Physicochemical Properties
| Molecular Formula | C28H34O8S2 |
| Molecular Weight | 562.69476 |
| Exact Mass | 562.169 |
| CAS # | 92761-26-7 |
| Related CAS # | 92761-26-7 (free);92841-53-7 (ditriethanolamine) |
| PubChem CID | 146382 |
| Appearance | Solid |
| Density | 1.4±0.1 g/cm3 |
| Melting Point | 255° (dec) |
| Index of Refraction | 1.631 |
| LogP | 1.35 |
| Hydrogen Bond Donor Count | 2 |
| Hydrogen Bond Acceptor Count | 8 |
| Rotatable Bond Count | 6 |
| Heavy Atom Count | 38 |
| Complexity | 1230 |
| Defined Atom Stereocenter Count | 0 |
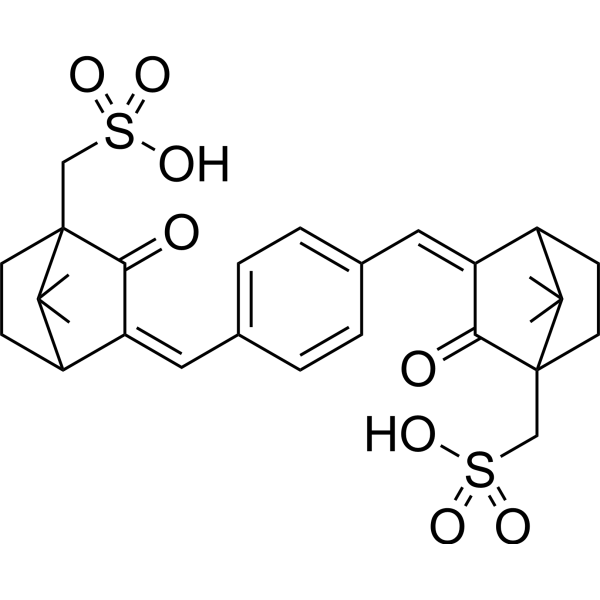
| SMILES | O=C1C2(C(C(CC2)C1=CC1C=CC(C=C2C3C(C(CS(O)(=O)=O)(CC3)C2=O)(C)C)=CC=1)(C)C)CS(O)(=O)=O |
| InChi Key | HEAHZSUCFKFERC-UHFFFAOYSA-N |
| InChi Code | InChI=1S/C28H34O8S2/c1-25(2)21-9-11-27(25,15-37(31,32)33)23(29)19(21)13-17-5-7-18(8-6-17)14-20-22-10-12-28(24(20)30,26(22,3)4)16-38(34,35)36/h5-8,13-14,21-22H,9-12,15-16H2,1-4H3,(H,31,32,33)(H,34,35,36) |
| Chemical Name | [3-[[4-[[7,7-dimethyl-3-oxo-4-(sulfomethyl)-2-bicyclo[2.2.1]heptanylidene]methyl]phenyl]methylidene]-7,7-dimethyl-2-oxo-1-bicyclo[2.2.1]heptanyl]methanesulfonic acid |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| ln Vitro | The maximal absorbance of escamsule, a broad-spectrum UVA absorber, is 344 nm[1]. The sensitivity of wild-type Fibs E6/E7 cells to Ecamsule treatment (200–1600 μM) is higher [1]. ..The production of ROS brought on by UV and AAPH can be inhibited by escamsule [1]. ..With a maximum ROS reduction of 25.7% at the highest measured concentration of 1600 μM in the UV setting, the impact was dose-dependent. The oxidative stress caused by AAPH was decreased by 10.8% and the basal level was decreased by 16.9% at the same Ecamsule concentration[1]. ..At the maximum dose of 1600 μM, Ecamsule can boost viability in cells treated with AAPH [1]. |
| ADME/Pharmacokinetics |
Absorption, Distribution and Excretion Ecamsule is a topical preparation, it should not be absorbed. Research done by L'Oreal on human subjects revealed that the systemically absorbed dose of [(14)C]-Ecamsule is less than 0.1% and under realistic exposure conditions, the human systemic exposure to this UVA filter is negligible and poses no risk to human health. Ecamsule is intended for topical application only. Ecamsule is intended for topical application and has no volume of distribution. Ecamsule is used topically, it not absorbed or metabolized. The potential human health risk of UV filters depends on their toxicity and the human systemic exposure which is a function of the extent of percutaneous absorption of the topically applied substance into the human organism. Using a 'mass balance' approach, a study was designed to investigate the systemically absorbed dose of [(14)C]-Mexoryl SX((R)) in humans after topical application of a typical sunscreen emulsion. In addition, to assess the correlation with in vitro experiments, the percutaneous absorption of this UVA filter through isolated human skin was measured under identical exposure conditions. When applied in vivo for a period of 4 hr, 89-94% of the applied radioactivity was recovered from the wash-off samples. In urine samples, the radioactivity slightly exceeded background levels and corresponded maximally to 0.014% of the topically applied dose. No radioactivity was measured in blood or feces sampled up to 120 hr after application. In vitro, 24 hr after a 4-hour application, [(14)C]-Mexoryl SX remained primarily on the skin surface. The mean in vitro absorption over 24 hr, adding up the amounts found in the dermis and receptor fluid, was 0.16% of the applied dose. It is concluded from the in vivo pharmacokinetic results that the systemically absorbed dose of [(14)C]-Mexoryl SX is less than 0.1%. The order of magnitude of this value correlates well with the corresponding in vitro data which overestimate the in vivo results as previously observed with other hydrophilic compounds. This study demonstrates that, under realistic exposure conditions, the human systemic exposure to this UVA filter is negligible and poses no risk to human health. An in vivo method in humans using radioactive terephthalylidene dicamphor sulfonic acid ((14)C site not specified) showed an absorption determined up to 24 hours after a 4-hours exposure to 0.16% of the applied dose. Metabolism / Metabolites Ecamsule is not absorbed or metabolized. Biological Half-Life Ecamsule is not absorbed and has no reported half life data. |
