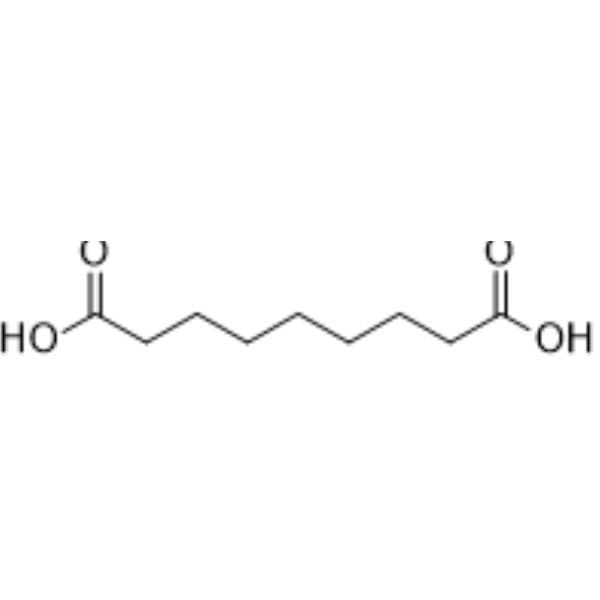
Physicochemical Properties
| Molecular Formula | C9H16O4 |
| Molecular Weight | 188.22 |
| Exact Mass | 188.104 |
| CAS # | 123-99-9 |
| Related CAS # | Azelaic acid-d14;119176-67-9 |
| PubChem CID | 2266 |
| Appearance | White to off-white solid powder |
| Density | 1.1±0.1 g/cm3 |
| Boiling Point | 286 ºC (100 mmHg) |
| Melting Point | 98-103 ºC |
| Flash Point | 215 ºC |
| Vapour Pressure | 0.0±1.8 mmHg at 25°C |
| Index of Refraction | 1.475 |
| LogP | 1.33 |
| Hydrogen Bond Donor Count | 2 |
| Hydrogen Bond Acceptor Count | 4 |
| Rotatable Bond Count | 8 |
| Heavy Atom Count | 13 |
| Complexity | 147 |
| Defined Atom Stereocenter Count | 0 |
| InChi Key | BDJRBEYXGGNYIS-UHFFFAOYSA-N |
| InChi Code | InChI=1S/C9H16O4/c10-8(11)6-4-2-1-3-5-7-9(12)13/h1-7H2,(H,10,11)(H,12,13) |
| Chemical Name | nonanedioic acid |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets |
Plant systemic acquired resistance (SAR) signaling pathway Induces the expression of AZELAIC ACID INDUCED 1 (AZI1) gene[1] The exact mechanism of action of azelaic acid is not fully known. It possesses antimicrobial activity against Propionibacterium acnes and Staphylococcus epidermidis, which may be due to inhibition of microbial cellular protein synthesis. Azelaic acid also exhibits antitryrosinase and antimitochondrial enzymatic activities, and may reduce hyperpigmentation through free radical scavenging. [2] |
| ln Vitro |
Azelaic acid (0.5 M, 48 h-7 D) exerts bacteriostatic properties [3]. < br /> Azelaic acid (5 M, 24 h) can lower intracellular reactive oxygen species (ROS) levels and boost antioxidant capacity [5] ]. < br /> Azelaic acid (1-100 nM, 24 hours) suppresses the transitory ability of B16, HMB2 and SK23 cells in a dose-regulated manner [6]. < br /> Azelaic acid has been shown to possess antimicrobial activity against Propionibacterium acnes and Staphylococcus epidermidis. Electron microscopic and immunohistochemical evaluation of skin biopsy specimens from human subjects treated with azelaic acid cream demonstrated a reduction in stratum corneum thickness, reduction in number and size of keratohyalin granules, and reduction in the amount and distribution of filaggrin in epidermal layers. [2] |
| ln Vivo |
For mild papulopustules, azelaic acid (15% Conductive, applied twice daily) is beneficial [4]. Azelaic acid accumulates in the vascular sap of Arabidopsis after bacterial infection and confers both local and systemic resistance against Pseudomonas syringae[1] Treatment with azelaic acid primes plants to accumulate higher levels of salicylic acid (SA) upon subsequent pathogen infection[1] Azelaic acid treatment increases expression of the SA-associated defense marker gene PRI upon infection[1] The mobility of azelaic acid within the plant was demonstrated, and its accumulation is increased in biologically active petiole exudates[1] Azelaic acid requires functional SA biosynthesis and signaling pathways, as well as the DIR1 protein, to confer disease resistance[1] Loss of the AZI1 gene abolishes systemic immunity triggered by azelaic acid and the priming of SA induction[1] In patients with papulopustular rosacea, topical application of azelaic acid (20% cream or 15% gel) resulted in significant decreases in mean inflammatory lesion count and erythema severity compared to vehicle in four out of five randomized controlled trials. No significant improvement in telangiectasia severity was observed. [2] |
| Cell Assay |
Cell viability assay[6] Cell Types: B16, HMB2 and SK23, CHO Tested Concentrations: 10 nM, 20 nM, 30 nM, 40 nM, 50 nM, 60 nM, 70 nM, 80 nM, 90 nM, 100 nM Incubation Duration: 24 hour Experimental Results: Dramatically diminished amounts of B16, HMB2 and SK23 compared to CHO. |
| Animal Protocol |
Animal/Disease Models: Human Rosacea 12 Weeks[4] Doses: 15% Gel Application: Smear Experimental Results: 78% of azelaic acid patients demonstrated excellent improvement. Arabidopsis thaliana plants (wild-type Col and mutant lines) were used[1] For local immunization, leaves were infiltrated with Pseudomonas syringae pv. maculicola DG3 (PmaDG3) or the avirulent strain PmaDG6/avrPtz2[1] Azelaic acid (concentration not specified) was infiltrated into leaves to test its ability to induce systemic resistance[1] Petiole exudates (Pex) were collected from infected leaves over 72 hours and used for transfer experiments[1] For systemic challenge, distal leaves were inoculated with PmaDG3 bacteria 2 days after primary treatment or exudate injection[1] Bacterial growth was measured to assess resistance[1] SA levels and PRI gene expression were analyzed in distal leaves after infection[1] |
