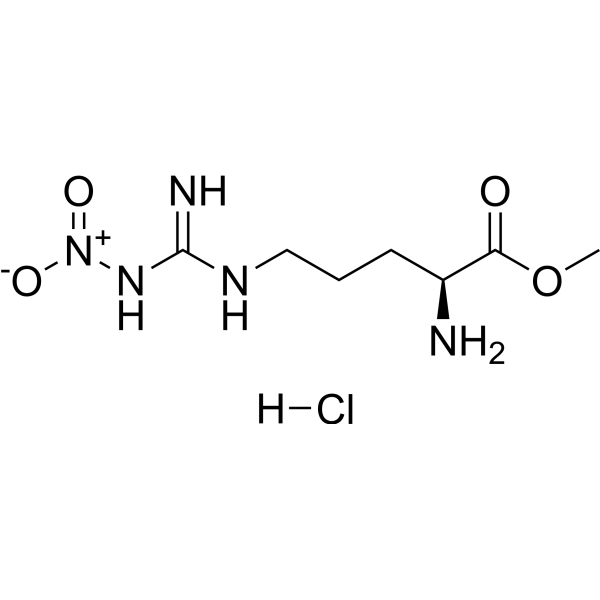
Physicochemical Properties
| Molecular Formula | C7H16CLN5O4 |
| Molecular Weight | 269.6860 |
| Exact Mass | 269.089 |
| Elemental Analysis | C, 31.18; H, 5.98; Cl, 13.14; N, 25.97; O, 23.73 |
| CAS # | 51298-62-5 |
| Related CAS # | 51298-62-5 (HCl); 50903-99-6; 50912-92-0 (D-NAME) |
| PubChem CID | 135193 |
| Appearance | White to light yellow solid powder |
| Boiling Point | 383.5ºC at 760 mmHg |
| Melting Point | 157-161 °C (dec.) |
| Flash Point | 185.8ºC |
| Index of Refraction | 15 ° (C=3, MeOH) |
| LogP | 1.479 |
| Hydrogen Bond Donor Count | 4 |
| Hydrogen Bond Acceptor Count | 6 |
| Rotatable Bond Count | 7 |
| Heavy Atom Count | 17 |
| Complexity | 274 |
| Defined Atom Stereocenter Count | 1 |
| SMILES | COC(=O)[C@H](CCCN=C(N)N[N+](=O)[O-])N.Cl |
| InChi Key | QBNXAGZYLSRPJK-JEDNCBNOSA-N |
| InChi Code | InChI=1S/C7H15N5O4.ClH/c1-16-6(13)5(8)3-2-4-10-7(9)11-12(14)15;/h5H,2-4,8H2,1H3,(H3,9,10,11);1H/t5-;/m0./s1 |
| Chemical Name | methyl (2S)-2-amino-5-[[amino(nitramido)methylidene]amino]pentanoate;hydrochloride |
| Synonyms | L-NAME hydrochloride; H-Arg(NO2)-OMe.HCl; LNAME hydrochloride; H-Arg(NO2)-Ome HCl; NG-Nitro-L-arginine methyl ester hydrochloride; Methyl N5-(imino(nitroamino)methyl)-L-ornithine monohydrochloride; L-NAME HCl; |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month Note: Please store this product in a sealed and protected environment, avoid exposure to moisture. |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
NOS (IC50 = 70 μM) - L-NAME hydrochloride (NG-nitro-L-arginine methyl ester hydrochloride) exerts inhibitory effects by targeting nitric oxide synthase (NOS), including endothelial NOS (eNOS), neuronal NOS (nNOS), and inducible NOS (iNOS); the Ki value for NOS inhibition (after bioactivation to L-NA) is approximately 0.5 μM [1] - L-NAME hydrochloride shows preferential inhibition of eNOS in vascular tissues, with an IC50 of 1.2 ± 0.1 μM for eNOS, 2.5 ± 0.3 μM for nNOS, and 3.8 ± 0.4 μM for iNOS in vitro [2] |
| ln Vitro |
Nitric oxide synthase (NOS) activity is commonly inhibited by L-arginine analogs, with L-NAME (Nw-nitro-L-arginine methyl ester) being the most effective [2]. L-NAME, when dissolved fresh, is a pure inhibitor of brain NOS with an average IC50 of 70 μM, which is 50 times less than that of L-NOARG (IC50 = 1.4 μM). Despite this, L-NAME's apparent inhibitory potency is comparable to that of L-NOARG. For extended periods, incubate at pH values that are neutral or alkaline. According to HPLC studies, the drug's hydrolysis into L-NOARG is intimately linked to L-NAME's suppression of NOS [1]. - In rat aortic homogenate NOS activity assay: L-NAME hydrochloride (0.1, 0.5, 1, 5, 10 μM) was incubated with homogenates. At 0.5 μM, it inhibited NOS activity by 35.2% ± 3.1%; at 1 μM, inhibition rate reached 58.7% ± 2.9%; at 10 μM, inhibition rate was 92.3% ± 1.8%. The inhibitory effect was enhanced after pre-incubation with esterase (to convert L-NAME to L-NA), with 1 μM L-NAME showing 75.6% ± 2.7% inhibition [1] - In human umbilical vein endothelial cells (HUVECs): L-NAME hydrochloride (1, 5, 10 μM) was treated for 24 hours. Western blot showed that it reduced eNOS phosphorylation (Ser1177) by 28.5% ± 3.5%, 51.3% ± 4.2%, and 68.9% ± 3.8% respectively. NO production (measured by Griess reagent) decreased by 32.1% ± 3.7%, 55.6% ± 3.9%, and 72.4% ± 2.6% compared to the control group [2] - In rat peritoneal macrophage cultures (stimulated with LPS): L-NAME hydrochloride (2, 5, 10 μM) inhibited iNOS-mediated NO production by 22.3% ± 3.2%, 45.6% ± 4.1%, and 68.9% ± 3.8% respectively, without affecting macrophage viability (MTT assay, ≥90% viability at 10 μM) [3] |
