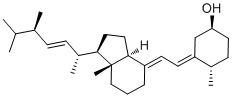
Dihydrotachysterol is a novel, synthetic vitamin D analogue that is activated in the liver and does not require renal hydroxylation like vitamin D2 (ergocalciferol) and vitamin D3 (cholecalciferol). DHT has a rapid onset of action (2 hours), a shorter half-life, and a greater effect on mineralization of bone salts than does vitamin D.
Physicochemical Properties
| Molecular Formula | C28H46O |
| Molecular Weight | 398.66 |
| Exact Mass | 398.355 |
| Elemental Analysis | C, 84.36; H, 11.63; O, 4.01 |
| CAS # | 67-96-9 |
| Related CAS # | 67-96-9 |
| PubChem CID | 5311071 |
| Appearance | White to off-white solid powder |
| Density | 1.003 g/cm3 |
| Boiling Point | 499.5ºC at 760 mmHg |
| Melting Point | 131ºC |
| Flash Point | 217.6ºC |
| Index of Refraction | 1.569 |
| LogP | 7.72 |
| Hydrogen Bond Donor Count | 1 |
| Hydrogen Bond Acceptor Count | 1 |
| Rotatable Bond Count | 5 |
| Heavy Atom Count | 29 |
| Complexity | 639 |
| Defined Atom Stereocenter Count | 7 |
| SMILES | CC([C@H](/C=C/[C@H]([C@]1(CC[C@]2(/C(=C/C=C3/C[C@@H](O)CC[C@@H]/3C)/CCC[C@]12C)[H])[H])C)C)C |
| InChi Key | ILYCWAKSDCYMBB-OPCMSESCSA-N |
| InChi Code | InChI=1S/C28H46O/c1-19(2)20(3)9-10-22(5)26-15-16-27-23(8-7-17-28(26,27)6)12-13-24-18-25(29)14-11-21(24)4/h9-10,12-13,19-22,25-27,29H,7-8,11,14-18H2,1-6H3/b10-9+,23-12+,24-13+/t20-,21-,22+,25-,26+,27-,28+/m0/s1 |
| Chemical Name | (1S,3E,4S)-3-[(2E)-2-[(1R,3aS,7aR)-1-[(E,2R,5R)-5,6-dimethylhept-3-en-2-yl]-7a-methyl-2,3,3a,5,6,7-hexahydro-1H-inden-4-ylidene]ethylidene]-4-methylcyclohexan-1-ol |
| Synonyms | Dihydrotachysterol; SDB 3314; HSDB3314; HSDB-3314; Parterol; Tachyrol; Hytakerol |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| ln Vitro | Dihydrotachysterol stimulates intestinal calcium absorption and mobilizes bone calcium to successfully raise serum calcium levels in the absence of parathyroid hormone and functional renal tissue [1]. Renal phosphate excretion can also be elevated by dihydrotachysterol [1]. |
| ln Vivo | A popular and powerful synthetic analog of vitamin D that costs more than vitamin D2 is dihydrotachysterol. Its half-life and onset time fall between that of calcitriol and vitamin D2. Hypoparathyroidism may be treated with dihydrotachysterol (final dose range: 0.004 to 0.04 mg/kg/day; first dose: 0.03 to 0.08 mg/kg/day for 2 to 3 days) [2]. |
| Animal Protocol |
Animal/Disease Models: Animal/Disease Models: 5 mixed-housed young to middle-aged cats [2] Doses: Initial dose is 0.03 to 0.08 mg/kg/day for 2 to 3 days. The final dose range is 0.004 to 0.04 mg/kg/day. Route of Administration: Oral Experimental Results: Effective in the treatment of hypoparathyroidism. |
| ADME/Pharmacokinetics |
Absorption, Distribution and Excretion Onset of action: Hypercalcemic: Several hours (maximal after 1 to 2 weeks). ...Major path of elimination of dihydrotachysterol & its metabolites is probably secretion into bile & excretion in feces ... dihydrotachysterol /is also/ excreted in breast milk ... Duration of action: following oral administration: Up to 9 weeks. The primary route of excretion of vitamin D is the bile; only a small percentage of an administered dose is found in urine. /Vitamin D/ For more Absorption, Distribution and Excretion (Complete) data for DIHYDROTACHYSTEROL (8 total), please visit the HSDB record page. Metabolism / Metabolites DHT3 /vitamin D3/ undergoes 25-hydroxylation to yield 25-hydroxydihydrotachysterol3 (25-OHDHT3), which appears to be active form of DHT (dihydrotachysterol) in both intestine & bone. High specific radioactivity (14)C- and (3)H-labeled dihydrotachysterol were prepared and their metabolites studied in rachitic chicks and rats. 20% dihydrotachysterol was excreted in the bile in the first 24 hours, about 50% as a carboxylic acid derivative. No hydroxylation at C-1 was observed, although polar metabolites were detected in all tissues. Larger proportions of the parent steroid and its 25-OH derivative were detected in tissues compared with cholecalciferol but no single metabolite was detected at the intracellular site of action of cholecalciferol. Biological Half-Life Absorbed vitamin D circulates in blood in association with vitamin D-binding protein, which is a specific alpha-globulin. Vitamin D disappears from plasma with /a half-life/ of 19 to 25 hr, but it is stored in body for prolonged periods (6 months or longer in rat) apparently in fat deposits throughout body. /Vitamin D/ |
