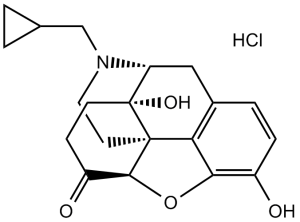
Naltrexone HCl is a potent opioid receptor antagonist used mainly in the management of alcohol dependence and opioid dependence. Naltrexone is a drug that reverses the effects of opioids and should not be confused with naloxone or nalorphine, which are used in emergency cases of opioid overdose. Opioid receptor is a group of G protein-coupled receptors with opioids as ligands (e.g. proenkephalin, prodynorphin, pronociceptin etc, functioning in regulating pain perception, hormonal secretion and affecting temperature control etc.
Physicochemical Properties
| Molecular Formula | C20H23NO4.HCL | |
| Molecular Weight | 377.86 | |
| Exact Mass | 377.139 | |
| Elemental Analysis | C, 63.57; H, 6.40; Cl, 9.38; N, 3.71; O, 16.94 | |
| CAS # | 16676-29-2 | |
| Related CAS # | 16590-41-3 (free);16676-29-2 (HCl); | |
| PubChem CID | 5485201 | |
| Appearance | Typically exists as solid at room temperature | |
| Density | 1.47 g/cm3 | |
| Boiling Point | 558.1ºC at 760 mmHg | |
| Melting Point | 274-2760C | |
| Flash Point | 291.4ºC | |
| Vapour Pressure | 2.71E-13mmHg at 25°C | |
| LogP | 2.265 | |
| Hydrogen Bond Donor Count | 3 | |
| Hydrogen Bond Acceptor Count | 5 | |
| Rotatable Bond Count | 2 | |
| Heavy Atom Count | 26 | |
| Complexity | 621 | |
| Defined Atom Stereocenter Count | 4 | |
| SMILES | Cl[H].O1C2=C(C([H])=C([H])C3C([H])([H])[C@]4([H])[C@@]5(C([H])([H])C([H])([H])C([C@@]1([H])[C@@]5(C=32)C([H])([H])C([H])([H])N4C([H])([H])C1([H])C([H])([H])C1([H])[H])=O)O[H])O[H] |
|
| InChi Key | RHBRMCOKKKZVRY-ITLPAZOVSA-N | |
| InChi Code | InChI=1S/C20H23NO4.ClH/c22-13-4-3-12-9-15-20(24)6-5-14(23)18-19(20,16(12)17(13)25-18)7-8-21(15)10-11-1-2-11;/h3-4,11,15,18,22,24H,1-2,5-10H2;1H/t15-,18+,19+,20-;/m1./s1 | |
| Chemical Name | (4R,4aS,7aR,12bS)-3-(cyclopropylmethyl)-4a,9-dihydroxy-2,4,5,6,7a,13-hexahydro-1H-4,12-methanobenzofuro[3,2-e]isoquinolin-7-one;hydrochloride | |
| Synonyms |
|
|
| HS Tariff Code | 2934.99.9001 | |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
|
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
- μ-opioid receptor (MOR) (Ki = 0.08–0.15 nM, competitive antagonist) [2][3][6] - κ-opioid receptor (KOR) (Ki = 0.4–0.8 nM, competitive antagonist) [2][3] - δ-opioid receptor (DOR) (Ki = 2.0–3.5 nM, weak competitive antagonist) [2][3] - No significant binding to non-opioid receptors (e.g., GABAₐ, NMDA) at concentrations ≤10 μM [3][6] |
| ln Vitro |
In vitro activity: Naltrexone (0.32 mg/kg) reduces ethanol-reinforced responding at the concentration that maintained the most responding (1% or 2%) in rhesus monkeys. Naltrexone (0.1 mg/kg) reduces ethanol-reinforced responding, both at a low ethanol concentration (0.25%) that produced little ethanol intake (g/kg), and at a higher concentration (4%) with an appreciable intake. Naltrexone (1-3 mg/kg) potently and dose-dependently inhibits reinstatement of ethanol-seeking produced by non-contingent deliveries of the liquid dipper filled with 8% ethanol. Naltrexone elicits optimal enhancement of morphines antinociceptive potency in mice when co-administered (i.p.) at about 100 ng/kg together with morphine (3 mg/kg). Naltrexone (10 ng/kg i.p.) augments the antinociception produced by an acute submaximal dose of intrathecal (5 mg) or systemic (7.5 mg/kg i.p.) morphine in the tail-flick test in rats. Naltrexone combined with Morphine inhibits the decline in morphine antinociception and prevented the loss of morphine potency in rats. Naltrexone significantly suppresses ethanol self-administration and prevents ethanol-induced increases in dialysate dopamine levels. Naltrexone completely prevents the reduction in anogenital distance in prenatally stressed (PS) males and