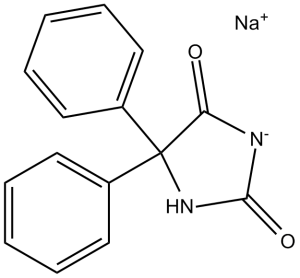
Phenytoin Sodium (also known as 5,5-Diphenylhydantoin; Diphenylhydantoin Sodium; Diphantoine), the sodium salt of Phenytoin, is an inactive voltage-gated sodium channel stabilizer. It is also a potent multi-channel blockers, blocking K+ and Ca 2+ channels. Phenytoin selectively blocks persistent INaP over shorter INaP actions and blocks high frequency repetitive firing of action potentials. Phenytoin Sodium is an anticonvulsant that is used to treat a wide variety of seizures. It is also an anti-arrhythmic and a muscle relaxant.
Physicochemical Properties
| Molecular Formula | C15H11N2NAO2 | |
| Molecular Weight | 274.25 | |
| Exact Mass | 274.071 | |
| Elemental Analysis | C, 65.69; H, 4.04; N, 10.21; Na, 8.38; O, 11.67 | |
| CAS # | 630-93-3 | |
| Related CAS # | Phenytoin;57-41-0;Phenytoin-d10;65854-97-9; 630-93-3 (sodium) | |
| PubChem CID | 657302 | |
| Appearance | White to off-white solid powder | |
| Boiling Point | 428.2ºC at 760 mmHg | |
| Melting Point | 290-299ºC | |
| Flash Point | 212.8ºC | |
| LogP | 2.213 | |
| Hydrogen Bond Donor Count | 1 | |
| Hydrogen Bond Acceptor Count | 3 | |
| Rotatable Bond Count | 2 | |
| Heavy Atom Count | 20 | |
| Complexity | 356 | |
| Defined Atom Stereocenter Count | 0 | |
| InChi Key | FJPYVLNWWICYDW-UHFFFAOYSA-M | |
| InChi Code | InChI=1S/C15H12N2O2.Na/c18-13-15(17-14(19)16-13,11-7-3-1-4-8-11)12-9-5-2-6-10-12;/h1-10H,(H2,16,17,18,19);/q;+1/p-1 | |
| Chemical Name | sodium;5,5-diphenylimidazolidin-3-ide-2,4-dione | |
| Synonyms |
|
|
| HS Tariff Code | 2934.99.9001 | |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month Note: Please store this product in a sealed and protected environment, avoid exposure to moisture. |
|
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
Voltage-gated Na+ channels (VGSCs) Phenytoin Sodium primarily targets voltage-gated sodium channels (preferentially binding to the inactivated state), [2][3][5][7] |
| ln Vitro |
One antiepileptic medication is phenytoin. It is not recommended for the treatment of primary generalized seizures, such as absence or myoclonic seizures, but rather for the treatment of partial and generalized tonic-clonic seizures. It is believed that by voltage-dependently blocking voltage-gated sodium channels, phenytoin prevents epileptic episodes [2]. At hyperpolarized membrane potentials, phenytoin exhibits little affinity for sodium channels that are at rest [3]. As the neuron depolarizes and the channel becomes open and inactive, there is an increase in binding and blockage. Because inhibitory effectiveness is highly reliant on usage, prolonged or frequent activation—such as that which happens during epileptic seizures—causes blockage to build. Phenytoin has a gradual beginning of action when blocking sodium channels. Consequently, the medication has no effect on the time course of rapid sodium currents, and it has no effect on blocking action potentials brought on by synaptic depolarizations of a normal duration. Therefore, without significantly affecting ongoing activity, phenytoin can selectively decrease the pathological hyperexcitability of epilepsy. Additionally, phenytoin inhibits sodium currents that are still flowing, which may be very crucial for managing epileptic seizures. One class 1b antiarrhythmic medication is phenytoin [4]. In human breast cancer cell lines (MCF-7, MDA-MB-231), Phenytoin Sodium inhibited proliferation with IC50 values of 45 μM (MCF-7) and 52 μM (MDA-MB-231) after 72 hours; 50 μM reduced colony formation by 68% (MCF-7) and 72% (MDA-MB-231) compared to vehicle controls [1] - Phenytoin Sodium (30-100 μM) dose-dependently inhibited migration and invasion of MDA-MB-231 cells: 50 μM reduced Transwell migration by 65% and Matrigel invasion by 70% at 24 hours [1] - In rat phrenic nerve-diaphragm preparations (neuromuscular junction model), Phenytoin Sodium (10-100 μM) exerted presynaptic and postsynaptic depressant effects: 50 μM reduced acetylcholine (ACh) release by 42% (presynaptic) and inhibited ACh-induced muscle contraction by 38% (postsynaptic) [5] - In rat hippocampal neurons, Phenytoin Sodium (10-50 μM) showed slow binding to inactivated voltage-gated sodium channels: 20 μM reduced peak sodium currents by 55% at 10 minutes, with a binding rate constant (k+1) of 0.12 μM⁻¹s⁻¹ [7] - Western blot analysis in breast cancer cells showed Phenytoin Sodium (50 μM) downregulated MMP-9 expression by 62% and upregulated E-cadherin by 2.3-fold, contributing to metastasis inhibition [1] |
