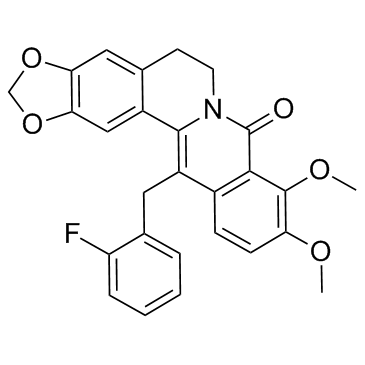
Physicochemical Properties
| Molecular Formula | C27H22FNO5 |
| Molecular Weight | 459.46569108963 |
| Exact Mass | 459.148 |
| CAS # | 1800465-47-7 |
| PubChem CID | 91820677 |
| Appearance | Light yellow to yellow solid powder |
| LogP | 4.5 |
| Hydrogen Bond Donor Count | 0 |
| Hydrogen Bond Acceptor Count | 6 |
| Rotatable Bond Count | 4 |
| Heavy Atom Count | 34 |
| Complexity | 819 |
| Defined Atom Stereocenter Count | 0 |
| InChi Key | WSIOACCDMOKVNM-UHFFFAOYSA-N |
| InChi Code | InChI=1S/C27H22FNO5/c1-31-21-8-7-17-19(11-16-5-3-4-6-20(16)28)25-18-13-23-22(33-14-34-23)12-15(18)9-10-29(25)27(30)24(17)26(21)32-2/h3-8,12-13H,9-11,14H2,1-2H3 |
| Chemical Name | 21-[(2-fluorophenyl)methyl]-16,17-dimethoxy-5,7-dioxa-13-azapentacyclo[11.8.0.02,10.04,8.015,20]henicosa-1(21),2,4(8),9,15(20),16,18-heptaen-14-one |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets | KRN5 is a possible therapeutic candidate because it is less toxic than BBR according to tests for cytotoxicity, hERG K+ channel, cytochrome inhibition, and liver microsomal metabolic stability [1]. KRN5 at 1 μM inhibited the expression of NFAT5, IL-6, MCP-1, and GM-CSF (NFAT5 target molecules) in LPS-stimulated RAW264.7 macrophages [1]. |
| ln Vitro |
KRN5 is a possible therapeutic candidate because it is less toxic than BBR according to tests for cytotoxicity, hERG K+ channel, cytochrome inhibition, and liver microsomal metabolic stability [1]. KRN5 at 1 μM inhibited the expression of NFAT5, IL-6, MCP-1, and GM-CSF (NFAT5 target molecules) in LPS-stimulated RAW264.7 macrophages [1]. KRN5 inhibited NFAT5-dependent GFP reporter activity in LPS-stimulated RAW 264.7 macrophages in a dose-dependent manner.[1] At a concentration of 1 µM, KRN5 suppressed NFAT5 protein expression in RAW 264.7 macrophages stimulated with LPS (1 µg/ml) for 24 hours.[1] At 1 µM, KRN5 also reduced the secretion of NFAT5 target cytokines, including GM-CSF, MCP-1, and IL-6, in LPS-stimulated RAW 264.7 macrophage culture supernatants.[1] |
| ln Vivo |
KRN5 (15 mg/kg and 60 mg/kg) taken orally every other day for three weeks, beginning on day 21, dose-dependently lessens the severity of arthritis [1]. Additionally, there was a significant decrease in the amount of serum anti-type II collagen IgG in the mice treated with KRN5. LPS-stimulated splenocytes in KRN5-treated CIA mice produced a considerably lower amount of TNF-α and IL-6 than did the mice treated with vehicle [1]. Oral administration of KRN5 (15 and 60 mg/kg, every other day) dose-dependently mitigated arthritis severity in a mouse model of collagen-induced arthritis (CIA). KRN5 (60 mg/kg, orally) showed more potent suppression of arthritis than methotrexate (5 mg/kg, orally, twice a week) used as a positive control. Treatment with KRN5 significantly decreased serum levels of anti-type II collagen IgG and pro-inflammatory cytokines (IL-6, TNF-α) in CIA mice.[1] |
| Cell Assay |
RAW 264.7 murine macrophage cells were seeded and cultured. For NFAT5 reporter assays, cells were stably transfected with an NFAT5-GFP reporter construct. Cells were pre-incubated with KRN5 at indicated doses for 1 hour, then stimulated with LPS (1 µg/ml) for 20-24 hours. GFP expression was measured by flow cytometry to assess NFAT5-dependent transcriptional activity.[1] For protein expression analysis, RAW 264.7 cells were treated with KRN5 and LPS as above. Cells were lysed, and proteins were separated by SDS-PAGE, transferred to nitrocellulose membranes, and probed with anti-NFAT5 antibody. Detection was performed using enhanced chemiluminescence.[1] For cytokine measurement, RAW 264.7 cells or mouse splenocytes were treated with KRN5 and LPS. Culture supernatants were collected, and levels of IL-6, TNF-α, GM-CSF, and MCP-1 were quantified using ELISA kits according to the manufacturer's instructions.[1] |