restores the growth rate of both sexes. Naltrexone also decreases the anxiety of PS rats in the plus-maze, increases the opioid component of exploration to control levels, but increases anxiety in control males 1. Antitumor activity (low-dose): - In human breast cancer cell lines (MCF-7, MDA-MB-231), naltrexone (1–10 nM) inhibited cell proliferation by 20–35% via downregulating NF-κB activity; Western blot showed reduced p65 phosphorylation (Ser536) by 40–50% [1] - In melanoma cells (A375), naltrexone (5 nM) induced apoptosis via caspase-9 activation, with apoptotic rates increasing from 4% (control) to 18% after 72 hours (Annexin V/PI staining) [1] 2. Opioid receptor antagonism: - In CHO cells stably expressing MOR, naltrexone (0.1–1 nM) blocked [³H]-dihydromorphine binding in a dose-dependent manner, with 50% inhibition at 0.12 nM (radioligand displacement assay) [3][6] - In SH-SY5Y neuroblastoma cells (expressing KOR), naltrexone (0.5 nM) inhibited U50,488H (KOR agonist)-induced Ca²⁺ influx by 80% (fluorescence-based Ca²⁺ imaging) [3] |
| ln Vivo |
In adult male Sprague-Dawley rats, ultra-low doses of naltrexone (16.7, 20.0, and 25.0 ng/kg) with morphine (1mg/kg) extended the duration of the morphine-induced conditioned place preference. In male Wistar rats, naltrexone significantly inhibited ethanol self-adminnistration and prevented ethanol-activated increases in dialysate dopamine amount. Subchronic treatment with naltrexone caused progressive decrease of ethanol self-administration. Single doses of naltrexone increased extinction and attenuated cue-induced reinstatement of ethanol-reinforced behavior. In rhesus monkeys, naltrexone lowered behavior kept non-selectively by either ethanol or sucrose. 1. Tumor growth inhibition (low-dose): - In nude mice bearing MCF-7 breast cancer xenografts, oral naltrexone (0.1 mg/kg daily for 28 days) reduced tumor volume by 40% and tumor weight by 35% (vehicle: 1.8 ± 0.3 g; naltrexone: 1.2 ± 0.2 g); immunohistochemistry showed reduced Ki-67 (proliferation marker) positivity from 60% to 30% [1] - In C57BL/6 mice with B16-F10 melanoma, naltrexone (0.05 mg/kg i.p. every other day) reduced lung metastatic nodules by 25% (vehicle: 42 ± 6; naltrexone: 32 ± 5) [1] 2. Opioid dependence reversal: - In rats with morphine-induced physical dependence, subcutaneous naltrexone (1 mg/kg) precipitated withdrawal symptoms (e.g., paw tremors, wet dog shakes) within 15 minutes, with symptom severity peaking at 60 minutes (behavioral scoring: 8/10 vs. vehicle: 1/10) [3] - In rhesus monkeys trained to self-administer heroin, oral naltrexone (3 mg/kg daily) reduced heroin self-administration by 70% over 14 days (vehicle: 25 ± 4 infusions/day; naltrexone: 7 ± 2) [2] 3. Alcohol dependence reduction: - In C57BL/6 mice with chronic alcohol intake (10% ethanol), oral naltrexone (2 mg/kg daily) decreased ethanol consumption by 55% (vehicle: 12 ± 2 g/kg/day; naltrexone: 5.4 ± 1.1) [6] - In rats with alcohol-induced conditioned place preference (CPP), naltrexone (1.5 mg/kg i.p.) blocked CPP expression, with preference score reduced from 45 ± 5 (vehicle) to 10 ± 3 [6] 4. Weight loss (combination with bupropion): - In diet-induced obese (DIO) Sprague-Dawley rats, oral naltrexone (3 mg/kg) + bupropion (10 mg/kg) daily for 4 weeks reduced body weight by 12% (vehicle: 520 ± 20 g; combination: 458 ± 15 g) and fat mass by 18% [5] |
| Enzyme Assay |
1. μ-opioid receptor binding assay:
- Membranes isolated from CHO cells expressing human MOR were incubated with [³H]-dihydromorphine (0.5 nM) and naltrexone (0.01–10 nM) in binding buffer (50 mM Tris-HCl, pH 7.4, 100 mM NaCl, 5 mM MgCl₂) at 25°C for 60 minutes. Bound ligand was separated by filtration through glass fiber filters, and radioactivity was measured by liquid scintillation counting. The assay was repeated in triplicate, and Ki was calculated using the Cheng-Prusoff equation [3][6] 2. NF-κB activity assay (for antitumor mechanism): - Nuclear extracts from MCF-7 cells treated with naltrexone (1–10 nM) were incubated with a biotinylated NF-κB consensus oligonucleotide in binding buffer (20 mM HEPES, pH 7.5, 50 mM KCl, 1 mM DTT) at 4°C for 30 minutes. Streptavidin-coated plates were used to capture the DNA-protein complex, and NF-κB binding was detected via a primary antibody against p65 and a horseradish peroxidase (HRP)-conjugated secondary antibody. Absorbance at 450 nm was measured, and activity was normalized to vehicle-treated controls [1] |
| Cell Assay |
1. Tumor cell proliferation assay (MTT):
- MCF-7/MDA-MB-231 cells (5×10³ cells/well) were seeded in 96-well plates and treated with naltrexone (0.1–100 nM) for 72 hours. MTT solution (0.5 mg/mL) was added, and plates were incubated at 37°C for 4 hours. Formazan crystals were solubilized with DMSO, and absorbance at 570 nm was measured. Cell viability was calculated relative to vehicle controls, and IC₅₀ for proliferation inhibition was 8–10 nM in MCF-7 cells [1] 2. Apoptosis assay (Annexin V/PI): - A375 melanoma cells (1×10⁵ cells/well) were treated with naltrexone (5 nM) for 48/72 hours. Cells were harvested, washed with PBS, and stained with Annexin V-FITC and PI for 15 minutes at room temperature in the dark. Flow cytometry was used to quantify early (Annexin V⁺/PI⁻) and late (Annexin V⁺/PI⁺) apoptotic cells, with triplicate samples per group [1] 3. Opioid agonist-induced Ca²⁺ influx assay: - SH-SY5Y cells (expressing KOR) were loaded with Fluo-4 AM (2 μM) in HBSS buffer at 37°C for 30 minutes. Cells were treated with naltrexone (0.1–1 nM) for 10 minutes, followed by U50,488H (1 μM, KOR agonist). Fluorescence intensity (excitation 488 nm, emission 525 nm) was measured every 5 seconds for 5 minutes to assess Ca²⁺ influx, with inhibition percentage calculated relative to U50,488H-only controls [3] |
| Animal Protocol |
1. Breast cancer xenograft model (nude mice):
- Female athymic nude mice (6–8 weeks old) were subcutaneously injected with 1×10⁷ MCF-7 cells (suspended in PBS:Matrigel = 1:1) into the right flank. When tumors reached 100 mm³, mice were randomized to vehicle (0.9% saline, 0.1 mL/10 g) or naltrexone (0.1 mg/kg, dissolved in vehicle) groups. Drugs were administered via oral gavage once daily for 28 days. Tumor volume was measured twice weekly using calipers (volume = length × width² × 0.52), and body weight was recorded weekly. On day 28, mice were euthanized, tumors were excised and weighed, and tumor tissues were fixed in 4% paraformaldehyde for immunohistochemistry [1] 2. Morphine dependence model (rats): - Male Sprague-Dawley rats (250–300 g) were implanted with subcutaneous morphine pellets (75 mg/pellet) once every 72 hours for 14 days to induce physical dependence. On day 15, rats were administered subcutaneous naltrexone (1 mg/kg, dissolved in 0.9% saline) or vehicle. Withdrawal symptoms (paw tremors, wet dog shakes, diarrhea) were scored every 15 minutes for 2 hours using a validated behavioral scale (0 = absent, 2 = severe) [3] 3. Long-acting naltrexone formulation (rhesus monkeys): - Male rhesus monkeys (4–6 kg) trained to self-administer heroin (0.1 mg/kg/infusion) were administered a single intramuscular injection of long-acting naltrexone depot (30 mg/kg, formulated as a microsphere suspension in aqueous buffer). Heroin self-administration was measured daily for 28 days, with infusions recorded via a computerized operant conditioning system. Blood samples were collected weekly to