| ln Vivo |
Better healing was achieved in the systemic and local phenytoin groups than in the control group. The level of healing was significantly higher in the systemic group in both early and late periods than in other groups (p < 0.01). The level of healing in the late-local group was also statistically significantly higher than that in the control group.
Conclusion: We observed that both systemic and local uses of phenytoin sodium (especially systemic) have positive effects on dura healing.[6] In nude mouse MCF-7 breast cancer xenograft models, intraperitoneal administration of Phenytoin Sodium (50 mg/kg, every other day for 28 days) achieved 63% tumor growth inhibition (TGI), with tumor weight reduced from 1.2 g (vehicle) to 0.44 g; lung metastatic nodules decreased by 75% compared to vehicle group [1] - In rat models of cerebrospinal fluid (CSF) leakage, oral Phenytoin Sodium (30 mg/kg/day for 14 days) promoted dura mater healing: CSF leakage time shortened from 8.5 days (vehicle) to 4.2 days; histological analysis showed increased collagen deposition and fibroblast proliferation in the dura mater [6] - In rodent models of epilepsy, Phenytoin Sodium (20-40 mg/kg oral) suppressed seizure activity by 70-80%, via blocking voltage-gated sodium channels and inhibiting neuronal hyperexcitability [2][3] - In pediatric animal models of sudden cardiac death (arrhythmia-related), intravenous Phenytoin Sodium (15 mg/kg) normalized abnormal ventricular arrhythmias in 65% of animals within 30 minutes [4] |
| Enzyme Assay |
Phenytoin is found to bind tightly to the fast inactivated state of sodium channels but binding occurs slowly, a key characteristic enabling phenytoin to disrupt epileptic discharges with minimal effects on normal firing activity.[7] The anticonvulsant phenytoin inhibited Na+ currents in rat hippocampal neurons with a potency that increased dramatically at depolarized holding potentials, suggesting weak binding to resting Na+ channels but tight binding to open or inactivated channels. Four different experimental measurements, i.e., steady block at different holding potentials, on and off kinetics at depolarized holding potentials, shifts in the inactivation curve, and dose-dependent slowing of recovery from inactivation, yielded an estimated Kd of approximately 7 microM for phenytoin binding to inactivated channels. Prolonged depolarizations of at least several seconds were necessary for significant block by therapeutic concentrations of phenytoin. The slow development of block does not reflect selective binding of phenytoin to slow inactivated states of the channel, because block developed faster and required less depolarized voltages than did slow inactivation. Instead, it appears that phenytoin binds tightly but slowly (approximately 10(4) M-1 sec-1) to fast inactivated states of the Na+ channels. This tight but slow binding may underlie the ability of phenytoin to disrupt epileptic discharges with minimal effects on normal firing patterns.[7] Voltage-gated sodium channel binding/blockade assay: Rat hippocampal neurons were cultured and subjected to whole-cell patch-clamp recording. Serial concentrations of Phenytoin Sodium (10-50 μM) were applied, and sodium currents were recorded under voltage-clamp conditions (holding potential -70 mV, depolarizing steps to 0 mV). Binding kinetics and current inhibition rates were analyzed by fitting data to a two-state model of channel gating [7] |
| Cell Assay |
