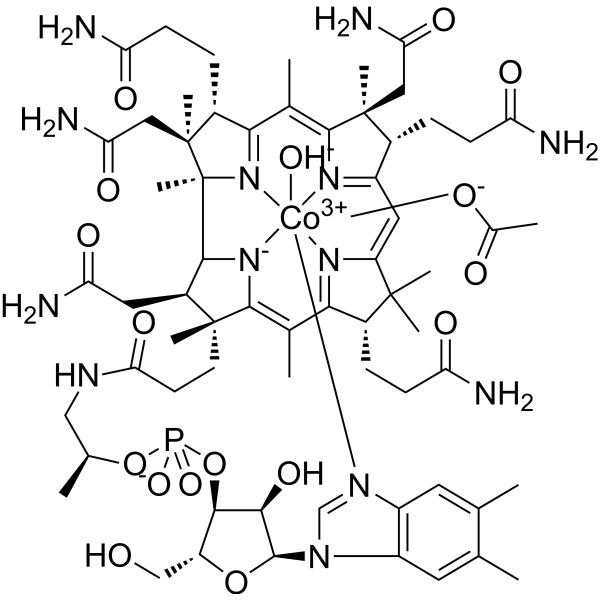
Physicochemical Properties
| Molecular Formula | C64H93CON13O16P |
| Molecular Weight | 1390.4077 |
| Exact Mass | 1387.58 |
| CAS # | 22465-48-1 |
| Related CAS # | Hydroxocobalamin;13422-51-0;Hydroxocobalamin monohydrochloride;59461-30-2;Hydroxocobalamin hydrochloride;58288-50-9 |
| PubChem CID | 168325098 |
| Appearance | Brown to black solid powder |
| Melting Point | >300ºC. |
| LogP | 6.629 |
| Hydrogen Bond Donor Count | 10 |
| Hydrogen Bond Acceptor Count | 20 |
| Rotatable Bond Count | 26 |
| Heavy Atom Count | 92 |
| Complexity | 3140 |
| Defined Atom Stereocenter Count | 14 |
| SMILES | CC1=CC2=C(C=C1C)N(C=N2)[C@@H]3[C@@H]([C@@H]([C@H](O3)CO)OP(=O)([O-])O[C@H](C)CNC(=O)CC[C@@]4([C@H]([C@@H]5[C@]6([C@@]([C@@H](C(=N6)C(=C7[C@@]([C@@H](C(=N7)C=C8C([C@@H](C(=N8)C(=C4[N-]5)C)CCC(=O)N)(C)C)CCC(=O)N)(C)CC(=O)N)C)CCC(=O)N)(C)CC(=O)N)C)CC(=O)N)C)O.O.[Co+2] |
| InChi Key | DQOCFCZRZOAIBN-WZHZPDAFSA-L |
| InChi Code | InChI=1S/C62H90N13O14P.Co.H2O/c1-29-20-39-40(21-30(29)2)75(28-70-39)57-52(84)53(41(27-76)87-57)89-90(85,86)88-31(3)26-69-49(83)18-19-59(8)37(22-46(66)80)56-62(11)61(10,25-48(68)82)36(14-17-45(65)79)51(74-62)33(5)55-60(9,24-47(67)81)34(12-15-43(63)77)38(71-55)23-42-58(6,7)35(13-16-44(64)78)50(72-42)32(4)54(59)73-56;;/h20-21,23,28,31,34-37,41,52-53,56-57,76,84H,12-19,22,24-27H2,1-11H3,(H15,63,64,65,66,67,68,69,71,72,73,74,77,78,79,80,81,82,83,85,86);;1H2/q;+2;/p-2/t31-,34-,35-,36-,37+,41-,52-,53-,56-,57+,59-,60+,61+,62+;;/m1../s1 |
| Chemical Name | cobalt(2+);[(2R,3S,4R,5S)-5-(5,6-dimethylbenzimidazol-1-yl)-4-hydroxy-2-(hydroxymethyl)oxolan-3-yl] [(2R)-1-[3-[(1R,2R,3R,7S,12S,13S,17S,18S,19R)-2,13,18-tris(2-amino-2-oxoethyl)-7,12,17-tris(3-amino-3-oxopropyl)-3,5,8,8,13,15,18,19-octamethyl-2,7,12,17-tetrahydro-1H-corrin-21-id-3-yl]propanoylamino]propan-2-yl] phosphate;hydrate |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month Note: Please store this product in a sealed and protected environment (e.g. under nitrogen), avoid exposure to moisture and light. |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
Hydroxocobalamin acetate targets nitric oxide synthase (NOS) [3] Hydroxocobalamin acetate acts as a coenzyme for methionine synthase and methylmalonyl-CoA mutase [2] |
| ln Vitro |
- Inhibition of NO production: Hydroxocobalamin acetate (100 μM-1 mM) dose-dependently inhibits lipopolysaccharide (LPS)-induced NO production in mouse peritoneal macrophages. At 500 μM, NO levels are reduced by 65% compared to LPS-stimulated control [3] - Preservation of macrophage viability: The compound (100 μM-1 mM) shows no cytotoxicity to LPS-stimulated macrophages, with cell viability > 90% after 24 hours of treatment [3] - Coenzyme activity in metabolic reactions: Hydroxocobalamin acetate (1-10 nM) restores the activity of methionine synthase in B12-deficient human fibroblasts, increasing methionine production by 70% at 10 nM [2] |
| ln Vivo |
- Treatment of vitamin B12 deficiency: Oral administration of Hydroxocobalamin acetate (1000 μg weekly) is as effective as intramuscular injection (1000 μg weekly) in correcting vitamin B12 deficiency. After 12 weeks, serum vitamin B12 levels increased from < 133 pmol/L to > 300 pmol/L in 90% of patients in both groups [2] - Prevention and reversal of endotoxin-induced hypotension: Rodents (rats/mice) administered Hydroxocobalamin acetate (30 mg/kg, intravenous injection) 30 minutes before LPS (10 mg/kg, intraperitoneal) challenge showed no significant hypotension (mean arterial pressure maintained at > 80% of baseline). In rodents with established LPS-induced hypotension, the same dose