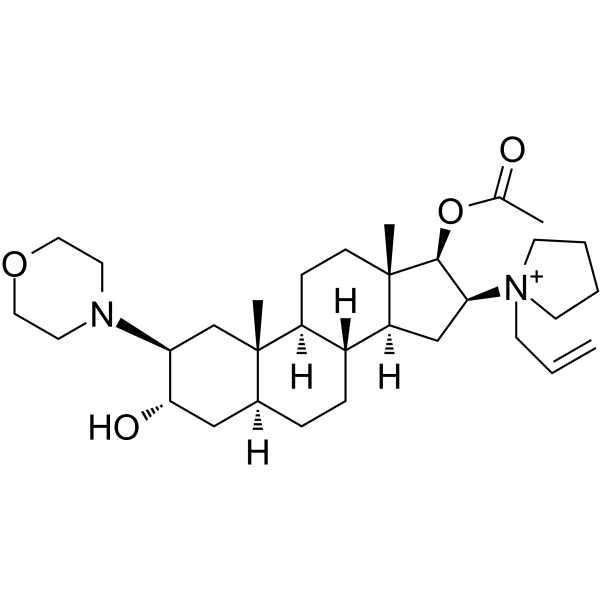
Physicochemical Properties
| Molecular Formula | C32H53N2O4+ |
| Molecular Weight | 529.77422 |
| Exact Mass | 529.40 |
| Elemental Analysis | C, 72.55; H, 10.08; N, 5.29; O, 12.08 |
| CAS # | 143558-00-3 |
| Related CAS # | Rocuronium Bromide;119302-91-9 |
| PubChem CID | 441290 |
| Appearance | Typically exists as solid at room temperature |
| LogP | 4.304 |
| Hydrogen Bond Donor Count | 1 |
| Hydrogen Bond Acceptor Count | 5 |
| Rotatable Bond Count | 6 |
| Heavy Atom Count | 38 |
| Complexity | 898 |
| Defined Atom Stereocenter Count | 10 |
| SMILES | O[C@@H]1[C@@H](N2CCOCC2)C[C@@]3(C)[C@](CC[C@]4([H])[C@]3([H])CC[C@@]5(C)[C@@]4([H])C[C@H]([N+]6(CC=C)CCCC6)[C@@H]5OC(C)=O)([H])C1 |
| InChi Key | YXRDKMPIGHSVRX-OOJCLDBCSA-N |
| InChi Code | InChI=1S/C32H53N2O4/c1-5-14-34(15-6-7-16-34)28-20-26-24-9-8-23-19-29(36)27(33-12-17-37-18-13-33)21-32(23,4)25(24)10-11-31(26,3)30(28)38-22(2)35/h5,23-30,36H,1,6-21H2,2-4H3/q+1/t23-,24+,25-,26-,27-,28-,29-,30-,31-,32-/m0/s1 |
| Chemical Name | [(2S,3S,5S,8R,9S,10S,13S,14S,16S,17R)-3-hydroxy-10,13-dimethyl-2-morpholin-4-yl-16-(1-prop-2-enylpyrrolidin-1-ium-1-yl)-2,3,4,5,6,7,8,9,11,12,14,15,16,17-tetradecahydro-1H-cyclopenta[a]phenanthren-17-yl] acetate |
| Synonyms | Rocuronium; 143558-00-3; Zemuron; Rocuronium ion; Rocuronium cation; UNII-WRE554RFEZ; WRE554RFEZ; CHEBI:8884; |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets | Non-depolarizing neuromuscular blocker; muscle relaxant |
| ADME/Pharmacokinetics |
Absorption, Distribution and Excretion Poorly absorbed from the GI tract. Studies of distribution, metabolism, and excretion in cats and dogs indicate that rocuronium is eliminated primarily by the liver. 0.3 L/kg [3 to <12 mos] 0.26 L/kg [1 to <3 yrs] 0.21 L/kg [3 to <8 yrs] 0.25 L/kg/hr [Adults (Ages 27 to 58 years)] 0.21 L/kg/hr [Geriatrics (>=65 yrs)] 0.16 L/kg/hr [Normal ewnal and hepatice function] 0.13 L/kg/hr [Renal transplant patients] 0.13 L/kg/hr [Hepatic dysfunction patients] 0.35 +/- 0.08 L/kg/hr [Pediatric Patients 3 to <12 mos] 0.32 +/- 0.07 L/kg/hr [Pediatric Patients 1 to 3 yrs] 0.44 +/- 0.16 L/kg/hr [Pediatric Patients 3 to 8 yrs] Metabolism / Metabolites Rocuronium is metabolized to a less active metabolite, 17-desacetyl-rocuronium, and is eliminated primarily by the liver. Biological Half-Life The rapid distribution half-life is 1-2 minutes and the slower distribution half-life is 14-18 minutes. Renal impairment has no net effect on half-life, however, half-life is almost doubled in patients with impaired liver function. |
| Toxicity/Toxicokinetics |
Effects During Pregnancy and Lactation ◉ Summary of Use during Lactation Limited information on the use of rocuronium during breastfeeding indicates that no adverse infant effects occur. Because it is short acting, highly polar and poorly absorbed orally, it is not likely to reach the breastmilk in high concentration or to reach the bloodstream of the infant. When a combination of anesthetic agents is used for a procedure, follow the recommendations for the most problematic medication used during the procedure. General anesthesia for cesarean section using rocuronium as a component may delay the onset of lactation. ◉ Effects in Breastfed Infants