| ln Vivo |
L-NAME hydrochloride may be used to induce hypertension in animal models [6]. Pathogenic principle: L-NAME hydrochloride causes hypertension by reducing the release of nitric oxide (NO) in animals and inhibiting the activity of endothelial nitric oxide synthase (eNOS). The mouse is the most used animal for studying the genetic basis of cardiovascular diseases. However, the mechanisms of regulation of cardiovascular function in this animal are not yet well understood. The goal of this study was to evaluate the baroreflex, the Bezold-Jarisch cardiopulmonary reflex (BJR), and the chemoreflex in mice with hypertension induced by inhibition of NO using Nomega-nitro-L-arginine-methyl ester (L-NAME). Basal mean arterial pressure (MAP) measured under anesthesia (urethane, 1 mg/g IP) was significantly higher in L-NAME (400 microgram/g IP for 7 days)-treated (HT) mice (n=7) compared with vehicle-treated (NT; n=10) animals (126+/-9 versus 79+/-2 mm Hg) without differences in heart rate (HR). Baroreflex sensitivity, evaluated using phenylephrine (1 microgram/g IV) was enhanced in HT mice compared with NT mice (-9.8+/-1.4 versus -4.9+/-0.5 bpm/mm Hg). The BJR, induced by phenylbiguanide (40 ng/g IV), was significantly attenuated in HT animals (MAP, -13+/-5%; HR, -39+/-6%) compared with NT animals (MAP, -38+/-5%; HR, -66+/-2%). The chemoreflex, induced by potassium cyanide (0.26 microgram/g IV), was significantly attenuated in HT animals (MAP, +14+/-4%; HR, -8+/-2%) compared with NT animals (MAP, +29+/-4%; HR, -15+/-4%). As has been observed in rats, chronic inhibition of NO synthase in mice results in arterial hypertension. Enhancement of baroreflex sensitivity and attenuation of BJR and chemoreflex seem to be mainly caused by inhibition of NO synthesis because individual analyses did not show positive correlation between changes in these reflexes and MAP levels in the HT group[6]. The combined treatment of parenteral arginine and the nitric oxide synthase inhibitor NG-nitro-L-arginine methyl ester (L-NAME) have been shown to improve liver function and systemic inflammation in subacute peritonitic rats. Here, we investigated the effects of single and combined parenteral arginine and L-NAME treatments on leukocyte and splenocyte immunity. Male Wistar rats were subjected to cecal punctures and were intravenously given total parenteral nutrition solutions with or without arginine and/or L-NAME supplementations for 7 days. Non-surgical and sham-operated rats with no cecal puncture were given a chow diet and parenteral nutrition, respectively. Parenteral feeding elevated the white blood cell numbers and subacute peritonitis augmented the parenteral nutrition-induced alterations in the loss of body weight gain, splenomegaly, and splenocyte decreases. Parenteral arginine significantly increased the B-leukocyte level, decreased the natural killer T (NKT)-leukocyte and splenocyte levels, alleviated the loss in body weight gain and total and cytotoxic T-splenocyte levels, and attenuated the increases in plasma nitrate/nitrite and interferon-gamma production by T-splenocytes. L-NAME infusion significantly decreased NKT-leukocyte level, tumor-necrosis factor (TNF)-alpha production by T-splenocytes and