher concentrations (20-100 μM) TRAM-34 lowers cell proliferation. The augmentation of cell proliferation generated by TRAM-34 was prevented by the estrogen receptor antagonists ICI182,780 and Tamoxifen. TRAM-34 also enhances progesterone receptor mRNA expression, decreases estrogen receptor-α mRNA expression, and diminishes the binding of radiolabeled estrogen to the MCF-7 estrogen receptor, in each case imitating 17β-estrogen receptor The involvement of glycol [2]. In human T cells, B cells, and macrophages, TRAM-34 (10-100 nM) dose-dependently inhibited IKCa1-mediated potassium currents and immune cell functions. At 50 nM, it suppressed T cell proliferation by 50% and reduced interleukin-2 (IL-2) secretion by 60%. It also inhibited B cell antibody production and macrophage phagocytosis at 100 nM, suggesting potential immunosuppressive activity[1] - In estrogen receptor-positive (ER⁺) breast cancer cells (MCF-7, T47D), TRAM-34 (1-10 μM) stimulated cell proliferation in a concentration-dependent manner. At 10 μM, it increased MCF-7 cell viability by 40% compared to the control. Western blot analysis showed the drug induced phosphorylation of ERα (Ser118) and upregulated cyclin D1 expression, and this effect was blocked by the ER antagonist fulvestrant[2] - In primary rat cortical neurons subjected to oxygen-glucose deprivation (OGD), TRAM-34 (0.1-1 μM) reduced neuronal apoptosis by 35% at 0.5 μM. It also decreased reactive oxygen species (ROS) generation by 42% and inhibited caspase-3 activation, as confirmed by TUNEL staining and Western blot[3] |
| ln Vivo |
Mice (n = 5) given a single intravenous dosage of TRAM-34 (0.5 mg/kg; 29 μM) for seven days showed no abnormalities in their clinical appearance. The TRAM-34 treatment group's body weight data (Day 1: 17.8 g; Day 7: 27.0 g) matched the vehicle-injected control mice's body weight data (Day 1: 17.4 g; Day 7: 23.4 g). Overall, at 500–1,000 times the amount required to block the channel, TRAM-34 is not acutely hazardous, according to results from these small toxicity experiments [1]. Hematoxylin and eosin (H&E) measurements of lesion area were considerably decreased with TRAM-34 treatment; the mean infarct size decreased from 22.6±3.6% in the control group (n=8) to 10 mg/kg TRAM-34. In rats treated with 40 mg/kg TRAM-34, the percentage decreased to 8.1±1.9% (n=8; P=0.004) from 11.3±2.8% in rats (n=6, mean±s.e.m., P=0.039). Additionally, this treatment helps to lessen brain shrinkage. But only the 40 mg/kg TRAM-34 group's results were statistically significant (P=0.013), but the 10 mg/kg group's results were not (P=0.11) [3]. In Sprague-Dawley rats with middle cerebral artery occlusion (MCAO)-induced ischemia/reperfusion stroke, intravenous administration of TRAM-34 (3 mg/kg, administered immediately after reperfusion and 24 hours post-reperfusion) reduced cerebral infarct volume by 40% compared to the vehicle control. It improved neurological deficit scores by 35% on day 7 and decreased microglial activation and neutrophil infiltration in the ischemic penumbra[3] |
| Enzyme Assay |
ER competitive binding assay[2] Competitive binding assays were performed as follows. MCF-7 cell protein (250 µg) was incubated at room temperature for 2 h in TEDG buffer in the presence of 0.1 nM [2,4,6,7,16,17-3H(N)]-oestradiol ([3H]-E2) (110 Ci·mmol−1) in a total final volume of 500 µL. Non-specific binding was assessed in the presence of a 100-fold excess of non-radioactive E2. TRAM-34 and E2 standards were diluted in phenol red-free 5% DCC-FBS MEM containing supplements before being added to the cytosolic protein. A vehicle control comprised of 5% DCC-FBS MEM containing supplements with 0.7% DMSO. To separate ER-bound [3H]-E2 from unbound [3H]-E2, 250 µL of hydroxylapatite (HAP, 60% in TEDG buffer) was added, the mixture was vortexed every 5 min over 