reversed blood pressure to 75% of baseline within 60 minutes [3] - Reduction of endotoxin-induced mortality: Hydroxocobalamin acetate (30 mg/kg, iv) reduced mortality in LPS-challenged rodents by 60% compared to vehicle control (mortality rate 30% vs. 75% in control) [3] - Management of vasoplegic syndrome: High-dose Hydroxocobalamin acetate (5 g, intravenous infusion) resolved refractory vasoplegia in patients after cardiac surgery, restoring mean arterial pressure to target levels (≥ 65 mmHg) without increasing catecholamine requirements [1] |
| Enzyme Assay |
- NO synthase (NOS) activity assay: Mouse peritoneal macrophages were stimulated with LPS (1 μg/mL) for 18 hours to induce NOS expression. Cells were treated with Hydroxocobalamin acetate (100 μM-1 mM) for 6 hours, and NOS activity was measured by detecting nitrite (stable NO metabolite) in cell supernatants using Griess reagent. Inhibition rate was calculated by comparing nitrite levels with LPS-stimulated control [3] - Methionine synthase activity assay: B12-deficient human fibroblasts were incubated with Hydroxocobalamin acetate (1-10 nM) in medium containing homocysteine and 5-methyltetrahydrofolate. Methionine produced by the enzyme reaction was quantified by high-performance liquid chromatography (HPLC) to assess enzyme activity restoration [2] |
| Cell Assay |
- Macrophage NO production assay: Mouse peritoneal macrophages were isolated and seeded into 96-well plates (5×10⁴ cells/well). Cells were stimulated with LPS (1 μg/mL) and co-treated with Hydroxocobalamin acetate (100 μM-1 mM) for 24 hours. Cell supernatants were collected, and nitrite levels were measured by Griess reagent to evaluate NO production [3] - Fibroblast metabolic function assay: B12-deficient human fibroblasts were seeded into 6-well plates (5×10⁵ cells/well) and treated with Hydroxocobalamin acetate (1-10 nM) for 48 hours. Cells were lysed, and methionine synthase activity was assessed by measuring methionine formation via HPLC [2] - Cell viability assay: LPS-stimulated macrophages were treated with Hydroxocobalamin acetate (100 μM-1 mM) for 24 hours. Cell viability was measured by tetrazolium salt-based assay to evaluate cytotoxicity [3] |
| Animal Protocol |
- LPS-induced hypotension and mortality model: Male Sprague-Dawley rats (250-300 g) or C57BL/6 mice (20-25 g) were randomly divided into control, LPS alone, and Hydroxocobalamin acetate groups (n=8 per group). The compound was dissolved in sterile physiological saline and administered intravenously at 30 mg/kg 30 minutes before or after LPS (10 mg/kg, intraperitoneal) injection. Mean arterial pressure was monitored continuously for 4 hours; mortality was recorded for 24 hours [3] - Vitamin B12 deficiency rodent model (for efficacy comparison): Rodents with diet-induced vitamin B12 deficiency (serum B12 < 100 pmol/L) were divided into oral and intramuscular Hydroxocobalamin acetate groups (1000 μg/kg weekly, n=6 per group). Serum vitamin B12 levels were measured by immunoassay at 4, 8, and 12 weeks [2] |
| ADME/Pharmacokinetics |
Absorption, Distribution and Excretion Readily absorbed from the gastrointestinal tract, except in malabsorption syndromes. Vitamin B12 is absorbed in the lower half of the ileum. Each hydroxocobalamin molecule can bind one cyanide ion by substituting it for the hydroxo ligand linked to the trivalent cobalt ion, to form cyanocobalamin, which is then excreted in the urine. The possibility of direct transport of hydroxocobalamin from the nasal cavity into the cerebrospinal fluid after nasal administration in rats was investigated and the results were compared with a