measure plasma naltrexone concentrations [2] 4. Diet-induced obesity model (rats): - Male Sprague-Dawley rats (180–200 g) were fed a high-fat diet (45% kcal from fat) for 8 weeks to induce obesity. Rats were then randomized to vehicle (0.5% methylcellulose), naltrexone (3 mg/kg, dissolved in vehicle), bupropion (10 mg/kg), or combination groups. Drugs were administered via oral gavage once daily for 4 weeks. Body weight was measured weekly, and food intake was recorded daily. At the end of the study, rats were euthanized, and epididymal fat pads were excised and weighed [5] |
| ADME/Pharmacokinetics |
- Absorption: Oral naltrexone has 5–40% bioavailability due to first-pass metabolism; peak plasma concentrations (Cₘₐₓ) of 10–20 ng/mL are reached 1–2 hours after a 50 mg oral dose [2][5][6] - Distribution: Volume of distribution (Vd) = 16–18 L/kg in humans; crosses the blood-brain barrier (BBB) with brain/plasma concentration ratio of 0.5–0.8 [2][6] - Metabolism: Primarily metabolized by hepatic CYP3A4 to 6β-naltrexol (active metabolite, MOR antagonist with ~1/10 potency of naltrexone); 6β-naltrexol is further glucuronidated to inactive conjugates [2][5][6] - Excretion: Elimination half-life (t₁/₂) of naltrexone = 4–6 hours, 6β-naltrexol = 12–14 hours; 60–80% of dose excreted in urine (30% as 6β-naltrexol, <10% as unchanged drug), 10–20% in feces [2][5][6] - Long-acting depot formulation: Intramuscular naltrexone depot (380 mg) maintains plasma concentrations >1 ng/mL for 4 weeks; Cₘₐₓ = 3–5 ng/mL at 2–3 days post-injection, t₁/₂ = 5–7 days [2] Metabolism / Metabolites Hepatic. When administered orally, naltrexone undergoes extensive biotransformation and is metabolized to 6 beta-naltrexol (which may contribute to the therapeutic effect) and other minor metabolites. Route of Elimination: Both parent drug and metabolites are excreted primarily by the kidney (53% to 79% of the dose), however, urinary excretion of unchanged naltrexone accounts for less than 2% of an oral dose and fecal excretion is a minor elimination pathway. The renal clearance for naltrexone ranges from 30 to 127 mL/min and suggests that renal elimination is primarily by glomerular filtration. Half Life: 4 hours for naltrexone and 13 hours for the active metabolite 6 beta-naltrexol. Absorption, Distribution and Excretion Although well absorbed orally, naltrexone is subject to significant first pass metabolism with oral bioavailability estimates ranging from 5 to 40%. Both parent drug and metabolites are excreted primarily by the kidney (53% to 79% of the dose), however, urinary excretion of unchanged naltrexone accounts for less than 2% of an oral dose and fecal excretion is a minor elimination pathway. The renal clearance for naltrexone ranges from 30 to 127 mL/min and suggests that renal elimination is primarily by glomerular filtration. 1350 L [intravenous administration] ~ 3.5 L/min [after IV administration] Naltrexone hydrochloride is rapidly and almost completely (about 96%) absorbed from the GI tract following oral administration, but the drug undergoes extensive first-pass metabolism in the liver. Only 5-40% of an orally administered dose reaches systemic circulation unchanged. Considerable interindividual variation in absorption of the drug during the first 24 hours after a single dose has been reported. The bioavailability of naltrexone hydrochloride tablets is reportedly similar to that of an oral solution of the drug (not commercially available in the US). Peak plasma concentrations of naltrexone and 6-beta-naltrexol (the major metabolite of naltrexone) usually occur within 1 hour following oral administration of the tablets and 0.6 hours following oral administration of the solution. Because