| Toxicity/Toxicokinetics |
Toxicity Summary IDENTIFICATION AND USE: Terephthalylidene dicamphor sulfonic acid is a solid. It is used as broad spectrum UVA absorber with some UVB absorption. It has been tested as an ultraviolet screen in animals. HUMAN STUDIES: There are no data available. ANIMAL STUDIES: In a 90-day oral repeat dose study in rats, no dose related effects were found at 300 mg/kg/day. At 1,000 mg/kg/day there was phosphoremia in males at week 4 and decreased protein, albumin and globulin levels in females at week 13. There was some evidence of variation in thyroid weight in the male animals fed terephthalylidene dicamphor sulfonic acid, however, there was some doubt as to validity of this observation as the control animals were found to have unusually low thyroid weights. Follow up 21-day studies using the triethalanoamine and sodium salts on thyroid metabolism found no treatment related changes at dose rates of 305 mg/kg and 444 mg/kg respectively. Protein Binding Ecamsule is intended for topical application only. Non-Human Toxicity Values LD50 Rat oral >1,835 mg/kg LD50 Rat dermal >1,637 mg/kg |
| References |
[1]. Contradictory effects of chemical filters in UV/ROS-stressed human keratinocyte and fibroblast cells. ALTEX. 2019;36(2):231-244. [2]. A new ecamsule-containing SPF 40 sunscreen cream for the prevention of polymorphous light eruption: a double-blind, randomized, controlled study in maximized outdoor conditions. Cutis. 2009 Feb;83(2):95-103. |
| Additional Infomation |
Ecamsule is a monoterpenoid. Ecamsule is an organic compound which is added to many sunscreens to filter out UVA rays. It is a benzylidene camphor derivative, many of which are known for their excellent photostability. Ecamsule has been approved for use in the U.S. since 2006, but only at a specific concentration and only in a few products manufactured by L'Oreal. The company got approval for those products through a new drug application process. Drug Indication Applied topically to filter out UVA rays. Mechanism of Action Ecamsule protects against UV wavelengths in the 290–400 nanometer range, with peak protection at 345 nm. Ecamsule is photostable and it does not degrade significantly when exposed to light. In studies done in mice it reduces the formation of UV induced pyrimidine dimers and delays the onset of skin cancer. In vitro, ecamsule has been shown to effectively protect against the harmful effects of UV. Therapeutic Uses Ultraviolet screen /EXPL THER/ The aim of this study was to determine, for regulatory purposes, the potential of Mexoryl SX, a broad UVA absorber that also absorbs to some extent in the UVB, to modify the UV radiation (UVR)-induced murine skin tumor development and growth. Skh-hr1 mice were exposed to solar-simulated UVR 5 days per week for 40 weeks. Two control groups were irradiated without topical application, three groups received a sunscreen preparation containing either the UVA absorber, Mexoryl SX at 5 or 10% concentration, or a filter that absorbs principally in the UVB, 2-ethylhexyl-p-methoxycinnamate (2-EHMC) at 5% concentration, introduced as a comparator test article. Sunscreen application was performed before UVR exposure 3 days per week and after UVR exposure on the other 2 days (consistent with the design of a standard photocarcinogenesis safety test). Two different weekly UVR doses were administrated: the lower dose was given to one group of unprotected animals, whereas the higher dose was administrated to the other unprotected group and to the three sunscreen-treated groups. The two UVR control groups demonstrated a UVR-dependent response for cumulative tumor prevalence, tumor yield and median latent period. Neither concentration of Mexoryl SX increased the probability of tumor development; consistent with the principles for safety testing, this provides evidence in that it is safe for use in sunlight. Although this study was explicitly designed as a safety test, the results also provide some clues about the efficacy of Mexoryl SX in decreasing the probability of tumor development. Topical administration of Mexoryl SX, at both