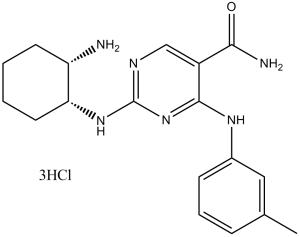
PRT-060318 3HCl (also known as PRT318 3HCl) is a novel, potent, selective inhibitor of the Syk tyrosine kinase, as an approach to HIT treatment. It was discovered that PRT-060318 is a strong inhibitor of pure Syk kinase. When PRT-060318 was assessed at a concentration of 50 nM in a wide range of kinase enzyme tests, Syk kinase was inhibited by 92%, while the activities of all other kinases retained more than 70% of their activity. Furthermore, PRT-060318 could inhibit the aggregation of human platelets induced by convulxin in a dose-responsive manner. Furthermore, it was discovered that PRT-060318 could inhibit the rises in intracellular calcium in platelets treated with convulxin in a dose-responsive manner.
Physicochemical Properties
| Molecular Formula | C18H26CL2N6O | |
| Molecular Weight | 413.3446 | |
| Exact Mass | 340.201 | |
| CAS # | 1194961-19-7 | |
| Related CAS # |
|
|
| PubChem CID | 11493841 | |
| Appearance | Light yellow to yellow solid powder | |
| Density | 1.3±0.1 g/cm3 | |
| Boiling Point | 602.1±65.0 °C at 760 mmHg | |
| Flash Point | 317.9±34.3 °C | |
| Vapour Pressure | 0.0±1.7 mmHg at 25°C | |
| Index of Refraction | 1.672 | |
| LogP | 1.62 | |
| Hydrogen Bond Donor Count | 4 | |
| Hydrogen Bond Acceptor Count | 6 | |
| Rotatable Bond Count | 5 | |
| Heavy Atom Count | 25 | |
| Complexity | 447 | |
| Defined Atom Stereocenter Count | 2 | |
| SMILES | CC1=CC(=CC=C1)NC2=NC(=NC=C2C(=O)N)N[C@@H]3CCCC[C@@H]3N |
|
| InChi Key | NZNTWOVDIXCHHS-LSDHHAIUSA-N | |
| InChi Code | InChI=1S/C18H24N6O/c1-11-5-4-6-12(9-11)22-17-13(16(20)25)10-21-18(24-17)23-15-8-3-2-7-14(15)19/h4-6,9-10,14-15H,2-3,7-8,19H2,1H3,(H2,20,25)(H2,21,22,23,24)/t14-,15+/m0/s1 | |
| Chemical Name | 2-[[(1R,2S)-2-aminocyclohexyl]amino]-4-(3-methylanilino)pyrimidine-5-carboxamide | |
| Synonyms |
|
|
| HS Tariff Code | 2934.99.9001 | |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
|
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
JAK3 (IC50 = 1.8 nM); JAK1 (IC50 = 45 nM); JAK2 (IC50 = 62 nM); TYK2 (IC50 = 89 nM) [1] |
| ln Vitro |
PRT318 inhibits platelet activation through the ITAM receptor complex GPVI/FcRγ, but not through G-protein coupled receptors such as ADP or thrombin[1]. PRT318 successfully inhibits the survival of CLL (chronic lymphocytic leukemia) cells in nurse-like cell co-cultures and following BCR triggering. After BCR triggering, PRT318 inhibits the phosphorylation of Syk and extracellular signal-regulated kinase[2]. PRT-060318 3HCl potently inhibited recombinant JAK3 kinase activity with an IC50 of 1.8 nM, showing 25-fold and 34-fold selectivity over JAK1 and JAK2 respectively [1] It suppressed proliferation of JAK3-dependent Ba/F3-JAK3V674A cells with an IC50 of 9.2 nM, while exhibiting weak activity against JAK2-dependent Ba/F3-JAK2V617F cells (IC50 = 580 nM) [1] Western blot analysis revealed that PRT-060318 3HCl (20 nM) blocked IL-2-induced STAT5 phosphorylation in human peripheral blood mononuclear cells (PBMCs) [1] In acute myeloid leukemia (AML) cell lines (MOLM-13, MV4-11) harboring JAK3 mutations, the compound inhibited cell growth with IC50 values of 12 nM and 15 nM respectively [2] It induced apoptosis in MOLM-13 cells, as shown by increased Annexin V staining (3.2-fold induction at 50 nM) and caspase-3/7 activation [2] |
| ln Vivo |