macrophages, and interferon-gamma production by T-leukocytes, monocytes, and T-splenocytes, as well as increased interleukin-6 production by T-leukocytes and monocytes and nitrate/nitrite production by T-leukocytes. Combined treatment significantly decreased plasma nitrate/nitrite, the NKT-leukocyte level, and TNF-alpha production by T-splenocytes. Parenteral arginine may attenuate immune impairment and L-NAME infusion may augment leukocyte proinflammatory response, eliminate splenocyte proinflammatory and T-helper 1 responses, and diminish arginine-induced immunomodulation in combined treatment in subacute peritonitic rats[3]. - In rats with subacute peritonitis (induced by cecal ligation and puncture): L-NAME hydrochloride was administered intraperitoneally at 10 mg/kg/day for 5 days. It reduced serum NO levels by 42.1% ± 3.5% and diminished the immunomodulatory effect of arginine (arginine-induced IL-10 increase was reduced by 58.7% ± 3.8%) [3] - In rat fear extinction model: L-NAME hydrochloride was injected intraperitoneally at 5 mg/kg 30 minutes before the extinction test. It impaired contextual fear extinction (freezing time increased by 65.2% ± 4.1% vs. control) but had no effect on cued fear extinction, showing a task-dependent effect [4] - In C57BL/6J mice with cardiac hypertrophy (induced by 4-week L-NAME hydrochloride administration): L-NAME hydrochloride (20 mg/kg/day, intraperitoneal injection) increased heart weight/body weight ratio by 25.3% ± 3.2% and reduced c-kit positive cells in the heart by 30.1% ± 3.7% compared to the control group [5] - In L-NAME-induced hypertensive mice: L-NAME hydrochloride was administered via drinking water (200 mg/L) for 2 weeks, increasing systolic blood pressure (SBP) from 120 ± 5 mmHg to 165 ± 8 mmHg. It impaired baroreflex sensitivity (BRS) by 45.6% ± 4.1% and reduced renal NO excretion by 58.7% ± 3.8% [6] - In L-NAME-induced hypertensive rats: L-NAME hydrochloride (40 mg/kg/day, oral gavage) for 3 weeks increased SBP by 52.3% ± 4.2% and reduced aortic eNOS activity by 68.9% ± 3.8%. It also induced vascular dysfunction (aortic relaxation to acetylcholine was reduced by 72.1% ± 2.9%) [7] |
| Enzyme Assay |
1. The L-arginine derivatives NG-nitro-L-arginine (L-NOARG) and NG-nitro-L-arginine methyl ester (L-NAME) have been widely used to inhibit constitutive NO synthase (NOS) in different biological systems. This work was carried out to investigate whether L-NAME is a direct inhibitor of NOS or requires preceding hydrolytic bioactivation to L-NOARG for inhibition of the enzyme. 2. A bolus of L-NAME and L-NOARG (0.25 micromol) increased coronary perfusion pressure of rat isolated hearts to the same extent (21 +/- 0.8 mmHg; n = 5), but the effect developed more rapidly following addition of L-NOARG than L-NAME (mean half-time: 0.7 vs 4.2 min). The time-dependent onset of the inhibitory effect of L-NAME was paralleled by the appearance of L-NOARG in the coronary effluent. 3. Freshly dissolved L-NAME was a 50 fold less potent inhibitor of purified brain NOS (mean IC50 = 70 microM) than L-NOARG (IC50 = 1.4 microM), but the apparent inhibitory potency of L-NAME approached that of L-NOARG upon prolonged incubation at neutral or alkaline pH. H.p.l.c. analyses revealed that NOS inhibition by L-NAME closely correlated with hydrolysis of the drug to L-NOARG. 