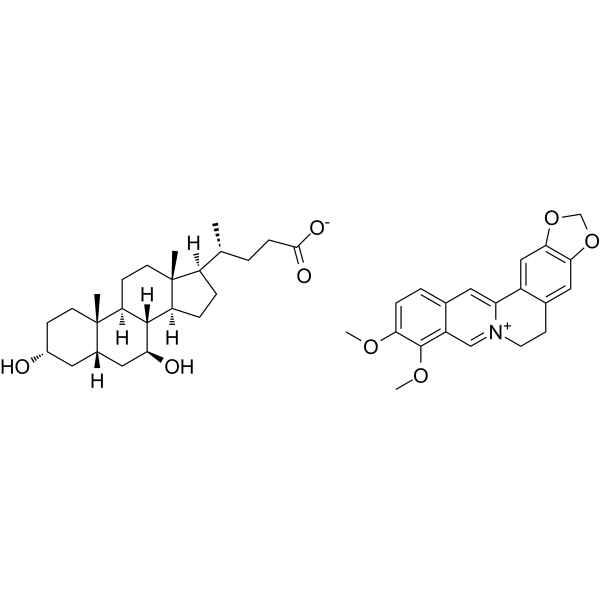
Physicochemical Properties
| Molecular Formula | C44H57NO8 |
| Molecular Weight | 727.925293684006 |
| Exact Mass | 727.408 |
| Elemental Analysis | C, 72.60; H, 7.89; N, 1.92; O, 17.58 |
| CAS # | 1868138-66-2 |
| Related CAS # | 117-74-8 (hydroxide);633-65-8 (chloride);316-41-6 (sulfate);633-66-9 (hydrosulfate); 2086-83-1 (cation); 1868138-66-2 (ursodeoxycholate); |
| PubChem CID | 137552085 |
| Appearance | Light yellow to yellow solid |
| Hydrogen Bond Donor Count | 2 |
| Hydrogen Bond Acceptor Count | 8 |
| Rotatable Bond Count | 5 |
| Heavy Atom Count | 53 |
| Complexity | 1090 |
| Defined Atom Stereocenter Count | 10 |
| SMILES | C[C@H](CCC(=O)[O-])[C@H]1CC[C@@H]2[C@@]1(CC[C@H]3[C@H]2[C@H](C[C@H]4[C@@]3(CC[C@H](C4)O)C)O)C.COC1=C(C2=C[N+]3=C(C=C2C=C1)C4=CC5=C(C=C4CC3)OCO5)OC |
| InChi Key | FHZVFXJRSFLYDY-FUXQPCDDSA-M |
| InChi Code | InChI=1S/C24H40O4.C20H18NO4/c1-14(4-7-21(27)28)17-5-6-18-22-19(9-11-24(17,18)3)23(2)10-8-16(25)12-15(23)13-20(22)26;1-22-17-4-3-12-7-16-14-9-19-18(24-11-25-19)8-13(14)5-6-21(16)10-15(12)20(17)23-2/h14-20,22,25-26H,4-13H2,1-3H3,(H,27,28);3-4,7-10H,5-6,11H2,1-2H3/q;+1/p-1/t14-,15+,16-,17-,18+,19+,20+,22+,23+,24-;/m1./s1 |
| Chemical Name | (4R)-4-[(3R,5S,7S,8R,9S,10S,13R,14S,17R)-3,7-dihydroxy-10,13-dimethyl-2,3,4,5,6,7,8,9,11,12,14,15,16,17-tetradecahydro-1H-cyclopenta[a]phenanthren-17-yl]pentanoate;16,17-dimethoxy-5,7-dioxa-13-azoniapentacyclo[11.8.0.02,10.04,8.015,20]henicosa-1(13),2,4(8),9,14,16,18,20-octaene |
| Synonyms | Berberine ursodeoxycholate; VM8KQ3W8GM; Berberine ursodeoxycholate; 1868138-66-2; VM8KQ3W8GM; UNII-VM8KQ3W8GM; 9,10-dimethoxy-5,6-dihydro-2H,8H-[1,3]dioxolo[4,5-g]isoquinolino[3,2-a]isoquinolin-8-ylium 3alpha,7beta-dihydroxy-5beta-cholan-24-oate; Cholan-24-oic acid, 3,7-dihydroxy-, ion(1-), (3alpha,5beta,7beta)-, 5,6-dihydro-9,10-dimethoxybenzo[g]-1,3-benzodioxolo[5,6-a]quinolizinium (1:1); 9,10-dimethoxy-5,6-dihydro-2H,8H-(1,3)dioxolo(4,5-g)isoquinolino(3,2-a)isoquinolin-8-ylium 3alpha,7beta-dihydroxy-5beta-cholan-24-oate; Cholan-24-oic acid, 3,7-dihydroxy-, ion(1-), (3alpha,5beta,7beta)-, 5,6-dihydro-9,10-dimethoxybenzo(g)-1,3-benzodioxolo(5,6-a)quinolizinium (1:1); HTD1801; HTD-1801; UNII-VM8KQ3W8GM; BUDCA |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month Note: Please store this product in a sealed and protected environment (e.g. under nitrogen), avoid exposure to moisture and light. |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
Hypolipidemic agent; - berberine ursodeoxycholate (BUDCA) was reported to modulate targets associated with non-alcoholic steatohepatitis (NASH) and type 2 diabetes (T2DM), including AMP-activated protein kinase (AMPK) and farnesoid X receptor (FXR), but no specific IC50, Ki, or EC50 values were provided in the study [1] |
| ln Vitro |
- In vitro metabolism studies of berberine ursodeoxycholate (BUDCA) were conducted using human liver microsomes to assess its interaction with cytochrome P450 (CYP) enzymes. Incubations were performed with different concentrations of BUDCA and specific CYP substrates; the results showed that BUDCA did not significantly inhibit the activity of major CYP isoforms (CYP1A2, CYP2C9, CYP2C19, CYP2D6, CYP3A4) at concentrations up to 100 μM, indicating a low potential for drug-drug interactions mediated by these enzymes [2] |