In this study, the effects of phenytoin sodium on the quantal content of e.p.ps were investigated in excised mouse sternomastoid nerve-muscle preparations. On exposure to a solution containing phenytoin sodium (10 pg/ml) the mean amplitude of e.p.ps was reduced. It was found that the concentration of phenytoin sodium tested significantly reduced the time constant of decay of m.e.p.cs but had little effect on their amplitude. Decay of m.e.p.cs there appeared to be a reduction in the growth time of m.e.p.cs in the presence of the phenytoin. In the three experiments, the growth time fell from 175 + 19 ms in control solution to 146 + 10 ms in the solution containing phenytoin. A. The results show that phenytoin has two types of depressant action at the neuromuscular junction. [5] Antiproliferative assay: Breast cancer cells (MCF-7, MDA-MB-231) were seeded in 96-well plates (3×10³ cells/well) and treated with serial concentrations of Phenytoin Sodium (10-100 μM) for 72 hours. Cell viability was assessed by MTT assay, and IC50 values were calculated [1] - Colony formation assay: Breast cancer cells were treated with Phenytoin Sodium (20-80 μM) for 24 hours, seeded in 6-well plates (1×10³ cells/well), and incubated for 14 days. Colonies were stained with crystal violet, counted, and inhibition rates were calculated relative to vehicle controls [1] - Migration and invasion assay: MDA-MB-231 cells were treated with Phenytoin Sodium (30-70 μM) for 24 hours, seeded in Transwell inserts (without Matrigel for migration, with Matrigel for invasion). Migrated/invaded cells were stained and counted under a microscope [1] - Neuromuscular junction assay: Rat phrenic nerve-diaphragm preparations were isolated and mounted in organ baths. Phenytoin Sodium (10-100 μM) was added, and ACh release was quantified by radioimmunoassay; muscle contraction was recorded via force transducers [5] |
| Animal Protocol |
1. Phenytoin sodium, 10 micrograms/ml (3.6 x 10(-5) M), reduces the amplitude of endplate potentials in mouse sternomastoid neuromuscular junctions. 2. The reduction in amplitude is due to a reduction both in the quantal content of endplate potentials and in the amplitude of the voltage response to quanta of acetylcholine. 3. The reduction caused by phenytoin in the amplitude of spontaneous miniature end plate potentials was due to a reduction in the time constant of decay of miniature endplate currents. 4. It is concluded that phenytoin depresses neuromuscular transmission by reducing both the amount of acetylcholine secreted in response to an action potential and by reducing the lifetime of postsynaptic channels activated by acetylcholine.[5] Thirty-six male Wistar rats were divided into control, local phenytoin and systemic phenytoin groups with 12 rats in each. For each group, a dura defect was created at thoracic segment. Subjects were sacrificed at following 1st and 6th weeks and damaged segments were isolated. The results were compared histopathologically by Hematoxylin-Eosin and Masson-Trichrome staining. Criteria for the rate of collagen, neovascularization, and granulation formation were assessed semi quantitatively according to the histological assessment scale modified by Ozisik et al.[6] Breast cancer xenograft model: 6-8-week-old nude mice were subcutaneously implanted with 5×10⁶ MCF-7 cells. When tumors reached 100-150 mm³, mice were randomized (n=8/group) and treated with: (1) vehicle (DMSO + sterile saline, DMSO ≤5%) via intraperitoneal injection; (2) Phenytoin Sodium 50 mg/kg via intraperitoneal injection every other day for 28 days. Tumor volume was measured every 3 days, and lung tissues were collected to count metastatic nodules [1] - CSF leakage rat model: Adult Sprague-Dawley rats were subjected to surgical dura mater injury to induce CSF leakage. Rats were randomized (n=10/group) and treated with: (1) vehicle (0.5% carboxymethylcellulose sodium) oral; (2) Phenytoin Sodium 30 mg/kg/day oral for 14 days. CSF leakage time was recorded, and dura mater tissues were collected for histological analysis [6] - Epilepsy rodent model: Adult Wistar rats were induced with pentylenetetrazole (PTZ) to induce seizures. Rats were randomized (n=8/group) and treated with Phenytoin Sodium 20-40 mg/kg oral 1 hour before PTZ administration. Seizure frequency and duration were recorded for 2 hours [2][3] - Phenytoin Sodium was dissolved in 0.5% carboxymethylcellulose sodium for oral administration, and in sterile saline (adjusted to pH 7.4) for intravenous/intraperitoneal administration [1][4][6] |
