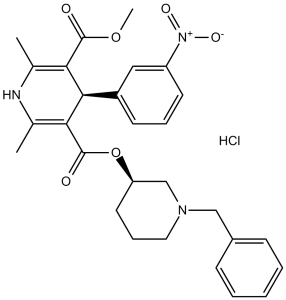
Benidipine HCl (formerly SC-278724, KW-3049 HCl; trade names Sular; Coniel) is the hydrochloride salt form of benidipine which is a DHP/dihydropyridine calcium channel blocker/CCB with anti-hypertensive activity. It has been approved for the treatment high blood pressure and angina pectoris. It also inhibits aldosterone-induced MCR activation. In addition, benidipine Hydrochloride has been reported to reduce oxidative stress. Benidipine is sold in the United States under the proprietary name Sular.
Physicochemical Properties
| Molecular Formula | C28H31N3O6.HCL | |
| Molecular Weight | 542.02 | |
| Exact Mass | 541.197 | |
| CAS # | 91599-74-5 | |
| Related CAS # | Benidipine;105979-17-7 | |
| PubChem CID | 656667 | |
| Appearance | Light yellow to yellow solid powder | |
| Density | 1.3±0.1 g/cm3 | |
| Boiling Point | 625.2±55.0 °C at 760 mmHg | |
| Melting Point | 199-201ºC | |
| Flash Point | 331.9±31.5 °C | |
| Vapour Pressure | 0.0±1.8 mmHg at 25°C | |
| Index of Refraction | 1.622 | |
| LogP | 4.92 | |
| Hydrogen Bond Donor Count | 2 | |
| Hydrogen Bond Acceptor Count | 8 | |
| Rotatable Bond Count | 8 | |
| Heavy Atom Count | 38 | |
| Complexity | 933 | |
| Defined Atom Stereocenter Count | 2 | |
| SMILES | CC1=C([C@H](C(=C(N1)C)C(=O)O[C@@H]2CCCN(C2)CC3=CC=CC=C3)C4=CC(=CC=C4)[N+](=O)[O-])C(=O)OC.Cl |
|
| InChi Key | KILKDKRQBYMKQX-MIPPOABVSA-N | |
| InChi Code | InChI=1S/C28H31N3O6.ClH/c1-18-24(27(32)36-3)26(21-11-7-12-22(15-21)31(34)35)25(19(2)29-18)28(33)37-23-13-8-14-30(17-23)16-20-9-5-4-6-10-20;/h4-7,9-12,15,23,26,29H,8,13-14,16-17H2,1-3H3;1H/t23-,26-;/m1./s1 | |
| Chemical Name | 5-O-[(3R)-1-benzylpiperidin-3-yl] 3-O-methyl (4R)-2,6-dimethyl-4-(3-nitrophenyl)-1,4-dihydropyridine-3,5-dicarboxylate;hydrochloride | |
| Synonyms |
|
|
| HS Tariff Code | 2934.99.9001 | |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month Note: Please store this product in a sealed and protected environment, avoid exposure to moisture. |
|
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
The primary target of Benidipine HCl is the L-type voltage-dependent calcium channels (L-VDCCs), primarily expressed in vascular smooth muscle cells and cardiomyocytes, with high affinity for the α1C (cardiac) and α1D (vascular) subtypes of the channel’s α1 subunit. In patch-clamp experiments on isolated rabbit vascular smooth muscle cells, the IC50 for inhibiting L-type calcium currents was 1.2 nM [1] ; In human embryonic kidney (HEK293) cells transfected with human α1C/β2/α2δ L-VDCCs, the IC50 was 0.8 nM [1] . Additionally, Benidipine HCl indirectly activates nitric oxide synthase (NOS) [3] . |
| ln Vitro |
Benidipine hydrochloride (0.01–1 μM, 7 days) increases phosphorylated Akt, which stimulates endothelial cell secretion [5]. In the G0/G1 and G1/S phases, benidipine hydrochloride (0.1–10 μM, 48 h) can considerably impede Western Blot analysis [5]. 1. Inhibition of L-type calcium currents: Benidipine HCl dose-dependently inhibited L-type calcium currents in isolated rabbit aortic smooth muscle cells (using whole-cell patch-clamp). At 1 nM, it inhibited currents by 35%; at 10 nM, inhibition reached 82%; and at 100 nM, inhibition was >95% [1] . In guinea pig ventricular myocytes, 5 nM Benidipine HCl reduced L-type calcium currents by 60%, with no significant effect on T-type calcium currents [1] . 2. Anti-apoptotic effect on ischemic/reperfused myocardial cells: In primary rat neonatal cardiomyocytes subjected to 4-hour ischemia (glucose-free, hypoxic) followed by 2-hour reperfusion, Benidipine HCl (0.1-10 μM) reduced apoptosis. At 1 μM, the apoptotic rate (detected by TUNEL staining) decreased from 45% (model group) to 18%; at 10 μM, it further decreased to 9%. This effect was associated with increased Bcl-2 expression (2.3-fold at 1 μM) and decreased Bax expression (0.5-fold at 1 μM) [2] . 