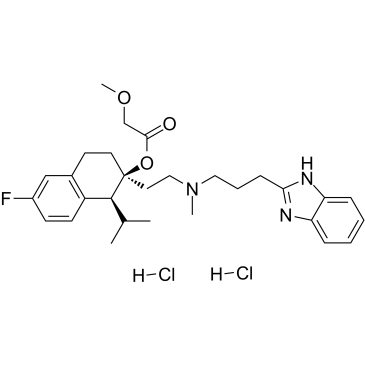
Mibefradil dihydrochloride (Ro 40-5967; trade name: Posicor), the dihydrochloride salt of miberfradil, is a CCB/calcium channel blocker with anti-hypertensive activity. It has with moderate selectivity for T-type Ca2+ channels displaying IC50s of 2.7 μM and 18.6 μM for T-type and L-type currents, respectively. It is an approved drug for the treatment of hypertension and chronic angina pectoris.
Physicochemical Properties
| Molecular Formula | C29H40CL2FN3O3 |
| Molecular Weight | 568.5506 |
| Exact Mass | 567.243 |
| Elemental Analysis | C, 61.26; H, 7.09; Cl, 12.47; F, 3.34; N, 7.39; O, 8.44 |
| CAS # | 116666-63-8 |
| Related CAS # | Mibefradil;116644-53-2;Mibefradil dihydrochloride hydrate;1049728-52-0 |
| PubChem CID | 60662 |
| Appearance | White to yellow solid powder |
| Boiling Point | 647.6ºC at 760mmHg |
| Flash Point | 345.5ºC |
| Vapour Pressure | 1.17E-16mmHg at 25°C |
| LogP | 6.874 |
| Hydrogen Bond Donor Count | 3 |
| Hydrogen Bond Acceptor Count | 6 |
| Rotatable Bond Count | 12 |
| Heavy Atom Count | 38 |
| Complexity | 709 |
| Defined Atom Stereocenter Count | 2 |
| SMILES | CC(C)[C@H]1C2=C(CC[C@@]1(CCN(C)CCCC3=NC4=CC=CC=C4N3)OC(=O)COC)C=C(C=C2)F.Cl.Cl |
| InChi Key | MTJLQTFHJIHXIX-GDUXWEAWSA-N |
| InChi Code | InChI=1S/C29H38FN3O3.2ClH/c1-20(2)28-23-12-11-22(30)18-21(23)13-14-29(28,36-27(34)19-35-4)15-17-33(3)16-7-10-26-31-24-8-5-6-9-25(24)32-26;;/h5-6,8-9,11-12,18,20,28H,7,10,13-17,19H2,1-4H3,(H,31,32);2*1H/t28-,29-;;/m0../s1 |
| Chemical Name | [(1S,2S)-2-[2-[3-(1H-benzimidazol-2-yl)propyl-methylamino]ethyl]-6-fluoro-1-propan-2-yl-3,4-dihydro-1H-naphthalen-2-yl] 2-methoxyacetate;dihydrochloride |
| Synonyms | Mibefradil dihydrochloride; 116666-63-8; Posicor; Mibefradil HCl; Mibefradil dihydrochloride [USAN]; Mibefradil (dihydrochloride); Mibefradil hydrochloride; Ro 40-5967; |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month Note: Please store this product in a sealed and protected environment (e.g. under nitrogen), avoid exposure to moisture. |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
T-type calcium channel (IC50 = 2.7 μM); (L-type calcium channel(IC50 = 18.6 μM) T-type voltage-gated Ca²⁺ channel blocker. It is also noted to possibly inhibit K⁺ channels at higher concentrations (20 µM) based on observed membrane depolarization and slowed repolarisation, which is consistent with K⁺ channel inhibition reported in other cell types[2] T-type calcium channel blocker [3] |
| ln Vitro |
T-type and L-type currents are reversibly inhibited by mibefradil dihydrochloride, with IC50 values of 2.7 and 18.6 μM, respectively. While T-type current suppression is independent of voltage, L-type current suppression is reliant on voltage. The T-shaped current is already blocked by Ro 40-5967 at a holding potential of -100 mV [1]. Mibefradil significantly depolarized the membrane potential (from -83±1 mV to -71±5 mV) at higher concentrations (20 μM), decreased the repolarization rate (44±16%), and lowered the amplitude of the excitatory junction potential (37±10%). The membrane potential exhibits a notable depolarization and repolarization slowdown at higher concentrations of Mibefradil dihydrochloride (20 μM). The observed effects of Mibefradil align with the evidence of K+ channel blockage in human myoblasts and other cell types [2]. At a concentration of 10 µM, mibefradil dihydrochloride had no significant effect on the amplitude of excitatory junction potentials (EJPs) in smooth muscle cells of the mouse vas deferens (-3 ± 10%) or on the amplitude of neuroeffector Ca²⁺ transients (NCTs) (3 ± 13%)[2] At a higher concentration (20 µM), mibefradil dihydrochloride reduced the amplitude of EJPs by 37 ± 10%, slowed the rate of repolarisation by 44 ± 16%, and caused significant membrane depolarization (from -83 ± 1 mV to -71 ± 5 mV)[2] The drug did not affect the probability of detecting an NCT following a stimulus (PNCT) at 10 µM[2] |
| ln Vivo |
