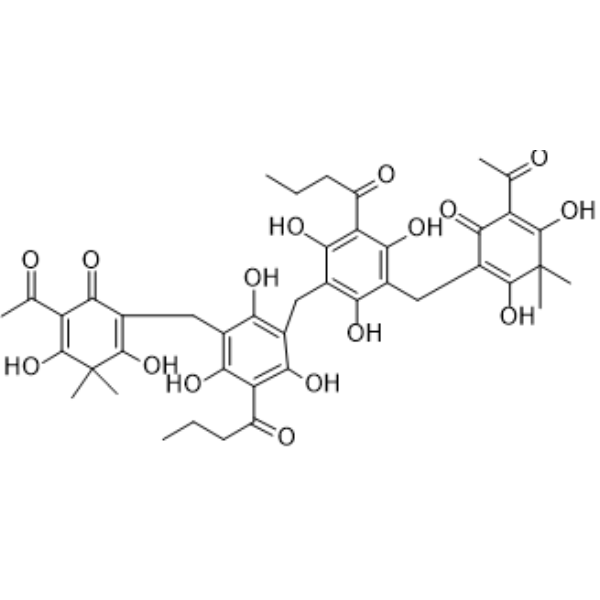
Physicochemical Properties
| Molecular Formula | C43H48O16 |
| Molecular Weight | 820.8316 |
| Exact Mass | 820.294 |
| CAS # | 12777-70-7 |
| PubChem CID | 3082025 |
| Appearance | Light yellow to green yellow solid powder |
| Density | 1.5±0.1 g/cm3 |
| Boiling Point | 1089.0±65.0 °C at 760 mmHg |
| Flash Point | 626.1±30.8 °C |
| Vapour Pressure | 0.0±0.3 mmHg at 25°C |
| Index of Refraction | 1.673 |
| LogP | 8.08 |
| Hydrogen Bond Donor Count | 10 |
| Hydrogen Bond Acceptor Count | 16 |
| Rotatable Bond Count | 14 |
| Heavy Atom Count | 59 |
| Complexity | 1760 |
| Defined Atom Stereocenter Count | 0 |
| InChi Key | PRVKSKWNDSLRBY-UHFFFAOYSA-N |
| InChi Code | InChI=1S/C43H48O16/c1-9-11-24(46)28-32(50)18(30(48)20(34(28)52)14-22-36(54)26(16(3)44)40(58)42(5,6)38(22)56)13-19-31(49)21(35(53)29(33(19)51)25(47)12-10-2)15-23-37(55)27(17(4)45)41(59)43(7,8)39(23)57/h48-57H,9-15H2,1-8H3 |
| Chemical Name | 2-acetyl-4-[[3-[[3-[(5-acetyl-2,6-dihydroxy-3,3-dimethyl-4-oxocyclohexa-1,5-dien-1-yl)methyl]-5-butanoyl-2,4,6-trihydroxyphenyl]methyl]-5-butanoyl-2,4,6-trihydroxyphenyl]methyl]-3,5-dihydroxy-6,6-dimethylcyclohexa-2,4-dien-1-one |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets | Staphylococcus aureus Sortase A (SrtA) (IC50 = 24.17 µM)[4]。 |
| ln Vitro |
The natural product Dryocrasin ABBA was identified as an effective inhibitor of Staphylococcus aureus Sortase A (SrtA) enzyme activity. In a fluorescence resonance energy transfer (FRET) assay, Dryocrasin ABBA significantly decreased the fluorescence signal generated by SrtA-mediated cleavage of a model substrate peptide (Dabcyl-QALPETGEE-Edans), indicating inhibition of SrtA catalytic activity. The half-maximal inhibitory concentration (IC50) was determined to be 24.17 µM[4]。 Molecular dynamics simulations and mutagenesis studies revealed the molecular mechanism of inhibition. Dryocrasin ABBA binds directly to the active site of SrtA, primarily interacting with residues Ala104, Glu105, Val166, Gly167, Val168, Ile182, and Trp194. Key binding interactions include van der Waals forces with Val166 and Val168, and a strong hydrogen bond with Gly167. The binding free energy (ΔGbind) for the wild-type SrtA-Dryocrasin ABBA complex was calculated to be -25.8 ± 2.8 kcal/mol[4]。 To validate the binding site, point mutants V166A-SrtA and V168A-SrtA were constructed. The inhibitory effect of Dryocrasin ABBA (at 40 µM) was significantly reduced against these mutants compared to the wild-type SrtA in the FRET assay. The binding free energy for the mutants was weaker: -19.2 ± 3.1 kcal/mol for V166A and -15.3 ± 1.9 kcal/mol for V168A, confirming Val166 and Val168 as critical residues for Dryocrasin ABBA binding and activity inhibition[4]。 |
| ln Vivo |
In a mouse model infected with an amantadine-resistant HPAIV H5N1 strain (A/Chicken/Hebei/706/2005), oral administration of Dryocrassin ABBA significantly improved survival in a dose-dependent manner. Survival rates on day 14 post-infection were 87%, 80%, and 60% for the 33, 18, and 12.5 mg/kg/day treatment groups, respectively, compared to 53% for the amantadine (20 mg/kg/day) group and 20% for the untreated virus control group. [1] Dryocrassin ABBA treatment (33 and 18 mg/kg/day) significantly increased body weight gain in infected mice compared to the amantadine-treated and untreated groups. [1] On day 7 post-infection, treatment with Dryocrassin ABBA at 33 and 18 mg/kg/day significantly reduced lung virus loads compared to the untreated group (P < 0.01), and the reduction was not significantly different from the amantadine-treated group. [1] The lung index (dry lung-to-body weight ratio) on day 7 was significantly increased in all virus-infected groups compared to the uninfected control, but no significant difference was found between the Dryocrassin ABBA-treated groups and the amantadine-treated group. [1] On day 7 post-infection, Dryocrassin ABBA treatment (33 and 18 mg/kg/day) significantly modulated cytokine levels in bronchoalveolar lavage fluid (BALF). It significantly decreased pro-inflammatory cytokines (IL-6, TNF-α, IFN-γ, IL-12) and significantly increased anti-inflammatory cytokines (IL-10, MCP-1) compared to both the amantadine-treated and untreated control groups (P < 0.01). These effects showed a dose-dependent pattern for IL-6, IL-10, MCP-1, and IFN-γ. [1] In mice infected with amantadine-resistant H5N1 avian influenza virus (A/Chicken/Hebei/706/2005), oral administration of Dryocassin ABBA at doses of 33, 18, and 12.5 mg/kg resulted in survival rates of 87%, 80%, and 60%, respectively, compared to 53% in the amantadine-treated group and 20% in the untreated group[2]。 