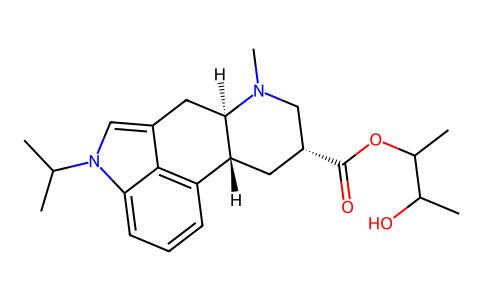
Physicochemical Properties
| Molecular Formula | C23H32N2O3 |
| Molecular Weight | 384.52 |
| Exact Mass | 384.241 |
| CAS # | 32896-53-0 |
| Related CAS # | 60634-51-7 |
| PubChem CID | 3034814 |
| Appearance | Typically exists as solid at room temperature |
| Density | 1.25±0.1 g/cm3(Predicted) |
| Boiling Point | 554.8±50.0 °C(Predicted) |
| LogP | 3.1 |
| Hydrogen Bond Donor Count | 1 |
| Hydrogen Bond Acceptor Count | 4 |
| Rotatable Bond Count | 5 |
| Heavy Atom Count | 28 |
| Complexity | 582 |
| Defined Atom Stereocenter Count | 3 |
| SMILES | O(C(C)C(C)O)C([C@H]1CN(C)[C@@H]2CC3=CN(C(C)C)C4=CC=CC(=C34)[C@H]2C1)=O |
| InChi Key | JQYLIGHHVGCTPR-LYRPIDSHSA-N |
| InChi Code | InChI=1S/C23H32N2O3/c1-13(2)25-12-16-10-21-19(18-7-6-8-20(25)22(16)18)9-17(11-24(21)5)23(27)28-15(4)14(3)26/h6-8,12-15,17,19,21,26H,9-11H2,1-5H3/t14?,15?,17-,19-,21-/m1/s1 |
| Chemical Name | 3-hydroxybutan-2-yl (6aR,9R,10aR)-7-methyl-4-propan-2-yl-6,6a,8,9,10,10a-hexahydroindolo[4,3-fg]quinoline-9-carboxylate |
| Synonyms | LY-53857 free base; 32896-53-0; OK43YC00I7; UNII-OK43YC00I7; 3-hydroxybutan-2-yl (6aR,9R,10aR)-7-methyl-4-propan-2-yl-6,6a,8,9,10,10a-hexahydroindolo[4,3-fg]quinoline-9-carboxylate; Ergoline-8beta-carboxylic acid, 1-isopropyl-6-methyl-, 2-hydroxy-1-methylpropyl ester; 4-Isopropyl-7-methyl-9-(2-hydroxy-1-methylpropoxycarbonyl)-4,6,6alpha,7,8,9,10,10alpha-octahydroindolo(4,3-fg)quinoline; Ergoline-8-carboxylic acid, 6-methyl-1-(1-methylethyl)-, 2-hydroxy-1-methylpropyl ester, (8beta)-; |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets | 5-HT2 receptor (ED50 = 17.5 nM) |
| ln Vivo | This study was carried out aiming to reach behavioral and neuropharmacological evidence of the permeability of the blood-brain barrier (BBB) to serotonin systemically administered in quails. Serotonin injected by a parenteral route (250-1000 microg x kg(-1), sc) elicited a sequence of behavioral events concerned with a sleeping-like state. Sleeping-like behaviors began with feather bristling, rapid oral movements, blinking and finally crouching and closure of the eyes. Previous administration of 5-HT2C antagonist, LY53857 (3 mg x kg(-1), sc) reduced the episodes of feather bristling and rapid oral movements significantly but without altering the frequency of blinking and closure of the eyes. Treatment with the 5-HT2A/2C antagonist, ketanserin (3 mg x kg(-1), sc) did not affect any of the responses evoked by the serotonin. Quipazine (5 mg x kg(-1), sc) a 5-HT2A/2C/3 agonist induced intense hypomotility, long periods of yawning-like and sleeping-like states. Previous ketanserin suppressed gaping responses and reduced hypomotility, rapid oral movements and bristling but was ineffective for remaining responses induced by quipazine. Results showed that unlike mammals, serotonin permeates the BBB and activates hypnogenic mechanisms in quails. Studies using serotoninergic agonist and antagonists have disclosed that among the actions of the serotonin, feather bristling, rapid oral movements and yawning-like state originated from activation of 5-HT2 receptors while blinking and closure of the eyes possibly require other subtypes of receptors [1]. |
| References | [1]. Behavioral and neuropharmacological evidence that serotonin crosses the blood-brain barrier in Coturnix japonica (Galliformes; Aves). Braz J Biol. 2007 Feb;67(1):167-71. |
| Additional Infomation | The highly effective anorexigen (+)-fenfluramine was widely used to control body weight until the association with primary pulmonary hypertension and valvular heart disease. (+)-Norfenfluramine is the major hepatic metabolite of (+)-fenfluramine and is primarily responsible for the anorexic effect as well as side effects. We reported that (+)-norfenfluramine causes vasoconstriction and a blood pressure increase in rats with normal blood pressure via the 5-hydroxytryptamine (5-HT)2A receptor. With the knowledge that (+)-norfenfluramine also has affinity for 5-HT2B receptors and that arterial 5-HT2B receptor expression is up-regulated in deoxycorticosterone acetate (DOCA)-salt hypertension, we tested the hypothesis that (+)-norfenfluramine-induced vasoconstriction and pressor effects are potentiated in DOCA-salt hypertensive rats in a 5-HT2 receptor-dependent manner. Contractions of arteries were measured using an isolated tissue bath system or myograph. Mean arterial blood pressure was measured in chronically instrumented conscious rats. Effects of (+)-norfenfluramine in stimulating arterial contraction (leftward shift versus SHAM, aorta, 5.13-fold; renal artery, 1.95-fold; mesenteric resistance artery, 1.77-fold) and raising blood pressure were significantly enhanced in hypertension. In arteries from both normotensive and hypertensive rats, (+)-norfenfluramine-induced contraction in aorta was inhibited by 5-HT2A receptor antagonists, ketanserin and LY53857 (4-isopropyl-7-methyl-9-(2-hydroxy-1-meth ylpropoxycarbonyl)4,6,6a,7,8,9,10,10a-octahydroindolo[4,3-fg]quinoline), but not by the 5-HT2B receptor antagonist, LY272015 [6-chloro-5-methyl-N-(5-quinolinyl)-2,3-dihydro-1H-indole-1-carboxamide]. Ketanserin (3 mg/kg) reduced (+)-norfenfluramine-induced pressor response in both SHAM and DOCA rats. Our results demonstrate that (+)-norfenfluramine-induced arterial contraction and blood pressure increases are potentiated in DOCA-salt hypertensive rats. However, it is the 5-HT2A receptor and not the 5-HT2B receptor that participates in these effects. https://pubmed.ncbi.nlm.nih.gov/17289838/ |
Solubility Data
| Solubility (In Vitro) | May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.6006 mL | 13.0032 mL | 26.0064 mL | |
| 5 mM | 0.5201 mL | 2.6006 mL | 5.2013 mL | |
| 10 mM | 0.2601 mL | 1.3003 mL | 2.6006 mL |