| ln Vivo |
Glycated hemoglobin (HbA1c) levels are considerably lowered by berberine ursodeoxycholate, with an average 0.6% drop in HbA1c values[1]. The gastrointestinal tract is assumed to quickly separate ingested berberine ursodeoxycholic acid, which is absorbed differently from berberine [1]. Berberine ursodeoxycholic acid is taken as a salt.
- In a phase 2 RCT involving patients with presumed NASH and T2DM, berberine ursodeoxycholate (BUDCA) was administered orally at a dose of 400 mg twice daily for 12 weeks. The primary efficacy endpoint was the change in liver fat content measured by magnetic resonance proton density fat fraction (MRI-PDFF). Compared with the placebo group, the BUDCA group showed a statistically significant reduction in liver fat content: the mean change from baseline was -2.3% in the BUDCA group versus -0.7% in the placebo group (p=0.02). Additionally, the BUDCA group exhibited a trend toward improvement in glycemic parameters, including a reduction in glycated hemoglobin (HbA1c) (mean change: -0.3% vs. -0.1% in placebo, p=0.12) and fasting plasma glucose (FPG) (mean change: -0.5 mmol/L vs. -0.1 mmol/L in placebo, p=0.08) [1] - In a pharmacokinetic/pharmacodynamic study of berberine ursodeoxycholate (BUDCA) (designated as HTD1801) in patients with hyperlipidemia, single oral doses (100 mg, 200 mg, 400 mg) and multiple oral doses (200 mg twice daily for 14 days) were administered. For the pharmacodynamic (PD) effects, after 14 days of multiple dosing, the BUDCA group showed significant reductions in total cholesterol (TC) (mean change: -12.3% from baseline, p<0.05), low-density lipoprotein cholesterol (LDL-C) (mean change: -15.6% from baseline, p<0.05), and triglycerides (TG) (mean change: -10.2% from baseline, p<0.05), compared with baseline values. No significant changes in high-density lipoprotein cholesterol (HDL-C) were observed [2] |
| Enzyme Assay |
- For the assessment of berberine ursodeoxycholate (BUDCA)’s effect on CYP enzyme activity, human liver microsomes were thawed and diluted in a reaction buffer containing NADPH-generating system (glucose-6-phosphate, glucose-6-phosphate dehydrogenase, NADP+). Different concentrations of BUDCA (0.1 μM to 100 μM) were added to the microsome mixture, followed by the addition of specific fluorescent or radiolabeled substrates for each CYP isoform (e.g., phenacetin for CYP1A2, tolbutamide for CYP2C9, omeprazole for CYP2C19, dextromethorphan for CYP2D6, midazolam for CYP3A4). The reaction mixtures were incubated at 37°C for a predetermined time (30-60 minutes) depending on the isoform. After incubation, the reactions were terminated by adding a quenching agent (e.g., acetonitrile). The formation of metabolite products was quantified using high-performance liquid chromatography (HPLC) or liquid chromatography-tandem mass spectrometry (LC-MS/MS). The activity of each CYP isoform in the presence of BUDCA was compared to that in the absence of BUDCA (vehicle control) to determine the inhibition potential [2] - No enzyme assay or target binding experiment (e.g., kinase activity, SPR, ITC, HTRF) related to berberine ursodeoxycholate (BUDCA) was described in the phase 2 RCT [1] |