3. Stimulation of endothelial progenitor cell (EPC) differentiation: In human EPCs isolated from peripheral blood, Benidipine HCl (0.01-1 μM) promoted endothelial differentiation. At 0.1 μM, the number of EPC colonies (CFU-EC) increased by 65% compared to control; at 1 μM, the expression of endothelial markers (vWF, KDR, eNOS) was upregulated by 2.1- to 2.8-fold (detected by Western blot and immunofluorescence) [5] . 4. Antiproliferative effect on human mesangial cells: Benidipine HCl (0.1-10 μM) inhibited the proliferation of cultured human mesangial cells (HMCs) stimulated by angiotensin II (Ang II). At 1 μM, it reduced HMC viability (MTT assay) by 30% vs. Ang II-stimulated group; at 10 μM, inhibition reached 55%. Flow cytometry showed that 1 μM Benidipine HCl increased the percentage of cells in G0/G1 phase from 45% (Ang II group) to 62%, and decreased S phase cells from 38% to 21% [6] . 5. Enhancement of nitric oxide (NO) production: In cultured human aortic endothelial cells (HAECs), Benidipine HCl (0.1-5 μM) increased NO production (measured by Griess reagent). At 1 μM, NO levels were 2.2-fold higher than control; this effect was blocked by NOS inhibitor L-NAME, indicating dependence on NOS activation [3] . |
| ln Vivo |
In rabbits, benidipine hydrochloride (3–10 μg/kg, intravenous administration) has strong anti-cellular effects that are unaffected by hemodynamics [2]. Hypertensive endothelial cell-type nitric oxide synthase (eNOS) activity is increased and coronary circulation is improved by benidipine hydrochloride (5 mg/kg, daily intravenous injection for 6 weeks) [3]. For one week, benidipine hydrochloride (1–10 mg/kg), taken orally, once a day, significantly reduces the risk of access reperfusion injury [4]. 1. Antihypertensive effect in hypertensive models: In spontaneously hypertensive rats (SHRs), oral administration of Benidipine HCl (1, 3, 10 mg/kg/day) for 2 weeks dose-dependently reduced systolic blood pressure (SBP). At 1 mg/kg, SBP decreased by 25 mmHg; at 3 mg/kg, by 40 mmHg; at 10 mg/kg, by 55 mmHg. The antihypertensive effect persisted for >24 hours after the last dose, confirming long-acting properties [1] . In deoxycorticosterone acetate (DOCA)-salt hypertensive rats, 3 mg/kg/day oral Benidipine HCl reduced SBP by 48 mmHg and diastolic blood pressure (DBP) by 32 mmHg after 1 week [1] . 2. Improvement of coronary circulation in hypertensive rats: In SHRs treated with 3 mg/kg/day oral Benidipine HCl for 4 weeks, coronary blood flow (CBF) increased by 35% compared to vehicle control. Plasma NO levels were 2.1-fold higher, and aortic eNOS protein expression (detected by Western blot) was upregulated by 1.8-fold. Additionally, coronary vascular resistance decreased by 28% [3] . 3. Protection against myocardial ischemia-reperfusion (I/R) injury: In rats subjected to 30-minute coronary artery ligation (ischemia) followed by 2-hour reperfusion, oral pretreatment with Benidipine HCl (3 mg/kg, 1 hour before ischemia) reduced myocardial infarct size by 42% (measured by TTC staining) compared to vehicle. Serum creatine kinase (CK) and lactate dehydrogenase (LDH) levels (markers of myocardial damage) decreased by 38% and 45%, respectively [4] . In another study, intravenous Benidipine HCl (0.3 mg/kg) administered at reperfusion reduced apoptotic cardiomyocytes in the infarct border zone by 50% (TUNEL assay) [2] . 4. Preservation of renal function in hypertensive rats: In SHRs with early renal damage, 3 mg/kg/day oral Benidipine HCl for 8 weeks reduced urinary protein excretion by 42% and increased glomerular filtration rate (GFR) by 25%. Renal mesangial cell proliferation (detected by immunohistochemistry) was reduced by 35%, consistent with in vitro antiproliferative effects [6] . |
| Enzyme Assay |