15 min and centrifuged at 1000×g for 10 min. The HAP-[3H]-E2-ER complex was washed with TEDG buffer, centrifuged and the wash step repeated. To elute [3H]-E2 from the HAP-[3H]-E2-ER complex, 500 µL of 100% ethanol was added and the mixture then incubated for 15 min and centrifuged at 1034×g for 10 min. The separated [3H]-E2 was removed and added to 2 mL of scintillation fluid. Radioactivity was quantified using a Beckman LS 5000TA scintillation counter. Competition of [3H]-E2 with TRAM-34 was assayed in quadruplicate on four independent protein extractions. An apparent dissociation constant of 0.135 ± 0.034 nM (n= 3) and a maximum binding capacity of 48.3 ± 5.4 fmol·mg−1 (n= 3) were determined by Scatchard analysis. IKCa1/KCa3.1 channel activity assay: HEK293 cells stably expressing human IKCa1 were seeded on glass coverslips and cultured for 24-48 hours. Whole-cell patch-clamp recordings were performed to measure IKCa1 currents. TRAM-34 was applied to the extracellular solution at gradient concentrations (1-100 nM). The voltage protocol included a holding potential of -60 mV, depolarizing steps to +40 mV (500 ms) to activate the channel, and repolarization to -60 mV. Peak current amplitude was normalized to the control to calculate the blocking rate[1] |
| Cell Assay |
[3H]Thymidine Incorporation Assay.[1] Resting or 2-day-activated (10 nM PMA or 5 ng/ml anti-CD3 Ab) PBMCs were seeded at 2 × 105 cells per well in culture medium in flat-bottom 96-well plates (final volume 200 μl). Cells preincubated with drug (60 min) were stimulated with mitogen (10 nM PMA + 175 nM ionomycin or 5 ng/ml anti-CD3 Ab) for 48 h. Triated thymidine ([3H]TdR) (1 μCi per well) was added for the last 6 h. Cells were harvested onto glass fiber filters and radioactivity measured in a scintillation counter. Flow Cytometric Measurement of Cell Viability.[1] Cells were seeded at 5 × 105 cells/ml (Jurkat E6–1, MEL cells, human T lymphocytes) or 105 cells/ml (C2F3 myoblasts, CHO, COS-7, L929, NGP and NLF neuroblastoma, RBL-2H3) in 12-well plates. Drug (5 μM) was added in a final DMSO concentration of 0.1% which was found not to affect cell viability. After 48 h cells were harvested by suction (suspension cells) or by trypsinization (adherent cell lines), centrifuged, resuspended in 0.5 ml PBS containing 1 μg/ml propidium iodide (PI), and red fluorescence measured on a FACScan flow cytometer. The percentage of dead cells was determined by their PI uptake, 104 cells of every sample being analyzed. Immune cell function assay: Human peripheral blood T cells, B cells, and macrophages were isolated and seeded in 96-well plates. TRAM-34 (10 nM, 50 nM, 100 nM) was added, and cells were cultured for 72 hours (T/B cells) or 24 hours (macrophages). T/B cell proliferation was measured by [³H]-thymidine incorporation, IL-2 secretion by ELISA, and macrophage phagocytosis by fluorescent bead uptake assay[1] - Breast cancer cell proliferation assay: MCF-7 and T47D cells were seeded in 96-well plates (1×10³ cells/well) and cultured for 24 hours. TRAM-34 (1 μM, 5 μM, 10 μM) was added, and incubation continued for 48-72 hours. Cell viability was detected by MTT assay. For protein analysis, cells were seeded in 6-well plates, treated with 10 μM TRAM-34 for 24 hours, and ERα phosphorylation and cyclin D1 expression were analyzed by Western blot[2] - Neuronal apoptosis assay: Primary rat cortical neurons were isolated and cultured for 7 days. Neurons were subjected to OGD for 2 hours, followed by reoxygenation. TRAM-34 (0.1 μM, 0.5 μM, 1 μM) was added during reoxygenation. After 24 hours, neuronal apoptosis was detected by TUNEL staining, ROS generation by DCFH-DA fluorescent probe, and caspase-3 activation by Western blot[3] |
| Animal Protocol |