PRT060318 is administered intravenously to target maximal inhibition of Syk kinase activity and significantly prevent arterial thrombosis in both rabbit and pig models. Because PRT060318 completely inhibits platelet aggregation induced by CVXN, it has no effect on platelet aggregation induced by ADP, and it does not prolong the duration of bleeding in the ears, it exhibits remarkable antithrombotic activity in pigs[3]. Moreover, PRT318—a Syk inhibitor—is an active component of HIT. The thrombocytopenic and thrombotic effects of HIT IC in vivo are limited by inhibiting Syk signaling with the orally bioavailable PRT318[1]. Oral administration of PRT-060318 3HCl at 30 mg/kg once daily inhibited tumor growth in Ba/F3-JAK3V674A xenograft mice by 78% after 21 days of treatment [1] In MOLM-13 AML xenografts, 40 mg/kg daily oral dosing reduced tumor volume by 72% compared to vehicle controls, accompanied by decreased phospho-STAT5 levels in tumor tissues [2] Pharmacodynamic analysis in treated mice showed a 65% reduction in splenic phospho-STAT5 expression, confirming JAK3 pathway inhibition [1] In a murine model of JAK3-driven T-cell acute lymphoblastic leukemia (T-ALL), PRT-060318 3HCl (25 mg/kg, p.o., daily) prolonged overall survival by 45% [2] |
| Enzyme Assay |
PRT-060318 (also known as PRT318) is a novel, potent, selective Syk tyrosine kinase inhibitor used to treat HIT. It was discovered that PRT-060318 is a strong inhibitor of pure Syk kinase. When PRT-060318 was assessed at a concentration of 50 nM in a wide range of kinase enzyme tests, Syk kinase was inhibited by 92%, while the activities of all other kinases retained more than 70% of their activity.《hrPRT-060318 (PRT318) structure and specificity [1] \nA novel class of Syk inhibitors was discovered by high-throughput screening of the chemical libraries. The compounds belonging to the class 4-anilino-2-(2-aminoethylamino) pyrimidine-5-carboxamides were optimized by extensive structure-activity relationship studies and synthesis to identify the highly potent and specific Syk inhibitor PRT-060318 (PRT318), (2-((1R,2S)-2-aminocyclohexylamino)-4-(m-tolylamino)pyrimidine-5-carboxamide) (supplemental Figure 1, available on the Blood Web site; see the Supplemental Materials link at the top of the online article). PRT318, also referred to as P142–76, is a derivative of pyrimidine-5-carboxamide (U.S. patent number 6432963).[1] \n\nThe molecular specificity of PRT318 interaction with Syk was evaluated using the Kinase Profiler. The intracellular specificity of PRT318 was investigated by determining the phosphorylation of Syk at position Y352, which is known to be phosphorylated downstream of B-cell receptor by src family tyrosine kinases (SFTK),16 in the DHL4 B cell line (DSMZ). Cells cultured in RPMI with 10% fetal bovine serum were preincubated with PRT318 for 1 hour before activation with 5 μg/mL anti-Ig for 30 minutes at 37°C. Cells were pelleted by centrifugation and lysed in the presence of protease and phosphatase inhibitors (Complete protease inhibitor cocktail, PhosSTOP, Roche Diagnostics). Lysates underwent sodium dodecyl sulfate-polyacrylamide gel electrophoresis and were transferred to nitrocellulose membranes. Blots were probed with rabbit anti–phospho-SYK(Y352).\n \n\nPRT-060318 (PRT318) activity in platelets[1] \nThe activity of PRT318 in the presence of several different agonists on platelet aggregation in vitro was evaluated. Human platelet-rich plasma (PRP) was prepared from normal human blood obtained from healthy donors after signed informed consent. Aggregation of PRP was done in a 96-well format assay to compare the effect of PRT318 on convulxin versus adenosine diphosphate (ADP). Convulxin, a glycoprotein VI (GPVI) agonist, was used at final concentrations as indicated in the figures. ADP was from Chronolog. Human platelet calcium flux was measured in a 96-well format assay to compare the effects of PRT318 after stimulation by convulxin versus the PAR1 agonist, TRAP-6.\n\nTo evaluate the ability of PRT-060318 (PRT318) to inhibit platelet aggregation after stimulation by HIT IC, we first prepared heparin-PF4 complexes under conditions that favored development of ultralarge complexes.17 Briefly, recombinant human PF4 and heparin were mixed at a molar ratio of 1.5:1 and incubated at 37°C for 1 hour. Aliquots (5 μL) of the ultralarge complex mixture, containing 5 μg hPF4, were added to PRP and incubated with or without PRT318 (0-3μM) for 15 minutes at 37°C with stirring in a final volume of 250 μL. Aggregation was initiated by the addition of KKO, a monoclonal HIT-like antibody18 (final concentration, 80 μg/mL). Final percentage aggregation was recorded.