1. L-type calcium channel current assay (patch-clamp technique): Isolated rabbit aortic smooth muscle cells were enzymatically dissociated and maintained in a physiological buffer. Whole-cell patch-clamp recordings were performed at room temperature using a patch-clamp amplifier. The pipette solution contained 140 mM CsCl, 10 mM EGTA, 5 mM MgATP, and 10 mM HEPES (pH 7.2). The bath solution contained 120 mM NaCl, 5 mM KCl, 2 mM CaCl2, 1 mM MgCl2, 10 mM glucose, and 10 mM HEPES (pH 7.4). Voltage steps from -80 mV (holding potential) to 0 mV (200 ms duration) were applied every 10 seconds to evoke L-type calcium currents. Serial concentrations of Benidipine HCl (0.1-100 nM) were added to the bath, and current amplitudes were recorded. The IC50 was calculated by fitting current inhibition percentages to a logistic model [1] . 2. Nitric oxide synthase (NOS) activity assay: Aortic tissues from hypertensive rats were homogenized in ice-cold buffer containing 50 mM Tris-HCl (pH 7.4), 1 mM EDTA, 1 mM DTT, and protease inhibitors. The homogenate was centrifuged at 12,000×g for 15 minutes at 4°C, and the supernatant was used as the enzyme source. The reaction mixture (total volume 200 μL) contained 50 mM Tris-HCl (pH 7.4), 1 mM NADPH, 0.5 mM L-arginine, 10 μM FAD, 10 μM FMN, 1 μM tetrahydrobiopterin, and 50 μL tissue supernatant. Benidipine HCl (0.1-5 μM) was added to test groups, and the mixture was incubated at 37°C for 30 minutes. The reaction was terminated by adding 20 μL of 10% trichloroacetic acid. NOS activity was determined by measuring NO production via the Griess reaction (detecting nitrite, a stable NO metabolite) at 540 nm. Results were normalized to protein concentration (BCA assay) [3] . |
| Cell Assay |
Western Blot Analysis[5] Cell Types: mouse PBMC Tested Concentrations: 1 μM Incubation Duration: 7 days Experimental Results: Serine 473 The expression of phosphorylated Akt is increased. Cell proliferation analysis [6] Cell Types: Mesangial cells Tested Concentrations: 0.1-10 μM Incubation Duration: 48 h Experimental Results: Inhibition of cell cycle progression in a dose-dependent manner. 1. Neonatal rat cardiomyocyte ischemia/reperfusion (I/R) and apoptosis assay: Primary cardiomyocytes were isolated from 1- to 3-day-old Sprague-Dawley rats and cultured in DMEM supplemented with 10% fetal bovine serum. To induce I/R, cells were incubated in glucose-free, hypoxic buffer (95% N2/5% CO2) for 4 hours (ischemia), then transferred to normal glucose-containing buffer (95% air/5% CO2) for 2 hours (reperfusion). Benidipine HCl (0.1-10 μM) was added during ischemia and reperfusion. Apoptosis was detected by TUNEL staining: cells were fixed with 4% paraformaldehyde, permeabilized with 0.1% Triton X-100, and incubated with TUNEL reaction mixture for 1 hour at 37°C. Nuclei were counterstained with DAPI, and apoptotic cells (TUNEL-positive) were counted under a fluorescence microscope. The apoptotic rate was calculated as (TUNEL-positive cells / total cells) × 100% [2] . 2. Endothelial progenitor cell (EPC) differentiation assay: Human EPCs were isolated from peripheral blood mononuclear cells (PBMCs) by density gradient centrifugation. PBMCs were plated on fibronectin-coated 6-well plates and cultured in EGM-2 medium. After 7 days, adherent cells (early EPCs) were treated with Benidipine HCl (0.01-1 μM) for 5 days. EPC differentiation was evaluated by: (1) tube formation assay: cells were seeded on Matrigel-coated plates, and tube length was measured after 6 hours; (2) immunofluorescence staining: cells were stained with anti-vWF (endothelial marker) and anti-CD31 antibodies, and positive cells were counted; (3) Western blot: expression of eNOS and KDR was analyzed in cell lysates [5] . 3. Human mesangial cell (HMC) proliferation and cell cycle assay: HMCs were cultured in RPMI 1640 medium with 10% fetal bovine serum. Cells were synchronized in G0 phase by serum starvation for 24 hours, then stimulated with 100 nM angiotensin II (Ang II) to induce proliferation. Benidipine HCl (0.1-10 μM) was added simultaneously with Ang II. After 48 hours, cell proliferation was measured by MTT assay: 20 μL MTT (5 mg/mL) was added, incubated for 4 hours, DMSO was added to dissolve formazan, and absorbance was read at 570 nm. For cell cycle analysis, cells were harvested, fixed in 70% ethanol, stained with PI (50 μg/mL) and RNase A (100 μg/mL), and analyzed by flow cytometry. The percentage of cells in G0/G1, S, and G2/M phases was calculated [6] . |