human study. Hydroxocobalamin was given to rats (n=8) both intranasally (214 ug/rat) and intravenously (49.5 ug/rat) into the jugular vein using a Vascular Access Port (VAP). Prior to and after drug administration, blood and cerebrospinal fluid samples were taken and analysed by radioimmunoassay. The AUCcerebrospinal fluid/AUCplasma ratio after nasal delivery does not differ from the ratio after intravenous infusion, indicating that hydroxocobalamin enters the cerebrospinal fluid via the blood circulation across the blood-brain barrier (BBB). This same transport route is confirmed by the cumulative AUC-time profiles in cerebrospinal fluid and plasma, demonstrating a 30 min delay between plasma absorption and cerebrospinal fluid uptake of hydroxocobalamin in rats and in a comparative human study. The present results in rats show that there is no additional uptake of hydroxocobalamin in the cerebrospinal fluid after nasal delivery compared to intravenous administration, which is in accordance with the results found in humans. Fifty percent of the administered dose of hydroxocobalamin disappears from the injection site in 2.5 hours. Hydroxocobalamin is bound to plasma proteins and stored in the liver. It is excreted in the bile and undergoes some enterohepatic recycling. Within 72 hours after injection of 500 to 1000 mcg of hydroxocobalamin, 16 to 66 percent of the injected dose may appear in the urine. The major portion is excreted within the first 24 hours. Hydroxocobalamin is absorbed more slowly from the site of injection than is cyanocobalamin and there is some evidence that liver uptake of hydroxocobalamin may be greater than that of cyanocobalamin. It is believed that the increased retention of hydroxocobalamin compared with that of cyanocobalamin results from the greater affinity of hydroxocobalamin for both specific and nonspecific binding proteins in blood and tissues, as well as to its slower absorption from the injection site. In the presence of gastric acid and pancreatic proteases, dietary vitamin B12 is released from food and salivary binding protein and bound to gastric intrinsic factor. When the vitamin B12-intrinsic factor complex reaches the ileum, it interacts with a receptor on the mucosal cell surface and is actively transported into circulation. Adequate intrinsic factor, bile, and sodium bicarbonate (to provide a suitable pH) all are required for ileal transport of vitamin B12. Vitamin B12 deficiency in adults is rarely the result of a deficient diet per se; rather, it usually reflects a defect in one or another aspect of this complex sequence of absorption. Achlorhydria and decreased secretion of intrinsic factor by parietal cells secondary to gastric atrophy or gastric surgery is a common cause of vitamin B12 deficiency in adults. Antibodies to parietal cells or intrinsic factor complex also can play a prominent role in producing a deficiency. A number of intestinal diseases can interfere with absorption, including pancreatic disorders (loss of pancreatic protease secretion), bacterial overgrowth, intestinal parasites, sprue, and localized damage to ileal mucosal cells by disease or as a result of surgery. /Vitamin B-12/ For more Absorption, Distribution and Excretion (Complete) data for HYDROXOCOBALAMIN (9 total), please visit the HSDB record page. Metabolism / Metabolites Primarily hepatic. Cobalamins are absorbed in the ileum and stored in the liver. They continuously undergo enterohepatic recycling via secretion in the bile. Part of a dose is excreted in the urine, most of it in the first 8 hours. Toxicokinetics of hydroxocobalamin were studied in rats