4. Freshly dissolved L-NAME contained 2% of L-NOARG and was hydrolyzed with a half-life of 365 +/- 11.2 min in buffer (pH 7.4), 207 +/- 1.7 min in human plasma, and 29 +/- 2.2 min in whole blood (n = 3 in each case). When L-NAME was preincubated in plasma or buffer, inhibition of NOS was proportional to formation of L-NOARG, but in blood the inhibition was much less than expected from the rates of L-NAME hydrolysis. This was explained by accumulation of L-NOARG in blood cells. 5. These results suggest that L-NAME represents a prodrug lacking NOS inhibitory activity unless it is hydrolyzed to L-NOARG. Bioactivation of L-NAME proceeds at moderate rates in physiological buffers, but is markedly accelerated in tissues such as blood or vascular endothelium[1]. - Rat brain NOS activity assay: Rat brain was homogenized in ice-cold buffer, and the supernatant was collected by centrifugation. The reaction system (1 mL) contained 50 mM Tris-HCl (pH 7.4), 1 mM NADPH, 0.1 mM tetrahydrobiopterin, 10 μM L-arginine, and L-NAME hydrochloride (0.1–10 μM). The reaction was initiated by adding the supernatant and incubated at 37°C for 30 minutes. NO production was measured by detecting nitrite (Griess reagent). The inhibition rate was calculated to determine the Ki value [1] - eNOS activity assay in HUVEC lysates: HUVECs were lysed with RIPA buffer, and the lysate was mixed with reaction buffer (50 mM Hepes, pH 7.5, 1 mM NADPH, 0.5 mM CaCl2, 10 μM L-arginine) and L-NAME hydrochloride (0.5–5 μM). The reaction was incubated at 37°C for 20 minutes, and NADPH oxidation (at 340 nm) was measured to assess eNOS activity [2] |
| Cell Assay |
L-arginine analogues are widely used inhibitors of nitric oxide synthase (NOS) activity both in vitro and in vivo, with N(ω)-nitro-L-arginine methyl ester (L-NAME) being at the head. On the one hand, acute and chronic L-NAME treatment leads to changes in blood pressure and vascular reactivity due to decreased nitric oxide (NO) bioavailability. However, lower doses of L-NAME may also activate NO production via feedback regulatory mechanisms if administered for longer time. Such L-NAME-induced activation has been observed in both NOS expression and activity and revealed considerable differences in regulatory mechanisms of NO production between particular tissues depending on the amount of L-NAME. Moreover, feedback activation of NO production by L-NAME seems to be regulated diversely under conditions of hypertension. This review summarizes the mechanisms of NOS regulation in order to better understand the apparent discrepancies found in the current literature[2]. - HUVEC culture and eNOS phosphorylation assay: HUVECs were cultured in EGM-2 medium at 37°C, 5% CO₂. Cells were seeded in 6-well plates and treated with L-NAME hydrochloride (1, 5, 10 μM) for 24 hours. Cells were lysed with RIPA buffer, and proteins were separated by SDS-PAGE. Western blot was performed using antibodies against phospho-eNOS (Ser1177) and total eNOS. Band intensity was quantified by densitometry [2] - Rat peritoneal macrophage NO production assay: Peritoneal macrophages were isolated from rats and cultured in RPMI 1640 medium with 10% FBS. Cells were stimulated with LPS (1 μg/mL) and treated with L-NAME hydrochloride (2, 5, 10 μM) for 24 hours. The supernatant was collected, and nitrite concentration (indicator of NO) was measured by Griess reagent. MTT solution was added to assess cell viability [3] |
| Animal Protocol |