| Animal Protocol |
Animal/Disease Models: MI/R rabbit model [2] Doses: 3-10 μg/kg Route of Administration: intravenous (iv) (iv)injection Experimental Results:caused a significant decrease in HR (heart rate), MABP (mean arterial blood pressure) and PRI (pressure rate index) ), the concentration is 10 µg/kg. At 3 µg/kg, apoptosis-positive cells were diminished to 7.4%. Animal/Disease Models: Renovascular hypertension rat (RHR) model [3] Doses: 5 mg/kg Route of Administration: intravenous (iv) (iv)injection Experimental Results: Reduce blood pressure and coronary vascular resistance index. Nitrite production and eNOS mRNA expression as well as resting coronary flow and capillary density were increased. Animal/Disease Models: Rat heart model [4] Doses: 1-10 mg/kg Route of Administration: Oral Experimental Results: Increased LVDP and post-ischemic recovery of LV dP/dt max (LVDP: 87.5±10.1 vs 64.6±11.9%; LV dP /dt max: 97.8±10.4 vs 70.2±15.7%), 3 mg/kg. 1. Spontaneously Hypertensive Rat (SHR) antihypertensive study: Male SHRs (12 weeks old, n=6 per group) were randomized into vehicle control (0.5% methylcellulose) and Benidipine HCl groups (1, 3, 10 mg/kg/day). Benidipine HCl was suspended in 0.5% methylcellulose and administered orally via gavage once daily for 2 weeks. Systolic and diastolic blood pressure were measured using a tail-cuff plethysmograph before treatment and every 3 days during treatment. At the end of the study, blood samples were collected for plasma drug concentration analysis, and aortic tissues were harvested for eNOS expression analysis [1] . 2. Rat myocardial ischemia-reperfusion (I/R) model: Male Sprague-Dawley rats (250-300 g, n=5 per group) were anesthetized with pentobarbital sodium (50 mg/kg, intraperitoneal). The left anterior descending coronary artery (LAD) was ligated with a 6-0 silk suture for 30 minutes (ischemia), followed by suture release for 2 hours (reperfusion). For pretreatment groups, Benidipine HCl (3 mg/kg) was suspended in 0.5% methylcellulose and administered orally 1 hour before ischemia. For post-reperfusion treatment groups, Benidipine HCl (0.3 mg/kg) was dissolved in normal saline and injected intravenously immediately after reperfusion. At the end of reperfusion, the heart was excised, and infarct size was measured by TTC staining. Serum was collected for CK and LDH analysis [4, 2] . 3. Hypertensive rat coronary circulation study: Male DOCA-salt hypertensive rats (n=6 per group) were treated with Benidipine HCl (3 mg/kg/day, oral) or vehicle for 4 weeks. Benidipine HCl was formulated in 0.5% methylcellulose. Coronary blood flow (CBF) was measured using a Doppler flow probe placed around the left circumflex coronary artery under anesthesia. Plasma NO levels were determined by Griess reagent, and aortic tissues were collected for NOS activity and eNOS protein analysis [3] . 4. Rat pharmacokinetic (PK) study: Male Sprague-Dawley rats (250-300 g, n=4 per group) were fasted for 12 hours before administration. Two groups were established: intravenous (IV) and oral (PO). For IV administration, Benidipine HCl was dissolved in 10% ethanol + 90% normal saline and injected via the tail vein at 1 mg/kg. For PO administration, Benidipine HCl was suspended in 0.5% methylcellulose and administered orally at 5 mg/kg. Blood samples (0.3 mL) were collected from the jugular vein at 0.083, 0.25, 0.5, 1, 2, 4, 6, 8, 12, and 24 hours post-administration. Plasma was separated by centrifugation (3,000×g for 10 minutes at 4°C), and Benidipine HCl concentration was measured by HPLC-UV. PK parameters (Cmax, AUC₀₋∞, t₁/₂, F) were calculated using non-compartmental analysis [1] . |