| Animal Protocol | Non-alcoholic steatohepatitis is frequently associated with diabetes and may cause progressive liver disease. Current treatment options are limited. Here we report on a prospective, randomised, double-blind, placebo-controlled trial of two doses of HTD1801 (berberine ursodeoxycholate, an ionic salt of berberine and ursodeoxycholic acid), versus placebo that was conducted in 100 subjects with fatty liver disease and diabetes (NCT03656744). Treatment was for 18 weeks with a primary endpoint of reduction in liver fat content measured by magnetic resonance imaging proton density fat fraction. Key secondary endpoints included improvement in glycemic control, liver-associated enzymes and safety. The pre-specified primary endpoint was met. Thus, subjects receiving 1000 mg twice a day of berberine ursodeoxycholate had significantly greater reduction in liver fat content than in placebo recipients (mean absolute decrease -4.8% vs. -2.0% (p = 0.011). Compared to placebo, subjects receiving this dose also experienced significant improvement in glycemic control as well as reductions in liver-associated enzymes and significant weight loss. Diarrhea and abdominal discomfort were the most frequently reported adverse events. We conclude that berberine ursodeoxycholate has a broad spectrum of metabolic activity in patients with presumed NASH and diabetes. It is relatively well tolerated and merits further development as a treatment for NASH with diabetes [1]. |
| ADME/Pharmacokinetics |
- In the phase 2 RCT of berberine ursodeoxycholate (BUDCA) in patients with NASH and T2DM, limited pharmacokinetic data were reported: after oral administration of 400 mg twice daily, the steady-state plasma concentration (Css) of BUDCA was approximately 15-20 ng/mL, with a time to reach steady state (Tss) of 7-10 days [1] - In the pharmacokinetic study of berberine ursodeoxycholate (BUDCA) (HTD1801) in hyperlipidemic patients: 1. Single-dose pharmacokinetics: After oral administration of 100 mg, 200 mg, and 400 mg BUDCA, the maximum plasma concentration (Cmax) values were 6.2 ± 1.8 ng/mL, 13.8 ± 3.5 ng/mL, and 28.5 ± 6.9 ng/mL, respectively (dose-proportional increase). The time to reach Cmax (Tmax) was 2.5 ± 0.8 h, 3.0 ± 1.0 h, and 3.2 ± 1.1 h, respectively. The area under the plasma concentration-time curve from time 0 to infinity (AUC0-∞) was 32.4 ± 8.7 ng·h/mL, 67.9 ± 15.2 ng·h/mL, and 139.6 ± 28.5 ng·h/mL, respectively. The elimination half-life (t1/2) was 9.8 ± 2.1 h, 10.2 ± 2.3 h, and 10.5 ± 2.5 h, respectively. 2. Multiple-dose pharmacokinetics: After 14 days of oral administration of 200 mg BUDCA twice daily, the steady-state Cmax (Css,max) was 21.6 ± 4.8 ng/mL, the steady-state minimum plasma concentration (Css,min) was 8.3 ± 2.2 ng/mL, and the area under the plasma concentration-time curve over a 24-hour period at steady state (AUC0-24,ss) was 102.3 ± 22.6 ng·h/mL. The accumulation ratio (Rac) (AUC0-24,ss / AUC0-24 after single dose) was 1.5 ± 0.3. 3. Absorption and distribution: BUDCA showed moderate oral absorption, with no significant binding to red blood cells. The apparent volume of distribution (Vd/F) after single 200 mg dose was 12,500 ± 3,200 L, indicating extensive tissue distribution. 4. Metabolism and excretion: Approximately 15-20% of the administered dose was excreted as unchanged BUDCA in urine within 24 hours; the remaining dose was metabolized in the liver (mainly via glucuronidation) and excreted in feces [2] |