Following a 4-week treatment period, hearing thresholds in C57BL/6J mice aged 24 to 26 weeks varied. The 24 kHz hearing threshold of both the benidipine- and Mibefradil dihydrochloride-treated groups was considerably (P<0.05) lower than that of the saline-treated group[3]. The expression of CaV3.2 in the DRG and spinal cord of rats in the Mibefradil dihydrochloride or NSC 64013 group was considerably lower than in the normal saline group [4]. Seven days after SNL, CaV3.2 protein levels were upregulated in ipsi-lateral L5/6 spinal cord and dorsal root ganglia (DRG) in immunofluorescence and Western blotting studies. Compared with the saline-treated group, rats receiving mibefradil or ethosuximide showed significant lower CaV3.2 expression in the spinal cord and DRG. No obvious histopathologic change in hematoxylin-eosin and toluidine blue staining were observed in all tested groups. Conclusion: In this study, we demonstrate that SNL-induced CaV3.2 upregulation in the spinal cord and DRG was attenuated by intrathecal infusion of mibefradil or ethosuximide. No obvious neurotoxicity effects were observed in all the tested groups. Our data suggest that continuous intrathecal infusion of TCC blockers may be considered as a promising alternative for the treatment of nerve injury-induced pain.[4] In 24-26-week-old C57BL/6J mice, oral administration of mibefradil dihydrochloride at 30 mg/kg/day for 4 consecutive weeks significantly decreased the hearing threshold at 24 kHz compared to the saline-treated group (P < 0.05). The hearing threshold at 32 kHz also showed a decreasing trend, but the difference was not statistically significant[3] Distortion product otoacoustic emission (DPOAE) amplitudes were significantly increased at F2 frequencies of 11.3 kHz and 13.4 kHz in the mibefradil dihydrochloride-treated group compared to the saline-treated group (P < 0.05), indicating improved outer hair cell (OHC) function[3] Scanning electron microscopy (SEM) analysis showed no obvious loss of outer hair cells (OHCs) in the mibefradil dihydrochloride-treated group, although the stereocilia of inner hair cells (IHCs) remained disorganized and sparse[3] |
| Enzyme Assay | The effects of Mibefradil/Ro 40-5967, a nondihydropyridine Ca++ channel blocker, on low-voltage activated (T-type) and high-voltage activated (L-type) Ca++ channels were compared. L-type barium currents were measured in Chinese hamster ovary cells stably transfected with the alpha 1 subunit of the class Cb Ca++ channel. T-type barium currents were investigated in human medullary thyroid carcinoma cells. The Ba++ currents of human medullary thyroid carcinoma cells were transient, activated at a threshold potential of -50 mV with the maximum at -14 +/- 3.2 mV and blocked by micromolar Ni++. The T- and L-type current inactivated with time constants of 33.4 +/- 4.1 and 416 +/- 26 msec at maximum barium currents, respectively. Ro 40-5967 inhibited reversibly the T- and L-type currents with IC50 values of 2.7 and 18.6 microM, respectively. The inhibition of the L-type current was voltage-dependent, whereas that of the T-type current was not. Ro 40-5967 blocked T-type current already at a holding potential of -100 mV. The different types of block, i.e., voltage-dependent vs. tonic block, may contribute to the pharmacological profile of Ro 40-5967 in intact animals.[1] |
| Cell Assay | Smooth muscle cells in whole mouse deferens were loaded with the Ca(2+) indicator Oregon Green 488 BAPTA-1 AM and viewed with a confocal microscope. Ryanodine (10 microM) decreased the amplitude of NCTs by 45 +/- 6 %. Cyclopiazonic acid slowed the recovery of NCTs (from a time course of 200 +/- 10 ms to 800 +/- 100 ms). Caffeine (3 mM) induced spontaneous focal smooth muscle Ca(2+) transients (sparks). Neither of the T-type Ca(2+) channel blockers NiCl2 (50 microM) or mibefradil dihydrochloride (10 microM) affected the amplitude of excitatory junction potentials (2 +/- 5 % and -3 +/- 10 %) or NCTs (-20 +/- 36 % and 3 +/- 13 %). In about 20 % of cells, NCTs were associated with a local, subcellular twitch that remained in the presence of the alpha1-adrenoceptor antagonist prazosin (100 nM), showing that NCTs can initiate local contractions. Slow (5.8 +/- 0.4 microm s(-1)), spontaneous smooth muscle Ca(2+) waves were occasionally observed. Thus, Ca(2+) stores initially amplify and then sequester the Ca(2+) that enters through P2X receptors and there is no amplification by local voltage-gated Ca(2+) channels.[2] |
