Physicochemical Properties
| Molecular Formula | C19H19N3O2 |
| Exact Mass | 321.147 |
| Elemental Analysis | C, 71.01; H, 5.96; N, 13.08; O, 9.96 |
| CAS # | 1254032-16-0 |
| Related CAS # | 1422144-42-0 (mesylate);1254032-66-0;1253952-02-1 (HCl);1254032-16-0; |
| PubChem CID | 134128281 |
| Appearance | White to off-white solid powder |
| LogP | 1.6 |
| Hydrogen Bond Donor Count | 3 |
| Hydrogen Bond Acceptor Count | 4 |
| Rotatable Bond Count | 5 |
| Heavy Atom Count | 24 |
| Complexity | 409 |
| Defined Atom Stereocenter Count | 1 |
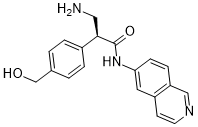
| SMILES | O=C([C@H](CN)C1C=CC(CO)=CC=1)NC1C=CC2C=NC=CC=2C=1 |
| InChi Key | LTXBFJFJUIJOQE-GOSISDBHSA-N |
| InChi Code | InChI=1S/C19H19N3O2/c20-10-18(14-3-1-13(12-23)2-4-14)19(24)22-17-6-5-16-11-21-8-7-15(16)9-17/h1-9,11,18,23H,10,12,20H2,(H,22,24)/t18-/m1/s1 |
| Chemical Name | (2S)-3-amino-2-[4-(hydroxymethyl)phenyl]-N-isoquinolin-6-ylpropanamide |
| Synonyms | AR-11324 metabolite; AR13503; AR11324 metabolite; AR-13324 M1 metabolite; AR-13503; 2309668-15-1; 4MVW7F3BCT; Netarsudil metabolite AR-13503; UNII-4MVW7F3BCT; 1254032-16-0; CHEMBL4753043; Netarsudil metabolite; AR 11324 metabolite; AR-13503 AR 13503 |
| HS Tariff Code | 2934.99.9001 |
| Storage |
Powder-20°C 3 years 4°C 2 years In solvent -80°C 6 months -20°C 1 month |
| Shipping Condition | Room temperature (This product is stable at ambient temperature for a few days during ordinary shipping and time spent in Customs) |
Biological Activity
| Targets | ROCK/PKC; metabolite of Netarsudil |
| ln Vitro | Human venous vascular endothelial cell (HUVEC) tube formation is inhibited by AR-13503 (16 hours) at an IC50 of 21 nM[1]. In a dose-dependent approach, AR-13503 (400 nM; 5 days) decreases the sprouting area of venous vasculature [1]. In a dose-dependent manner, AR-13503 (400 nM; 2 weeks) improves the primary RPE barrier function in pigs [1]. |
| ln Vivo | In combination with Aflibercept, AR-13503 (1.25 mg/kg; intraperitoneal injection; once daily for 5 days) effectively inhibits the development of aberrant neovascularization (NV) [1]. |
| Animal Protocol |
Animal/Disease Models: Oxygen-induced retinopathy (OIR) mouse model (C57BL/6; 7 days old) [1] Doses: 1.25 mg/kg Route of Administration: intraperitoneal (ip) injection; one time/day for 5 days Experimental Results: Combination treatment group The reduction in NV (approximately 75%) was greater than that in the aflibercept alone group (approximately 55%). In the oxygen-induced retinopathy (OIR) animal model, 7-day old neonatal C57BL/6 mice were housed with foster mothers at 75% oxygen from postnatal day (P)7 to P12. Upon return to normoxia on P12, mice were treated by once daily intraperitoneal injections with vehicle control, aflibercept, or AR-13503 in combination with aflibercept. Tissues were harvested following 5 days of treatment and stained for isolectin-IB4 for visualization and analysis of NV. Retinas were also harvested for pharmacokinetic analysis.[2] |
| References |
[1]. ROCK/PKC inhibitor AR-13503 inhibits angiogenesis and protects the barrier function of retinal pigment epithelium. Investigative Ophthalmology & Visual Science, 2018, 59(9): 205-205. [2]. AR-13503 Enhances the efficacy of aflibercept in a mouse model of proliferative diabetic retinopathy. Investigative Ophthalmology & Visual Science, 2018, 59(9): 200-200. |
| Additional Infomation |
Diabetic retinopathy (DR) and its complications can lead to irreversible vision loss. New therapies with novel mechanisms of action are needed as anti-vascular endothelial growth factor (VEGF) and steroid treatments have significant limitations. Rho kinase (ROCK) has been implicated in the development of retinal neovascularization (NV) and vascular leakage in neovascular age-related macular degeneration (nAMD) and proliferative diabetic retinopathy (PDR). AR-13503 is a potent ROCK and protein kinase C (PKC) inhibitor. We have separately shown that AR-13503 inhibited angiogenesis and enhanced retinal pigmented epithelium barrier function in in vitro and ex vivo assays. Here, we investigated the effect of AR-13503 on the formation of aberrant neovascularization (NV) in an animal model of PDR.[2] Results : AR-13503 was detectable in mouse retinas following systemic treatment with 1.25 mg/kg/day. Mice treated with aflibercept alone had a reduction in NV of ~55% relative to vehicle control. The combination of AR-13503 and aflibercept had a greater (~75%) reduction in NV than aflibercept alone. There were no significant differences in the size of avascular areas among groups.[2] |