orally administered naltrexone undergoes substantial first-pass metabolism, plasma concentrations of 6-beta-naltrexol following oral administration are substantially higher than corresponding concentrations of naltrexone. Following oral administration, the area under the serum concentration-time curve (AUC) for 6-beta-naltrexol is 10-30 times greater than the AUC for naltrexone. Following single- or multiple-dose (i.e., once daily) oral administration of naltrexone hydrochloride 50 mg in healthy individuals, peak plasma concentrations of naltrexone and 6-beta-naltrexol averaged 10.6-13.7 and 109-139 ng/mL, respectively. Little, if any, accumulation of naltrexone and/or 6-beta-naltrexol appears to occur following chronic administration of the drug. Following chronic administration of naltrexone, plasma concentrations of 6-beta-naltrexol are at least 40% higher than those following administration of a single dose of the drug; however, plasma concentrations of naltrexone and 6-beta-naltrexol 24 hours after each dose of chronically administered drug are similar to concentrations 24 hours after a single dose of the drug in most patients. Naltrexone hydrochloride is widely distributed throughout the body, but considerable interindividual variation in distribution parameters during the first 24 hours following a single oral dose has been reported. Following subcutaneous administration of radiolabeled drug in rats, the drug distributes into CSF within 30 minutes. In animals, CSF naltrexone concentrations are reported to be approximately 30% of concurrent peak plasma concentrations. The drug and its metabolites have been shown to distribute into saliva and erythrocytes following oral administration in humans. For more Absorption, Distribution and Excretion (Complete) data for Naltrexone (13 total), please visit the HSDB record page. Metabolism / Metabolites Hepatic. When administered orally, naltrexone undergoes extensive biotransformation and is metabolized to 6 beta-naltrexol (which may contribute to the therapeutic effect) and other minor metabolites. Naltrexone is metabolized in the liver principally by reduction of the 6-keto group of naltrexone to 6-beta-naltrexol (6-beta-hydroxynaltrexone). Naltrexone also undergoes metabolism by catechol-O-methyl transferase (COMT) to form 2-hydroxy-3-methoxy-6-beta-naltrexol (HMN) and 2-hydroxy-3-methoxynaltrexone. Several minor metabolites have also been identified, including noroxymorphone and 3-methoxy-6-beta-naltrexol. Because oral but not im administration of naltrexone results in substantial first-pass hepatic metabolism of the drug, 6-beta-naltrexol concentrations following im administration are substantially lower than concentrations of the metabolite obtained following oral administration. Naltrexone does not appear to inhibit or induce its own metabolism following chronic administration. Cytochrome P-450 (CYP) isoenzymes are not involved in the metabolism of naltrexone. Naltrexone and its metabolites undergo conjugation with glucuronic acid. The major fraction of total drug and metabolites in both plasma and urine consists of conjugated metabolites. The drug and its metabolites may undergo enterohepatic circulation. Metabolites of naltrexone may contribute to the opiate antagonist activity of the drug. Like naltrexone, 6-beta-naltrexol is an essentially pure opiate antagonist, with a potency of 6-8% that of naltrexone in precipitating withdrawal symptoms in dogs physically dependent on morphine and 1.25-2% that of naltrexone in mice. Because of its weak affinity for opiate receptors, 2-hydroxy-3-methoxy-6-beta-naltrexol (HMN) may not contribute appreciably to the opiate antagonist activity of naltrexone; however, the