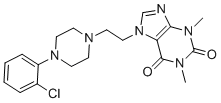
KMUP-1, a xanthine derivative, has been demonstrated to modulate K+-channel activity in smooth muscles and is a stimulator of the NO/sGC/cGMP pathway. KMUP-1 prevents STZ impairment of MA reactivity, eNOS levels and KATP channels, and accordingly protects against vascular dysfunction in diabetic rats. . KMUP-1 significantly attenuated STZ-stimulated MA contractions in response to high K+, suggesting that KMUP-1 may partly restore the vascular reactivity of MAs. In addition, STZ decreased the expression of endothelial nitric oxide synthase (eNOS) and this effect was reversed by KMUP-1, suggesting that KMUP-1could improve STZ-induced vascular endothelial dysfunction.
Physicochemical Properties
| Molecular Formula | C19H23N6O2CL | |
| Molecular Weight | 402.87792 | |
| Exact Mass | 402.157 | |
| Elemental Analysis | C, 56.64; H, 5.75; Cl, 8.80; N, 20.86; O, 7.94 | |
| CAS # | 81996-46-5 | |
| Related CAS # |
|
|
| PubChem CID | 10453764 | |
| Appearance | Typically exists as solid at room temperature | |
| LogP | 0.912 | |
| Hydrogen Bond Donor Count | 0 | |
| Hydrogen Bond Acceptor Count | 5 | |
| Rotatable Bond Count | 4 | |
| Heavy Atom Count | 28 | |
| Complexity | 599 | |
| Defined Atom Stereocenter Count | 0 | |
| SMILES | CN1C2=C(C(=O)N(C1=O)C)N(C=N2)CCN3CCN(CC3)C4=CC=CC=C4Cl |
|
| InChi Key | NIDVDYQCGWISJZ-UHFFFAOYSA-N | |
| InChi Code | InChI=1S/C19H23ClN6O2/c1-22-17-16(18(27)23(2)19(22)28)26(13-21-17)12-9-24-7-10-25(11-8-24)15-6-4-3-5-14(15)20/h3-6,13H,7-12H2,1-2H3 | |
| Chemical Name |
|
|
| Synonyms |
|
|
| HS Tariff Code | 2934.99.9001 | |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
|
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets | K+-channel |
| ln Vitro | Xanthine-based KMUP-1 was shown to inhibit phosphodiesterases (PDEs) and modulate G-protein coupled receptors (GPCRs) to lower hyperlipidemia and body weight. This study further investigated whether KMUP-1 affects adipogenesis and lipolysis in 3T3-L1 preadipocytes. KMUP-1 (1⁻40 µM) concentration-dependently attenuated Oil Red O (ORO) staining and decreased triglyceride (TG) accumulation, indicating adipogenesis inhibition in 3T3-L1 cells. In contrast, the β-agonist ractopamine increased ORO staining and TG accumulation and adipogenesis. KMUP-1 (1⁻40 µM) also reduced MAPKs/Akt/PPARγ expression, PPARγ1/PPARγ2 mRNA, and p-ERK immunoreactivity at the adipogenesis stage, but enhanced hormone sensitive lipase (HSL) immunoreactivity at the lipolysis stage. Addition of protein kinase A (PKA) or protein kinase G (PKG) antagonist (KT5720 or KT5728) to adipocytes did not affect HSL immunoreactivity. However, KMUP-1 did increase HSL immunoreactivity and the effect was reduced by PKA or PKG antagonist. Simvastatin, theophylline, caffeine, and sildenafil, like KMUP-1, also enhanced HSL immunoreactivity. Phosphorylated HSL (p-HSL) was enhanced by KMUP-1, indicating increased lipolysis in mature 3T3-L1 adipocytes. Decreases of MAPKs/Akt/PPARγ during adipogenesis contributed to inhibition of adipocyte differentiation, and increases of PKA/PKG at lipolysis contributed to HSL activation and TG hydrolysis. Taken together, the data suggest that KMUP-1 can inhibit hyperadiposity in 3T3-L1 adipocytes[1]. |
| ln Vivo | STZ (streptozotocin) decreased MA KATP currents in a time-course dependent manner and achieved steady inhibition at day 14. In the MASMCs of STZ-treated rats, KMUP-1 partially recovered the KATP currents, suggesting that vascular KATP channels were activated by KMUP-1. K+ (80 mM KCl)-induced MA contractions in STZ-treated rats were higher than those of control rats. KMUP-1 significantly attenuated STZ-stimulated MA contractions in response to high K+, suggesting that KMUP-1 may partly restore the vascular reactivity of MAs. In addition, STZ decreased the expression of endothelial nitric oxide synthase (eNOS) and this effect was reversed by KMUP-1, suggesting that KMUP-1 could improve STZ-induced vascular endothelial dysfunction. Conclusion: KMUP-1 prevents STZ impairment of MA reactivity, eNOS levels and KATP channels, and accordingly protects against vascular dysfunction in diabetic rats[2]. |