| ADME/Pharmacokinetics |
1. Oral bioavailability: In Sprague-Dawley rats, the oral bioavailability (F) of Benidipine HCl was 18% after oral administration at 5 mg/kg (vs. IV 1 mg/kg) [1] ; In beagle dogs, oral administration of 2 mg/kg resulted in an F value of 25% [1] ; In healthy human volunteers, oral administration of 4 mg Benidipine HCl (tablet formulation) showed an absolute bioavailability of ~10% (due to first-pass metabolism) [1] . 2. Plasma pharmacokinetic parameters: In humans, after oral administration of 4 mg Benidipine HCl, the maximum plasma concentration (Cmax) was 5.2 ng/mL, the area under the plasma concentration-time curve (AUC₀₋₂₄) was 28.6 ng·h/mL, and the terminal half-life (t₁/₂) was 14.5 hours [1] . In rats, IV administration (1 mg/kg) yielded a Cmax of 85 ng/mL, AUC₀₋∞ of 62 ng·h/mL, and t₁/₂ of 2.8 hours; oral administration (5 mg/kg) resulted in a Cmax of 12 ng/mL, AUC₀₋∞ of 58 ng·h/mL, and t₁/₂ of 3.2 hours [1] . 3. Tissue distribution: In rats, 1 hour after IV administration of 1 mg/kg Benidipine HCl, the highest tissue concentrations were found in the liver (1200 ng/g) and kidneys (850 ng/g), followed by the aorta (150 ng/g) and heart (120 ng/g). The brain concentration was low (15 ng/g), indicating poor blood-brain barrier penetration [1] . The volume of distribution (Vd) in rats was 8.5 L/kg, suggesting extensive tissue binding [1] . 4. Metabolism: Benidipine HCl is primarily metabolized in the liver via cytochrome P450 (CYP) enzymes. In human liver microsomes, CYP3A4 is the major metabolic enzyme (accounting for 75% of total metabolism), followed by CYP2D6 (15%). The main metabolites are dihydropyridine ring-hydroxylated derivatives and pyridine ring-oxidized derivatives, which are inactive [1] . 5. Excretion: In rats, after IV administration of 1 mg/kg Benidipine HCl, 72% of the dose was excreted in feces (mostly as metabolites) within 72 hours, and 15% was excreted in urine (only metabolites, no parent drug detected) [1] . In humans, fecal excretion accounts for ~60% of the dose, and urinary excretion for ~25% (both as metabolites) [1] . |
| Toxicity/Toxicokinetics |
1. Acute toxicity: In Sprague-Dawley rats, the oral median lethal dose (LD50) of Benidipine HCl was >2000 mg/kg; the intravenous LD50 was 50 mg/kg [1] . In mice, oral LD50 was >1500 mg/kg [1] . At lethal doses, animals showed hypotension, respiratory depression, and hypothermia [1] . 2. Chronic toxicity: In rats treated with Benidipine HCl (10, 30, 100 mg/kg/day, oral) for 6 months, no significant toxicity was observed at 10 mg/kg. At 30 mg/kg, mild myocardial hypertrophy was noted (no functional impairment). At 100 mg/kg, severe hypotension (SBP <80 mmHg), renal tubular degeneration, and hepatic steatosis were detected. The no-observed-adverse-effect level (NOAEL) was 10 mg/kg [1] . In dogs treated with 5, 15, 50 mg/kg/day for 6 months, NOAEL was 15 mg/kg (50 mg/kg caused gastrointestinal disturbances and weight loss) [1] . 3. Plasma protein binding: In human plasma, the protein binding rate of Benidipine HCl was >99% (determined by equilibrium dialysis) [1] ; In rat and dog plasma, binding rates were 98.5% and 99.2%, respectively [1] . 4. Drug-drug interactions: Benidipine HCl co-administration with CYP3A4 inhibitors (e.g., ketoconazole) increased human plasma AUC by 3.2-fold, due to reduced metabolism [1] . Co-administration with other antihypertensive drugs (e.g., ACE inhibitors, β-blockers) enhanced hypotensive effects (additive effect), requiring dose adjustment [1] . No significant interactions with CYP2C9, CYP2C19, or CYP2E1 substrates were observed [1] . 5. Reproductive and developmental toxicity: In pregnant rats, oral Benidipine HCl (10, 30, 100 mg/kg/day) during gestation had no teratogenic effects at 30 mg/kg; 100 mg/kg caused fetal growth retardation (reduced birth weight) [1] . |