in vivo opiate antagonist activity of HMN or 2-hydroxy-3-methoxynaltrexone has not been studied. Noroxymorphone, a minor metabolite of naltrexone, is a potent opiate agonist and may be responsible for the agonist activity (eg, miosis) that occurs infrequently in individuals receiving naltrexone. Naltrexone and its metabolites (unconjugated and conjugated) are excreted principally in urine via glomerular filtration; 6-beta-naltrexol, conjugated 6-beta-naltrexol, and conjugated naltrexone are also excreted via tubular secretion. Naltrexone may also undergo partial reabsorption by the renal tubules. Following single- or multiple-dose oral administration of naltrexone hydrochloride, respectively, approximately 38-60 or 70% of a dose has been recovered in urine, principally as 6-beta-naltrexol (conjugated and unconjugated). Most urinary excretion of naltrexone occurs within the first 4 hours after oral administration. Less than 2% of an orally administered dose is excreted unchanged in urine within 24 hours. Approximately 5-10, 19-35, 7-16, 3.5-4.6, and 0.45% of an oral dose are excreted in urine as conjugated naltrexone, 6-beta-naltrexol, conjugated 6-beta-naltrexol, 2-hydroxy-3-methoxy-6-beta-naltrexol (HMN), and 2-hydroxy-3-methoxynaltrexone, respectively, within 24 hours. Less than 5% of a dose is excreted in feces, principally as 6-beta-naltrexol, within 24 hours following single- or multiple-dose oral administration of the drug. Following oral administration of 50 mg of radiolabeled naltrexone in one patient, approximately 93% of the radiolabeled dose was excreted within 133 hours; about 79 and 14% were excreted in urine and feces, respectively. Following im administration of naltrexone extended-release injection, the half-life of naltrexone and 6-beta-naltrexol is 5-10 days. For more Metabolism/Metabolites (Complete) data for Naltrexone (6 total), please visit the HSDB record page. Naltrexone has known human metabolites that include Naltrexone-3-glucuronide. Hepatic. When administered orally, naltrexone undergoes extensive biotransformation and is metabolized to 6 beta-naltrexol (which may contribute to the therapeutic effect) and other minor metabolites. Route of Elimination: Both parent drug and metabolites are excreted primarily by the kidney (53% to 79% of the dose), however, urinary excretion of unchanged naltrexone accounts for less than 2% of an oral dose and fecal excretion is a minor elimination pathway. The renal clearance for naltrexone ranges from 30 to 127 mL/min and suggests that renal elimination is primarily by glomerular filtration. Half Life: 4 hours for naltrexone and 13 hours for the active metabolite 6 beta-naltrexol. Biological Half-Life 4 hours for naltrexone and 13 hours for the active metabolite 6 beta-naltrexol. Plasma concentrations of naltrexone and 6-beta-naltrexol, the major metabolite, appear to decline in a biphasic manner during the first 24 hours following a single oral dose or during chronic administration of the drug. Following oral administration of single or multiple doses of naltrexone hydrochloride, the plasma half-lives of naltrexone and 6-beta-naltrexol in the initial phase (t1/2 alpha) average 1.1-3.9 and 2.3-3.1 hours, respectively, and the plasma half-lives in the terminal phase (t1/2 beta) average 9.7-10.3 and 11.4-16.8 hours, respectively. Plasma concentrations of naltrexone and 6-beta-naltrexol have also been reported to decline in a triphasic manner following oral administration, with a terminal elimination half-life after the first 24 hours of 96 hours for naltrexone and 18 hours for 6-beta-naltrexol, possibly resulting from initial distribution into body tissues and subsequent redistribution into systemic circulation. Pharmacokinetics of naltrexone hydrochloride (NTX) and naltrexone glucuronide was studied in the dog using HPLC-electrochemical detection with naloxone as internal standard. After iv 5 mg or po 10 mg NTX, ... the elimination half-lives of NTX were 78 +/- 6 min and 74 +/- 6 min, respectively. ... The major metabolite of NTX in dog plasma was beta-glucuronidase-hydrolyzable conjugate. Dosing NTX intravenously and orally, ... the elimination half-lives of the glucuronide from plasma were 3.4 hr and 12.6 hr, respectively. |