Mice treated with Dryocassin ABBA showed significant body weight gain compared to the untreated group[2]。 Lung virus loads were significantly reduced in the 33 and 18 mg/kg Dryocassin ABBA groups compared to the untreated group on day 7 post-infection[2]。 Pro-inflammatory cytokines (IL-6, TNF-α, IFN-γ, IL-12) in bronchoalveolar lavage fluid were significantly decreased, while anti-inflammatory cytokines (IL-10, MCP-1) were significantly increased in the 33 and 18 mg/kg Dryocassin ABBA groups compared to the amantadine and untreated groups on day 7[2]。 Lung index was reduced in Dryocassin ABBA-treated groups compared to the untreated group, though not statistically significant compared to the amantadine group[2]。 |
| Enzyme Assay |
A fluorescence resonance energy transfer (FRET) assay was used to determine the inhibitory activity of Dryocrasin ABBA against Staphylococcus aureus Sortase A (SrtA). Recombinant SrtA protein (wild-type or mutant) was pre-incubated with varying concentrations of Dryocrasin ABBA or a control solvent in a reaction buffer (50 mM Tris-HCl, 5 mM CaCl2, 150 mM NaCl, pH 7.5) for 30 minutes at 37°C. Subsequently, a fluorescent peptide substrate (Dabcyl-QALPETGEE-Edans) was added to each well of a 96-well plate to initiate the enzymatic reaction. The mixture was further incubated for 1 hour at 37°C. The cleavage of the substrate by SrtA relieves fluorescence quenching, leading to an increase in fluorescence intensity. The fluorescence signal was measured using a microplate reader with excitation at 350 nm and emission at 520 nm. The decrease in fluorescence signal in the presence of Dryocrasin ABBA compared to the control indicates inhibition of SrtA activity[4]。 The binding affinity (association constant, K_A) between Dryocrasin ABBA and SrtA was also measured using a fluorescence quenching method. Fluorescence emission spectra of SrtA were recorded at 345 nm (with a 10 nm band-pass) upon excitation at 280 nm (with a 5 nm band-pass) in the presence of increasing concentrations of Dryocrasin ABBA. The binding constant was calculated from the quenching data[4]。 |
| Animal Protocol |
Mouse Efficacy Study against H5N1: Specific pathogen-free (SPF) female BALB/c mice (n=20 per group) were infected intranasally with 10^4.5 ELD50 of the amantadine-resistant H5N1 virus (A/Chicken/Hebei/706/2005) in 100 µl saline. Starting from day 2 post-infection, mice received Dryocrassin ABBA via oral gavage once daily for 7 consecutive days (days 2 to 8). Three dose groups were used: 12.5, 18.0, and 33 mg/kg body weight per day. The positive control group received amantadine hydrochloride at 20 mg/kg/day via the same route and schedule. The untreated virus control and normal control groups received equivalent volumes of physiological saline. Mice were monitored daily for 14 days for body weight, activity, and mortality. On days 7 and 14 post-infection, subsets of mice were euthanized to collect lungs for lung index calculation and virus titration. [1] Cytokine Analysis: On day 7 post-infection, mice were euthanized, and lungs were lavaged with sterile saline to obtain bronchoalveolar lavage fluid (BALF). The BALF supernatant was collected after centrifugation. Cytokine concentrations (IL-12, IL-6, IL-10, INF-γ, MCP-1, TNF-α) were measured using a commercial cytokine bead array kit and flow cytometry. [1] SPF BALB/C female mice were inoculated intranasally with 10^4.5 ELD50 of H5N1 virus in 100 µL saline[2]。 Starting from day 2 post-infection, mice were orally administered Dryocassin ABBA at doses of 12.5, 18, and 33 mg/kg body weight, or amantadine hydrochloride at 20 mg/kg body weight, once daily for 7 days[2]。 Control groups received equivalent volumes of physiological saline[2]。 Body weight, activity, mortality, and survival time were monitored daily for 14 days[2]。 On days 7 and 14, mice were euthanized to collect lungs for lung index calculation and virus load determination[2]。 Bronchoalveolar lavage fluid was collected on day 7 for cytokine analysis using a flow cytometry-based cytokine kit[2]。 |