| Toxicity/Toxicokinetics |
- In the phase 2 RCT of berberine ursodeoxycholate (BUDCA) (400 mg twice daily for 12 weeks) in NASH and T2DM patients: 1. Adverse events (AEs): The most common AEs were gastrointestinal reactions, including diarrhea (12% in BUDCA group vs. 8% in placebo group), nausea (8% vs. 5%), and abdominal discomfort (6% vs. 3%). All AEs were mild to moderate in severity, and no severe AEs or treatment-related serious adverse events (SAEs) were reported. 2. Liver and kidney function: No significant changes in alanine aminotransferase (ALT), aspartate aminotransferase (AST), bilirubin, serum creatinine, or estimated glomerular filtration rate (eGFR) were observed in the BUDCA group compared with baseline or placebo group [1] - In the pharmacokinetic/pharmacodynamic study of berberine ursodeoxycholate (BUDCA) in hyperlipidemic patients (single doses up to 400 mg and multiple doses of 200 mg twice daily for 14 days): 1. Adverse events: Similar to the phase 2 RCT, mild gastrointestinal AEs (diarrhea: 10%, nausea: 7%) were reported, with no severe or serious AEs. 2. Plasma protein binding: In vitro plasma protein binding assay showed that BUDCA bound to human plasma proteins at a rate of 82 ± 4% (determined by ultrafiltration method) [2] |
| References |
[1]. A phase 2, proof of concept, randomised controlled trial of berberine ursodeoxycholate in patients with presumed non-alcoholic steatohepatitis and type 2 diabetes. Nat Commun. 2021 Sep 17;12(1):5503. [2]. Pharmacokinetics and pharmacodynamics of HTD1801 (berberine ursodeoxycholate, BUDCA) in patients with hyperlipidemia. Lipids Health Dis. 2020 Nov 12;19(1):239. |
| Additional Infomation |
- berberine ursodeoxycholate (BUDCA) is a novel conjugate of berberine (a natural alkaloid with hypoglycemic and hypolipidemic effects) and ursodeoxycholic acid (a bile acid with hepatoprotective effects), designed to synergistically target the pathogenesis of NASH and metabolic comorbidities (e.g., T2DM, hyperlipidemia). The phase 2 RCT (NCT03590362) included 100 patients (50 in BUDCA group, 50 in placebo group) who met the criteria of presumed NASH (based on MRI-PDFF ≥5%) and T2DM (HbA1c 7.0-10.0%). The study concluded that BUDCA was well-tolerated and showed preliminary efficacy in reducing liver fat content in this patient population [1] - The pharmacokinetic/pharmacodynamic study of berberine ursodeoxycholate (BUDCA) (HTD1801) was a phase 1b, open-label, single-center study involving 36 hyperlipidemic patients (TC ≥5.2 mmol/L or LDL-C ≥3.4 mmol/L). The study aimed to characterize the PK profile of BUDCA and evaluate its preliminary PD effects on lipid parameters. The results supported the further development of BUDCA for the treatment of hyperlipidemia, particularly in patients with comorbid metabolic disorders [2] |
Solubility Data
| Solubility (In Vitro) | DMSO : ~5 mg/mL (~6.87 mM) |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 1.3738 mL | 6.8688 mL | 13.7376 mL | |
| 5 mM | 0.2748 mL | 1.3738 mL | 2.7475 mL | |
| 10 mM | 0.1374 mL | 0.6869 mL | 1.3738 mL |