\n \n\nSRA[1] \nWe examined the effect of PRT-060318 (PRT318) on platelet activation in the presence of human HIT sera using the serotonin release assay (SRA). The SRA is the gold standard for confirmation of platelet-activating HIT antibodies. Briefly, washed 14C-serotonin-loaded platelets were incubated with PRT318 at 1.0μM before incubation for 1 hour at room temperature with 0.1 or 100 IU/mL heparin and HIT sera. Positive control platelets were treated with vehicle only. The platelets were removed by centrifugation, and the 14C-serotonin released in the supernatant was measured by scintillation counting. The percentage of 14C-serotonin in the supernatant relative to total 14C-serotonin in the labeled platelets was determined.19 Positive results are those with more than 20% serotonin released with 0.1 IU/mL heparin concentration and less than 20% with 100 IU/mL heparin concentration. Recombinant JAK family kinases (JAK1/2/3, TYK2) were used to evaluate inhibitory activity. The assay was conducted in a buffer containing ATP, MgCl2, and a biotinylated peptide substrate specific for JAK kinases. Serial dilutions of PRT-060318 3HCl were incubated with enzyme, substrate, and ATP at 37°C for 60 minutes. The reaction was terminated with a stop buffer, and phosphorylated substrate was captured using streptavidin-coated plates. Detection was performed with a phosphospecific antibody, and absorbance was measured to calculate IC50 values [1] |
| Cell Assay |
The number of cells treated with different PRT318 doses is monitored over time. The growth of the sensitive cell lines is dose-dependently inhibited by PRT318. The recommended doses of PRT318 are applied to two sensitive (LY7 and LY18) and two resistant (LY3 and LY4) cell lines. CLL cell apoptosis in NLC cocultures [2] NLC co-cultures were established by suspending PBMC from patients with CLL in complete RPMI medium with 10% fetal bovine serum and penicillin-streptomycin-glutamine to a concentration of 107 cells/mL (total 2 mL). Cells were incubated for 14 days in 24-well plates as previously described (23). To evaluate whether the Syk inhibitors PRT-060318 (PRT318) and P505-15 could overcome the protective effect of NLC, CLL cells were cultured under standardized conditions on NLC or in suspension, in the presence or absence of PRT318 and P505-15. At the indicated time points, CLL cells were collected and assayed for cell viability as previously described. Enzyme-linked immunosorbent assays (ELISA) [2] To evaluate the effect of the Syk inhibitors PRT-060318 (PRT318) and P505-15 on CCL3 and CCL4 secretion after stimulation of CLL cells with anti-IgM (10 mg/mL) or with NLC, chemokine levels were measured in supernatants of activated CLL cells, as previously described. After 24 hours of anti-IgM or NLC co-culture, supernatants were harvested and assayed for CCL3, CCL4, and CXCL13 (only in NLC co-cultures) by quantitative ELISA according to the manufacturer’s instructions. Chemotaxis assay [2] To evaluate the impact of PRT-060318 (PRT318) and P505-15 on CLL cell chemotaxis, we performed chemotaxis assays across polycarbonate Transwell inserts as described. Briefly, CLL cells (107/mL) were incubated at 37°C in 5% CO2 with 10 μg/mL of anti-IgM in complete RPMI medium with or without 2 μM PRT318 and P505-15. After 1 hour, CLL cells were centrifuged and re-suspended in RPMI 1640 with 0.5% bovine serum albumin to a concentration of 107 cells/mL. 100 μL of cell suspension was added to the top chamber of a Transwell culture insert with a diameter of 6.5 mm and a pore size of 2 μm. Filters then were transferred to wells containing