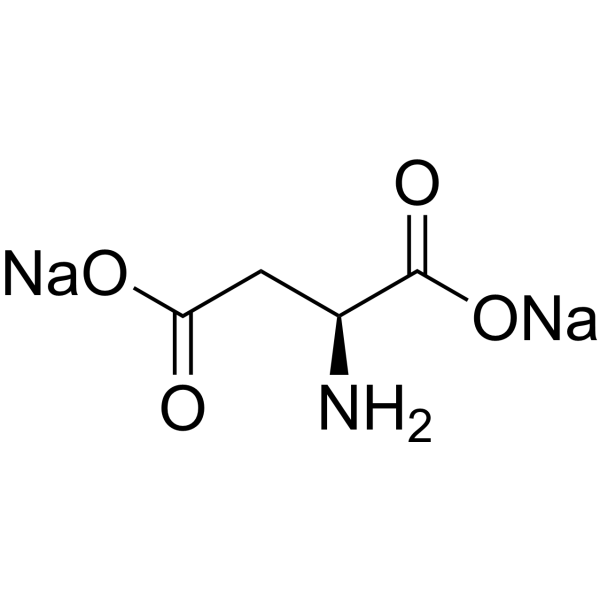
Physicochemical Properties
| Molecular Formula | C4H6NNAO4 |
| Molecular Weight | 155.0845 |
| Exact Mass | 155.006 |
| CAS # | 5598-53-8 |
| Related CAS # | L-Aspartic acid;56-84-8 |
| PubChem CID | 90470772 |
| Appearance | White to off-white solid powder |
| Density | 1.514g/cm3 |
| Boiling Point | 264.1ºC at 760mmHg |
| Melting Point | 270-271ºC |
| Flash Point | 113.5ºC |
| Hydrogen Bond Donor Count | 1 |
| Hydrogen Bond Acceptor Count | 5 |
| Rotatable Bond Count | 0 |
| Heavy Atom Count | 10 |
| Complexity | 137 |
| Defined Atom Stereocenter Count | 1 |
| SMILES | C([C@@H](C(=O)[O-])N)C(=O)[O-].[Mg+2] |
| InChi Key | NFFJLMKHRCXLJO-DKWTVANSSA-L |
| InChi Code | InChI=1S/C4H7NO4.Mg/c5-2(4(8)9)1-3(6)7;/h2H,1,5H2,(H,6,7)(H,8,9);/q;+2/p-2/t2-;/m0./s1 |
| Chemical Name | magnesium;(2S)-2-aminobutanedioate |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Toxicity/Toxicokinetics |
Effects During Pregnancy and Lactation ◉ Summary of Use during Lactation No information is available on the excretion of magnesium following magnesium aspartate during breastfeeding. However, other magnesium salts have been studied. Intravenous magnesium sulfate increases milk magnesium concentrations only slightly. Oral absorption of magnesium by the infant is poor, so maternal magnesium aspartate is not expected to affect the breastfed infant's serum magnesium. Magnesium aspartate supplementation during pregnancy might delay the onset of lactation, but it can be taken during breastfeeding and no special precautions are required. ◉ Effects in Breastfed Infants Fifty mothers who were in the first day postpartum received 15 mL of either mineral oil or an emulsion of mineral oil and another magnesium salt, magnesium hydroxide equivalent to 900 mg of magnesium hydroxide, although the exact number who received each product was not stated. Additional doses were given on subsequent days if needed. None of the breastfed infants were noted to have any markedly abnormal stools, but all of the infants also received supplemental feedings. ◉ Effects on Lactation and Breastmilk One mother who received intravenous magnesium sulfate for 3 days for pregnancy-induced hypertension had lactogenesis II delayed until day 10 postpartum. No other specific cause was found for the delay, although a complete work-up was not done. A subsequent controlled clinical trial found no evidence of delayed lactation in mothers who received intravenous magnesium sulfate therapy. Some, but not all, studies have found a trend toward increased time to the first feeding or decreased sucking in infants of mothers treated with intravenous magnesium sulfate during labor because of placental transfer of magnesium to the fetus. A study in 40 pairs of matched healthy women with vaginally delivered singleton pregnancies, outcome endpoints were compared in those receiving continuous oral magnesium aspartate HCl supplementation mean dose of 459 mg daily (range 365 to 729 mg of magnesium daily) for at least 4 weeks before delivery versus non-supplemented controls. In the magnesium group, significantly fewer women could breastfeed their infants exclusively at discharge (63% vs 80%). |
| References |
[1]. Blood-brain barrier produces significant efflux of L-aspartic acid but not D-aspartic acid: in vivo evidence using the brain efflux index method. J Neurochem. 1999 Sep;73(3):1206-11. [2]. In vivo pharmacokinetic study for the assessment of poly(L-aspartic acid) as a drug carrier for colon-specific drug delivery. J Pharmacokinet Biopharm. 1995 Aug;23(4):397-406. |
| Additional Infomation |
Magnesium aspartate is a magnesium salt of aspartic acid that is commonly used as a mineral supplement. It displays high oral bioavailability and water solubiltiy compared to other magnesium salts such as magnesium citrate, magnesium carbonate and magnesium oxide. One of the non-essential amino acids commonly occurring in the L-form. It is found in animals and plants, especially in sugar cane and sugar beets. It may be a neurotransmitter. |
Solubility Data
| Solubility (In Vitro) | H2O : ≥ 50 mg/mL (~282.37 mM) |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 6.4483 mL | 32.2414 mL | 64.4828 mL | |
| 5 mM | 1.2897 mL | 6.4483 mL | 12.8966 mL | |
| 10 mM | 0.6448 mL | 3.2241 mL | 6.4483 mL |