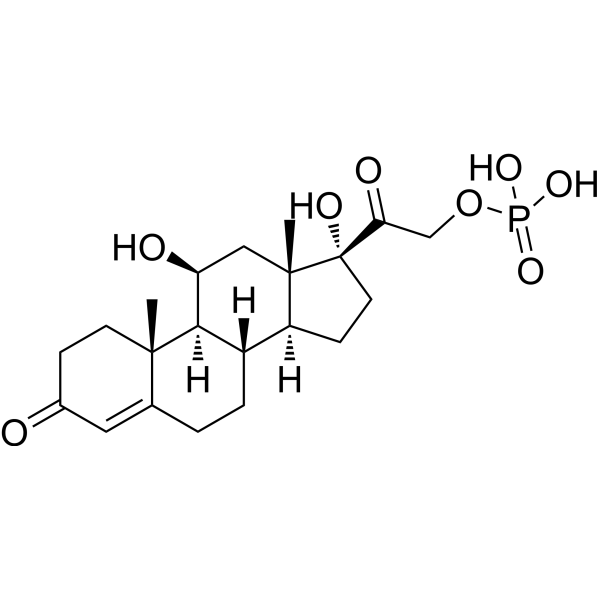
Physicochemical Properties
| Molecular Formula | C21H31O8P |
| Molecular Weight | 442.43984 |
| Exact Mass | 442.176 |
| CAS # | 3863-59-0 |
| Related CAS # | Hydrocortisone 17-butyrate;13609-67-1;Hydrocortisone acetate;50-03-3;Hydrocortisone 17-valerate;57524-89-7;Hydrocortisone hemisuccinate;2203-97-6;Hydrocortisone;50-23-7; 6000-74-4 |
| PubChem CID | 441407 |
| Appearance | Typically exists as solid at room temperature |
| Density | 1.42g/cm3 |
| Boiling Point | 669.9ºC at 760mmHg |
| Flash Point | 358.9ºC |
| Index of Refraction | 1.596 |
| LogP | 1.898 |
| Hydrogen Bond Donor Count | 4 |
| Hydrogen Bond Acceptor Count | 8 |
| Rotatable Bond Count | 4 |
| Heavy Atom Count | 30 |
| Complexity | 848 |
| Defined Atom Stereocenter Count | 7 |
| SMILES | C[C@@]12[C@](C(COP(O)(O)=O)=O)(O)CC[C@@]1([H])[C@]3([H])CCC4=CC(CC[C@]4(C)[C@@]3([H])[C@@H](O)C2)=O |
| InChi Key | BGSOJVFOEQLVMH-VWUMJDOOSA-N |
| InChi Code | InChI=1S/C21H31O8P/c1-19-7-5-13(22)9-12(19)3-4-14-15-6-8-21(25,17(24)11-29-30(26,27)28)20(15,2)10-16(23)18(14)19/h9,14-16,18,23,25H,3-8,10-11H2,1-2H3,(H2,26,27,28)/t14-,15-,16-,18+,19-,20-,21-/m0/s1 |
| Chemical Name | [2-[(8S,9S,10R,11S,13S,14S,17R)-11,17-dihydroxy-10,13-dimethyl-3-oxo-2,6,7,8,9,11,12,14,15,16-decahydro-1H-cyclopenta[a]phenanthren-17-yl]-2-oxoethyl] dihydrogen phosphate |
| Synonyms | Hydrocortisone phosphate; 3863-59-0; Cortisol 21-phosphate; Hydrocortisone 21-phosphate; 2Y87E22X71; DTXSID7048160; NSC-529660; PREGN-4-ENE-3,20-DIONE, 11,17-DIHYDROXY-21-(PHOSPHONOOXY)-; |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets | Glucocorticoid receptor (GR) |
| ln Vitro | Hydrocortisone phosphate has no lethal effect on MH60 cells that are IL-6-independent, but it inhibits the biological activities of IL-6 and IL-3 with IC50s of 6.7 and 21.4 μM, respectively [3]. PHA responses in peripheral lymphocyte (PBL) and T lymphocyte cultures are inhibited by hydrocortisone phosphate (0.12-60 μM; 72 hours) [3]. |
| ln Vivo | In mice, oral hydrocortisone phosphate (30 mg/kg) given twice a day for five days decreases weight loss and enhances food intake [2]. |
| Animal Protocol |
Animal/Disease Models: Male SD (SD (Sprague-Dawley)) rats (200-220 g, 10-11 weeks) induced colitis [2] Doses: 30 mg/kg Route of Administration: Po twice (two times) daily for 5 days Experimental Results: Significant reduction in disease Activity index (DAI) scores and myeloperoxidase (MPO) activity compared with the 2,4,6-trinitrobenzene sulfonic acid (TNBS) group. Weight gain. |
| ADME/Pharmacokinetics |
Absorption, Distribution and Excretion Topical corticosteroids can be absorbed from normal intact skin. Inflammation and/or other disease processes in the skin increase percutaneous absorption. Corticosteroids are metabolized primarily in the liver and are then excreted by the kidneys. Some of the topical corticosteroids and their metabolites are also excreted into the bile. Metabolism / Metabolites Primarily hepatic via CYP3A4 Biological Half-Life 6-8 hours |
| Toxicity/Toxicokinetics |
Protein Binding 95% |
| References |