Four mothers who were breastfeeding 3- to 5-month-old infants underwent general anesthesia were given intravenous propofol and remifentanil as induction agents and rocuronium 0.5 mg/kg for intubation. After induction, propofol was stopped and xenon inhalation was used to maintain anesthesia for between 57 and 70 minutes. Infants resumed breastfeeding from 1.5 to 5 hours after the end of surgery. None of the infants had noticeable symptoms of dizziness or drowsiness. All infants fared well at home after their mothers were discharged with no adverse events noticed at home. ◉ Effects on Lactation and Breastmilk A randomized study compared the effects of cesarean section using general anesthesia, spinal anesthesia, or epidural anesthesia, to normal vaginal delivery on serum prolactin and oxytocin as well as time to initiation of lactation. General anesthesia was performed using propofol 2 mg/kg and rocuronium 0.6 mg/kg for induction, followed by sevoflurane and rocuronium 0.15 mg/kg as needed. After delivery, patients in all groups received an infusion of oxytocin 30 international units in 1 L of saline, and 0.2 mg of methylergonovine if they were not hypertensive. Fentanyl 1 to 1.5 mcg/kg was administered after delivery to the general anesthesia group. Patients in the general anesthesia group (n = 21) had higher post-procedure prolactin levels and a longer mean time to lactation initiation (25 hours) than in the other groups (10.8 to 11.8 hours). Postpartum oxytocin levels in the nonmedicated vaginal delivery group were higher than in the general and spinal anesthesia groups. Protein Binding Approximately 30% bound to human plasma proteins. |
| References |
[1]. Konishi J, Suzuki T, Kondo Y, Baba M, Ogawa S. Rocuronium and sugammadex used effectively for electroconvulsive therapy in a patient with Brugada syndrome. J ECT. 2012 Jun;28(2):e21-2. [2]. Zhang Y, Xiang Y, Liu J. Prevention of pain on injection of rocuronium: a comparison of lidocaine with different doses of parecoxib. J Clin Anesth. 2012 Jul 2. [3]. Suzuki T, Nameki K, Shimizu H, Shimizu Y, Nakamura R, Ogawa S. Efficacy of rocuronium and sugammadex in a patient with dermatomyositis. Br J Anaesth. 2012 Apr;108(4):703. [4]. Illodo Miramontes G, Doniz Campos M, Filgueira Garrido P, Vázquez Martínez A. Rocuronium used in rapid sequence intubation and reversal with sugammadex in a patient with myasthenia gravis.Rev Esp Anestesiol Reanim. 2011 Dec;58(10):626-7. [5]. García Sánchez JI, Martínez Hurtado ED, Tordecilla Echenique YY, Santa-Ursula TJ. Rocuronium used after sugammadex.Rev Esp Anestesiol Reanim. 2011 Dec;58(10):620-1. |
| Additional Infomation |
Rocuronium is a 5alpha-androstane compound having 3alpha-hydroxy-, 17beta-acetoxy-, 2beta-morpholino- and 16beta-N-allyllyrrolidinium substituents. It has a role as a neuromuscular agent, a muscle relaxant and a drug allergen. It is an androstane, a 3alpha-hydroxy steroid, a quaternary ammonium ion, an acetate ester, a member of morpholines and a tertiary amino compound. It derives from a hydride of a 5alpha-androstane. Rocuronium (rapid onset-curonium) is a desacetoxy analogue of vecuronium with a more rapid onset of action. It is an aminosteroid non-depolarizing neuromuscular blocker or muscle