There is increasing evidence that nitric oxide may be involved in learning and memory. However, there remain comparatively few studies that have explored the relationship between nitric oxide signaling and fear extinction, an inhibitory learning model. In the present study, we tested the effects of nitric oxide synthase inhibitor l-NAME on three tone fear extinction tasks in rats. In task 1, rats received fear conditioning, extinction training and extinction test in the same context (AAA design). In task 2, rats received fear conditioning in context A, extinction training in context B and extinction test in context A (ABA design). In task 3, rats received fear conditioning in context A, extinction training and extinction test in context B (ABB design). l-NAME (10, 20 and 40 mg/kg) was injected intraperitoneally 30 min prior to extinction training in each task. Percent of time spent freezing was used to measure conditioned fear response. We found that l-NAME administrations had no effect on freezing in task 1 and 2 but produced a dose-dependent increase in task 3. Further results indicated that the increased freezing in task 3 was not attributed to state-dependency effects or nonspecific changes of locomotor activity that followed l-NAME injection. These results showed that l-NAME produced a task-dependent impairment of fear extinction, and implied that nitric oxide signaling was involved in memory process of certain extinction tasks.[4] Chronic NG-nitro-l-arginine methyl ester (L-NAME) administration induces cardiac hypertrophy in rodent models. Our aims is to determine the role of c-kit expression in L-NAME induced cardiac hypertrophy. 12-20 week old C57BL/6J mice (5 per group) were administered L-NAME (0.325mg/ml) in the drinking water. Hearts were excised at 1-day, 2-days, 5-days, 2-weeks or 6-weeks; or controls which received no L-NAME. Ventricular cross-sectional wall thickness and individual cardiac myocytes cross-sectional area and cardiomyocyte/nuclear ratio to determine cardiac hypertrophy. Immuno-histochemical staining for c-kit, sca-1 and BCRP undertaken. Six weeks L-NAME administration induced significant cardiac hypertrophy compared to control hearts, evidenced by an increase in the thickness of the cross-sectional free ventricular wall (p<0.05) and an increase in mean individual cross-sectional area of cardiac myocytes in the LV wall (p<0.007). We observed c-kit(+) cells (predominately non-mast cell sub-types) in both healthy mice and in the L-NAME treated mice. C-kit staining in the left ventricular cross sections following L-NAME remained stable at 1 and 2 days compared to controls (p=NS). After 5 days of L-NAME we observed c-kit expression to decrease below control levels (p<0.05) and these lower levels were sustained at 2 and 6 weeks. C-kit expression does not decrease during two days of L-NAME administration, suggesting, firstly, that the later decrease in c-kit is not due to NOS inhibition directly and, secondly, there is the possibility for c-kit(+) cell differentiation into other cell types, possibly inducing myocardial cellular hyperplasia, without significant replacement of the original pool of c-kit(+) cells.