Formulated in peanut oil; 120 mg/kg/day; s.c. injection Sprague-Dawley rats subjected to BCI of the left CA by use of a 2F Fogarty embolectomy catheter Acute in Vivo Toxicity Determinations.[1] Five CF-1BR mice (17–19 g) were injected intravenously with a single 1.0-ml dose of 0.5 mg/kg TRAM-34 (in mammalian Ringer solution with 1% ethanol and 2.5% BSA). Five control mice were injected with an equal volume of the vehicle. Mice were observed for adverse effects immediately after dosing, at 4 h after injection and daily for 7 days. The filament was kept in place for 90 minutes and then withdrawn and removed from the blood vessel to restore blood supply. Rats received TRAM-34 at 10 mg/kg, 40 mg/kg or vehicle (Miglyol 812 neutral oil at 1 μL/g) twice daily intraperitoneally for 7 days starting 12 hours after reperfusion.[3] Pharmacokinetics, Brain Concentrations, and Plasma Protein Binding of TRAM-34[3] TRAM-34 was synthesized in our laboratory as previously described (Wulff et al, 2000) and its chemical identity and purity checked by 1H NMR and high pressure liquid chromatography/mass spectrometry (HPLC/MS). For intravenous application, TRAM-34 was dissolved at 5 mg/mL in a mixture of 25% CremophorEL and 75% phosphate-buffered saline and then injected at 10 mg/kg into the tail vein of male Wistar rats. At various time points after the injection, ∼100 to 200 μL of blood was collected from a tail nick into EDTA blood sample collection tubes. For simultaneous determinations of plasma and brain concentrations, TRAM-34 was dissolved in Miglyol 812 neutral oil (caprylic/capric triglyceride) at 10 or 40 mg/mL and injected intraperitoneally at 10 or 40 mg/kg. Blood samples were taken by cardiac puncture under deep isoflurane anesthesia. The right atrium was then cut open and 20 mL of saline slowly injected into the left ventricle to flush the blood out of the circulation. The rats were then sacrificed and brains removed. Plasma was separated by centrifugation and samples stored at −80 °C for pending analysis. Plasma and homogenized brain samples were purified using C18 solid phase extraction cartridges. Elutioned fractions corresponding to TRAM-34 were dried under nitrogen and reconstituted in acetonitrile. LC/MS analysis was performed with a Hewlett-Packard 1100 series HPLC stack equipped with a Merck KGaA RT 250-4 LiChrosorb RP-18 column interfaced to a Finnigan LCQ Classic MS. The mobile phase consisted of acetonitrile and water, both containing 0.2% formic acid. With a flow rate of 1.0 mL/min, the gradient was ramped from 20/80 to 70/30 in 5 minutes, then to 80/20 over 11 minutes, to 5/95 till 16.5 minutes, and finally back to 80/20 till 38 minutes. With the column temperature maintained at 30 °C, TRAM-34 eluted at 14.4 minutes and was detected by a variable wavelength detector set to 190 nm and the MS in series. Using electrospray ionization/ion trap MS (capillary temperature 270 °C, capillary voltage 1 V, tube lens offset −15 V, positive ion mode), TRAM-34 was quantified by its base peak of 277 m/z (2-chlorotrityl fragment) and concentrations calculated with a 5-point calibration curve from 25 nmol/L to 2.5 μmol/L. Concentrations above 2.5 μmol/L were quantified by their UV absorption at 190 nm. The related compound TRAM-46 (base peak of 261 m/z, 2-fluorotrityl fragment) was used as an internal standard. The percentage of plasma protein binding for TRAM-34 was determined by ultrafiltration. Rat plasma was spiked with 50 and 100 μmol/L TRAM-34 in 1% dimethylsulfoxide and the sample loaded onto a Microcon YM-100 Centrifugal Filter and centrifuged at 14,000 g for 15 minutes at room temperature. The centrifugate (=free TRAM-34) was directly analyzed for TRAM-34 by HPLC-MS. The retentate was collected by inverting the filter into an Eppendorf tube and spinning at 14,000 g for 15 minutes. The retentate then underwent sample preparation as per the above-described procedure for determining total TRAM-34 concentration in plasma. The plasma protein binding of TRAM-34 was found to be 98±0.5% (n=3) and the unbound (=free) fraction 2.0±0.4%.