relaxant used in modern anaesthesia, to facilitate endotracheal intubation and to provide skeletal muscle relaxation during surgery or mechanical ventilation. Introduced in 1994, rocuronium has rapid onset, and intermediate duration of action. It is commonly marketed under the trade names Zemuron and Esmeron. The drug is associated with the risk of developing allergic reactions in some high-risk patients, such as those with asthma. However, there was a similar incidence of allergic reactions associated with other non-depolarizing neuromuscular blocking agents. [Sugammadex] is a γ-cyclodextrin derivative that has been introduced as a novel agent to reverse the action of rocuronium. Rocuronium is a Nondepolarizing Neuromuscular Blocker. The physiologic effect of rocuronium is by means of Neuromuscular Nondepolarizing Blockade. An androstanol non-depolarizing neuromuscular blocking agent. It has a mono-quaternary structure and is a weaker nicotinic antagonist than PANCURONIUM. See also: Rocuronium Bromide (active moiety of). Drug Indication For inpatients and outpatients as an adjunct to general anesthesia to facilitate both rapid sequence and routine tracheal intubation, and to provide skeletal muscle relaxation during surgery or mechanical ventilation. Mechanism of Action Rocuronium acts by competing for cholinergic receptors at the motor end-plate. This action is antagonized by acetylcholinesterase inhibitors, such as neostigmine and edrophonium. Rocuronium acts by competitively binding to nicotinic cholinergic receptors. The binding of vecuronium decreases the opportunity for acetylcholine to bind to the nicotinic receptor at the postjunctional membrane of the myoneural junction. As a result, depolarization is prevented, calcium ions are not released and muscle contraction does not occur. Evidence also suggests that nondepolarizing agents can affect ACh release. It has been hypothesized that nondepolarzing agents bind to postjunctional ("curare") receptors and may therefore interfere with the sodium and potassium flux, which is responsible for depolarization and repolarization of the membranes involved in muscle contraction. Pharmacodynamics Neuromuscular blocking agents are drugs that cause skeletal muscle relaxation primarily by causing a decreased response to the neurotransmitter acetylcholine (ACh) at the myoneural (neuromuscular) junction of skeletal muscle. At that site, ACh normally produces electrical depolarization of the postjunctional membrane of motor end-plate, which leads to conduction of muscle action potential and subsequently induces skeletal muscle contraction. Neuromuscular agents are classified as depolarizing or nondepolarizing. Rocuronium is a nondepolarizing neuromuscular blocking agent with a rapid to intermediate onset depending on dose and intermediate duration. Rocuronium, like vecuronium is longer acting in infants than in children. However, unlike vecuronium, rocuronium retains the characteristics of an intermediate-acting NMBD in infants. |
Solubility Data
| Solubility (In Vitro) | May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 1.8876 mL | 9.4381 mL | 18.8761 mL | |
| 5 mM | 0.3775 mL | 1.8876 mL | 3.7752 mL | |
| 10 mM | 0.1888 mL | 0.9438 mL | 1.8876 mL |