Solubility Data
| Solubility (In Vitro) | May dissolve in DMSO (in most cases), if not, try other solvents such as H2O, Ethanol, or DMF with a minute amount of products to avoid loss of samples |
| Solubility (In Vivo) |
Note: Listed below are some common formulations that may be used to formulate products with low water solubility (e.g. < 1 mg/mL), you may test these formulations using a minute amount of products to avoid loss of samples. Injection Formulations (e.g. IP/IV/IM/SC) Injection Formulation 1: DMSO : Tween 80: Saline = 10 : 5 : 85 (i.e. 100 μL DMSO stock solution → 50 μL Tween 80 → 850 μL Saline) *Preparation of saline: Dissolve 0.9 g of sodium chloride in 100 mL ddH ₂ O to obtain a clear solution. Injection Formulation 2: DMSO : PEG300 :Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL DMSO → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Injection Formulation 3: DMSO : Corn oil = 10 : 90 (i.e. 100 μL DMSO → 900 μL Corn oil) Example: Take the Injection Formulation 3 (DMSO : Corn oil = 10 : 90) as an example, if 1 mL of 2.5 mg/mL working solution is to be prepared, you can take 100 μL 25 mg/mL DMSO stock solution and add to 900 μL corn oil, mix well to obtain a clear or suspension solution (2.5 mg/mL, ready for use in animals). Injection Formulation 4: DMSO : 20% SBE-β-CD in saline = 10 : 90 [i.e. 100 μL DMSO → 900 μL (20% SBE-β-CD in saline)] *Preparation of 20% SBE-β-CD in Saline (4°C,1 week): Dissolve 2 g SBE-β-CD in 10 mL saline to obtain a clear solution. Injection Formulation 5: 2-Hydroxypropyl-β-cyclodextrin : Saline = 50 : 50 (i.e. 500 μL 2-Hydroxypropyl-β-cyclodextrin → 500 μL Saline) Injection Formulation 6: DMSO : PEG300 : castor oil : Saline = 5 : 10 : 20 : 65 (i.e. 50 μL DMSO → 100 μLPEG300 → 200 μL castor oil → 650 μL Saline) Injection Formulation 7: Ethanol : Cremophor : Saline = 10: 10 : 80 (i.e. 100 μL Ethanol → 100 μL Cremophor → 800 μL Saline) Injection Formulation 8: Dissolve in Cremophor/Ethanol (50 : 50), then diluted by Saline Injection Formulation 9: EtOH : Corn oil = 10 : 90 (i.e. 100 μL EtOH → 900 μL Corn oil) Injection Formulation 10: EtOH : PEG300:Tween 80 : Saline = 10 : 40 : 5 : 45 (i.e. 100 μL EtOH → 400 μLPEG300 → 50 μL Tween 80 → 450 μL Saline) Oral Formulations Oral Formulation 1: Suspend in 0.5% CMC Na (carboxymethylcellulose sodium) Oral Formulation 2: Suspend in 0.5% Carboxymethyl cellulose Example: Take the Oral Formulation 1 (Suspend in 0.5% CMC Na) as an example, if 100 mL of 2.5 mg/mL working solution is to be prepared, you can first prepare 0.5% CMC Na solution by measuring 0.5 g CMC Na and dissolve it in 100 mL ddH2O to obtain a clear solution; then add 250 mg of the product to 100 mL 0.5% CMC Na solution, to make the suspension solution (2.5 mg/mL, ready for use in animals). Oral Formulation 3: Dissolved in PEG400 Oral Formulation 4: Suspend in 0.2% Carboxymethyl cellulose Oral Formulation 5: Dissolve in 0.25% Tween 80 and 0.5% Carboxymethyl cellulose Oral Formulation 6: Mixing with food powders Note: Please be aware that the above formulations are for reference only. InvivoChem strongly recommends customers to read literature methods/protocols carefully before determining which formulation you should use for in vivo studies, as different compounds have different solubility properties and have to be formulated differently. (Please use freshly prepared in vivo formulations for optimal results.) |