concentrations, resulted in a 6 week delay in the median latent period compared to high UVR controls, whereas 5% 2-EHMC delayed the median latent periods only by 2 weeks. Tumor prevalence and yield show the same efficacy differences between the two sunscreen ingredients. Tumor protection factors were calculated from these results and found to be equal to 2.4 for the two preparations containing Mexoryl SX and to 1.3 for the 5% 2-EHMC preparation. These findings illustrate the efficacy of Mexoryl SX in preventing UVR-induced carcinogenesis. /EXPL THER/ In a previous study on the hairless mouse it was shown that sub-erythemal doses of pure UV-A enhanced the numerous changes normally observed during chronological aging. A new sunscreen (a bis-benzylidene campho sulfonic acid derivative) has been synthesized in our research laboratory (lambda max: 345 nm, epsilon: 47,000). Its photoprotective properties against UV-A induced damages were assessed in our mouse model. Three-month-old albino hairless mice were exposed for 1 y to suberythemal doses (35 J/sq cm) of UV-A obtained from a xenon source filtered through a WG 345 filter. One group of animals was exposed untreated, the other received a formulation containing 5% of the sunscreen prior to irradiation. At the end of the study the cutaneous properties of protected mice were compared to those of unprotected animals and to 3 and 15-month-old unirradiated controls. We found that the visible changes induced by UV-A irradiation were mainly sagging and wrinkling. Histological and electron microscopic alterations consisted of hyperkeratosis, increased density of elastic fibers with alteration of fiber orientation and increased glycosaminoglycan deposits. Biochemical changes consisted of decreases in total collagen and collagen hydroxylation and increases in both collagen III/I + III ratio and fibronectin biosynthesis. All these changes were reduced or abolished by the sunscreen. /EXPL THER/ BACKGROUND/PURPOSE: Exposure to ultraviolet (UV) radiation increases skin pigmentation and usually results in an even darkening of the skin. However, it may also occasionally lead to the development of hyperpigmented lesions due to a local overproduction of pigment. Skin pigmentation is induced both by UVB and UVA rays. METHODS: The in vivo protection by sunscreens against pigmentation was studied using the determination of a level of protection against pigmentation based on the standardized sun protection factor (SPF) test method. The method includes delayed UVB and UVA pigmentations. The level of prevention against pigmentation was determined 7 days after exposure to solar-simulated radiation by visual assessment. It was calculated using the ratio of the minimal pigmenting dose on protected skin to the minimal pigmenting dose on unprotected skin. Broadspectrum UVB/UVA filters, Mexoryl SX and Mexoryl XL, and complete formula were tested. RESULTS: Protection against pigmentation correlates with the concentration of Mexoryl SX. The levels of protection obtained show a synergetic effect of Mexoryl SX when associated with Mexoryl XL. When different products having the same SPF (same protection against erythema) and different levels of UVA protection are compared, only sunscreen products with a high level of UVA protection show a similar level of protection against sunburn and pigmentation. Products with low UVA protection have a lower capacity of preventing induced pigmentation compared with their efficacy against erythema. CONCLUSIONS: These studies have evidenced that SPF determination was not sufficient to account for the efficiency in preventing pigmentation and that UVA protection was an essential part of this prevention. For more Therapeutic Uses (Complete) data for Terephthalylidene dicamphor sulfonic acid (6 total), please visit the HSDB record page. Pharmacodynamics When exposed to UV ecamsule undergoes reversible photoisomerization followed by photoexcitation. The absorbed UV is then released as thermal energy, without penetrating the skin, thereby protecting the skin from UV exposure. |
Solubility Data
| Solubility (In Vitro) | May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 1.7772 mL | 8.8859 mL | 17.7718 mL | |
| 5 mM | 0.3554 mL | 1.7772 mL | 3.5544 mL | |
| 10 mM | 0.1777 mL | 0.8886 mL | 1.7772 mL |