| Animal Protocol |
Male Sprague-Dawley rats (200-250 g) were used for right L5/6 SNL to induce neuropathic pain. Intrathecal infusion of saline or TCC blockers [mibefradil (0.7 μg/h) or ethosuximide (60 μg/h)] was started after surgery for 7 days. Fluorescent immunohistochemistry and Western blotting were used to determine the expression pattern and protein level of CaV3.2. Hematoxylin-eosin and toluidine blue staining were used to evaluate the neurotoxicity of tested agents.[4] The aim of the present study was to investigate the protective effect of T-type calcium channel blockers against presbycusis, using a C57BL/6J mice model. The expression of three T-type calcium channel receptor subunits in the cochlea of 6-8-week-old C57BL/6J mice was evaluated using reverse transcription-quantitative polymerase chain reaction. The results confirmed that the three subunits were expressed in the cochlea. In addition, the capacity of T-type calcium channel blockers to protect the cochlear hair cells of 24-26-week-old C57BL/6J mice was investigated in mice treated with mibefradil, benidipine or saline for 4 weeks. Differences in hearing threshold were detected using auditory brainstem recording (ABR), while differences in amplitudes were measured using a distortion product otoacoustic emission (DPOAE) test. The ABR test results showed that the hearing threshold significantly decreased at 24 kHz in the mibefradil-treated and benidipine-treated groups compared with the saline-treated group. The DPOAE amplitudes in the mibefradil-treated group were increased compared with those in the saline-treated group at the F2 frequencies of 11.3 and 13.4 kHz. Furthermore, the DPOAE amplitudes in the benidipine-treated group were increased compared with those in the saline-treated group at an F2 frequency of 13.4 kHz. The loss of outer hair cells (OHCs) was not evident in the mibefradil-treated group; however, the stereocilia of the inner hair cells (IHCs) were disorganised and sparse. In summary, these results indicate that the administration of a T-type calcium channel blocker for four consecutive weeks may improve the hearing at 24 kHz of 24-26-week-old C57BL/6J mice. The function and morphology of the OHCs of the C57BL/6J mice were significantly altered by the administration of a T-type calcium channel blocker; however, the IHCs were unaffected.[3] Experiments were conducted on isolated vas deferens from 8- to 12-week-old Balb/c mice. The tissue was dissected, loaded with Ca²⁺ indicator, and placed in an organ bath for confocal imaging or intracellular recording. Mibefradil dihydrochloride was applied via perfusion at final bath concentrations of 10 µM or 20 µM. Field stimulation (0.33 Hz or 2 Hz) was applied via electrodes to evoke responses. Recordings were made before and after drug application to assess effects on EJPs and NCTs[2] Thirty 24-26-week-old male C57BL/6J mice were randomly divided into three groups: saline control, mibefradil dihydrochloride treatment, and benidipine treatment. Mibefradil dihydrochloride was dissolved in physiological saline. It was administered orally by gavage at a dosage of 30 mg/kg/day for four consecutive weeks[3] Following the treatment period, auditory brainstem response (ABR) and distortion product otoacoustic emission (DPOAE) tests were performed to assess hearing function and outer hair cell activity, respectively[3] For ABR testing, mice were anesthetized with an intramuscular injection of xylazine (25 mg/kg) and ketamine (100 mg/kg). Subcutaneous needle electrodes were placed at the vertex and mastoid prominences. Tone burst stimuli (5 ms duration) were delivered at frequencies of 8, 16, 24, and 32 kHz. The sound pressure level was decreased from 100 dB in