[1]. Inhibitory effects of anti-inflammatory drugs on interleukin-6 bioactivity. Biol Pharm Bull. 2001 Jun;24(6):701-3. [2]. In vitro and in vivo application of pH-sensitive colon-targeting polysaccharide hydrogel used for ulcerative colitis therapy. Carbohydr Polym. 2015 Oct 5;130:243-53. [3]. The immunosuppressive potency in vitro of physiological and synthetic steroids on lymphocyte cultures. Int J Immunopharmacol. 1987;9(4):469-73. |
| Additional Infomation |
Cortisol phosphate is a steroid phosphate that is the 21-O-phospho derivative of cortisol. It is a cortisol ester, a steroid phosphate, an 11beta-hydroxy steroid, a 3-oxo-Delta(4) steroid, a 17alpha-hydroxy steroid and a tertiary alpha-hydroxy ketone. It is a conjugate acid of a cortisol phosphate(2-). Drug Indication For the relief of the inflammatory and pruritic manifestations of corticosteroid-responsive dermatoses. Also used to treat endocrine (hormonal) disorders (adrenal insufficiency, Addisons disease). It is also used to treat many immune and allergic disorders, such as arthritis, lupus, severe psoriasis, severe asthma, ulcerative colitis, and Crohn's disease. Mechanism of Action Hydrocortisone binds to the cytosolic glucocorticoid receptor. After binding the receptor the newly formed receptor-ligand complex translocates itself into the cell nucleus, where it binds to many glucocorticoid response elements (GRE) in the promoter region of the target genes. The DNA bound receptor then interacts with basic transcription factors, causing the increase in expression of specific target genes. The anti-inflammatory actions of corticosteroids are thought to involve lipocortins, phospholipase A2 inhibitory proteins which, through inhibition arachidonic acid, control the biosynthesis of prostaglandins and leukotrienes. Specifically glucocorticoids induce lipocortin-1 (annexin-1) synthesis, which then binds to cell membranes preventing the phospholipase A2 from coming into contact with its substrate arachidonic acid. This leads to diminished eicosanoid production. The cyclooxygenase (both COX-1 and COX-2) expression is also suppressed, potentiating the effect. In other words, the two main products in inflammation Prostaglandins and Leukotrienes are inhibited by the action of Glucocorticoids. Glucocorticoids also stimulate the lipocortin-1 escaping to the extracellular space, where it binds to the leukocyte membrane receptors and inhibits various inflammatory events: epithelial adhesion, emigration, chemotaxis, phagocytosis, respiratory burst and the release of various inflammatory mediators (lysosomal enzymes, cytokines, tissue plasminogen activator, chemokines etc.) from neutrophils, macrophages and mastocytes. Additionally the immune system is suppressed by corticosteroids due to a decrease in the function of the lymphatic system, a reduction in immunoglobulin and complement concentrations, the precipitation of lymphocytopenia, and interference with antigen-antibody binding. |
Solubility Data
| Solubility (In Vitro) | May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.2602 mL | 11.3010 mL | 22.6019 mL | |
| 5 mM | 0.4520 mL | 2.2602 mL | 4.5204 mL | |
| 10 mM | 0.2260 mL | 1.1301 mL | 2.2602 mL |