and in dogs after single administration. In dogs, the AUCs of free cobalamins-(III) and total cobalamins-(III) increased proportionally to the dose. Mean Cmax measured for free- and total cobalamins-(III) were 1 to 5 fold higher than those measured in humans treated with 5.0 and 10.0 g hydroxocobalamin. Terminal half-lives reached approximately 6 and 8 hours for free and total cobalamins-(III), respectively in dogs. Corresponding figures in rats amounted to 3 and 5 hours. In dogs, the clearance of total cobalamins-(III) (0.064 to 0.083 L/h/kg) was 6-7 fold lower than clearance of free cobalamins-(III). The binding of hydroxocobalamin to proteins may be regarded as reversible metabolism. Hydroxocobalamin also reacts with cyanide thereby forming cyanocobalamin. This complex is highly stable and is therefore regarded as a physiological end product of hydroxocobalamin especially during cyanide intoxication. Biological Half-Life Approximately 6 days (peak plasma concentration after 8-12 hours from oral administration) In normal individuals, hydroxocobalamin has a plasma half life of 3-20 hours. In patients with cyanide poisoning, the half life is 14-24 hours. - Absorption: Oral Hydroxocobalamin acetate is absorbed via intrinsic factor-mediated transport in the ileum, with absolute oral bioavailability of 1-3% in healthy individuals; intramuscular injection shows 100% bioavailability [2] - Distribution: The compound binds to transcobalamin II in plasma, distributing widely to tissues (highest concentrations in liver, kidneys, and bone marrow). Volume of distribution (Vd) is 0.3-0.5 L/kg in humans [2] - Metabolism: Hydroxocobalamin acetate is converted to active coenzyme forms (methylcobalamin, adenosylcobalamin) in the liver and other tissues; no significant metabolism to inactive products [2] - Excretion: Elimination is slow, with a terminal half-life (t1/2) of 6-12 days in humans. Approximately 70% of the dose is excreted in bile, 10-20% in urine (mainly as active metabolites) [2] - Pharmacokinetics in patients: In patients with vitamin B12 deficiency, weekly intramuscular or oral administration of 1000 μg maintains serum B12 levels above 300 pmol/L for 7 days [2] |
| Toxicity/Toxicokinetics |
Protein Binding Very high (90%). Cobalamins are extensively bound to two specific plasma proteins called transcobalamin 1 and 2; 70% to transcobalamin 1, 5% to transcobalamin 2. Interactions Concurrent administration of chloramphenicol and vitamin B12 reportedly may antagonize the hematopoietic response to vitamin B12 in vitamin B12-deficient patients. The hematologic response to vitamin B12 in patients receiving both drugs should be carefully monitored and alternate anti-infectives should be considered. /Vitamin B12/ Prednisone has been reported to increase the absorption of vitamin B12 and secretion of intrinsic factor (IF) in a few patients with pernicious anemia, but not in patients with partial or total gastrectomy. The clinical importance of these findings is unknown. /Vitamin B12/ Ascorbic acid may destroy substantial amounts of dietary vitamin B12 in vitro; this possibility should be considered when large doses of ascorbic acid are ingested within 1 hour of oral vitamin B12 administration. /Vitamin B12/ Absorption of vitamin B12 from the GI tract may be decreased by aminoglycoside antibiotics, colchicine, extended-release potassium preparations, aminosalicylic acid and its salts, anticonvulsants (e.g., phenytoin, phenobarbital, primidone), cobalt irradiation of the small bowel, and by excessive alcohol intake lasting longer than 2 weeks. Neomycin-induced malabsorption of vitamin B12 may