| Animal Protocol |
Animal/Disease Models: 8weeks old DBA/1J mice were immunized with bovine type II collagen [1]. Doses: 15 mg/kg and 60 mg/kg. Route of Administration: Take orally every other day (every other day) for 3 weeks. Experimental Results: Arthritis severity was diminished in a dose-dependent manner. Collagen-induced arthritis (CIA) was induced in 8-week-old DBA/1J mice by immunization with bovine type II collagen emulsified in Complete Freund's Adjuvant on day 0, followed by a booster injection on day 14. Starting on day 21, mice were orally administered KRN5 at doses of 15 mg/kg or 60 mg/kg, every other day, for 3 weeks. Methotrexate (5 mg/kg, orally, twice a week) was used as a positive control. Arthritis severity was assessed daily by visual inspection and scoring. On day 40 or 44, paws and ankles were harvested for histological evaluation. Serum was collected for antibody and cytokine analysis.[1] |
| ADME/Pharmacokinetics |
KRN5 exhibits high oral bioavailability and metabolic stability compared to its precursor KRN2. Following oral administration in rats, KRN5 showed a remarkable increase in plasma concentration and a plasma half-life estimated to be >8 hours. The oral bioavailability (F%) of KRN5 in rats was 15%.[1] |
| Toxicity/Toxicokinetics |
KRN5 is reported to be less toxic than berberine (BBR), based on cytotoxicity assays, hERG K⁺ channel assays, cytochrome P450 inhibition assays, and liver microsomal metabolic stability tests. No serious adverse effects were noted in mice treated with KRN5 throughout the arthritis experiments.[1] |
| References |
[1]. Suppression of NFAT5-mediated Inflammation and Chronic Arthritis by Novel κB-binding Inhibitors. EBioMedicine. 2017 Apr;18:261-273. |
| Additional Infomation |
KRN5 is an 8-oxo derivative of KRN2 (13-(2-fluorobenzyl)-berberine), developed to improve oral bioavailability and metabolic stability. It is a novel, orally available small-molecule inhibitor of NFAT5, identified through high-throughput screening targeting NFAT5 activity. KRN5 selectively suppresses the expression of pro-inflammatory genes regulated by NFAT5 in TLR4-stimulated macrophages without affecting high salt-induced ('osmotic') NFAT5 and its target genes. It is a potential therapeutic candidate for chronic inflammatory arthritis, such as rheumatoid arthritis.[1] |
Solubility Data
| Solubility (In Vitro) | DMSO : ~5 mg/mL (~10.88 mM) |
| Solubility (In Vivo) |
Solubility in Formulation 1: 0.5 mg/mL (1.09 mM) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (add these co-solvents sequentially from left to right, and one by one), suspension solution; with sonication. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 5.0 mg/mL clear DMSO stock solution to 400 μL PEG300 and mix evenly; then add 50 μL Tween-80 to the above solution and mix evenly; then add 450 μL normal saline to adjust the volume to 1 mL. Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH₂ O to obtain a clear solution. Solubility in Formulation 2: 0.5 mg/mL (1.09 mM) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (add these co-solvents sequentially from left to right, and one by one), suspension solution; with ultrasonication. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 5.0 mg/mL clear DMSO stock solution to 900 μL of 20% SBE-β-CD physiological saline solution and mix evenly. Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.1764 mL | 10.8821 mL | 21.7642 mL | |
| 5 mM | 0.4353 mL | 2.1764 mL | 4.3528 mL | |
| 10 mM | 0.2176 mL | 1.0882 mL | 2.1764 mL |