| Toxicity/Toxicokinetics |
Toxicity Summary Once hydroxylated to 25-hydroxydihydrotachysterol, the modified drug binds to the vitamin D receptor. The bound form of the vitamin D receptor serves as a transcriptional regulator of bone matrix proteins, inducing the expression of osteocalcin and suppressing synthesis of type I collagen. Vitamin D (when bound to the vitamin D receptor)stimulates the expression of a number of proteins involved in transporting calcium from the lumen of the intestine, across the epithelial cells and into blood. This stimulates intestinal calcium absorption and increases renal phosphate excretion. These are functions that are normally carried out by the parathyroid hormone. Protein Binding >99% Interactions Corticosteroids counteract the effects of vitamin D analogs. /Vitamin D analogs/ Concurrent administration of thiazide diuretics and pharmacologic doses of vitamin D analogs in patients with hypoparathyroidism may result in hypercalcemia which may be transient and self-limited or may require discontinuance of vitamin D analogs. Thiazide-induced hypercalcemia in hypoparathyroid patients is probably caused by increased release of calcium from bone. /Vitamin D analogs/ Excessive use of mineral oil may interfere with intestinal absorption of vitamin D analogs. /Vitamin D analogs/ Orlistat may result in decreased GI absorption of fat-soluble vitamins such as vitamin D analogs. At least 2 hours should elapse between (before or after) any orlistat dose and vitamin D analog administration ... . /Vitamin D analogs/ For more Interactions (Complete) data for DIHYDROTACHYSTEROL (6 total), please visit the HSDB record page. |
| References |
[1]. Dihydrotachysterol therapy for hypoparathyroidism: consequences of inadequate monitoring. Five cases and a review. Exp Clin Endocrinol Diabetes. 2005 Jul;113(7):376-80. [2]. Idiopathic hypoparathyroidism in five cats. J Vet Intern Med. Jan-Feb 1991;5(1):47-51. |
| Additional Infomation |
Dihydrotachysterol is a hydroxy seco-steroid that is 9,10-secoergosta-5,7,22-triene substituted by a hydroxy group at position 3. A synthetic analogue of vitamin D that acts a bone density conservation agent. It has a role as a bone density conservation agent. It is a vitamin D, a hydroxy seco-steroid and a seco-ergostane. A vitamin D that can be regarded as a reduction product of vitamin D2. Dihydrotachysterol is only found in individuals that have used or taken this drug. It is a vitamin D that can be regarded as a reduction product of vitamin D2. [PubChem]Once hydroxylated to 25-hydroxydihydrotachysterol, the modified drug binds to the vitamin D receptor. The bound form of the vitamin D receptor serves as a transcriptional regulator of bone matrix proteins, inducing the expression of osteocalcin and suppressing synthesis of type I collagen. Vitamin D (when bound to the vitamin D receptor)stimulates the expression of a number of proteins involved in transporting calcium from the lumen of the intestine, across the epithelial cells and into blood. This stimulates intestinal calcium absorption and increases renal phosphate excretion. These are functions that are normally carried out by the parathyroid hormone. A VITAMIN D that can be regarded as a reduction product of vitamin D2. Drug Indication Used for the prevention and treatment of rickets or osteomalacia, and to manage hypocalcemia associated with hypoparathyroidism or pseudohypoparathyroidism. Also used for the treatment of vitamin D dependent rickets, rickets or osteomalacia secondary to long-term high dose anticonvulsant therapy, early renal osteodystrophy, osteoporosis (in conjunction with calcium), and hypophosphatemia associated with Fanconi syndrome (with treatment of acidosis). Mechanism of Action Once hydroxylated to 25-hydroxydihydrotachysterol, the modified drug binds to the vitamin D receptor. The bound form of the vitamin D receptor serves as a transcriptional regulator of bone matrix proteins, inducing the expression of osteocalcin and suppressing synthesis of type I collagen. Vitamin D (when bound to the vitamin D receptor)stimulates the expression of a number of proteins involved in transporting calcium from the lumen of the intestine, across the epithelial cells and into blood. This stimulates intestinal calcium