be increased by concurrent administration of colchicine. /Vitamin B12 Caution should be exercised when administering other cyanide antidotes simultaneously with Cyanokit, as the safety of coadministration has not been established. If a decision is made to administer another cyanide antidote with Cyanokit, these drugs should not be administered concurrently in the same IV line. Non-Human Toxicity Values LD50 Mouse iv 2 g/kg - Acute toxicity: No mortality or severe toxicity is observed in rodents after single intravenous doses of Hydroxocobalamin acetate up to 200 mg/kg [3] - Subacute/chronic toxicity: Long-term administration (12 weeks) of 1000 μg weekly (oral/intramuscular) in humans shows no significant changes in liver function (ALT, AST), kidney function (creatinine, urea nitrogen), or blood routine parameters [2] - Adverse effects: High-dose intravenous Hydroxocobalamin acetate (5 g) may cause transient skin discoloration (red-pink), urine discoloration, and false blood leak alarms in hemodialysis patients (due to absorption of light by the compound) [1] - Drug interactions: No significant interactions with folic acid, iron supplements, or common medications (anticoagulants, antihypertensives) are reported [2] |
| References |
[1]. High-dose hydroxocobalamin for vasoplegic syndrome causing false blood leak alarm. Clin Kidney J. 2017 Jun;10(3):357-362. [2]. Oral vitamin B12 versus intramuscular vitamin B12 for vitamin B12 deficiency. Cochrane Database Syst Rev. 2018 Mar 15;3:CD004655. [3]. Hydroxocobalamin (vitamin B12a) prevents and reverses endotoxin-induced hypotension and mortality in rodents: role of nitric oxide. J Pharmacol Exp Ther. 1995 Apr;273(1):257-65. |
| Additional Infomation |
Hydroxocobalamin, also known as vitamin B12a and hydroxycobalamin, is an injectable form of vitamin B 12 that has been used therapeutically to treat vitamin B 12 deficiency. It is also used in cyanide poisoning, Leber's optic atrophy, and toxic amblyopia. Hydroxocobalamin is a synthetic form of vitamin B12 that can be used as a dietary supplement to treat vitamin B12 deficiency. Upon administration, hydroxocobalamin mimics vitamin B12 and acts as an essential cofactor in various cellular reactions required for cell growth and replication, and hematopoiesis. Injectable form of VITAMIN B 12 that has been used therapeutically to treat VITAMIN B 12 DEFICIENCY. Drug Indication For treatment of pernicious anemia and the prevention and treatment of vitamin B12 deficiency arising from alcoholism, malabsorption, tapeworm infestation, celiac, hyperthyroidism, hepatic-biliary tract disease, persistent diarrhea, ileal resection, pancreatic cancer, renal disease, prolonged stress, vegan diets, macrobiotic diets or other restrictive diets. Also for the treatment of known or suspected cyanide poisoning. Treatment of known or suspected cyanide poisoning. Cyanokit is to be administered together with appropriate decontamination and supportive measures. Mechanism of Action Vitamin B12 exists in four major forms referred to collectively as cobalamins; deoxyadenosylcobalamin, methylcobalamin, hydroxocobalamin, and cyanocobalamin. Two of these, methylcobalamin and 5-deoxyadenosyl cobalamin, are primarily used by the body. Methionine synthase needs methylcobalamin as a cofactor. This enzyme is involved in the conversion of the amino acid homocysteine into methionine. Methionine in turn is required for DNA methylation. 