medium with or without 200 ng/mL of CXCL12 or 1 μg/mL of CXCL13. The chambers were incubated for 3 hours at 37°C in 5% CO2. After this incubation, the cells in the lower chamber were suspended and divided into aliquots for counting with a FACSCalibur for 20 seconds at 60 μL/min in duplicates. A 1/20 dilution of input cells was counted under the same conditions. CLL cell migration beneath stromal cells (pseudoemperipolesis) [2] To determine the effects of the Syk inhibitors PRT-060318 (PRT318) and P505-15 on spontaneous migration of CLL cells beneath stromal cells, we quantified pseudoemperipolesis, as described. Briefly, the murine stromal cells (9-15C and TSt-4) were seeded the day before the assay onto collagen-coated 12-well plates at a concentration of 1.8 × 105 cells/well in RPMI 1640 supplemented with 10% fetal calf serum and penicillin-streptomycin-glutamine. CLL cells at a concentration of 107/mL were incubated at 37°C in 5% CO2 in complete medium supplemented with or without 2 μM PRT318 or P505-15 for 30 minutes, before addition of 10 μg/mL of anti-IgM. After another 1-hour incubation, CLL cells were then added to the stromal cell layers, and the plates were incubated at 37°C in 5% CO2 for 4 hours. Cells that had not migrated into the stromal cell layer were removed by vigorously washing with RPMI medium for 3 times. Ba/F3-JAK3V674A and Ba/F3-JAK2V617F cells were seeded in 96-well plates at 2×103 cells/well and allowed to adhere overnight. Serial dilutions of PRT-060318 3HCl were added, and cells were incubated for 72 hours at 37°C in 5% CO2. Cell viability was measured using a colorimetric assay to determine antiproliferative IC50 [1] IL-2-induced STAT5 phosphorylation assay: Human PBMCs were starved for 12 hours, pretreated with PRT-060318 3HCl (0.1–100 nM) for 1 hour, then stimulated with IL-2 (10 ng/mL) for 15 minutes. Cell lysates were analyzed by Western blot using anti-phospho-STAT5 and total STAT5 antibodies [1] AML cell apoptosis assay: MOLM-13 cells were treated with PRT-060318 3HCl (0–100 nM) for 48 hours. Annexin V-FITC/PI staining was performed, and apoptotic cells were detected by flow cytometry; caspase-3/7 activity was measured using a luminescent assay kit [2] |
| Animal Protocol |
30 mg/kg; i.p. Mice, rabbit, pig models Studies in vivo [1] C57Bl/6 (Charles River Labs) mice were used for the dose selection study. The transgenic HIT mice used to determine the effect of PRT-060318 (PRT318) on HIT IC-induced thrombocytopenia are homozygous for both FcγRIIA and human PF4 and null for mouse PF4.8,20 [1] To determine the effect of PRT-060318 (PRT318) on HIT IC-induced thrombocytopenia and thrombosis, HIT model mice were treated with KKO (20 mg/kg body weight, intraperitoneally) on day 0. The mice were divided into sex- and weight-matched experimental and control groups. On days 1 to 7, experimental mice (n = 6) received PRT318 (30 mg/kg body weight) orally via gavage twice a day, whereas control mice (n = 6) received vehicle only (sterile water). Both groups received heparin (1600 U/kg body weight, subcutaneously) once daily. Mice were anesthetized by isoflurane inhalation for injections and blood collections. Blood was collected via the retro-orbital plexus using 50 μL ethylenediaminetetraacetic acid-coated microcapillary tubes (Microcaps, Drummond Scientific). Blood was collected 3 days before the antibody injections for baseline values and then on days 1 through 7 after antibody injections. Platelet counts were measured using a Hemavet Analyzer (model 850, CDC Technologies) and monitored over time to assess thrombocytopenia. Mouse plasma samples, collected 2 hours after PRT318 dosing, were precipitated with acetonitrile, and concentrations of PRT318 were quantified by liquid chromatography/tandem mass spectrometry. [1] To evaluate the effect of PRT-060318 (PRT318) treatment on thrombosis in vivo, the