steps until a clear wave response was elicited[3] For DPOAE testing, an acoustic probe was inserted into the external auditory meatus. Two primary tones (F1 and F2, with a frequency ratio of 1.25) were presented at intensities L1=65 dB SPL and L2=55 dB SPL. The amplitude of the distortion product (2F1-F2) was recorded at 12 specific F2 frequencies ranging from 6.7 to 39.8 kHz[3] After functional tests, mice were sacrificed by cervical dislocation. Cochleae were harvested for scanning electron microscopy (SEM) analysis. For SEM, cochleae were fixed in 2.5% glutaraldehyde, post-fixed in 1% osmium tetroxide, dehydrated through a graded ethanol series, critical-point dried, and sputter-coated with gold before observation[3] |
| ADME/Pharmacokinetics |
Absorption Bioavailability after a single dose is 70%. After multiple dosing, the proportion of mibefradil undergoing first-pass metabolism is reduced, resulting in a steady state bioavailability of approximately 90%. Food does not affect the rate or extent of absorption of mibefradil. Metabolism / Metabolites The two metabolic pathways that mibefradil undergoes are esterase-catalyzed hydrolysis of the ester side chain (producing an alcohol metabolite) and cytochrome P450 3A4-catalyzed oxidation (that becomes less important during chronic dosing). The pharmacologic effect of the metabolite is approximately 10% of that of the parent mibefradil. Biological Half-Life 17 to 25 hours at steady state. |
| Toxicity/Toxicokinetics |
Protein Binding: ≥ 99%, primarily to alpha 1-acid glycoprotein. rat LD50 oral >800 mg/kg Cardiovascular Drug Reviews., 9(4), 1991 rat LD50 intravenous 23 mg/kg Cardiovascular Drug Reviews., 9(4), 1991 mouse LD50 oral >800 mg/kg Cardiovascular Drug Reviews., 9(4), 1991 mouse LD50 intravenous 35 mg/kg Cardiovascular Drug Reviews., 9(4), 1991 |
| References |
[1]. The Ca(++)-channel blocker Ro 40-5967 blocks differently T-type and L-type Ca++ channels. J Pharmacol Exp Ther. 1994 Dec;271(3):1483-8. [2]. The sources and sequestration of Ca(2+) contributing to neuroeffector Ca(2+) transients in the mouse vas deferens. J Physiol. 2003 Dec 1;553(Pt 2):627-35. [3]. Protection of the cochlear hair cells in adult C57BL/6J mice by T-type calcium channel blockers. Exp Ther Med. 2016 Mar;11(3):1039-1044. [4]. Chronic intrathecal infusion of T-type calcium channel blockers attenuates CaV3.2 upregulation in nerve-ligated rats. Acta Anaesthesiol Taiwan. 2016 Oct 17. pii: S1875-4597(16)30071-6. |
| Additional Infomation |
A benzimidazoyl-substituted tetraline that selectively binds and inhibits CALCIUM CHANNELS, T-TYPE. Mibefradil dihydrochloride was used as a T-type Ca²⁺ channel blocker to investigate its role in neuroeffector Ca²⁺ transients in mouse vas deferens smooth muscle[2] It was donated by Dr. E. V. Gutknecht and P. Weber from Hoffmann-La Roche[2] Stock solutions were prepared at 10 mM in distilled water and stored frozen until use[2] The study concluded that T-type Ca²⁺ channels do not contribute to the local Ca²⁺ influx following P2X receptor activation in this tissue[2] The study investigated the protective effect of T-type calcium channel blockers against age-related hearing loss (presbycusis) using a C57BL/6J mouse model[3] Mibefradil dihydrochloride was described as a selective T-type calcium channel blocker[3] The expression of three T-type calcium channel subunits (α1G, α1H, α1I corresponding to CaV3.1, CaV3.2, CaV3.3) was confirmed in the cochlea of 6-8-week-old C57BL/6J mice by RT-qPCR, providing a rationale for using T-type channel blockers[3] The results suggest that mibefradil dihydrochloride administration can protect outer hair cells (OHCs) from age-related degeneration and improve high-frequency hearing in this mouse model, but it does not appear to protect inner hair cells (IHCs)[3] |
Solubility Data
| Solubility (In Vitro) | H2O : ~150 mg/mL (~263.83 mM) |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 1.7589 mL | 8.7943 mL | 17.5886 mL | |
| 5 mM | 0.3518 mL | 1.7589 mL | 3.5177 mL | |
| 10 mM | 0.1759 mL | 0.8794 mL | 1.7589 mL |