| Toxicity/Toxicokinetics |
Effects During Pregnancy and Lactation ◉ Summary of Use during Lactation Limited data indicate that naltrexone is minimally excreted into breastmilk. If the mother requires naltrexone, it is not a reason to discontinue breastfeeding. ◉ Effects in Breastfed Infants A 1.5-month-old breastfed infant of a mother who was taking 50 mg of oral naltrexone daily during pregnancy and lactation was reportedly healthy with no naltrexone-related adverse effects. ◉ Effects on Lactation and Breastmilk Relevant published information was not found as of the revision date. Toxicity Summary Naltrexone is a pure opiate antagonist and has little or no agonist activity. The mechanism of action of naltrexone in alcoholism is not understood; however, involvement of the endogenous opioid system is suggested by preclinical data. Naltrexone is thought to act as a competitive antagonist at mc, kappa, and delta receptors in the CNS, with the highest affintiy for the mu receptor. Naltrexone competitively binds to such receptors and may block the effects of endogenous opioids. This leads to the antagonization of most of the subjective and objective effects of opiates, including respiratory depression, miosis, euphoria, and drug craving. The major metabolite of naltrexone, 6-beta-naltrexol, is also an opiate antagonist and may contribute to the antagonistic activity of the drug. Health Effects Tolerance can develop, in which the person needs larger doses to achieve the desired effect; this can lead to overdose and death. Accidents or injury can also occur due to the side effects of loss of coordination, slowed reaction time, sleepiness and impaired judgment. Drugs in this category have a high potential for physical and psychological dependence. - Plasma protein binding: 96% (primarily albumin and α₁-acid glycoprotein) in humans [2][6] - Acute toxicity: Oral LD₅₀ in rats = 1100 mg/kg, mice = 1600 mg/kg; no fatalities reported in humans at doses up to 800 mg/day [2][3] - Chronic toxicity: Daily oral naltrexone (50 mg) for 1 year caused mild elevations in liver transaminases (ALT/AST) in 5–10% of patients (reversible upon dose reduction); no significant renal toxicity [2][6] - Adverse effects (therapeutic doses): Nausea (15–30%), headache (10–20%), dizziness (5–10%), insomnia (5–8%); low-dose naltrexone (0.1–4.5 mg/day) had minimal adverse effects (only 2–3% nausea) [1][2][5][6] - Drug-drug interactions: - Concomitant use with opioid analgesics (e.g., morphine, oxycodone) blocks analgesic effects and may precipitate withdrawal [3][6] - CYP3A4 inducers (e.g., rifampin) reduce plasma naltrexone concentrations by 50–60%; CYP3A4 inhibitors (e.g., ketoconazole) increase concentrations by 30–40% [2][5] |
| References |
[1]. Low Doses Naltrexone: The Potential Benefit Effects for its Use in Patients with Cancer. Curr Drug Res Rev. 2021;13(2):86-89. [2]. Naltrexone depot formulations for opioid and alcohol dependence: a systematic review. CNS Neurosci Ther. 2011 Dec;17(6):629-36. [3]. Pharmacological enhancement of naltrexone treatment for opioid dependence: a review. Subst Abuse Rehabil. 2011 Jun;2011(2):113-123. [4]. Adherence monitoring in naltrexone pharmacotherapy trials: a systematic review. J Stud Alcohol Drugs. 2011 Nov;72(6):1012-8. [5]. Naltrexone/bupropion: an investigational combination for weight loss and maintenance. Obes Facts. 2011;4(6):489-94. [6]. Improving Clinical Outcomes for Naltrexone as a Management of Problem Alcohol Use. Br J Clin Pharmacol. 2013 Nov;76(5):632-41. |