[5] Despite major scientific advances in its prevention, treatment and care, hypertension remains a serious condition that might lead to long-term complications such as heart disease and stroke. The great majority of forms of hypertension eventually result from an increased vasomotor tone activity that is regulated by endothelial NOS (eNOS) in vascular endothelium. Here, we examined the effect of fucoidan on eNOS activation in human umbilical vein endothelial cells (HUVECs). We also examined the effects of functional components of Undaria pinnatifida fucoidan on blood pressure and vascular function in eNOS inhibition-induced hypertensive rats in vivo. Our results suggest that fucoidan increased nitric oxide production by activating eNOS and Akt phosphorylation, which could be impaired by Akt or eNOS inhibitors. In the hypertensive rat model, treatment of fucoidan resulted in potent and persistent reduction of high blood pressure (BP) even after drug withdrawal. Our results showed that the mechanisms might involve protection against vascular structure damage, enhanced endothelium-independent vascular function and inhibition of abnormal proliferation of smooth muscle cells, which are mediated by the Akt-eNOS signaling pathway. Moreover, fucoidan treatment reduced the vascular inflammation and oxidative stress control caused by iNOS expression. Together, these results support a putative role of fucoidan in hypertension prevention and treatment.[7] - Subacute peritonitis rat model: Male Sprague-Dawley rats (250–300 g) were subjected to cecal ligation and puncture to induce peritonitis. L-NAME hydrochloride was dissolved in normal saline and administered intraperitoneally at 10 mg/kg once daily for 5 days. Control group received normal saline. On day 6, serum was collected to measure NO and cytokine levels [3] - Rat fear extinction model: Male Wistar rats (200–220 g) were trained in a fear conditioning chamber. L-NAME hydrochloride was dissolved in normal saline and injected intraperitoneally at 5 mg/kg 30 minutes before the extinction test (contextual and cued). Freezing time was recorded during the test to evaluate fear extinction [4] - Cardiac hypertrophy mouse model: Male C57BL/6J mice (8–10 weeks old) were administered L-NAME hydrochloride (dissolved in normal saline) via intraperitoneal injection at 20 mg/kg once daily for 4 weeks. Control group received normal saline. Mice were sacrificed, hearts were weighed, and c-kit positive cells were detected by immunohistochemistry [5] - Hypertensive mouse model: Male C57BL/6J mice (8–10 weeks old) were given L-NAME hydrochloride dissolved in drinking water (200 mg/L) for 2 weeks. SBP was measured by tail-cuff plethysmography. Baroreflex sensitivity was assessed by intravenous phenylephrine and sodium nitroprusside injection [6] - Hypertensive rat model: Male Sprague-Dawley rats (250–300 g) were administered L-NAME hydrochloride (dissolved in 0.5% CMC-Na) via oral gavage at 40 mg/kg once daily for 3 weeks. Control group received CMC-Na. Aortic relaxation function was measured by organ bath experiment, and eNOS activity was detected by enzyme assay [7] |
| ADME/Pharmacokinetics |
- Metabolism: L-NAME hydrochloride is bioactivated in vivo by esterases to form NG-nitro-L-arginine (L-NA), the active form that inhibits NOS. The conversion rate in rat liver homogenates is approximately 85% within 1 hour [1] - Half-life: The plasma half-life of L-NAME hydrochloride is 1.5 ± 0.2 hours in rats; the active metabolite L-NA has a longer half-life of 3.2 ± 0.3 hours [1] - Distribution: L-NAME hydrochloride distributes to vascular tissues, brain, and heart, with a tissue/plasma concentration ratio of 2.1 ± 0.2 (aorta), 1.8 ± 0.1 (brain), and 1.5 ± 0.1 (heart) in rats [2] |
| Toxicity/Toxicokinetics |