| References |
[1]. Pharmacological, pharmacokinetic, and clinical properties of benidipine hydrochloride, a novel, long-acting calcium channel blocker. J Pharmacol Sci. 2006 Apr;100(4):243-61. [2]. Anti-apoptotic effect of benidipine, a long-lasting vasodilating calcium antagonist, in ischaemic/reperfused myocardial cells. Br J Pharmacol. 2001 Feb;132(4):869-78. [3]. Benidipine stimulates nitric oxide synthase and improves coronary circulation in hypertensive rats. Am J Hypertens. 1999 May;12(5):483-91. [4]. Orally administered benidipine and manidipine prevent ischemia-reperfusion injury in the rat heart. Circ J. 2004 Mar;68(3):241-6. [5]. Benidipine, a dihydropyridine-Ca2+ channel blocker, increases the endothelial differentiation of endothelial progenitor cells in vitro. Hypertens Res. 2006 Dec;29(12):1047-54. [6]. Broad antiproliferative effects of benidipine on cultured human mesangial cells in cell cycle phases. Am J Nephrol. 2002 Sep-Dec;22(5-6):581-6. |
| Additional Infomation |
1. Chemical class and mechanism of action: Benidipine HCl is a long-acting dihydropyridine-type calcium channel blocker (DHP-CCB). Its mechanism involves: (1) blocking L-type calcium channels in vascular smooth muscle cells, reducing calcium influx and vasodilation (main antihypertensive effect); (2) activating endothelial NOS, increasing NO production to enhance vasodilation and protect vascular endothelium; (3) inhibiting myocardial cell apoptosis and mesangial cell proliferation, exerting organ protection (heart, kidney) [1, 2, 3, 6] . 2. Clinical indications and dosage: Benidipine HCl is clinically approved for the treatment of essential hypertension and chronic stable angina pectoris. The recommended oral dose for hypertension is 4-8 mg once daily (maximum 12 mg/day); for angina, 4 mg twice daily [1] . Its long-acting property (t₁/₂ ~14 hours in humans) allows once-daily administration, improving patient compliance [1] . 3. Advantage over other DHP-CCBs: Compared to short-acting DHP-CCBs (e.g., nifedipine), Benidipine HCl has a longer duration of action and less reflex tachycardia (due to weaker cardiac calcium channel blocking effect relative to vascular effects). Compared to other long-acting DHPs (e.g., amlodipine), it shows stronger endothelial protection and renal protective effects (reducing mesangial proliferation) [1, 3, 6] . 4. Preclinical organ protection evidence: Beyond antihypertension, Benidipine HCl demonstrates: (1) myocardial protection against I/R injury (reducing infarct size, inhibiting apoptosis); (2) renal protection (reducing proteinuria, preserving GFR); (3) coronary circulation improvement (increasing CBF via NO activation) [2, 3, 4, 6] . |
Solubility Data
| Solubility (In Vitro) |
|
|||
| Solubility (In Vivo) |
Solubility in Formulation 1: ≥ 2.08 mg/mL (3.84 mM) (saturation unknown) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 20.8 mg/mL clear DMSO stock solution to 400 μL PEG300 and mix evenly; then add 50 μL Tween-80 to the above solution and mix evenly; then add 450 μL normal saline to adjust the volume to 1 mL. Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH₂ O to obtain a clear solution. Solubility in Formulation 2: 2.08 mg/mL (3.84 mM) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (add these co-solvents sequentially from left to right, and one by one), suspension solution; with ultrasonication. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 20.8 mg/mL clear DMSO stock solution to 900 μL of 20% SBE-β-CD physiological saline solution and mix evenly. Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 1.8450 mL | 9.2248 mL | 18.4495 mL | |
| 5 mM | 0.3690 mL | 1.8450 mL | 3.6899 mL | |
| 10 mM | 0.1845 mL | 0.9225 mL | 1.8450 mL |