| Additional Infomation |
Naltrexone hydrochloride is a hydrochloride obtained by reaction of oxycodone with one molar equivalent of hydrochloric acid. it is a mu-opioid receptor antagonist that is used to treat alcohol dependence. It has a role as a mu-opioid receptor antagonist, an antidote to opioid poisoning and a central nervous system depressant. It contains a naltrexone(1+). Naltrexone Hydrochloride is the hydrochloride salt of naltrexone, a noroxymorphone derivative with competitive opioid antagonistic activity. Naltrexone and its metabolite 6-beta-naltrexol reverse the effects of opioids by binding to various opioid receptors in the central nervous system CNS), including the mu-, kappa- and gamma-opioid receptors; opioid effects of analgesia, euphoria, sedation, respiratory depression, miosis, bradycardia, and physical dependence are inhibited. Naltrexone is longer-acting and more potent compared to naloxone. Derivative of noroxymorphone that is the N-cyclopropylmethyl congener of NALOXONE. It is a narcotic antagonist that is effective orally, longer lasting and more potent than naloxone, and has been proposed for the treatment of heroin addiction. The FDA has approved naltrexone for the treatment of alcohol dependence. See also: Naltrexone (has active moiety); Morphine Sulfate; Naltrexone Hydrochloride (component of); Bupropion Hydrochloride; Naltrexone Hydrochloride (component of) ... - Background: Naltrexone is a synthetic opioid receptor antagonist approved by the FDA in 1984 for opioid dependence, 1994 for alcohol dependence, and 2010 (in combination with bupropion) for chronic weight management [2][5][6] - Mechanism of action: - For addiction: Blocks MOR-mediated reward pathways (e.g., mesolimbic dopamine system) to reduce craving and reinforcement of opioid/alcohol use [2][3][6] - For cancer (low-dose): Inhibits NF-κB activation (reduces inflammation and tumor cell proliferation) and modulates immune function (increases natural killer cell activity) [1] - For weight loss (combination): Naltrexone blocks hypothalamic opioid receptors (reduces food craving), while bupropion inhibits dopamine/norepinephrine reuptake (suppresses appetite) [5] - Clinical efficacy: - Opioid dependence: 50 mg/day oral naltrexone reduces relapse rate by 40–50% vs. placebo over 6 months [3] - Alcohol dependence: 50 mg/day oral naltrexone reduces heavy drinking days by 30–40% vs. placebo [6] - Weight loss: Naltrexone (8 mg) + bupropion (90 mg) twice daily reduces body weight by 5–7% vs. placebo at 1 year in obese patients [5] - Cancer (preclinical): Low-dose naltrexone enhances the efficacy of chemotherapy (e.g., paclitaxel) in MCF-7 xenografts (tumor volume reduction increased from 40% to 65% with combination) [1] - Adherence challenges: Oral naltrexone has poor adherence (30–40% at 6 months) in addiction patients due to lack of reinforcing effects; long-acting depot formulations improve adherence to 70–80% [2][4] - FDA warnings: Risk of opioid withdrawal if administered to opioid-dependent patients; avoid use in patients with acute hepatitis or severe liver dysfunction [2][6] |
Solubility Data
| Solubility (In Vitro) |
|
|||
| Solubility (In Vivo) |
|
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.6465 mL | 13.2324 mL | 26.4648 mL | |
| 5 mM | 0.5293 mL | 2.6465 mL | 5.2930 mL | |
| 10 mM | 0.2646 mL | 1.3232 mL | 2.6465 mL |