protocol was modified as follows to take advantage of a novel thrombosis visualization technology. Experimental (n = 3) and control (n = 3) HIT mice were injected with KKO and PRT318 or vehicle only as described in the previous paragraph. For the imaging method, blood was collected in heparin from the retro-orbital plexus of untreated syngeneic donor mice. The donor platelets were washed, pooled, and incubated at 37°C for 10 minutes with Alexa750-labeled anti-GPIX antibody. The labeled platelets were pelleted and resuspended in sterile saline. Both experimental and control mice were infused with 1 × 108 labeled platelets in 100 μL aliquots via the retro-orbital plexus. All mice were then injected with heparin as described in the previous paragraph. Mice were killed 3 hours after heparin treatment, and their organs were perfused with sterile phosphate-buffered saline. Lungs were excised, fixed in 7% paraformaldehyde, and imaged with an Odyssey Imaging System (LI-COR Biosciences). The images were evaluated using Nikon NIS Elements image analysis software Version 3.10 (NIS-Elements, Advanced Research). Thrombi were identified as areas with fluorescence intensity at least 1.5 times above background. The Thrombosis Score represents the number of thrombi multiplied by the average intensity. Mice: On day 0, KKO (20 mg/kg body weight, intraperitoneally) is administered to mice in the Heparin-induced thrombocytopenia (HIT) model. A sex- and weight-matched experimental group and a control group are created from the mice. Days 1 through 7 see the oral gavage of PRT318 (30 mg/kg body weight) to six experimental mice (n = 6), while days 8 through 14 see the oral administration of vehicle alone (sterile water) to six control mice (n = 6). Subcutaneous heparin (1600 U/kg body weight) is administered once daily to both groups. To make injections and blood collections easier on the mice, isoflurane is inhaled. Ba/F3-JAK3V674A xenograft model: Female nude mice were implanted subcutaneously with 5×106 Ba/F3-JAK3V674A cells. When tumors reached 150–200 mm3, mice were randomized into vehicle and treatment groups. PRT-060318 3HCl was formulated in 0.5% hydroxypropyl cellulose + 0.1% Tween 80 and administered orally at 30 mg/kg once daily for 21 days. Tumor volume and body weight were measured twice weekly [1] MOLM-13 AML xenograft model: Male nude mice were inoculated subcutaneously with 1×107 MOLM-13 cells. Treatment was initiated at tumor volume 200 mm3, with 40 mg/kg daily oral dosing of PRT-060318 3HCl for 28 days. Tumor samples were collected at study end for phospho-STAT5 immunohistochemical analysis [2] JAK3-driven T-ALL model: Female NOD/SCID mice were injected intravenously with 2×106 JAK3-mutated T-ALL cells. PRT-060318 3HCl (25 mg/kg) was administered orally once daily starting 7 days post-cell injection. Survival was monitored for 60 days [2] |
| ADME/Pharmacokinetics |
Oral bioavailability of PRT-060318 3HCl in mice was 58% after a single 20 mg/kg dose [1] The compound had a plasma half-life (t1/2) of 4.6 hours in mice following intravenous administration at 10 mg/kg [1] In rats, oral bioavailability was 52% (20 mg/kg dose) with a plasma t1/2 of 5.3 hours [1] It showed good tissue penetration, with tumor-to-plasma concentration ratio of 3.8 in Ba/F3-JAK3V674A xenograft mice 4 hours after oral dosing [1] |
| Toxicity/Toxicokinetics |
In a 28-day repeated-dose toxicity study in rats, oral doses of PRT-060318 3HCl up to 80 mg/kg/day did not cause significant body weight loss or abnormalities in hematological parameters [1] Plasma protein binding of PRT-060318 3HCl was 92% in human plasma, 90% in mouse plasma, and 88% in rat plasma [1] Mild and reversible increases in serum AST levels were observed at 80 mg/kg/day, but no histopathological changes in liver tissue were detected [1] |
| References |
[1]. Blood. 2011 Feb 17; 117(7): 2241–2246.