| Enzyme Assay | 7-[2-[4-(2-chlorophenyl)piperazinyl]ethyl]-1,3-dimethylxanthine (KMUP-1) produces tracheal relaxation, intracellular accumulation of cyclic nucleotides, inhibition of phosphodiesterases (PDEs) and activation of K+ channels. KMUP-1 (0.01-100 microm) induced concentration-dependent relaxation responses in guinea-pig epithelium-intact trachea precontracted with carbachol. Relaxation responses were also elicited by the PDE inhibitors theophylline, 3-isobutyl-1-methylxanthine (IBMX), milrinone, rolipram and zaprinast (100 microm), and a KATP channel opener, levcromakalim. Tracheal relaxation induced by KMUP-1 was attenuated by epithelium removal and by pretreatment with inhibitors of soluble guanylate cyclase (sGC) (1H-[1,2,4]oxadiazolo[4,3-a]quinoxalin-1-one (ODQ), 1 microm), nitric oxide synthase (Nomega-nitro-L-arginine methyl ester, 100 microm), K+ channels (tetraethylammonium, 10 mm), KATP channels (glibenclamide, 1 microm), voltage-dependent K+ channels (4-aminopyridine, 100 microm) and Ca2+-dependent K+ channels (charybdotoxin, 0.1 microm or apamin, 1 microm). Both KMUP-1 (10 microm) and theophylline nonselectively and slightly inhibited the enzyme activity of PDE3, 4 and 5, suggesting that they are able to inhibit the metabolism of adenosine 3',5'-cyclic monophosphate (cyclic AMP) and guanosine 3',5'-cyclic monophosphate (cyclic GMP). Likewise, the effects of IBMX were also measured and its IC50 values for PDE3, 4 and 5 were 6.5 +/- 1.2, 26.3 +/- 3.9 and 31.7 +/- 5.3 microm, respectively. KMUP-1 (0.01-10 microm) augmented intracellular cyclic AMP and cyclic GMP levels in guinea-pig cultured tracheal smooth muscle cells. These increases in cyclic AMP and cyclic GMP were abolished in the presence of an adenylate cyclase inhibitor SQ 22536 (100 microm) and an sGC inhibitor ODQ (10 microm), respectively. KMUP-1 (10 microm) increased the expression of protein kinase A (PKARI) and protein kinase G (PKG1alpha1beta) in a time-dependent manner, but this was only significant for PKG after 9 h. Intratracheal administration of tumour necrosis factor-alpha (TNF-alpha, 0.01 mg kg(-1)) induced bronchoconstriction and exhibited a time-dependent increase in lung resistance (RL) and decrease in dynamic lung compliance (Cdyn). KMUP-1 (1.0 mg kg(-1)), injected intravenously for 10 min before the intratracheal TNF-alpha, reversed these changes in RL and Cdyn. These data indicate that KMUP-1 activates sGC, produces relaxation that was partly dependent on an intact epithelium, inhibits PDEs and increases intracellular cyclic AMP and cyclic GMP, which then increases PKA and PKG, leading to the opening of K+ channels and resulting tracheal relaxation[3]. |
| Animal Protocol | Rats were divided into three groups: control, STZ (65 mg/kg, ip) and STZ + KMUP-1 (5 or 10 mg/kg/day, ip). MA reactivity was measured by dual wire myograph. MA smooth muscle cells (MASMCs) were enzymatically dissociated and the KATP currents recorded by a whole-cell patch-clamp technique.[2] |
| References |
[1]. Molecules.2018 Sep 23;23(10). pii: E2433; [2]. Pharmacol Rep.2018 Aug;70(4):746-752. [3]. Br J Pharmacol. 2004 Aug;142(7):1105-14. |
| Additional Infomation | Potassium Ionophores: Chemical agents that increase the permeability of CELL MEMBRANES to POTASSIUM ions. |
Solubility Data
| Solubility (In Vitro) |
|
|||
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.4821 mL | 12.4106 mL | 24.8213 mL | |
| 5 mM | 0.4964 mL | 2.4821 mL | 4.9643 mL | |
| 10 mM | 0.2482 mL | 1.2411 mL | 2.4821 mL |