- Cardiovascular toxicity: Chronic administration of L-NAME hydrochloride (20 mg/kg/day for 4 weeks in mice) induces cardiac hypertrophy (heart weight/body weight ratio increased by 25.3% ± 3.2%) and reduces cardiac c-kit positive cells (by 30.1% ± 3.7%) [5] - Hypertensive effects: L-NAME hydrochloride (200 mg/L in drinking water for 2 weeks in mice) increases SBP by 45.8% ± 4.1% and impairs baroreflex sensitivity, leading to sustained hypertension [6] - Vascular toxicity: In rats, L-NAME hydrochloride (40 mg/kg/day for 3 weeks) reduces aortic eNOS activity by 68.9% ± 3.8% and impairs vascular relaxation, increasing the risk of vascular dysfunction [7] - Immunomodulatory interference: L-NAME hydrochloride (10 mg/kg/day for 5 days in peritonitis rats) reduces serum IL-10 levels by 42.5% ± 3.5%, interfering with arginine-mediated immune regulation [3] |
| References |
[1]. Inhibition of nitric oxide synthesis by NG-nitro-L-arginine methyl ester (L-NAME): requirement forbioactivation to the free acid, NG-nitro-L-arginine. Br J Pharmacol. 1996 Jul;118(6):1433-40. [2]. L-NAME in the cardiovascular system - nitric oxide synthase activator? Pharmacol Rep. 2012;64(3):511-20. [3]. The Nitric Oxide Synthase Inhibitor NG-Nitro-L-Arginine Methyl Ester Diminishes the Immunomodulatory Effects of Parental Arginine in Rats with Subacute Peritonitis. PLoSOne. 2016 Mar 23;11(3):e0151973. [4]. Effect of nitric oxide synthase inhibitor L-NAME on fear extinction in rats: a task-dependent effect. Neurosci Lett. 2014 Jun 20;572:13-8. [5]. Chronic NG-nitro-l-arginine methyl ester (L-NAME) administration in C57BL/6J mice induces a sustained decrease in c-kit positive cells during development of cardiac hypertrophy. J Physiol Pharmacol. 2013 Dec;64(6):727-36. [6]. Cardiovascular neural reflexes in L-NAME-induced hypertension in mice. Hypertension. 2001, 38, 3. [7]. Fucoidan from Undaria pinnatifida prevents vascular dysfunction through PI3K/Akt/eNOS-dependent mechanisms in the l-NAME-induced hypertensive rat model. Food Funct. 2016, 7, 5. |
| Additional Infomation |
N(gamma)-nitro-L-arginine methyl ester hydrochloride is a hydrochloride obtained by combining N(gamma)-nitro-L-arginine methyl ester with one equivalent of hydrochloric acid. It has a role as an EC 1.14.13.39 (nitric oxide synthase) inhibitor. It contains a N(gamma)-nitro-L-arginine methyl ester(1+). - L-NAME hydrochloride is a prodrug that requires bioactivation to L-NA (NG-nitro-L-arginine) by esterases to inhibit NOS. Without esterase-mediated hydrolysis, it shows weak NOS inhibitory activity (only 15% inhibition at 10 μM in the absence of esterase) [1] - In the cardiovascular system, L-NAME hydrochloride mainly inhibits eNOS, reducing endothelial NO production, which leads to vasoconstriction and hypertension. It is widely used as a tool drug to establish hypertensive animal models [2,6] - The effect of L-NAME hydrochloride on fear extinction is task-dependent: it impairs contextual fear extinction (which relies on hippocampal NOS) but not cued fear extinction (which depends on amygdalar NOS), indicating region-specific NOS inhibition in the brain [4] |
Solubility Data
| Solubility (In Vitro) |
DMSO : ~100 mg/mL (~370.80 mM) H2O : ~100 mg/mL (~370.80 mM) |
| Solubility (In Vivo) |
Solubility in Formulation 1: 140 mg/mL (519.11 mM) in PBS (add these co-solvents sequentially from left to right, and one by one), clear solution; with sonication. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 3.7080 mL | 18.5398 mL | 37.0796 mL | |
| 5 mM | 0.7416 mL | 3.7080 mL | 7.4159 mL | |
| 10 mM | 0.3708 mL | 1.8540 mL | 3.7080 mL |