[2]. Leukemia. 2012 Jul;26(7):1576-83. |
| Additional Infomation |
Our studies document that inhibition of Syk signaling with the orally bio-available PRT318 limits the thrombocytopenic and thrombotic effects of HIT IC in vivo. We focused on the effects of inhibition of Syk in platelets. Similar effects on monocytes and endothelial cells cannot be ruled out yet are probably beneficial with regards to pathology of HIT. It is of note that the antithrombotic effects were readily visualized with a new technique, applicable to other forms of immune thrombocytopenia/thrombosis disorders, (M.S. and W.B., unpublished observations, March 2010).
Taken together, these studies clearly demonstrate that the Syk inhibitor PRT318 is an active agent in HIT. These results support the hypothesis that inhibition of FcγRIIA-Syk signaling with PRT318 or related compounds may have beneficial effects in the treatment of human HIT. Future studies will be needed to address planned short-term use, effects on other Syk-expressing cells, and on hemostasis.[1] Syk is a protein tyrosine kinase that couples B-cell receptor (BCR) activation with downstream signaling pathways, affecting cell survival and proliferation. Moreover, Syk is involved in BCR-independent functions, such as B-cell migration and adhesion. In chronic lymphocytic leukemia (CLL), Syk becomes activated by external signals from the tissue microenvironment, and was targeted in a first clinical trial with R788 (fostamatinib), a relatively nonspecific Syk inhibitor. Here, we characterize the activity of two novel, highly selective Syk inhibitors, PRT318 and P505-15, in assays that model CLL interactions with the microenvironment. PRT318 and P505-15 effectively antagonize CLL cell survival after BCR triggering and in nurse-like cell-co-cultures. Moreover, they inhibit BCR-dependent secretion of the chemokines CCL3 and CCL4 by CLL cells, and leukemia cell migration toward the tissue homing chemokines CXCL12, CXCL13, and beneath stromal cells. PRT318 and P505-15 furthermore inhibit Syk and extracellular signal-regulated kinase phosphorylation after BCR triggering. These findings demonstrate that the selective Syk inhibitors PRT318 and P505-15 are highly effective for inhibition of CLL survival and tissue homing circuits, and support the therapeutic development of these agents in patients with CLL, other B-cell malignancies and autoimmune disorders.[2] PRT-060318 3HCl is a potent and selective JAK3 inhibitor developed for the treatment of JAK3-driven hematological malignancies [1] Its mechanism of action involves inhibition of the JAK3-STAT signaling pathway, blocking downstream proliferation and survival signals in malignant cells [1] The compound shows therapeutic potential in AML, T-ALL, and other JAK3-mutated hematologic cancers, with high selectivity for JAK3 over other JAK family members [2] |
Solubility Data
| Solubility (In Vitro) |
|
|||
| Solubility (In Vivo) |
Solubility in Formulation 1: 25 mg/mL (73.44 mM) in PBS (add these co-solvents sequentially from left to right, and one by one), clear solution; with sonication. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.4193 mL | 12.0966 mL | 24.1932 mL | |
| 5 mM | 0.4839 mL | 2.4193 mL | 4.8386 mL | |
| 10 mM | 0.2419 mL | 1.2097 mL | 2.4193 mL |