| Toxicity/Toxicokinetics |
The article cites a previous study stating that the maximum toxic dosage (MTD) of Dryocrassin ABBA is up to 2000 mg/kg body weight in Sprague-Dawley rats, and it is considered a non-toxic substance according to The European Pharmacopoeia 7.0. [1] In the current mouse study, no significant adverse effects or toxicity related to Dryocrassin ABBA administration at the tested doses (up to 33 mg/kg/day) were reported. [1] The maximum toxic dosage of Dryocassin ABBA in Sprague-Dawley rats is reported as 2000 mg/kg body weight, and it is considered a non-toxic substance according to The European Pharmacopoeia 7.0 (cited from another study, not from this article)[2]。 |
| References |
[1]. Dryocrassin ABBA, a novel active substance for use against amantadine-resistant H5N1 avian influenza virus. Front Microbiol. 2015 Jun 16;6:592. [2]. Dryocrassin ABBA, a novel active substance for use against amantadine-resistant H5N1 avian influenza virus. Front Microbiol. 2015 Jun 16;6:592. [3]. Dryocrassin ABBA Induces Apoptosis in Human Hepatocellular Carcinoma HepG2 Cells Through a Caspase-Dependent Mitochondrial Pathway. Asian Pac J Cancer Prev. 2016;17(4):1823-8. [4]. Molecular Mechanism of the Flavonoid Natural Product Dryocrassin ABBA against Staphylococcus aureus Sortase A. Molecules. 2016 Oct 26;21(11). [5]. An Inhibitory Effect of Dryocrassin ABBA on Staphylococcus aureus vWbp That Protects Mice From Pneumonia. Front Microbiol. 2019 Jan 23;10:7. [6]. Dryocrassin suppresses immunostimulatory function of dendritic cells and prolongs skin allograft survival. Cell Transplant. 2014;23(4-5):641-56. |
| Additional Infomation |
Dryocrassin ABBA is a phloroglucinol compound and is the major active component isolated from the traditional Chinese medicine Rhizoma Dryopteridis Crassirhizomatis (RDC). [1] RDC has been traditionally used to treat inflammatory and infectious diseases. [1] Dryocrassin ABBA demonstrated protective efficacy in mice against a lethal infection with an amantadine-resistant H5N1 avian influenza virus. [1] The proposed mechanism of action involves immunomodulation rather than direct virus inhibition. The protective effect is associated with alleviation of lung lesions, reduction of viral load, and a shift in the cytokine profile from pro-inflammatory to anti-inflammatory (decreasing IL-6, TNF-α, IFN-γ, IL-12; increasing IL-10 and MCP-1). [1] Dryocrassin ABBA is suggested as a potential novel lead compound for the development of therapies against amantadine-resistant avian influenza viruses. [1] Dryocassin ABBA is a phloroglucinol compound isolated from Rhizoma Dryopteridis Crassirhizomatis (RDC)[2]。 It exhibits antiviral activity against amantadine-resistant H5N1 avian influenza virus in a mouse model, likely through modulation of inflammatory cytokine responses[2]。 The compound is suggested as a potential lead compound for treating resistant avian influenza infections[2]。 Dryocrasin ABBA is a flavonoid natural product. This study identifies it as a novel inhibitor of Staphylococcus aureus Sortase A (SrtA), a key virulence factor enzyme that anchors surface proteins to the bacterial cell wall. Inhibiting SrtA represents an anti-virulence strategy, potentially disarming the bacteria without killing them, which may reduce selective pressure for antibiotic resistance. The findings suggest that Dryocrasin ABBA is a promising candidate for the development of therapeutic agents against S. aureus infections[4]。 |
Solubility Data
| Solubility (In Vitro) | May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 1.2183 mL | 6.0914 mL | 12.1828 mL | |
| 5 mM | 0.2437 mL | 1.2183 mL | 2.4366 mL | |
| 10 mM | 0.1218 mL | 0.6091 mL | 1.2183 mL |