| ADME/Pharmacokinetics |
Absorption, Distribution and Excretion Approximately 4% of the topically applied azelaic acid is systemically absorbed. Azelaic acid is mainly excreted unchanged in the urine, but undergoes some ß-oxidation to shorter chain dicarboxylic acids. ...Azelaic acid (AA, C9 dicarboxylic acid)... when administered perorally to humans, at the same concentrations as the other /dicarboxylic acids/ (DA), it reaches much higher serum and urinary concentrations. Serum concentrations and urinary excretion obtained with intravenous or intra-arterial infusions of AA are significantly higher than those achievable by oral administration. Together with AA, variable amounts of its catabolites, mainly pimelic acid, are found in serum and urine, indicating an involvement of mitochondrial beta-oxidative enzymes. Short-lived serum levels of AA follow a single 1 hr intravenous infusion, but prolonging the period of infusion with successive doses of similar concentration produces sustained higher levels during the period of administration. These levels are consistent with the concentrations of AA capable of producing a cytotoxic effect on tumoral cells in vitro. AA is capable of crossing the blood-brain barrier: its concentration in the cerebrospinal fluid is normally in the range of 2-5% of the values in the serum. Azelaic acid was the first dicarboxylic acid proposed as an alternative energy substrate in total parenteral nutrition. In this study, the pharmacokinetics of azelaic acid were investigated in 12 healthy volunteers, 7 receiving a constant infusion (10 g over 90 min) and 5 a bolus dose (1g). The 24 hr urinary excretion and plasma concentration in blood samples taken at regular intervals were assayed by gas-liquid chromatography. Experimental data were analysed by a 2-compartment nonlinear model that describes both tubular secretion and cellular uptake in Michaelis-Menten terms. A high value of urinary excretion (mean 76.9% of infused dose) and a mean clearance of 8.42 L/hr were found, suggesting the presence of tubular secretion. Estimating the population mean of the pharmacokinetic model parameters gave a maximal cellular uptake of 0.657 g/hr. The model predicts that 90% of the maximal uptake should be reached in the plateau phase of a constant infusion of 2.2 g/hr. The presence of extensive and rapid losses through urinary excretion, and the low estimated value of the maximal cellular uptake, indicate that azelaic acid is not suitable as an energy substrate for total parenteral nutrition. Follicular concentrations of azelaic acid (AzA) were determined in vivo using a rapid, non-invasive method, after a single topical application of 20% (w/w) AzA cream, in order to establish whether the in vitro antimicrobial effects observed in previous studies are relevant in vivo. Preweighed amounts of 20% (w/w) AzA cream were applied over demarcated areas on the forehead and back of nine young adults, and samples were taken over a period of 5 hr. AzA was removed from the skin surface by washing with acetone, and follicular casts were collected using cyanacrylate gel. The samples were centrifuged to remove particulate matter, and the supernatants derivatized for analysis by HPLC. Although the results showed wide-ranging variability, the follicular concentration increased as the amount present on the surface declined. The maximum follicular concentrations of AzA attained ranged from 7.5 to 52.5 ng (micrograms of follicular casts)-1 and 0.5 to 23.4 ng/(ug of follicular casts) in samples taken from the back and forehead, respectively. Assuming an average density of follicular material of 0.9 g/mL, the mean maximum follicular concentration attained on the back was between 36 and 251 mmol/L, and on the forehead was between 2 and 112 mmol/L, and indicates that the concentration of AzA attained in follicular casts after a single topical application is comparable with the concentration required to inhibit the growth of Propionibacterium acnes and Staphylococcus epidermidis, in vitro. Six healthy male volunteers received a single topical treatment with 5 g of an anti-acne cream containing 20% azelaic