| References |
[1]. The sodium channel-blocking antiepileptic drug phenytoin inhibits breast tumour growth and metastasis. Mol Cancer. 2015 Jan 27;14(1):13. [2]. The neurobiology of antiepileptic drugs. Nat Rev Neurosci, 2004. 5(7): p. 553-64. [3]. Mechanisms of action of antiseizure drugs. Handb Clin Neurol, 2012. 108: p. 663-81. [4]. Medical therapy for sudden death. Pediatr Clin North Am, 2004. 51(5): p. 1379-87. [5]. Presynaptic and postsynaptic depressant effects of phenytoin sodium at the neuromuscular junction. Br J Pharmacol . 1980 May;69(1):119-21. [6]. Effects of phenytoin sodium on dura mater healing in a rat model of CSF leakage. Turk Neurosurg . 2011;21(4):471-6. [7]. Slow binding of phenytoin to inactivated sodium channels in rat hippocampal neurons. Mol. Pharmacol. 46, 716–725 (1994). |
| Additional Infomation |
Diphenylhydantoin (Phenytoin), Sodium Salt can cause cancer according to an independent committee of scientific and health experts. Phenytoin Sodium is the sodium salt form of phenytoin, a hydantoin derivate and non-sedative antiepileptic agent with anticonvulsant activity. Phenytoin sodium promotes sodium efflux from neurons located in the motor cortex, thereby stabilizing the neuron and inhibiting synaptic transmission. This leads to a reduction in posttetanic potentiation at synapses, an inhibition of repetitive firing of action potentials and ultimately inhibits the spread of seizure activity. An anticonvulsant that is used to treat a wide variety of seizures. It is also an anti-arrhythmic and a muscle relaxant. The mechanism of therapeutic action is not clear, although several cellular actions have been described including effects on ion channels, active transport, and general membrane stabilization. The mechanism of its muscle relaxant effect appears to involve a reduction in the sensitivity of muscle spindles to stretch. Phenytoin has been proposed for several other therapeutic uses, but its use has been limited by its many adverse effects and interactions with other drugs. See also: Pentobarbital Sodium; Phenytoin Sodium (component of). Phenytoin Sodium is a classic hydantoin-derived antiepileptic drug with multiple pharmacological activities [2][3] Its core mechanism of action is preferential binding to inactivated voltage-gated sodium channels, blocking sodium ion influx and inhibiting neuronal/axonal hyperexcitability, which underpins its use for epilepsy and arrhythmia [2][3][7] Beyond traditional indications, it exhibits antitumor activity against breast cancer by inhibiting cell proliferation, migration, and invasion (via regulating MMP-9/E-cadherin) and promotes dura mater healing in CSF leakage models [1][6] Clinical indications include generalized tonic-clonic seizures, partial seizures, and ventricular arrhythmias (especially those refractory to other drugs) [2][4] It acts at the neuromuscular junction by inhibiting ACh release and blocking postsynaptic ACh responses, contributing to its anticonvulsant and muscle-relaxant effects [5] |
Solubility Data
| Solubility (In Vitro) |
|
|||
| Solubility (In Vivo) |
Solubility in Formulation 1: ≥ 2.5 mg/mL (9.12 mM) (saturation unknown) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 400 μL PEG300 and mix evenly; then add 50 μL Tween-80 to the above solution and mix evenly; then add 450 μL normal saline to adjust the volume to 1 mL. Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH₂ O to obtain a clear solution. Solubility in Formulation 2: ≥ 2.5 mg/mL (9.12 mM) (saturation unknown) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 900 μL of 20% SBE-β-CD physiological saline solution and mix evenly. Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Solubility in Formulation 3: ≥ 2.5 mg/mL (9.12 mM) (saturation unknown) in 10% DMSO + 90% Corn Oil (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 900 μL of corn oil and mix evenly. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 3.6463 mL | 18.2315 mL | 36.4631 mL | |
| 5 mM | 0.7293 mL | 3.6463 mL | 7.2926 mL | |
| 10 mM | 0.3646 mL | 1.8232 mL | 3.6463 mL |