5-Deoxyadenosyl cobalamin is a cofactor needed by the enzyme that converts L-methylmalonyl-CoA to succinyl-CoA. This conversion is an important step in the extraction of energy from proteins and fats. Furthermore, succinyl CoA is necessary for the production of hemoglobin, the substances that carries oxygen in red blood cells. Hydroxocobalamin is a complexation agent that acts by direct binding of the cyanide ions, resulting in cyanocobalamin which is a highly stable, nontoxic compound that is excreted in the urine. In addition, increased blood pressure observed in some healthy subjects of the phase I clinical study and results of a non-clinical study performed in anesthetized rabbits suggest an interference of hydroxocobalamin with the NO system. VITAMIN B12 IS IMPLICATED IN PROTEIN SYNTH THROUGH ITS ROLE IN SYNTH OF AMINE ACID METHIONINE... /COBALAMINS/ COENZYME B12 IS REQUIRED FOR HYDROGEN TRANSFER & ISOMERIZATION WHEReBY METHYLMALONATE IS CONVERTED TO SUCCINATE, THUS INVOLVING COBALAMIN IN BOTH FAT & CARBOHYDRATE METABOLISM. ... METHYLCOBALAMIN IS REQUIRED FOR CONVERSION OF HOMOCYSTEINE TO METHIONINE IN MAMMALS. /COBALAMINS/ Therapeutic Uses Hematinics Cyanokit is indicated for the treatment of known or suspected cyanide poisoning. Pernicious anemia, both uncomplicated and accompanied by nervous system involvement. The US government considers cyanide to be among the most likely agents of chemical terrorism. Cyanide differs from many other biological or chemical agents for which little or no defense is available because its individual and public health effects are largely remediable through appropriate preparedness and response. Because the toxicity of the cyanide antidote currently available in the United States renders it ill-suited for use in terrorist incidents and other situations requiring rapid out-of-hospital treatment, hydroxocobalamin--an effective and safe cyanide antidote being used in other countries--has been introduced in the United States. Unlike the other available cyanide antidote, hydroxocobalamin can be administered at the scene of a cyanide disaster, and it need not be reserved for cases of confirmed cyanide poisoning but can be administered in cases of suspected poisoning. Both of these attributes facilitate the rapid intervention necessary for saving lives. To realize the potential benefits of hydroxocobalamin, progress also needs to be realized in other aspects of readiness, including but not limited to developing plans for ensuring local and regional availability of antidote, educating emergency responders and health care professionals in the recognition and management of cyanide poisoning, and raising public awareness of the potential for a chemical weapons attack and of how to respond. For more Therapeutic Uses (Complete) data for HYDROXOCOBALAMIN (10 total), please visit the HSDB record page. Drug Warnings Caution should be exercised when administering other cyanide antidotes simultaneously with Cyanokit, as the safety of coadministration has not been established. If a decision is made to administer another cyanide antidote with Cyanokit, these drugs should not be administered concurrently in the same IV line. Use caution in the management of patients with known anaphylactic reactions to hydroxocobalamin or cyanocobalamin. Consideration should be given to use of alternative therapies, if available. Allergic reactions may include: anaphylaxis, chest tightness, edema, urticaria, pruritus, dyspnea, and rash. Allergic reactions including angioneurotic edema have also been reported in postmarketing experience. Maternal Medication usually Compatible with Breast-Feeding: B12: Reported Sign or Symptom in Infant or Effect on Lactation: None. /from Table 6/ While determination of blood cyanide concentration is not required for management of cyanide