absorption and increases renal phosphate excretion. These are functions that are normally carried out by the parathyroid hormone. Elevates serum calcium concentration by increasing intestinal absorption of calcium & possibly by enhancing urinary excretion of inorganic phosphate... /drug-induced/ phosphaturia may be ... due to increased serum calcium level and its effect on phosphate clearance by kidneys. Therapeutic Uses Bone Density Conservation Agents; Vitamins MEDICATION (VET): Calcium regulator used in veterinary medicine to treat hypercalcemia. Dihydrotachysterol is indicated ... for treatment of chronic and latent forms of post operative tetany and idiopathic tetany. /Included in US product labeling/ Therapeutic doses of specific vitamin D analogs are used in the treatment of chronic hypocalcemia, hypophosphatemia, rickets, and osteodystrophy associated with various medical conditions including chronic renal failure, familial hypophosphatemia, and hypoparathyroidism (postsurgical or idiopathic, or pseudohypoparathyroidism). Some analogs have been found to reduce elevated parathyroid hormone concentrations in patients with renal osteodystrophy associated with hyperparathyroidism. Theoretically, any of the vitamin D analogs may be used for the above conditions, However, because of their pharmacologic properties, some may be more useful in certain situations than others. Alfacalcidol, calcitriol, and dihydrotachysterol are usually preferred in patients with renal failure since these patients have impaired ability to synthesize calcitriol from cholecalciferol and ergocalciferol; therefore, the response is more predictable. In addition, their shorter half-lives may make toxicity easier to manage (hypercalcemia reverses more quickly). Ergocalciferol may not be the preferred agent in the treatment of familial hypophosphatemia or hypoparathyroidism because the large doses needed are associated with a risk of overdose and hypercalcemia; dihydrotachysterol and calcitriol may be preferred. /Included in US product labeling/ Drug Warnings /Dihydrotachysterol/...should not be used in presence of renal insufficiency or hyperphosphatemia. Extreme care must be used to prevent overdosage. Doses of vitamin D analogs that do not exceed the physiologic requirement are usually nontoxic. However, some infants and patients with sarcoidosis or hypoparathyroidism may have increased sensitivity to vitamin D analogs. /Vitamin D analogs/ Acute or chronic administration of excessive doses of vitamin D analogs or enhanced responsiveness to physiologic amounts of ergocalciferol or cholecalciferol may lead to hypervitaminosis D manifested by hypercalcemia. /Vitamin D analogs/ Decreased renal function without hypercalcemia has also been reported in patients with hypoparathyroidism after long-term vitamin D analog therapy. Before therapy with vitamin D analogs is initiated, serum phosphate concentrations must be controlled. To avoid ectopic calcification, the serum calcium (in mg/dL) times phosphorus (in mg/dL) should not be allowed to exceed 70. Because administration of vitamin D analogs may increase phosphate absorption, patients with renal failure may require adjustment in the dosage of aluminum-containing antacids used to decrease phosphate absorption. /Vitamin D analogs/ FDA Pregnancy Risk Category: C /RISK CANNOT BE RULED OUT. Adequate, well controlled human studies are lacking, and animal studies have shown risk to the fetus or are lacking as well. There is a chance of fetal harm if the drug is given during pregnancy; but the potential benefits may outweigh the potential risk./ Pharmacodynamics Dihydrotachysterol is hydroxylated in the liver to 25-hydroxydihydrotachysterol, which is the major circulating active form of the drug. It does not undergo further hydroxylation by the kidney and therefore is the analogue of 1, 25-dihydroxyvitamin D. Dihydrotachysterol is effective in the elevation of serum calcium by stimulating intestinal calcium absorption and mobilizing bone calcium in the absence of parathyroid hormone and of functioning renal tissue. Dihydrotachysterol also increases renal phosphate excretion. |
Solubility Data
| Solubility (In Vitro) | May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 2.5084 mL | 12.5420 mL | 25.0840 mL | |
| 5 mM | 0.5017 mL | 2.5084 mL | 5.0168 mL | |
| 10 mM | 0.2508 mL | 1.2542 mL | 2.5084 mL |