acid (AzA) onto the face, the chest and the upper back. One week later 1 g of AzA was given orally to the same subjects as aqueous microcrystalline suspension. Following the two treatments the renal excretion of the unchanged compound was measured. Analysis included ether extraction of the urine, derivatization of extract and HPLC with UV detection. After topical application 2.2 +/- 0.7%, and after oral administration 61.2 +/- 8.8% of the dose had been excreted unchanged with the urine. By comparing both amounts, the percutaneous absorption of AzA from the cream was assessed to 3.6% of the dermally applied dose. For more Absorption, Distribution and Excretion (Complete) data for 1,7-HEPTANEDICARBOXYLIC ACID (7 total), please visit the HSDB record page. Metabolism / Metabolites Mainly excreted unchanged in the urine but undergoes some b-oxidation to shorter chain dicarboxylic acids. Approximately 60% of an oral-dose is excreted unchanged in the urine within 12 hr, and it is partly metabolized by -oxidation. After 8 hr, 6% of the radioactivity from a tracer dose of [14C]azelaic acid to rats was recovered as 14CO2. Successive cleavage by -oxidation results in the formation of pimelic and glutaric acids and subsequently malonyl-CoA and acetyl-CoA. Thus, azelaic acid is incorporated into fatty acid biosynthesis and the citric acid cycle Pimelic acid is largely excreted unchanged in humans and dogs; the extent varies with the dose. Some degree of -oxidation occurs with dicarboxylic acids and, results in the formation of dicarboxylic acids that have two fewer carbon atoms than the parent acid. Pimelic acid has been identified as a metabolite of azelaic acid in microorganisms. Mainly excreted unchanged in the urine but undergoes some b-oxidation to shorter chain dicarboxylic acids. Route of Elimination: Azelaic acid is mainly excreted unchanged in the urine, but undergoes some нф-oxidation to shorter chain dicarboxylic acids. Half Life: The observed half-lives in healthy subjects are approximately 45 minutes after oral dosing and 12 hours after topical dosing, indicating percutaneous absorption rate-limited kinetics. Biological Half-Life The observed half-lives in healthy subjects are approximately 45 minutes after oral dosing and 12 hours after topical dosing, indicating percutaneous absorption rate-limited kinetics. The observed half-lives in healthy subjects are approximately 45 minutes after oral dosing and 12 hours after topical dosing, Azelaic acid is described as a mobile metabolite that moves within the plant vascular system[1] Its concentration increases in the vascular sap following local bacterial infection[1] |
| Toxicity/Toxicokinetics |
Effects During Pregnancy and Lactation ◉ Summary of Use during Lactation Topical azelaic acid has not been studied during breastfeeding. Because only 4% of a dose is absorbed after topical application and it is a chemical that appears in foods, bloodstream and breastmilk normally, azelaic acid is considered a low risk to the nursing infant. If azelaic acid is required by the mother, it is not a reason to discontinue breastfeeding. Do not apply azelaic acid to the breast or nipple and ensure that the infant's skin does not come into direct contact with the areas of skin that have been treated. Only water-miscible cream or gel products should be applied to the breast because ointments may expose the infant to high levels of mineral paraffins via licking. ◉ Effects in Breastfed Infants Relevant published information was not found as of the revision date. ◉ Effects on Lactation and Breastmilk Relevant published information was not found as of the revision date. Common treatment-related adverse effects associated with azelaic acid use included local cutaneous irritation symptoms such as burning and stinging, which were generally transient and mild to moderate in intensity. [2] |
| References |
[1]. Priming in systemic plant immunity. Science. 2009 Apr 3;324(5923):89-91. [2]. Azelaic acid in the treatment of papulopustular rosacea: a systematic review of randomized controlled trials. Arch Dermatol. 2006 Aug;142(8):1047-52. [3]. The in vitro antimicrobial effect of azelaic acid. Br J Dermatol. 1986 Nov;115(5):551-6. [4]. Azelaic acid 15% gel in the treatment of rosacea. [5]. Azelaic Acid Exerts Antileukemia Effects against Acute Myeloid Leukemia by Regulating the Prdxs/ROS Signaling Pathway. Oxid Med Cell Longev. 2020 Dec 23:2020:1295984. [6]. Effect of azelaic acid on melanoma cells in culture. Exp Dermatol. 1995 Apr;4(2):79-81. |