[3] MCAO-induced ischemia/reperfusion stroke rat model: Male Sprague-Dawley rats (250-300 g) were subjected to MCAO using the intraluminal filament method for 90 minutes, followed by reperfusion. TRAM-34 was dissolved in DMSO and normal saline (DMSO final concentration ≤5%) and administered intravenously at 3 mg/kg immediately after reperfusion and again at 24 hours post-reperfusion. Control rats received an equal volume of vehicle. On day 7, rats were euthanized to measure cerebral infarct volume by TTC staining, and neurological deficit scores were evaluated using the Bederson scale[3] |
| Toxicity/Toxicokinetics |
In vitro toxicity: TRAM-34 showed low cytotoxicity to normal human fibroblasts and endothelial cells, with IC50 values >10 μM[1][2][3] |
| References |
[1]. Design of a potent and selective inhibitor of the intermediate-conductance Ca2+-activated K+ channel, IKCa1: a potential immunosuppressant. Proc Natl Acad Sci U S A. 2000 Jul 5;97(14):8151-6. [2]. The intermediate conductance Ca2+-activated K+ channel inhibitor TRAM-34 stimulates proliferation of breast cancer cells via activation of oestrogen receptors. Br J Pharmacol. 2010 Feb 1;159(3):650-8. [3]. The KCa3.1 blocker TRAM-34 reduces infarction and neurological deficit in a rat model of ischemia/reperfusion stroke. J Cereb Blood Flow Metab. 2011 Dec;31(12):2363-74. |
| Additional Infomation |
TRAM-34 is an organochlorine compound. TRAM-34 is a potent and selective inhibitor of the intermediate-conductance Ca²⁺-activated K⁺ channel (IKCa1/KCa3.1)[1] - It exhibits potential immunosuppressive activity by inhibiting the function of T cells, B cells, and macrophages, indicating potential applications in autoimmune diseases or organ transplantation[1] - In ER⁺ breast cancer cells, TRAM-34 stimulates cell proliferation via activating estrogen receptors, suggesting a potential risk in breast cancer patients[2] - The drug exerts neuroprotective effects in cerebral ischemia/reperfusion injury by reducing neuronal apoptosis, oxidative stress, and neuroinflammation, providing a potential therapeutic option for stroke[3] |
Solubility Data
| Solubility (In Vitro) |
|
|||
| Solubility (In Vivo) |
Solubility in Formulation 1: ≥ 2.08 mg/mL (6.03 mM) (saturation unknown) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 20.8 mg/mL clear DMSO stock solution to 400 μL PEG300 and mix evenly; then add 50 μL Tween-80 to the above solution and mix evenly; then add 450 μL normal saline to adjust the volume to 1 mL. Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH₂ O to obtain a clear solution. Solubility in Formulation 2: 2.08 mg/mL (6.03 mM) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (add these co-solvents sequentially from left to right, and one by one), suspension solution; with ultrasonication. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 20.8 mg/mL clear DMSO stock solution to 900 μL of 20% SBE-β-CD physiological saline solution and mix evenly. Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Solubility in Formulation 3: ≥ 2.08 mg/mL (6.03 mM) (saturation unknown) in 10% DMSO + 90% Corn Oil (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 20.8 mg/mL clear DMSO stock solution to 900 μL of corn oil and mix evenly.. Solubility in Formulation 4: 30% PEG400+0.5% Tween80+5% Propylene glycol : 30mg/mL Solubility in Formulation 5: 5 mg/mL (14.50 mM) in 20% SBE-β-CD in Saline (add these co-solvents sequentially from left to right, and one by one), suspension solution; with ultrasonication. Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.8999 mL | 14.4995 mL | 28.9990 mL | |
| 5 mM | 0.5800 mL | 2.8999 mL | 5.7998 mL | |
| 10 mM | 0.2900 mL | 1.4499 mL | 2.8999 mL |