poisoning and should not delay treatment with Cyanokit, collecting a pretreatment blood sample may be useful for documenting cyanide poisoning as sampling post- Cyanokit use may be inaccurate. For more Drug Warnings (Complete) data for HYDROXOCOBALAMIN (19 total), please visit the HSDB record page. Pharmacodynamics Hydroxocobalamin is a synthetic, injectable form of Vitamin B12. Hydroxocobalamin is actually a precursor of two cofactors or vitamins (Vitamin B12 and Methylcobalamin) which are involved in various biological systems in man. Vitamin B12 is required for the conversion of methylmalonate to succinate. Deficiency of this enzyme could therefore interfere with the production of lipoprotein in myelin sheath tissue and so give rise to neurological lesions. The second cofactor, Methylcobalamin, is necessary for the conversion of homocysteine to methionine which is essential for the metabolism of folic acid. Deficiency of tetrahydrafolate leads to reduced synthesis of thymidylate resulting in reduced synthesis of DNA which is essential for cell maturation. Vitamin B12 is also concerned in the maintenance of sulphydryl groups in reduced form, deficiency leading to decreased amounts of reduced SH content of erythrocytes and liver cells. Overall, vitamin B12 acts as a coenzyme for various metabolic functions, including fat and carbohydrate metabolism and protein synthesis. It is necessary for growth, cell replication, hematopoiesis, and nucleoprotein as well as myelin synthesis. This is largely due to its effects on metabolism of methionine folic acid, and malonic acid. - Chemical classification: Hydroxocobalamin acetate is a water-soluble vitamin (vitamin B12 analog) and a cobalt-containing corrinoid compound [2] - Mechanism of action: As a vitamin B12 active form, it acts as a coenzyme for methionine synthase (facilitating homocysteine conversion to methionine) and methylmalonyl-CoA mutase (participating in fatty acid metabolism), correcting vitamin B12 deficiency. It also scavenges excessive nitric oxide (NO) and inhibits NOS activity, reversing vasodilation and hypotension induced by endotoxin or vasoplegic syndrome [1][2][3] - Therapeutic indications: Approved for the treatment of vitamin B12 deficiency (including pernicious anemia). Used off-label for refractory vasoplegic syndrome (post-cardiac surgery) and prevention/treatment of endotoxin-induced hypotension [1][2][3] - Administration routes: Available as oral tablets, intramuscular injection, and intravenous infusion. High-dose intravenous formulations (5 g) are used for vasoplegic syndrome; oral and intramuscular formulations for vitamin B12 deficiency [1][2] |
Solubility Data
| Solubility (In Vitro) | DMSO : ~100 mg/mL (~71.15 mM) |
| Solubility (In Vivo) |
Solubility in Formulation 1: 2.5 mg/mL (1.78 mM) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (add these co-solvents sequentially from left to right, and one by one), suspension solution; with sonication. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 400 μL PEG300 and mix evenly; then add 50 μL Tween-80 to the above solution and mix evenly; then add 450 μL normal saline to adjust the volume to 1 mL. Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH₂ O to obtain a clear solution. Solubility in Formulation 2: ≥ 2.5 mg/mL (1.78 mM) (saturation unknown) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 900 μL of 20% SBE-β-CD physiological saline solution and mix evenly. Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 0.7192 mL | 3.5961 mL | 7.1921 mL | |
| 5 mM | 0.1438 mL | 0.7192 mL | 1.4384 mL | |
| 10 mM | 0.0719 mL | 0.3596 mL | 0.7192 mL |