| Additional Infomation |
Nonanedioic acid is an alpha,omega-dicarboxylic acid that is heptane substituted at positions 1 and 7 by carboxy groups. It has a role as an antibacterial agent, an antineoplastic agent, a dermatologic drug and a plant metabolite. It is a dicarboxylic fatty acid and an alpha,omega-dicarboxylic acid. It is a conjugate acid of an azelaate(2-) and an azelaate. Azelaic acid is a saturated dicarboxylic acid found naturally in wheat, rye, and barley. It is also produced by Malassezia furfur, also known as Pityrosporum ovale, which is a species of fungus that is normally found on human skin. Azelaic acid is effective against a number of skin conditions, such as mild to moderate acne, when applied topically in a cream formulation of 20%. It works in part by stopping the growth of skin bacteria that cause acne, and by keeping skin pores clear. Azelaic acid's antimicrobial action may be attributable to inhibition of microbial cellular protein synthesis. Azelaic acid is a metabolite found in or produced by Escherichia coli (strain K12, MG1655). The physiologic effect of azelaic acid is by means of Decreased Protein Synthesis, and Decreased Sebaceous Gland Activity. Azelaic acid has been reported in Tuber indicum, Streptomyces nigra, and other organisms with data available. Azelaic Acid is a naturally occurring dicarboxylic acid produced by Malassezia furfur and found in whole grain cereals, rye, barley and animal products. Azelaic acid possesses antibacterial, keratolytic, comedolytic, and anti-oxidant activity. Azelaic acid is bactericidal against Proprionibacterium acnes and Staphylococcus epidermidis due to its inhibitory effect on the synthesis of microbial cellular proteins. Azelaic acid exerts its keratolytic and comedolytic effects by reducing the thickness of the stratum corneum and decreasing the number of keratohyalin granules by reducing the amount and distribution of filaggrin in epidermal layers. Azelaic acid also possesses a direct anti-inflammatory effect due to its scavenger activity of free oxygen radical. This drug is used topically to reduce inflammation associated with acne and rosacea. Azelaic acid is a saturated dicarboxylic acid found naturally in wheat, rye, and barley. It is a natural substance that is produced by Malassezia furfur (also known as Pityrosporum ovale), a yeast that lives on normal skin. It is effective against a number of skin conditions, such as mild to moderate acne, when applied topically in a cream formulation of 20%. It works in part by stopping the growth of skin bacteria that cause acne, and by keeping skin pores clear. Azelaic acid's antimicrobial action may be attributable to inhibition of microbial cellular protein synthesis. See also: Azelaic acid; niacinamide (component of) ... View More ... Drug Indication For the topical treatment of mild-to-moderate inflammatory acne vulgaris. FDA Label Mechanism of Action The exact mechanism of action of azelaic acid is not known. It is thought that azelaic acid manifests its antibacterial effects by inhibiting the synthesis of cellular protein in anaerobic and aerobic bacteria, especially Staphylococcus epidermidis and Propionibacterium acnes. In aerobic bacteria, azelaic acid reversibly inhibits several oxidoreductive enzymes including tyrosinase, mitochondrial enzymes of the respiratory chain, thioredoxin reductase, 5-alpha-reductase, and DNA polymerases. In anaerobic bacteria, azelaic acid impedes glycolysis. Along with these actions, azelaic acid also improves acne vulgaris by normalizing the keratin process and decreasing microcomedo formation. Azelaic acid may be effective against both inflamed and noninflamed lesions. Specifically, azelaic acid reduces the thickness of the stratum corneum, shrinks keratohyalin granules by reducing the amount and distribution of filaggrin (a component of keratohyalin) in epidermal layers, and lowers the number of keratohyalin granules. Azelaic acid, and other saturated dicarboxylic acids (C9-C12), are shown to be competitive inhibitors of tyrosinase (KI azelaic acid = 2.73 X 10(-3) M) and of membrane-associated thioredoxin reductase (KI azelaic acid = 1.25 X 10(-5) M). The monomethyl ester of azelaic acid does not inhibit thioredoxin reductase, but it does inhibit tyrosinase, although double the concentration is necessary compared with azelaic acid (KI azelaic acid monomethyl ester = 5.24 X 10(-3) M). Neither azelaic acid nor its monomethyl ester inhibit tyrosinase when catechol is used as a substrate instead of L-tyrosine. Therefore, the weak inhibitory action of azelaic acid on tyrosinase appears to be due to the competition of a single carboxylate group on this inhibitor for the alpha-carboxylate binding site of the L-tyrosine substrate on the enzyme active site. Based on the inhibitor constant on tyrosinase, at least cytotoxic levels of azelaic acid would be required for the direct inhibition of melanin biosynthesis in melanosomes if this mechanism is responsible for depigmentation in the hyperpigmentation disorders lentigo maligna and melasma. Alternatively only 10(-5) M azelaic acid is required to inhibit thioredoxin reductase. This enzyme is shown to regulate tyrosinase through a feedback mechanism involving electron transfer to intracellular thioredoxin, followed by a specific interaction between reduced thioredoxin and tyrosinase. Furthermore, the thioredoxin reductase/thioredoxin system is shown to be a principal electron donor for the ribonucleotide reductases which regulates DNA synthesis. The exact mechanism of action of topically applied azelaic acid in the treatment of acne vulgaris has not been fully elucidated; however, the effect appears to result partly from the antibacterial activity of the drug. Azelaic acid inhibits the growth of susceptible organisms (principally Propionibacterium acnes) on the surface of the skin by inhibiting protein synthesis. In addition, the drug also may inhibit follicular keratinization, which may prevent development or maintenance of comedones. Azelaic acid usually is bacteriostatic in action, but may be bactericidal in high concentrations against P. acnes and Staphylococcus epidermidis. Azelaic acid also exhibits antiproliferative effects against hyperactive and abnormal melanocytes but does not exhibit an appreciable depigmenting effect on normally pigmented skin. Azelaic acid is a nine-carbon dicarboxylic acid[1] It is identified as a component of plant systemic acquired resistance (SAR)[1] It functions upstream of salicylic acid (SA) accumulation and the DIR1-dependent signaling pathway, and downstream or independent of SFD1 and FAD7 genes[1] It does not cause major transcriptional reprogramming; microarray analysis showed no significant changes in defense-related gene expression upon treatment[1] The AZI1 gene, which encodes a predicted secreted protein, is induced by azelaic acid and is essential for SAR signal production/translocation[1] Azelaic acid is used in the treatment of papulopustular rosacea and acne vulgaris. It appears to be as effective as, if not better than, topical metronidazole in reducing inflammatory lesions and erythema. The review suggests that a standardized scoring system for rosacea severity assessment is needed. [2] |
Solubility Data
| Solubility (In Vitro) |
DMSO : ≥ 100 mg/mL (~531.29 mM) H2O : ~2 mg/mL (~10.63 mM) |
| Solubility (In Vivo) |
Solubility in Formulation 1: ≥ 2.5 mg/mL (13.28 mM) (saturation unknown) in 10% DMSO + 40% PEG300 + 5% Tween80 + 45% Saline (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 400 μL PEG300 and mix evenly; then add 50 μL Tween-80 to the above solution and mix evenly; then add 450 μL normal saline to adjust the volume to 1 mL. Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH₂ O to obtain a clear solution. Solubility in Formulation 2: ≥ 2.5 mg/mL (13.28 mM) (saturation unknown) in 10% DMSO + 90% (20% SBE-β-CD in Saline) (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 900 μL of 20% SBE-β-CD physiological saline solution and mix evenly. Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Solubility in Formulation 3: ≥ 2.5 mg/mL (13.28 mM) (saturation unknown) in 10% DMSO + 90% Corn Oil (add these co-solvents sequentially from left to right, and one by one), clear solution. For example, if 1 mL of working solution is to be prepared, you can add 100 μL of 25.0 mg/mL clear DMSO stock solution to 900 μL of corn oil and mix evenly. (Please use freshly prepared in vivo formulations for optimal results.) |
| Preparing Stock Solutions | 1 mg | 5 mg | 10 mg | |
| 1 mM | 5.3129 mL | 26.5647 mL | 53.1293 mL | |
| 5 mM | 1.0626 mL | 5.3129 mL | 10.6259 mL | |
| 10 mM | 0.5313 mL | 2.6565 mL | 5.3129 mL |